Endocarditis: Symptoms, Causes & Treatment
Understanding endocarditis: Learn about symptoms, causes, diagnosis, and treatment options for this serious heart infection.
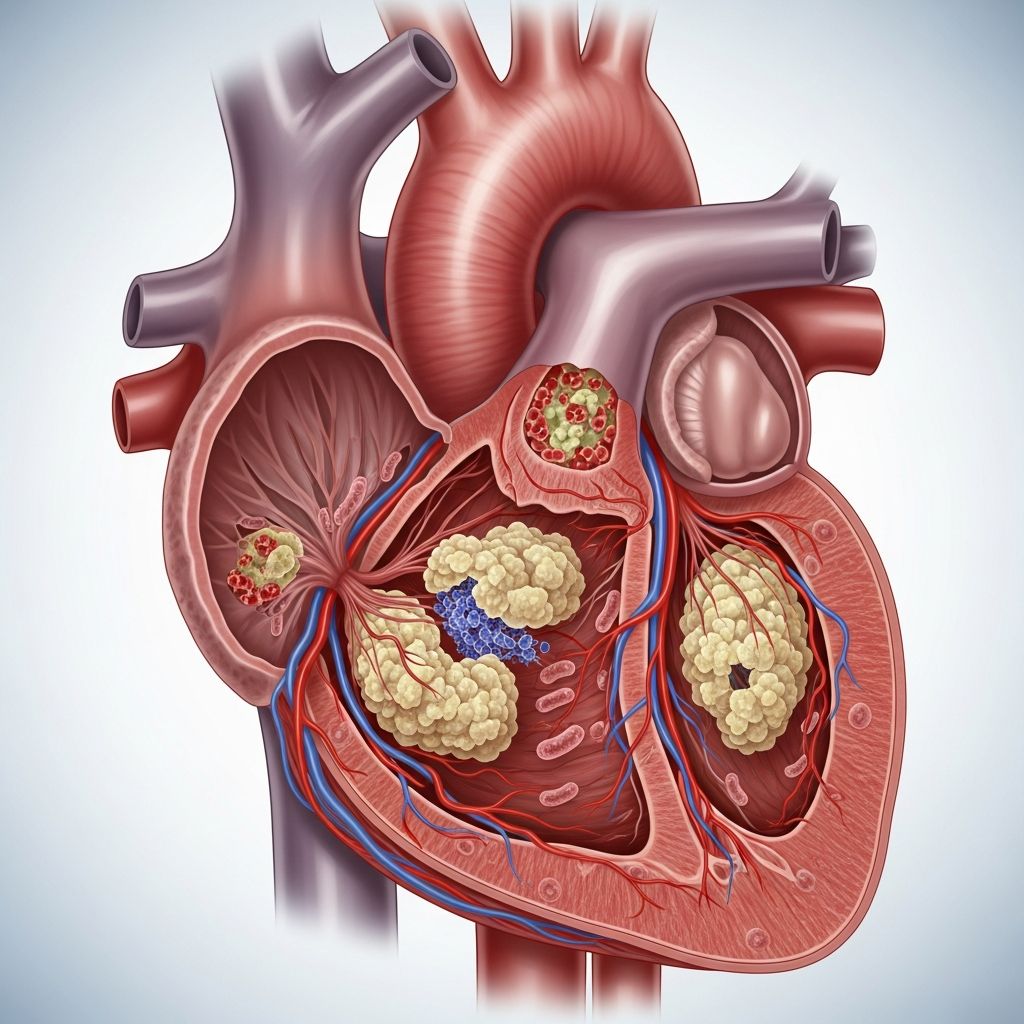
What Is Endocarditis?
Endocarditis is inflammation of the endocardium, which is the inner lining of your heart’s chambers and valves. This serious condition typically develops when bacteria or other microorganisms enter the bloodstream and settle on the heart’s inner surfaces. When bacteria attach to the heart tissue, they can cause infection and damage to the valves and surrounding structures. The infection can develop suddenly (acute endocarditis) or gradually over time (subacute endocarditis), with each presentation carrying different clinical characteristics and treatment requirements.
The condition presents as a systemic disease with complications that affect multiple organ systems, making diagnosis and treatment particularly challenging. Without prompt medical intervention, endocarditis can lead to life-threatening complications and permanent heart damage. Understanding the nature of this infection is critical for recognizing symptoms and seeking appropriate care.
Understanding the Risk Factors
Several conditions and situations increase your risk of developing endocarditis. People with pre-existing heart valve disease, including rheumatic heart disease, mitral valve prolapse, and congenital heart defects, face elevated risk. Additionally, individuals with prosthetic heart valves (artificial replacements) are at higher risk for developing valve infections.
Intravenous drug use represents one of the most significant risk factors for endocarditis. Other important risk factors include recent dental procedures, poor dental hygiene, skin infections, and compromised immune systems. People with certain implanted devices, such as pacemakers and ventricular assist devices, may also develop device-related endocarditis.
