Eczema: What It Is, Symptoms, Causes, Types & Treatment
Complete guide to understanding eczema: causes, symptoms, types, and effective treatment options.
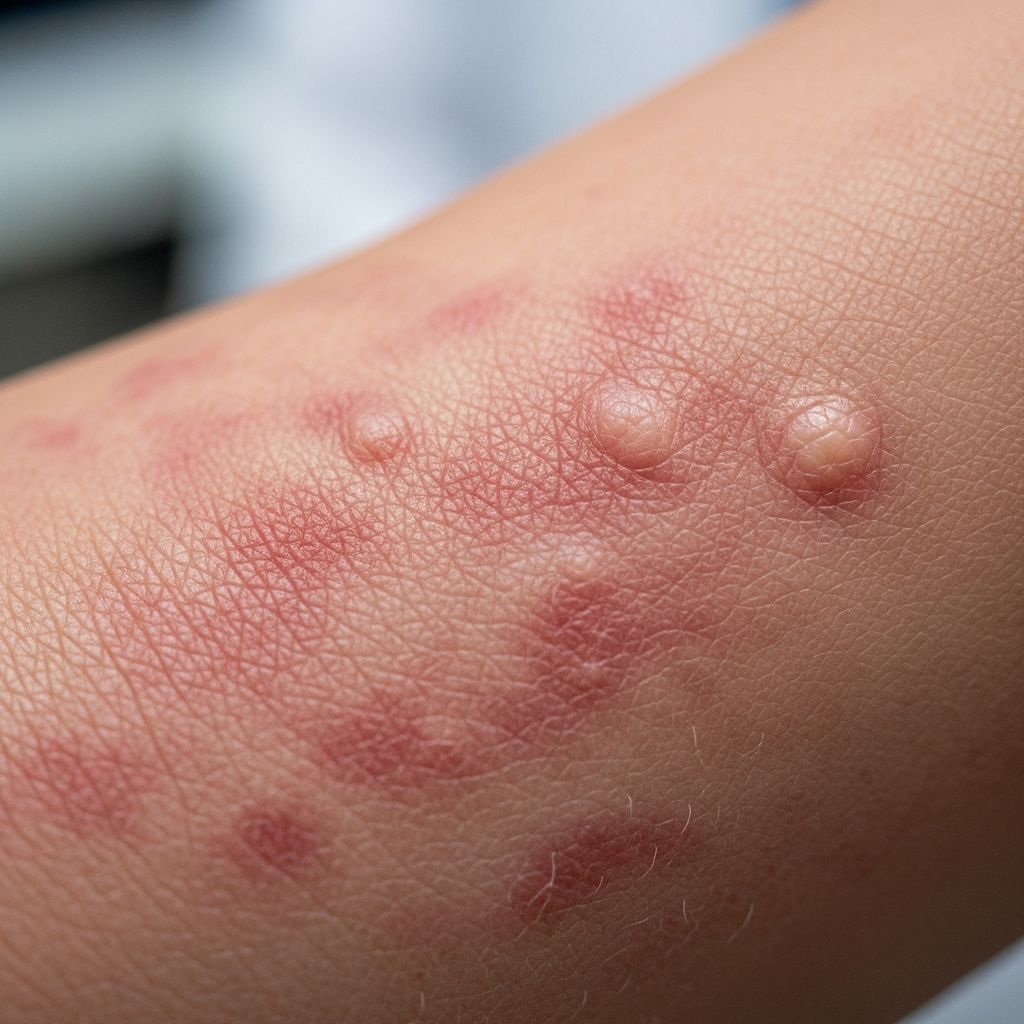
Eczema is a common skin condition that affects millions of people worldwide, causing discomfort through itching, inflammation, and visible skin changes. The term “eczema” actually describes a group of inflammatory skin conditions rather than a single disease. While there is currently no cure for eczema, understanding what it is, recognizing its symptoms, and implementing proper management strategies can significantly improve quality of life and reduce the frequency and severity of flare-ups.
Understanding Eczema: Definition and Overview
Eczema is fundamentally a condition characterized by inflammation of the skin that manifests as red, itchy, and often dry patches. The condition disrupts the skin’s natural protective barrier, allowing moisture to escape and irritants to penetrate more easily. This barrier dysfunction is central to why people with eczema experience persistent dryness and heightened sensitivity to environmental triggers.
The most common form of eczema is atopic dermatitis, which typically begins in childhood but can develop at any age. Eczema is not contagious, meaning you cannot transmit it to another person through physical contact or close proximity. This is an important distinction that helps reduce stigma and allows people with eczema to maintain normal social interactions without concern for spreading the condition.
