Emphysema: 9 Warning Signs, Causes & Treatments
Understand emphysema: causes, symptoms, diagnosis, treatment, and living with this progressive lung disease affecting millions worldwide.
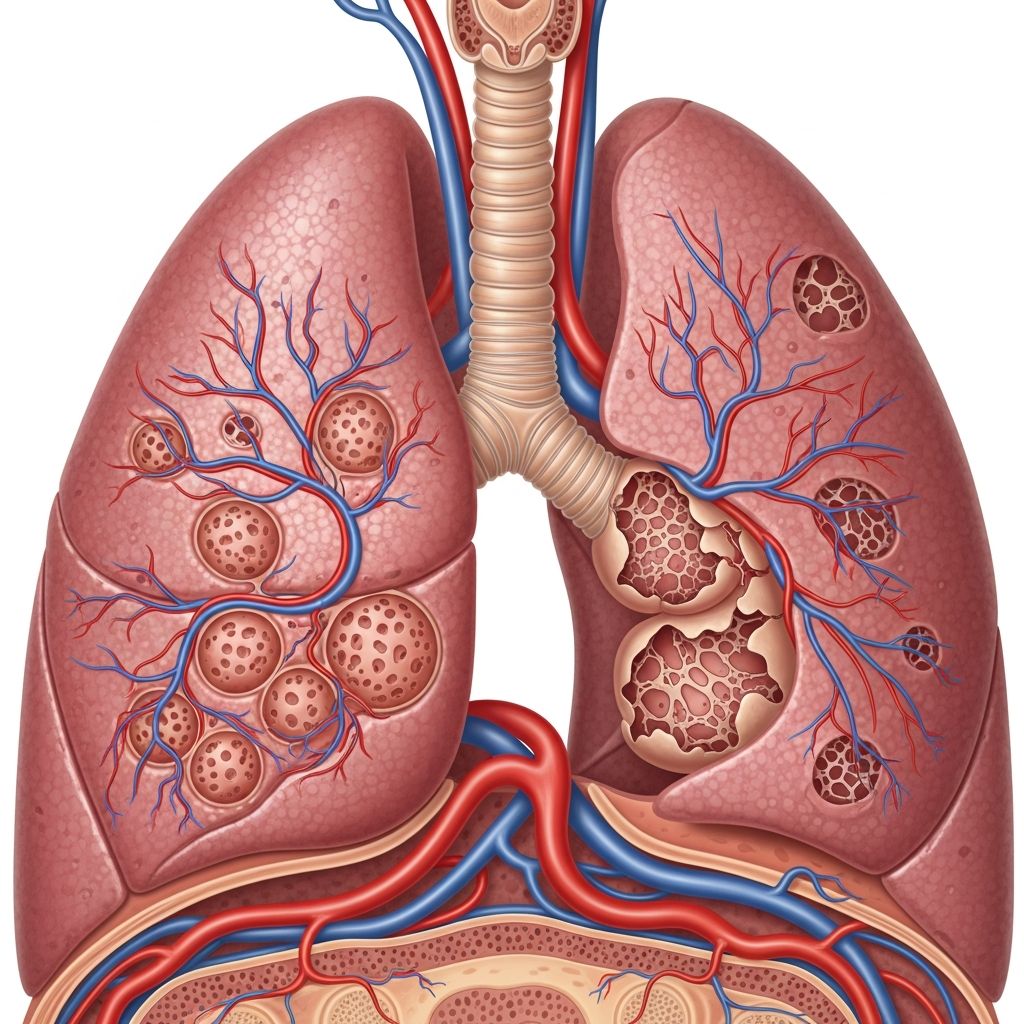
Emphysema Overview
Emphysema is a progressive lung disease and a major form of chronic obstructive pulmonary disease (COPD), characterized by damage to the air sacs (alveoli) in the lungs, leading to shortness of breath and reduced lung function.
What Is Emphysema?
Emphysema involves the abnormal and permanent enlargement of air spaces distal to the terminal bronchiole, accompanied by destruction of their walls without obvious fibrosis, resulting in loss of lung elasticity. This damage reduces the surface area for gas exchange, trapping air in the lungs and impairing oxygen intake and carbon dioxide expulsion.
As part of COPD, emphysema often overlaps with chronic bronchitis, where airways become inflamed and produce excess mucus. Globally, COPD ranks as the third leading cause of death, with emphysema contributing significantly to respiratory symptoms and airflow limitation usually triggered by noxious particles or gases.
The alveoli, tiny sacs resembling bubble wrap bubbles, rupture and merge into larger spaces, shrinking the lungs’ effective surface area and causing a barrel-shaped chest appearance in advanced cases.
Types of Emphysema
Emphysema is classified pathologically by the acinus region affected:
- Centrilobular (proximal acinar) emphysema: Most common, linked to smoking and coal workers’ pneumoconiosis; affects central parts of the acinus.
- Panacinar emphysema: Involves the entire acinus, primarily due to alpha-1 antitrypsin (AAT) deficiency.
- Paraseptal (distal acinar) emphysema: Targets outer acinus regions, often linked to spontaneous pneumothorax in young adults; may combine with other types.
These subtypes influence symptom severity and treatment approaches, with centrilobular being predominant in smokers.
