Electrochemotherapy: What It Is, Benefits, And When It Helps
Electrochemotherapy enhances chemotherapy effectiveness using electric pulses for targeted cancer treatment with minimal side effects.
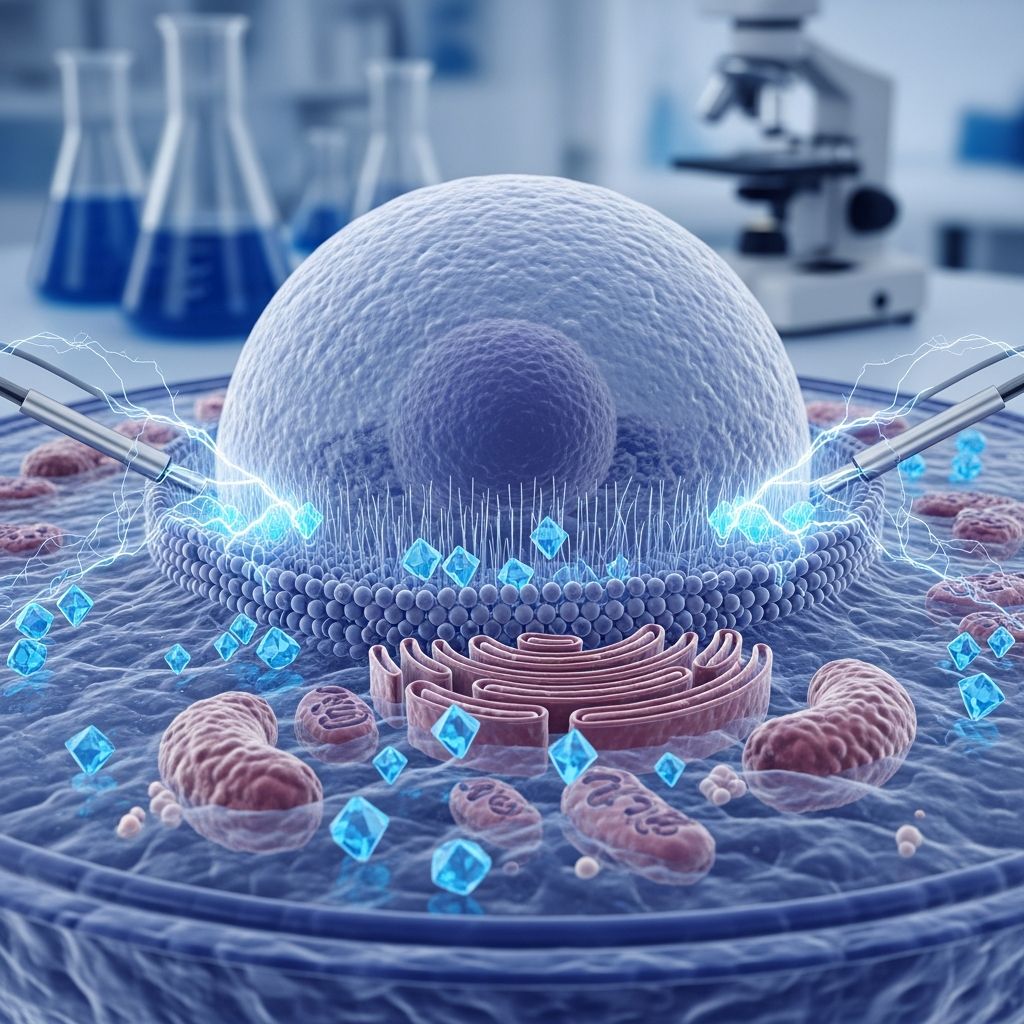
Electrochemotherapy
Author: Reviewed by dermatologists and oncologists
Electrochemotherapy (ECT) is a targeted cancer treatment that combines low doses of chemotherapy drugs with electric pulses to permeabilize cancer cell membranes, dramatically increasing drug uptake and efficacy while minimizing systemic side effects.
What is electrochemotherapy?
Electrochemotherapy is an innovative locoregional therapy designed to treat cutaneous and subcutaneous tumors, as well as metastases. It integrates standard chemotherapeutic agents—most commonly bleomycin or cisplatin—with electroporation, a process where short, high-voltage electric pulses temporarily disrupt cell membranes. This allows hydrophilic drugs that normally struggle to enter cells to achieve intracellular concentrations increased by 80 to 1,000-fold.
The technique is particularly valuable for tumors that are inoperable, resistant to conventional chemotherapy or radiotherapy, or when preserving organ function is critical. By using significantly lower drug doses (often 10-20 times less than standard chemotherapy), ECT reduces toxicity, spares healthy tissues, and improves patient quality of life.
Who is suitable for electrochemotherapy?
ECT is suitable for patients with:
- Primary cutaneous tumors such as melanoma, basal cell carcinoma, and squamous cell carcinoma.
- Metastatic lesions, including breast cancer skin metastases, head and neck cancers, and soft tissue sarcomas.
- Inoperable or recurrent tumors unresponsive to surgery, radiation, or standard chemotherapy.
- Patients seeking organ-sparing treatments, e.g., anal, vulvar, or penile cancers.
- Those with good performance status who can tolerate brief anesthesia or local procedures.
Contraindications include pacemakers (due to electrical pulses), active infections at the treatment site, or severe coagulopathies. Pre-treatment imaging assesses tumor size, depth, and location to ensure electrode accessibility.
How does electrochemotherapy work?