Common Symptoms of Eczema
Recognizing the symptoms of eczema is the first step toward effective management. The condition manifests differently from person to person, but several hallmark signs are consistent across most cases:
- Intense itching, often worse at night or during stress
- Dry, sensitive, and easily irritated skin
- Red or inflamed patches of skin
- Small, raised bumps that may leak fluid when scratched
- Cracked, swollen, or thickened skin
- Raw, swollen skin from scratching
- Flaky or peeling skin
The intensity of symptoms can vary significantly between individuals and even fluctuate in the same person depending on environmental conditions, stress levels, and other triggering factors. Some people experience mild symptoms that require minimal intervention, while others develop severe manifestations that significantly impact daily functioning, sleep quality, and emotional well-being.
What Causes Eczema?
The development of eczema involves a complex interplay between genetic predisposition and environmental factors. Research indicates that eczema tends to run in families, suggesting a hereditary component. If your parents or close relatives have eczema, you have a higher likelihood of developing the condition yourself.
Beyond genetics, several environmental and lifestyle factors can trigger or exacerbate eczema:
- Harsh soaps and cleansers that strip natural oils from skin
- Extreme temperatures and humidity levels
- Stress and emotional triggers
- Allergens such as pollen, pet dander, or dust mites
- Irritating fabrics like wool or synthetic materials
- Fragrances and dyes in personal care products
- Frequent bathing or prolonged water exposure
- Certain foods that may trigger allergic responses
Understanding your personal triggers is crucial for effective eczema management. Triggers vary significantly from person to person, and what causes a flare-up in one individual may have no effect on another. Keeping a diary of symptoms, activities, and environmental exposures can help identify your specific triggers.
Types of Eczema
While atopic dermatitis is the most common form of eczema, several other types exist, each with distinct characteristics and triggers:
Atopic Dermatitis
Atopic dermatitis is the most prevalent form of eczema and typically begins in early childhood. It is characterized by intense itching, dry skin, and a predisposition to allergic conditions. The condition often improves with age but can persist into adulthood.
Contact Dermatitis
Contact dermatitis develops when the skin comes into direct contact with an irritating substance or allergen. Common triggers include poison ivy, nickel, latex, and certain personal care products. This type is often preventable by identifying and avoiding the offending substance.
Asteatotic Eczema
Also known as xerotic eczema, asteatotic eczema causes the skin to become extremely dry, cracked, and often appears as a network of fine lines. This type is particularly common in older adults, especially during winter months when humidity levels drop.
Seborrheic Dermatitis
This form of eczema typically affects the scalp, face, and upper chest, causing greasy, scaly patches. It is often associated with an overgrowth of yeast on the skin.
Dyshidrotic Eczema
Characterized by small, fluid-filled blisters on the hands and feet, dyshidrotic eczema often develops in response to stress or contact with irritants.
Diagnosis of Eczema
Diagnosing eczema typically involves a visual examination by a dermatologist or healthcare provider. Your doctor will look for characteristic signs such as patches of dry skin, discoloration, and inflammation. In some cases, when symptoms resemble other skin conditions, your provider may recommend additional tests to confirm the diagnosis or identify contributing factors.
Possible diagnostic tests may include:
- Patch testing to identify specific allergens or irritants
- Skin biopsy to rule out other conditions
- Blood tests to check for allergies or other underlying issues
Treatment Options for Eczema
Effective eczema management involves a layered approach, often described as rungs on a treatment ladder. This framework allows healthcare providers to start with basic interventions and escalate to more intensive treatments as needed.
First-Line Treatment: Daily Skincare and Home Remedies
For mild to moderate eczema, a comprehensive daily skincare routine often provides sufficient relief. The foundation of home care includes:
- Taking short, lukewarm showers rather than hot baths
- Using gentle, fragrance-free cleansers
- Applying moisturizer immediately after bathing while skin is still damp
- Choosing moisturizers with ceramides, which help restore the skin barrier
- Using cool compresses to soothe inflamed areas
- Avoiding harsh fabrics and wearing soft, breathable clothing
- Keeping fingernails short to minimize damage from scratching
Many people find that following these basic steps consistently significantly reduces eczema symptoms and prevents flare-ups. However, if symptoms persist despite diligent home care, escalation to medical treatments becomes necessary.
Topical Corticosteroids
When over-the-counter measures prove insufficient, dermatologists typically prescribe topical corticosteroids as the next treatment step. These anti-inflammatory medications come in various potencies—gentle formulations for sensitive areas like the face, standard potency for the body, and ultra-potent options for severe flares or thick-skinned areas such as hands and feet.
Topical corticosteroids work by reducing the immune system response that triggers inflammation and itching. They are formulated as creams, ointments, and oils for direct application to affected areas. While highly effective, these medications should be used as directed by your healthcare provider to avoid potential side effects from overuse.