Symptoms of Emphysema
Symptoms develop gradually and may go unnoticed for years. The hallmark is shortness of breath (dyspnea), starting with exertion and progressing to rest.
Common symptoms include:
- Shortness of breath, especially during physical activity or arm work above shoulder level.
- Chronic cough, often with phlegm (sputum) production.
- Wheezing or whistling sounds on exhalation.
- Fatigue and reduced exercise tolerance.
- Chest tightness or heaviness.
- Barrel-shaped chest from lung hyperinflation.
- Cyanosis (bluish skin tint) from oxygen lack in advanced stages.
- Susceptibility to chest infections.
- Weight loss and ankle swelling as the disease worsens.
Progression leads to constant breathlessness, impacting daily activities and quality of life.
Causes and Risk Factors
The primary cause is long-term exposure to irritants damaging lung tissue. Cigarette smoking accounts for most cases, with other contributors including:
- Air pollution, chemical fumes, dust, and workplace pollutants.
- Alpha-1 antitrypsin deficiency, a genetic disorder causing low protective protein levels, leading to early-onset emphysema even in nonsmokers.
- Chronic bronchitis overlap in COPD patients.
Inflammatory responses from macrophages, neutrophils, and T-lymphocytes release proteinases that destroy alveolar walls after irritant exposure. Family history signals genetic risks like AAT deficiency.
Pathophysiology
Damage targets the acinus (respiratory bronchioles, alveolar ducts, sacs, and alveoli). Proteinase-antiproteinase imbalance from inflammation causes permanent airspace dilatation and wall destruction, reducing elasticity and gas exchange efficiency.
Smoking recruits inflammatory cells releasing chemotactic factors like leukotriene B4 and interleukin-8, exacerbating mucus hypersecretion and tissue breakdown. This leads to air trapping, hyperinflation, and ventilation-perfusion mismatch.
Diagnosis
Diagnosis combines history, physical exam, and tests. Patients report progressive dyspnea and cough.
Physical findings: Prolonged exhalation, pursed-lip breathing, barrel chest, reduced breath sounds, wheezing.
Key tests:
| Test | Purpose |
|---|---|
| Spirometry | Measures FEV1/FVC ratio <0.70 confirms obstruction. |
| Chest X-ray/CT scan | Reveals hyperinflation, bullae, paraseptal changes. |
| Alpha-1 antitrypsin level | Tests for genetic deficiency. |
| Arterial blood gas | Assesses oxygenation, CO2 retention. |
| 6-minute walk test | Evaluates exercise capacity. |
Early diagnosis via spirometry is crucial for intervention.
Treatment
No cure exists, but treatments relieve symptoms, slow progression, and improve quality of life. Core strategy: smoking cessation.
Medications:
- Bronchodilators (SABA, LABA, anticholinergics) relax airways.
- Inhaled corticosteroids for frequent exacerbations.
- Phosphodiesterase-4 inhibitors like roflumilast.
- Theophylline as add-on.
Oxygen therapy: For hypoxemia (PaO2 ≤55 mmHg), prolongs survival.
Pulmonary rehabilitation: Exercise, education, nutrition to enhance endurance.
Surgical options: Lung volume reduction surgery (LVRS), bullectomy for giant bullae, lung transplant for end-stage.
Exacerbation management: Antibiotics, systemic steroids, NIV.
Prevention
Preventable through risk factor avoidance:
- Never smoke or quit immediately; avoid secondhand smoke.
- Minimize pollutant exposure with masks in dusty environments.
- Genetic testing and AAT augmentation for deficiency.
- Vaccinations (influenza, pneumococcal) to prevent infections.
- Healthy lifestyle: exercise, balanced diet.
Public health efforts focus on tobacco control.
Living With Emphysema
Manage daily challenges with pulmonary rehab, energy conservation, and support groups. Monitor for exacerbations (worsening dyspnea, sputum changes). Comorbidities like heart disease complicate care. Prognosis varies; GOLD staging guides management.
Complications
Include respiratory failure, cor pulmonale, pneumothorax, frequent infections, and comorbidities (cardiovascular disease, osteoporosis).
Frequently Asked Questions
Is emphysema curable?
No, emphysema is irreversible, but treatments manage symptoms and slow progression.
Can you live a long life with emphysema?
Yes, with smoking cessation, therapy, and lifestyle changes; life expectancy depends on severity and management.
Does emphysema show on X-ray?
Yes, advanced cases show hyperinflation and bullae; CT is more sensitive.
Is emphysema a terminal illness?
It can be end-stage without treatment, but early intervention improves outcomes significantly.
What is the difference between emphysema and COPD?
Emphysema is a subtype of COPD focusing on alveolar destruction; COPD includes chronic bronchitis features.
References
- Emphysema – StatPearls — NCBI Bookshelf. 2023-07-17. https://www.ncbi.nlm.nih.gov/books/NBK482217/
- Emphysema — Better Health Channel, Victoria Government. Accessed 2026. https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/emphysema
- Emphysema – Symptoms and causes — Mayo Clinic. 2023-11-22. https://www.mayoclinic.org/diseases-conditions/emphysema/symptoms-causes/syc-20355555
- Emphysema: Causes, Symptoms, Diagnosis & Treatment — Cleveland Clinic. 2023-09-13. https://my.clevelandclinic.org/health/diseases/9370-emphysema
Read full bio of medha deb