ECT exploits electroporation, where electric fields (typically 1,000–1,500 V/cm for 100 µs pulses) create transient pores in cell membranes. Administered shortly before pulses (5–15 minutes for intravenous bleomycin), the drug floods into cells during this window before membranes reseal, trapping the agent inside to induce apoptosis.
Key mechanism stages:
| Stage | Description | Effect |
|---|---|---|
| Drug Administration | Low-dose bleomycin IV or intratumoral cisplatin | Drug circulates to tumor site |
| Electrode Placement | Needle/array electrodes inserted under imaging guidance | Precise targeting of tumor volume + margin |
| Electric Pulses | 8 pulses of 100 µs at 1.3 kV/cm | Electroporation: 80–1,000x drug uptake |
| Membrane Resealing | Pores close within 5–10 minutes | Drugs trapped; DNA damage/apoptosis |
This localized effect treats not only the tumor core but also a safety margin, reducing recurrence risk.
What are the advantages of electrochemotherapy?
- High efficacy: Objective response rates of 70–100% in cutaneous metastases; complete responses in 40–80% of melanoma lesions.
- Low toxicity: Uses 1/8–1/20 standard chemo doses, minimizing nausea, alopecia, myelosuppression.
- Tissue preservation: Non-surgical; maintains function in critical areas (e.g., eyelids, genitals).
- Versatility: Applicable to irregular tumors via various electrode geometries (needle, plate, endoscopic).
- Repeatable: Safe for multiple sessions if needed.
- Cost-effective: Outpatient procedure, short hospital stays.
Procedure details
Preparation
Patients undergo tumor staging via ultrasound/CT. Bleeding risk is managed with premedication. Treatment occurs under local anesthesia for superficial lesions or brief general anesthesia for deeper tumors.
Treatment delivery
- Drug administration: Bleomycin 15,000 IU/m² IV (8x lower than standard) or cisplatin 1 mg/cm² intratumoral.
- Electrode insertion: Image-guided for precision; computer-controlled pulse generators optimize parameters.
- Pulse application: 8–10 square-wave pulses; patient may feel mild tingling.
- Post-treatment: Wound care; monitoring for 1–2 hours.
Session duration: 15–45 minutes per tumor field.
Drugs used
- Bleomycin: Intravenous; gold standard due to poor natural uptake (electroporation boosts efficacy 300–1,000x).
- Cisplatin: Intratumoral; ideal for superficial lesions.
What to expect after electrochemotherapy
Tumors initially swell (Knutson-Rosenberg effect) within 24–48 hours due to inflammation, peaking at 5–7 days. Ulceration follows as cells die, healing over 4–8 weeks with scarring.
Side effects (mild, localized):
- Pain/swelling at site (managed with paracetamol/ice).
- Skin ulceration (dressings required).
- Rare: Pigmentation changes, infection (<5%).
No significant systemic effects; patients resume normal activities within days.
Results and effectiveness
ECT yields high local control:
| Tumor Type | Complete Response Rate | Reference |
|---|---|---|
| Melanoma metastases | 70–85% | |
| Breast cancer skin mets | 60–80% | |
| Head/neck SCC | 75–90% | |
| Sarcomas | 50–70% |
Combining with immunotherapy or regional perfusion enhances outcomes for visceral metastases.
Electrochemotherapy in veterinary medicine
ECT translates effectively to veterinary oncology, treating canine/feline tumors like mast cell tumors, melanomas, and sarcomas with similar protocols under anesthesia. Low doses minimize toxicity in pets; response rates mirror human data.
Future directions
Ongoing trials explore endoscopic ECT for GI/pancreatic tumors, gene therapy integration, and MDR reversal. Standardization via ESOPE guidelines ensures reproducibility.
Frequently asked questions
What is the difference between chemotherapy and electrochemotherapy?
Standard chemotherapy uses high systemic doses causing widespread toxicity. ECT employs electroporation for 80–1,000x targeted uptake with 1/10th doses, limiting effects to the tumor.
What types of cancer can be treated?
Primarily skin/subcutaneous: melanoma, breast metastases, SCC, sarcomas, carcinomas. Emerging: head/neck, gynecological, colorectal.
Is electrochemotherapy painful?
Local anesthesia eliminates pain during pulses; post-treatment soreness resembles bruising.
How many sessions are needed?
Typically 1–2 per tumor; repeatable every 8 weeks.
Is ECT available worldwide?
Widely in Europe; growing in US/Australia via specialized centers.
References
- Electrochemotherapy ECT for Cancer Patients — Booking Health. 2023. https://bookinghealth.com/blog/oncology/732903-electrochemotherapy-for-cancer-treatment.html
- Electrochemotherapy treatment and side effects — Macmillan Cancer Support. 2024-01-15. https://www.macmillan.org.uk/cancer-information-and-support/treatments-and-drugs/electrochemotherapy
- Electrochemotherapy: A New Cancer Treatment Option — LeadER Veterinary. 2023-06-10. https://leadervet.com/specialties/oncology/electrochemotherapy/
- Electrochemotherapy: technological advancements — PMC (Springer). 2012-11-15. https://pmc.ncbi.nlm.nih.gov/articles/PMC3514699/
- Electrochemotherapy: A New Wave of Cancer Treatment — Vet Specialists. 2024-01-23. https://www.vetspecialists.com/vet-blog-landing/animal-health-articles/2024/01/23/electrochemotherapy-cancer-treatment
- Electrochemotherapy: An Alternative Strategy — PMC. 2022-09-12. https://pmc.ncbi.nlm.nih.gov/articles/PMC9454613/
Read full bio of Sneha Tete