Esophagitis: Symptoms, Causes, and Treatment
Understand esophagitis: inflammation of the esophagus causing pain, swallowing difficulties, and potential complications if untreated.
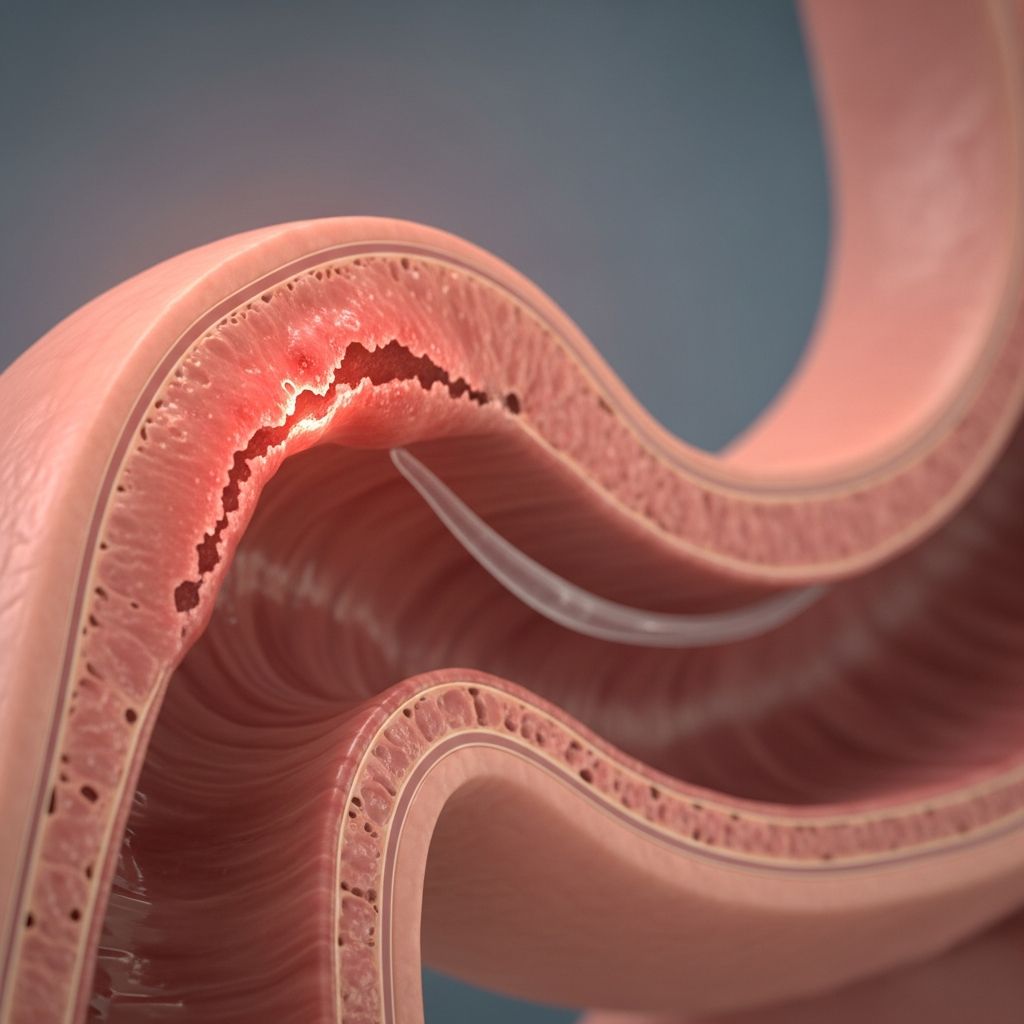
Esophagitis refers to inflammation of the esophagus, the muscular tube that carries food from the throat to the stomach. This condition can cause discomfort ranging from mild soreness to severe pain, often making swallowing difficult. It arises when the esophageal lining becomes irritated by acid, infections, medications, or allergic reactions. Early diagnosis and treatment are crucial to prevent complications like strictures or Barrett’s esophagus.
What Is Esophagitis?
The esophagus is lined with a protective mucous membrane that can become inflamed due to various irritants. Inflammation triggers the immune system to respond, leading to swelling, redness, and potential erosion of tissues. Esophagitis may feel like a raw, burning sensation in the chest or throat, sometimes mimicking heartburn or more serious conditions.
Symptoms often include painful swallowing (odynophagia), difficulty swallowing (dysphagia), and chest pain that may worsen after eating. In severe cases, individuals experience nausea, vomiting, or weight loss due to avoided meals. The condition affects people of all ages but is more common in those with chronic acid reflux or weakened immunity.
Symptoms of Esophagitis
Esophagitis symptoms vary by cause and severity but commonly involve:
- Painful or difficult swallowing: Food or liquids may feel stuck, causing discomfort behind the breastbone.
- Chest pain: A burning or squeezing sensation, often confused with heart issues.
- Heartburn: Frequent acid reflux sensations rising to the throat.
- Nausea and vomiting: Especially if erosion leads to bleeding.
- Hoarseness or sore throat: Due to irritation extending upward.
Pain can be constant or intermittent, mild to severe. Some notice mouth sores or a feeling of food regurgitation. Seek immediate care if symptoms include severe pain, bloody vomit, or black stools, indicating possible bleeding.
Causes of Esophagitis
Esophagitis stems from several mechanisms, categorized into subtypes based on triggers. The esophagus lacks strong protection against stomach acid, making it vulnerable to reflux and other insults.
