Eczema in Sensitive Zones: Nipples and Genitals
Discover effective strategies for managing eczema on nipples and genital areas, from symptoms to treatments and when to seek help.
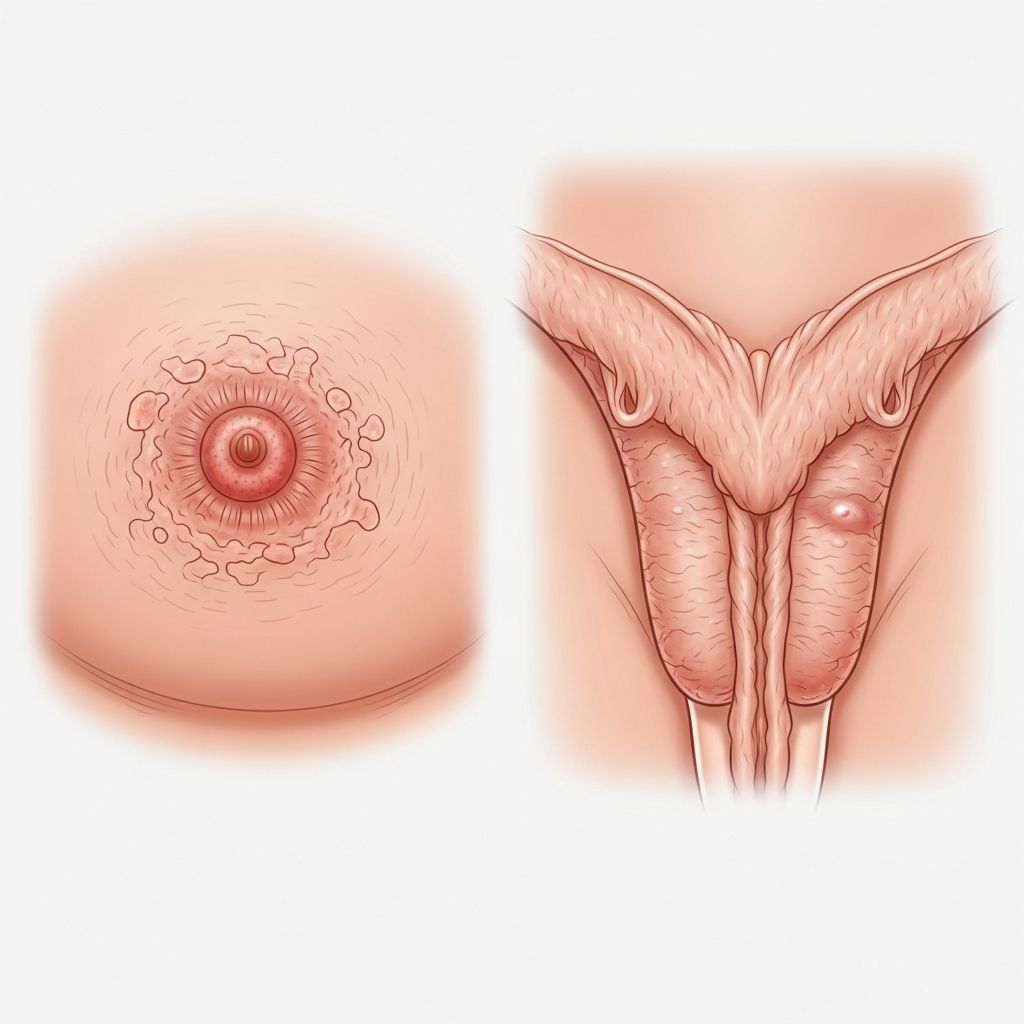
Eczema, a chronic inflammatory skin disorder, can appear on highly sensitive areas like the nipples and genitals, causing significant discomfort due to the thin skin and constant exposure to friction or moisture in these regions. These locations demand specialized care because standard treatments may irritate further or fail to address unique triggers.
Recognizing Eczema on Nipples
Nipple eczema primarily impacts the areola, the pigmented skin encircling the nipple, leading to red, scaly patches that itch intensely. The skin may become dry, rough, or leathery, with possible swelling, oozing, or crusting in acute phases. Unlike other body areas, nipple involvement often heightens sensitivity, amplifying pain during touch or clothing friction.
Common manifestations include:
- Persistent itching, sometimes burning or stinging sensations.
- Flaky or peeling skin around the areola.
- Thickening or lichenification from chronic scratching.
- Cracks or fissures, raising infection risk.
This condition affects various groups, including lactating individuals where breast pumps or infant saliva act as irritants. It may occur bilaterally or unilaterally but rarely extends beyond the areola unless part of widespread atopic dermatitis.
Understanding Genital Eczema
Genital eczema targets the vulva in women or scrotum and penis in men, presenting as red, inflamed skin with intense itching that prompts scratching cycles. The area’s warmth, moisture, and friction from clothing exacerbate symptoms, leading to soreness or raw patches.
- Vulvar eczema often causes dryness, fissuring, and secondary infections from yeast or bacteria.
- Male genital involvement features scaling, swelling, and discomfort during movement.
Hormonal shifts, such as those during menopause, can worsen dryness and irritation in genital skin, compounding eczema flares. Unlike nipple eczema, genital cases frequently mimic infections, requiring careful diagnosis.
