Erythema Ab Igne: Symptoms, Causes, And Treatment Guide
Understanding toasted skin syndrome: causes, symptoms, diagnosis, and management of heat-induced skin changes.
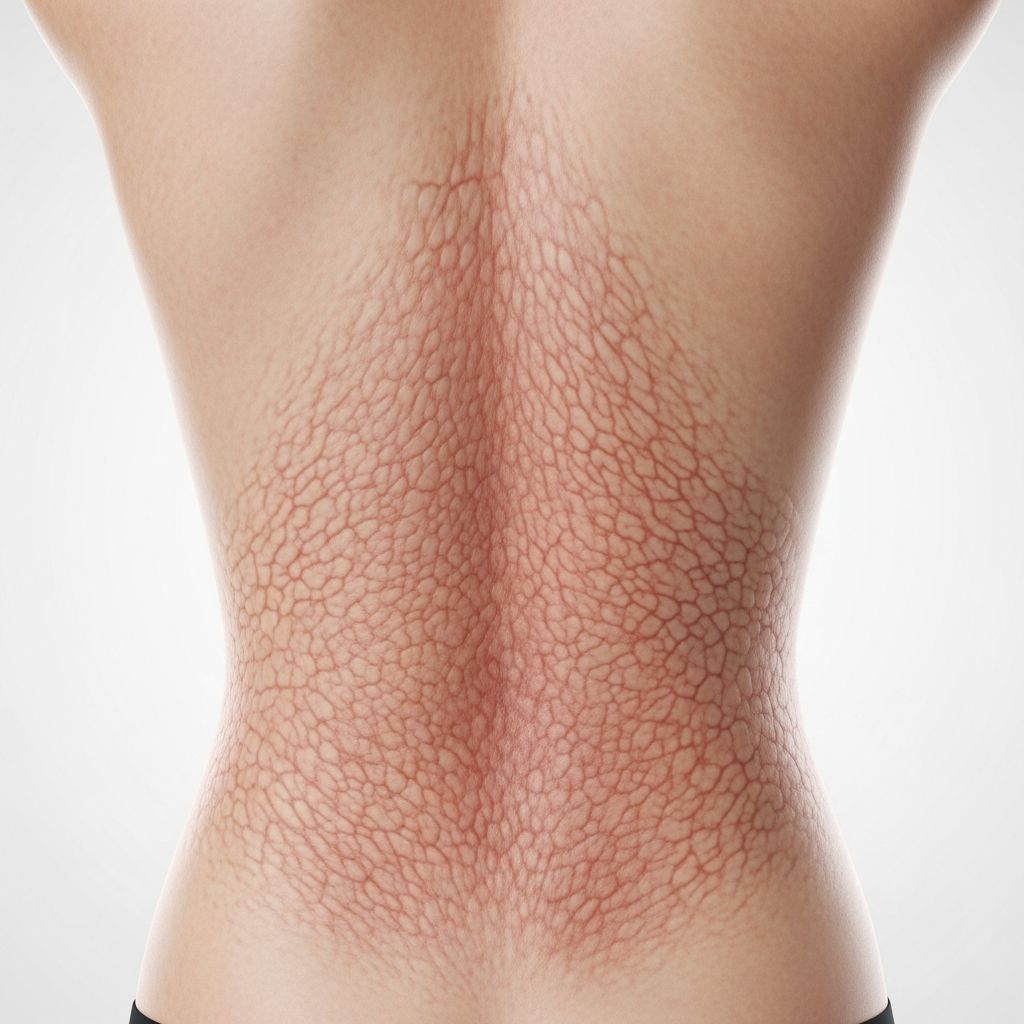
Erythema ab igne
Author: Dermatological Society Revised: January 2026
What is erythema ab igne?
Erythema ab igne (EAI), also known as toasted skin syndrome, fire stains, or livedo reticularis e calore, is a skin condition caused by chronic exposure to moderate heat, typically from infrared radiation sources below the threshold for thermal burns. This dermatosis manifests as localised areas of reticulated (net-like) erythema, hyperpigmentation, and sometimes scaling or telangiectasias on the skin. The term ‘erythema ab igne’ translates from Latin as ‘redness from fire’, reflecting its historical association with open flames or heating devices.
EAI develops gradually over weeks to months or years due to repeated application of heat sources like hot water bottles, heating pads, or laptops directly on the skin. It is benign in most cases but can persist and rarely progress to serious complications such as skin malignancies. Early recognition is crucial, as it often signals underlying chronic pain prompting heat use.
The condition spares deeper tissues but affects the superficial dermis and epidermis, leading to vascular changes and pigment deposition. Prevalence is higher in elderly individuals, those with chronic pain (e.g., back pain, abdominal discomfort), and certain occupations involving heat exposure.
Who gets erythema ab igne?
EAI affects individuals of all ages but is more common in older adults due to increased use of heating devices for pain relief. Risk factors include:
- Chronic pain sufferers using heat therapy for conditions like back pain, pancreatitis, or malignancy-related discomfort.
- Elderly people exposed to space heaters, fireplaces, or heated seats.
- Occupational exposure in bakers, chefs, silversmiths, jewelers, or glassblowers whose skin contacts heat sources.
- Modern causes: laptop use on laps, mobile phones in pockets, or heated car seats.
Women are disproportionately affected due to higher rates of using hot water bottles for abdominal or pelvic pain. No strong genetic predisposition exists, but fair-skinned individuals may show changes more prominently.
What causes erythema ab igne?