Alternative Topical Treatments
For patients who require more frequent treatment or who develop tolerance to corticosteroids, alternative topical options include:
- Calcineurin inhibitors, which modulate immune response without the side effects of steroids
- Phosphodiesterase-4 (PDE-4) inhibitors, offering targeted anti-inflammatory action
- JAK inhibitors, a newer class of medications that prevent inflammation from within cells
These medications can be used more frequently as part of a maintenance regimen and often work synergistically when combined with topical steroids.
Phototherapy
For moderate to severe eczema that hasn’t responded to topical treatments, phototherapy offers an effective alternative. During phototherapy sessions, patients enter a special booth where controlled doses of ultraviolet B (UVB) light are delivered to affected skin areas. This specialized wavelength of UVB light reduces inflammation and helps keep eczema under control. Treatment typically requires multiple sessions over several weeks.
Systemic Medications
When eczema severely impacts quality of life, sleep, work, or school performance, systemic medications become appropriate. These include:
- Oral corticosteroids for short-term management of severe flares
- Self-injection medications approved for children as young as six months old, administered every other week
- Biologic medications that target specific components of the immune system
These injectable medications focus specifically on the inflammatory pathways involved in eczema without broadly suppressing the entire immune system, making them safer for long-term use.
Choosing the Right Skincare Products
Selecting appropriate skincare products is critical for eczema management. Dermatologists recommend products with simple, minimalist ingredient lists. A good rule of thumb is to avoid products with fragrance, as botanicals used in scented lotions and creams can trigger allergic contact dermatitis in sensitive individuals.
When evaluating skincare products for eczema:
- Look for fragrance-free formulations
- Choose products with minimal ingredients
- Select moisturizers rich in ceramides, which strengthen the skin barrier
- Opt for “healing” creams or ointments with high oil content
- Avoid products containing dyes, alcohol, and strong preservatives
- Patch test new products on a small area before widespread use
It’s important to note that “organic” or “natural” products aren’t automatically better for eczema-prone skin. Some people with eczema develop allergic reactions to natural ingredients, so product choice should be based on individual tolerance rather than marketing claims.
Managing Eczema Triggers
While environmental modifications cannot eliminate eczema, they can significantly reduce flare-up frequency and severity. Key management strategies include:
- Maintaining consistent humidity levels in your home, especially during winter
- Using a humidifier during dry seasons
- Wearing soft, breathable fabrics and avoiding irritating materials
- Stress management through relaxation techniques, exercise, or counseling
- Identifying and avoiding personal allergens
- Maintaining a consistent skincare routine even during symptom-free periods
When to Seek Professional Help
You should consult a dermatologist if:
- Eczema significantly impacts your sleep quality
- Skin becomes infected or develops signs of infection
- Symptoms prevent concentration at work or school
- Home treatments have failed to improve symptoms after several weeks
- Eczema affects your emotional well-being or quality of life
Frequently Asked Questions
Q: Is eczema contagious?
A: No, eczema is not contagious. You cannot contract eczema through physical contact or close proximity with someone who has the condition. It is a personal skin condition determined by genetics and environmental factors.
Q: Can eczema be cured?
A: There is currently no cure for eczema, but it can be effectively managed with proper skincare, appropriate medications, and trigger avoidance. Many people experience significant symptom improvement and extended periods of remission with proper treatment.
Q: What is the best moisturizer for eczema?
A: The best moisturizer is one that works for your individual skin. Look for fragrance-free products with ceramides and minimal ingredients. Greasy ointments often work better than light lotions for eczema-prone skin.
Q: Can stress trigger eczema flare-ups?
A: Yes, stress is a common eczema trigger for many people. Managing stress through relaxation techniques, exercise, and adequate sleep can help reduce flare-up frequency.
Q: At what age does eczema typically develop?
A: Eczema most commonly develops in childhood, often before age five. However, it can develop at any age, including adulthood, and may persist or reappear throughout life.
Q: Are newer eczema treatments better than traditional ones?
A: Newer treatments like JAK inhibitors and biologic medications offer additional options, particularly for severe cases. However, the best treatment varies by individual. Discuss options with your dermatologist to find the most appropriate approach for your specific situation.
References
- How To Choose the Best Eczema Cream — Cleveland Clinic Health. 2024. https://health.clevelandclinic.org/eczema-cream
- Treatment Options for Severe Eczema — Cleveland Clinic Health. 2024. https://health.clevelandclinic.org/severe-eczema-treatment
- Asteatotic (Xerotic) Eczema: Symptoms, Causes & Treatment — Cleveland Clinic. 2022. https://my.clevelandclinic.org/health/diseases/asteatotic-eczema
- Eczema on Face: Symptoms, Causes, Types & Treatment — Cleveland Clinic. 2023. https://my.clevelandclinic.org/health/diseases/24604-eczema-on-face
- Atopic Dermatitis: Symptoms, Causes & Treatment — Cleveland Clinic. 2022. https://my.clevelandclinic.org/health/diseases/24299-atopic-dermatitis
Read full bio of Sneha Tete