Reflux Esophagitis (GERD-Related)
The most prevalent type occurs when stomach acid and digestive enzymes reflux into the esophagus due to a weakened lower esophageal sphincter. Frequent heartburn, obesity, pregnancy, or hiatal hernia increase risk. Chronic exposure erodes the mucosa, causing inflammation.
Pill Esophagitis
Certain medications irritate the esophagus if they linger without sufficient liquid. Common culprits include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen.
- Antibiotics such as doxycycline or tetracycline.
- Bisphosphonates (e.g., alendronate for osteoporosis).
- Potassium chloride supplements.
- Quinidine (for heart rhythm issues).
To prevent this, take pills with ample water and remain upright for 30 minutes afterward.
Infectious Esophagitis
Uncommon in healthy individuals, infections thrive in immunocompromised people, such as those with HIV/AIDS, cancer, or on steroids. Fungal (Candida), viral (herpes simplex, cytomegalovirus), or bacterial pathogens spread from elsewhere in the body. Risk factors include diabetes, organ transplants, or chemotherapy.
Eosinophilic Esophagitis (EoE)
This immune-mediated condition involves excessive eosinophils (white blood cells) accumulating in the esophagus, often triggered by food allergens like dairy, wheat, eggs, or soy. It’s chronic, more common in males and those with asthma or allergies. Genetic factors play a role, leading to fibrosis if untreated.
Other Causes
Radiation therapy, caustic ingestions (e.g., lye), or autoimmune diseases like scleroderma can also inflame the esophagus. Smoking, alcohol, and spicy foods exacerbate symptoms.
Diagnosis of Esophagitis
Diagnosis starts with a medical history and physical exam focusing on symptoms and risk factors. Providers may trial acid-suppressing medications; improvement suggests reflux esophagitis.
Confirmatory tests include:
- Upper endoscopy (EGD): A camera examines the esophagus for inflammation, erosions, or strictures. Biopsies rule out infection or EoE.
- Esophageal pH monitoring: Measures acid exposure over 24-48 hours.
- Barium swallow X-ray: Visualizes structural issues like narrowing.
- Allergy testing: For suspected EoE.
These ensure accurate subtyping for targeted therapy.
Treatment for Esophagitis
Treatment addresses the cause while promoting healing. Most cases resolve in 3-6 weeks with proper management.
Lifestyle Modifications
Essential for all types:
- Elevate bed head 6-8 inches.
- Avoid trigger foods (spicy, fatty, caffeine, chocolate, alcohol).
- Eat smaller, frequent meals; no eating 3 hours before bed.
- Lose weight if overweight.
- Quit smoking.
- Stay upright post-meals.
Medications
| Type | Examples | Use |
|---|---|---|
| Proton pump inhibitors (PPIs) | Omeprazole, esomeprazole | Block acid production for reflux esophagitis. |
| H2 blockers | Famotidine, ranitidine | Reduce acid for milder cases. |
| Antacids | Tums, Maalox | Neutralize existing acid. |
| Antifungals/Antivirals | Fluconazole, acyclovir | Treat infections. |
| Steroids | Budesonide slurry | For EoE to reduce inflammation. |
| Prokinetics | Metoclopramide | Strengthen sphincter motility. |
Severe cases may require dilation for strictures.
Advanced Therapies
For refractory GERD: Fundoplication surgery or LINX device. EoE may need elimination diets or biologics like dupilumab.
Complications of Esophagitis
Untreated esophagitis risks:
- Esophageal strictures: Narrowing from scarring, causing obstruction.
- Barrett’s esophagus: Precancerous cell changes.
- Esophageal ulcers/bleeding: Leading to anemia.
- Perforation: Rare tear requiring emergency surgery.
Regular monitoring prevents progression.
Prevention Tips
Minimize risk by:
- Maintaining healthy weight.
- Avoiding late-night eating.
- Taking medications correctly.
- Managing allergies and immunity.
- Using PPIs prophylactically if high-risk.
Annual check-ups for chronic sufferers.
Frequently Asked Questions (FAQs)
What does esophagitis pain feel like?
It often feels like burning chest pain, sore throat, or pain when swallowing, similar to severe heartburn.
Can esophagitis go away on its own?
Mild cases may resolve with lifestyle changes, but most require treatment to heal fully and prevent recurrence.
Is esophagitis the same as GERD?
No, GERD is a cause of reflux esophagitis; not all GERD leads to inflammation.
How long does esophagitis take to heal?
Typically 3-6 weeks with treatment, though chronic forms need ongoing management.
Who is at risk for infectious esophagitis?
Immunocompromised individuals, such as those with HIV, diabetes, or on immunosuppressants.
References
- Esophagitis: What It Is, Symptoms, Causes & Treatment — Cleveland Clinic. 2023-10-12. https://my.clevelandclinic.org/health/diseases/10138-esophagitis
- Esophagitis — Mayo Clinic. 2024-05-15. https://www.mayoclinic.org/diseases-conditions/esophagitis/symptoms-causes/syc-20361224
- Eosinophilic Esophagitis — National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). 2023-08-01. https://www.niddk.nih.gov/health-information/digestive-diseases/eosinophilic-esophagitis
- Gastroesophageal Reflux Disease (GERD) — American College of Gastroenterology. 2022-11-20. https://gi.org/topics/gerd/
Read full bio of medha deb