Recognizing the Symptoms
Endocarditis symptoms can develop gradually or appear suddenly, depending on the type of infection and organism involved. The most common symptoms include:
- Persistent fever, often irregular and difficult to treat
- Chills and night sweats
- Fatigue and weakness
- Joint and muscle aches
- Shortness of breath
- New or changing heart murmurs
- Chest pain or discomfort
- Swollen feet, legs, or abdomen
- Pale skin
- Red or purple spots on the skin, fingers, or toes
Fever combined with a regurgitant heart murmur, classic vascular skin lesions, and multiple positive blood cultures are virtually diagnostic of endocarditis. Some patients may experience neurological symptoms if infection has caused emboli to travel to the brain, resulting in stroke or other complications.
Diagnosis of Endocarditis
Blood Tests and Cultures
Accurate diagnosis begins with blood cultures, which are essential for identifying the specific microorganism causing the infection. Multiple blood samples are taken to increase the likelihood of detecting the infecting organism. Blood tests also help evaluate kidney function, liver function, and blood cell counts, which may be affected by the infection.
Heart Imaging
Imaging tests play a crucial role in diagnosing endocarditis and assessing cardiac damage. Echocardiography can detect valve lesions and abnormal growths called vegetations on the heart valves. Two types of echocardiography may be used: transthoracic echocardiography (performed through the chest) and transesophageal echocardiography (TEE), which provides more detailed images by passing a probe down the esophagus.
Your provider may also recommend electrocardiogram (ECG) to evaluate the heart’s electrical activity, chest X-rays to assess heart size and pulmonary complications, and advanced imaging such as MRI or CT scans to visualize infection and abscesses around the heart valves.
Complications of Endocarditis
Without proper treatment, endocarditis can cause severe and potentially fatal complications. Understanding these risks underscores the importance of early diagnosis and aggressive treatment.
Valve Damage
The infection can destroy valve tissue, leading to valve regurgitation (leakiness) and subsequent heart failure. Damaged valves may fail to close properly, allowing blood to flow backward through the heart chambers. This hemodynamic abnormality forces the heart to work harder, potentially leading to acute or chronic heart failure.
Embolic Events
Pieces of infected tissue and bacterial growths can break off and travel through the bloodstream as emboli. These emboli can lodge in various organs, causing stroke (when traveling to the brain), kidney infarction, splenic infarction, or pulmonary embolism. Brain emboli represent a particularly serious complication, as they can cause sudden neurological deficits.
Heart Abscess Formation
The infection may create pockets of infected material (abscesses) around the heart valves and myocardium. These abscesses can compromise cardiac structure and function, potentially leading to conduction abnormalities, heart block, and mechanical complications requiring surgical intervention.
Treatment Approaches
Antibiotic Therapy
The cornerstone of endocarditis treatment is antibiotic therapy administered intravenously. Most patients require IV antibiotics for two to eight weeks, with typical treatment lasting up to six weeks, depending on the organism identified and clinical response. Your healthcare provider will perform blood cultures to identify the specific bacteria or fungi responsible for the infection, allowing for targeted antibiotic selection.
Your provider will monitor your symptoms throughout therapy to assess treatment effectiveness and will repeat blood cultures to confirm bacterial clearance. Antibiotic regimens may be adjusted based on culture results and susceptibility testing to ensure optimal outcomes.
Surgical Intervention
When endocarditis damages heart valves or other cardiac structures, surgery may be necessary. Surgical options include valve repair, valve replacement with prosthetic valves, removal of infected tissue (debridement), and drainage of abscesses. Indications for surgery include severe valve dysfunction, persistent infection despite antibiotic therapy, large vegetations with high embolic risk, heart block, and complications such as heart failure or sepsis.
Experienced endocarditis surgeons employ various techniques depending on the valve involved, extent of infection, and presence of complications. Timing of surgery is critical, requiring careful coordination between infectious disease specialists, cardiologists, and cardiothoracic surgeons to balance the risks of surgery against the benefits of infection control and prevention of embolic events.
The Multidisciplinary Treatment Team
Effective endocarditis management requires expertise from multiple medical specialties working collaboratively. A cardiologist establishes the diagnosis, manages heart failure and rhythm problems. An infectious disease specialist selects and monitors appropriate antibiotic therapy. A cardiothoracic surgeon evaluates and performs necessary surgical interventions. Additional specialists may include neurologists to manage stroke and neurological complications, nephrologists to address kidney involvement, and neurosurgeons for severe brain complications.
Prognosis and Survival
Most people survive endocarditis when they receive aggressive, prompt treatment. However, the risk of serious complications or death depends on multiple factors, including the type of infecting organism, patient age, presence of pre-existing heart disease, and speed of diagnosis and treatment initiation. Acute endocarditis with virulent organisms carries higher mortality risk compared to subacute presentations.