EAI results from prolonged exposure to heat sources emitting infrared radiation at temperatures of 43–47°C (109–117°F), insufficient for burns but enough to damage superficial skin structures. Common culprits include:
- Hot water bottles, heating pads, or electric blankets applied repeatedly for pain relief.
- Space heaters, fireplaces, or radiant heaters causing direct skin exposure.
- Heated car seats, recliners, or steering wheels in cold climates.
- Electronic devices like laptops, tablets, or cell phones held against the skin.
- Occupational: ovens, flames, or hot tools in cooking or metalworking.
Typically, exposure lasts 15–30 minutes multiple times daily over weeks. The heat induces vasodilation in dermal vessels, leading to the characteristic reticular pattern mirroring the vascular plexus.
What are the clinical features of erythema ab igne?
EAI evolves in stages:
- Early/Acute Phase (days to weeks): Transient blanchable erythema or mild redness in a net-like pattern, often asymptomatic or with slight warmth/pruritus.
- Subacute Phase (weeks to months): Persistent non-blanching erythema with fine scaling, itchiness, or burning sensation.
- Chronic Phase (months to years): Brownish hyperpigmentation in reticulated distribution, skin atrophy, telangiectasias, and possible bullae or keratoses. Texture becomes dry, thinned, or leathery.
Affected sites correspond to heat source placement: shins/abdomen (hot water bottles), thighs (laptops/heating pads), face/arms (occupational), lower legs (heaters). The rash is usually asymptomatic but may itch or burn. Advanced cases show permanent pigmentation.
| Stage | Features | Duration |
|---|---|---|
| Early | Blanchable erythema, reticular | Weeks |
| Intermediate | Hyperpigmentation, scaling | Months |
| Chronic | Atrophy, telangiectasia, cancer risk | Years |
Diagnosis
Diagnosis is clinical, based on characteristic reticulated hyperpigmentation with a history of heat exposure. Key diagnostic clues:
- History: Repeated use of heat sources on the affected area.
- Examination: Net-like erythema/hyperpigmentation sparing deeper structures.
- Differential Diagnosis: Livedo reticularis, cutis marmorata, erythema nodosum, phytophotodermatitis, or malignancies like mycosis fungoides.
No lab tests are required unless underlying pain etiology is unclear (e.g., imaging for abdominal pain). Skin biopsy, if performed, shows epidermal atrophy, dilated vessels, hemosiderin deposits, and interface changes.
What is the treatment for erythema ab igne?
The cornerstone of treatment is immediate cessation of heat exposure, which halts progression. Outcomes vary:
- Mild erythema: Resolves in 3–12 months spontaneously.
- Hyperpigmentation: May fade slowly over years; persistent cases benefit from topical retinoids (tretinoin), hydroquinone, or 5-fluorouracil cream for precancerous changes.
- Atrophic skin: Unlikely to fully resolve; laser therapy (e.g., Q-switched Nd:YAG) improves cosmesis.
- Suspected malignancy: Biopsy any non-healing ulcers or nodules; monitor for squamous cell carcinoma (SCC) or Merkel cell carcinoma.
Supportive care includes emollients for dryness and sun protection to prevent worsening pigmentation. Address underlying pain with non-heat alternatives like NSAIDs or physical therapy.
Complications
While usually benign, chronic EAI carries risks:
- Skin Cancer: Rare development of SCC or keratoacanthomas within atrophic plaques; Merkel cell carcinoma reported. Biopsy persistent lesions.
- Permanent Changes: Hyperpigmentation, atrophy, scarring.
- Underlying Disease: EAI may indicate occult malignancy or pancreatitis causing pain.
Long-term follow-up is advised for chronic cases, with annual skin exams.
Prevention
Prevent EAI by:
- Avoiding direct skin contact with heat sources; use barriers like towels.
- Limiting exposure time and temperature.
- Using alternative pain relief: medications, TENS units, or acupuncture.
- Educating at-risk groups (elderly, chronic pain patients) about risks.
Frequently asked questions
What does erythema ab igne look like?
Net-like red-brown patches matching heat source shape, evolving from mild redness to pigmented, atrophic skin.
Is erythema ab igne permanent?
Mild cases resolve; chronic pigmentation/atrophy often persists but can improve with treatment.
Can erythema ab igne cause cancer?
Rarely; monitor for non-healing sores and biopsy suspicious changes.
How is erythema ab igne treated?
Stop heat exposure; use topicals/laser for cosmesis.
Who is at risk for toasted skin syndrome?
Chronic pain patients, elderly, heat-exposed workers.
References
- Erythema ab igne — Wikipedia. 2023-10-15. https://en.wikipedia.org/wiki/Erythema_ab_igne
- Erythema ab igne — Cleveland Clinic Journal of Medicine. 2018-02-01. https://www.ccjm.org/content/85/2/96
- Erythema Ab Igne — StatPearls, NCBI Bookshelf. 2023-07-17. https://www.ncbi.nlm.nih.gov/books/NBK538250/
- Erythema Ab Igne — Dermatology Advisor. 2023. https://www.dermatologyadvisor.com/ddi/erythema-ab-igne/
- Erythema ab igne: Toasted Skin Syndrome — HCA Healthcare Journal. 2023. https://scholarlycommons.hcahealthcare.com/cgi/viewcontent.cgi?article=1149&context=hcahealthcarejournal
- Erythema ab igne — DermNet NZ. 2023. https://dermnetnz.org/topics/erythema-ab-igne
Read full bio of Sneha Tete