Root Causes and Triggers
Eczema in these zones stems from a mix of genetic factors, immune overactivity, and environmental exposures. A compromised skin barrier allows irritants and allergens to penetrate easily, sparking inflammation.
| Trigger Type | Nipple-Specific Examples | Genital-Specific Examples |
|---|---|---|
| Irritants | Soaps, detergents, lanolin creams, friction from bras | Sweat, tight underwear, hygiene wipes, bubble baths |
| Allergens | Perfumes, dyes in fabrics, pollen | Latex, spermicides, personal care fragrances |
| Lifestyle Factors | Hot showers, dry air, breastfeeding | Menopause dryness, sexual activity friction |
| Genetic/Immune | Atopic history, overactive response | Hormonal influences post-puberty |
Post-puberty hormonal changes, especially estrogen and progesterone, may heighten risk in young adults by boosting type 2 immune responses. For nipples, contact with infant saliva or pumps during lactation is a frequent culprit.
Diagnostic Challenges and Look-Alikes
Distinguishing eczema from mimics is crucial, as misdiagnosis delays proper care. On nipples, Paget’s disease—a rare breast cancer—presents similarly with unilateral scaling, itching, and discharge, often with an underlying lump. Inflammatory breast cancer may also cause redness and swelling.
For genitals, differentials include:
- Fungal infections like candidiasis, showing white patches.
- Bacterial overgrowth or STIs with discharge or odor.
- Psoriasis with thicker plaques.
- Lichen sclerosus, causing white, scarred skin.
Consult a dermatologist for biopsy or swab if symptoms persist unilaterally, involve discharge, or resist basic treatments.
Treatment Approaches for Nipple Eczema
Management focuses on barrier repair, inflammation control, and trigger avoidance. Start with gentle cleansing using fragrance-free emollients instead of soap.
- Moisturize frequently: Apply thick, hypoallergenic creams like petroleum jelly post-shower to lock in hydration.
- Topical corticosteroids: Low-potency options (e.g., hydrocortisone 1%) for short bursts; avoid prolonged use to prevent thinning.
- Wet wraps: For severe flares, soak in cool water then apply steroid under damp bandages overnight.
- Antibiotics: If infected, indicated by pus or fever.
Breastfeeding mothers should pump and discard milk during topical treatments, resuming after clearance.
Strategies for Genital Eczema Relief
Genital skin requires ultra-gentle care due to absorption risks. Avoid douching, powders, or scented products.
- Use plain water or emollient washes for hygiene.
- Pat dry gently; apply barrier ointments like zinc oxide.
- Medium-potency steroids (e.g., clobetasone) under medical supervision for flares.
- Antihistamines or menthol creams for itch control.
Wear loose cotton underwear and change post-exercise to minimize moisture buildup.
Daily Prevention Tips
Proactive habits reduce flare frequency:
- Skin care routine: Short lukewarm showers, immediate moisturizing.
- Clothing choices: Breathable fabrics, no wool or synthetics next to skin.
- Diet and environment: Track food triggers like citrus; use humidifiers in dry climates.
- Stress management: Techniques like mindfulness, as stress worsens immunity.
For lactating individuals, ensure proper latch to reduce friction and clean nipples with water only.
Living with Chronic Eczema in Private Areas
Emotional toll accompanies physical symptoms; seek support groups for coping strategies. Long-term, calcineurin inhibitors like tacrolimus offer steroid-sparing options for sensitive sites. Phototherapy may help refractory cases under specialist guidance.
Monitor for complications like infections, marked by worsening pain or fever, necessitating prompt antibiotics.
Frequently Asked Questions (FAQs)
Can eczema on nipples affect breastfeeding?
Yes, it causes pain and cracking, but treatments allow continuation with precautions like milk expression during therapy.
Is genital eczema contagious?
No, it’s not infectious; secondary infections from scratching require treatment but don’t spread eczema itself.
How long do flares last?
With proper care, 1-2 weeks; chronic cases need ongoing management to prevent recurrence.
Are there natural remedies?
Cool compresses and colloidal oatmeal baths soothe, but consult doctors before alternatives to avoid irritation.
When to see a doctor urgently?
If unilateral, with discharge, lumps, or non-responsive to OTC care—rule out serious conditions.
Consistent care transforms management of eczema in these delicate areas, improving quality of life significantly.
References
- Breast Eczema: Symptoms, Causes and Best Treatment — Revival Research. 2023-07-06. https://revivalresearch.org/blogs/breast-eczema-cause-for-itchy-breasts/
- Nipple eczema: Symptoms, treatment, and alternative diagnoses — Medical News Today. N/A. https://www.medicalnewstoday.com/articles/eczema-on-nipple
- Nipple eczema — DermNet NZ. N/A. https://dermnetnz.org/topics/nipple-eczema
- Female genital eczema — National Eczema Society. N/A. https://eczema.org/information-and-advice/types-of-eczema/female-genital-eczema/
- Nipple eczema — LactApp. N/A. https://blog.lactapp.es/en/eczema-of-the-nipple-and-or-areola/
- Real-World Prevalence and Associated Factors of Nipple Eczema — PMC (PubMed Central). N/A. https://pmc.ncbi.nlm.nih.gov/articles/PMC12715881/
Read full bio of medha deb