Without treatment, endocarditis is a fatal disease. Early evaluation and comprehensive treatment are essential to prevent serious consequences and improve survival outcomes. Long-term follow-up care helps monitor for recurrence and manage residual cardiac dysfunction.
Prevention Strategies
Prevention of endocarditis focuses on reducing bacteremia risk in susceptible individuals. Maintaining excellent dental hygiene and regular dental care helps minimize oral bacterial sources. Prompt treatment of skin and soft tissue infections prevents hematogenous spread. For individuals with high-risk cardiac conditions, antibiotic prophylaxis before certain dental and surgical procedures may be recommended by your healthcare provider.
Avoiding intravenous drug use eliminates a major risk factor for endocarditis. For those with existing cardiac conditions, regular medical follow-up and adherence to treatment recommendations help optimize cardiac health and reduce complication risk.
When to Seek Emergency Care
If you suspect you have active endocarditis, you need immediate evaluation in an emergency room. Symptoms such as persistent unexplained fever combined with a new heart murmur, shortness of breath, chest pain, or neurological symptoms warrant urgent assessment. Early diagnosis dramatically improves treatment outcomes and reduces complication risk.
Living with Endocarditis
Recovery from endocarditis requires patience and adherence to medical recommendations. Completing the full course of antibiotics as prescribed is crucial, even if you begin feeling better. Regular follow-up appointments allow your healthcare team to monitor your recovery and assess cardiac function. Most follow-up occurs at 6 months to 1 year or as needed based on your clinical situation.
If you required surgical intervention, cardiac rehabilitation may help you regain strength and improve exercise tolerance. Addressing modifiable risk factors, such as improving dental hygiene and managing underlying cardiac conditions, helps prevent recurrence. Many patients return to normal activities after appropriate recovery, though some may have permanent cardiac limitations depending on valve damage sustained.
Frequently Asked Questions (FAQs)
Q: Can endocarditis be cured?
A: Yes, endocarditis can be cured with aggressive antibiotic treatment and, when necessary, surgical intervention. Early diagnosis and treatment significantly improve cure rates and reduce complications. Most people who receive prompt, comprehensive care survive and recover from endocarditis.
Q: How long does endocarditis treatment take?
A: Most patients require intravenous antibiotics for two to eight weeks, with typical treatment lasting up to six weeks. The exact duration depends on the organism identified, antibiotic chosen, and clinical response. Some patients may require longer treatment or additional surgical intervention.
Q: Can I get endocarditis more than once?
A: Yes, recurrent endocarditis is possible, particularly in individuals with ongoing risk factors such as intravenous drug use or underlying cardiac conditions. Preventing recurrence involves addressing modifiable risk factors, maintaining good hygiene, and following medical recommendations for prophylactic antibiotics when appropriate.
Q: Is endocarditis contagious?
A: Endocarditis itself is not contagious between people. However, the bacteria or organisms that cause endocarditis may be spread through contact. The infection develops when microorganisms enter the bloodstream and settle on the heart, not through casual contact with infected individuals.
Q: Who needs antibiotic prophylaxis for endocarditis prevention?
A: People with certain high-risk cardiac conditions may benefit from prophylactic antibiotics before dental procedures, surgeries, or other procedures that could introduce bacteria into the bloodstream. Your cardiologist can determine if you need prophylaxis based on your specific cardiac condition and risk factors.
Q: What happens if endocarditis is left untreated?
A: Untreated endocarditis is a fatal disease. Without treatment, the infection progressively damages heart valves, causes embolic stroke, creates heart abscesses, and leads to heart failure and sepsis. This is why early diagnosis and aggressive treatment are absolutely essential.
References
- Endocarditis Center — Cleveland Clinic. 2024. https://my.clevelandclinic.org/departments/heart/depts/endocarditis-center
- AATS Guidelines on Surgery for Infective Endocarditis: Q&A with Dr. Gosta Pettersson — Cleveland Clinic ConsultQD. June 2017. https://consultqd.clevelandclinic.org/aats-guidelines-surgery-infective-endocarditis-qa-dr-gosta-pettersson
- Infective endocarditis: Prevention, diagnosis, treatment, referral — Cleveland Clinic Journal of Medicine, Vol. 67, No. 5. 2000. https://www.ccjm.org/content/ccjom/67/5/353.full.pdf
- Endocarditis: Symptoms, Causes & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/16957-endocarditis
- Diagnosis and management of infective endocarditis — Cleveland Clinic Journal of Medicine, Vol. 57, No. 6. 1990. https://www.ccjm.org/content/ccjom/57/6/558.full.pdf
- Surgery for Infective Endocarditis — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/treatments/17125-infective-endocarditis-surgery
Read full bio of medha deb











