Facial Red Vein and Vascular Birthmark Treatments
Effective laser and medical treatments for facial red veins, telangiectasia, and vascular birthmarks like port wine stains.
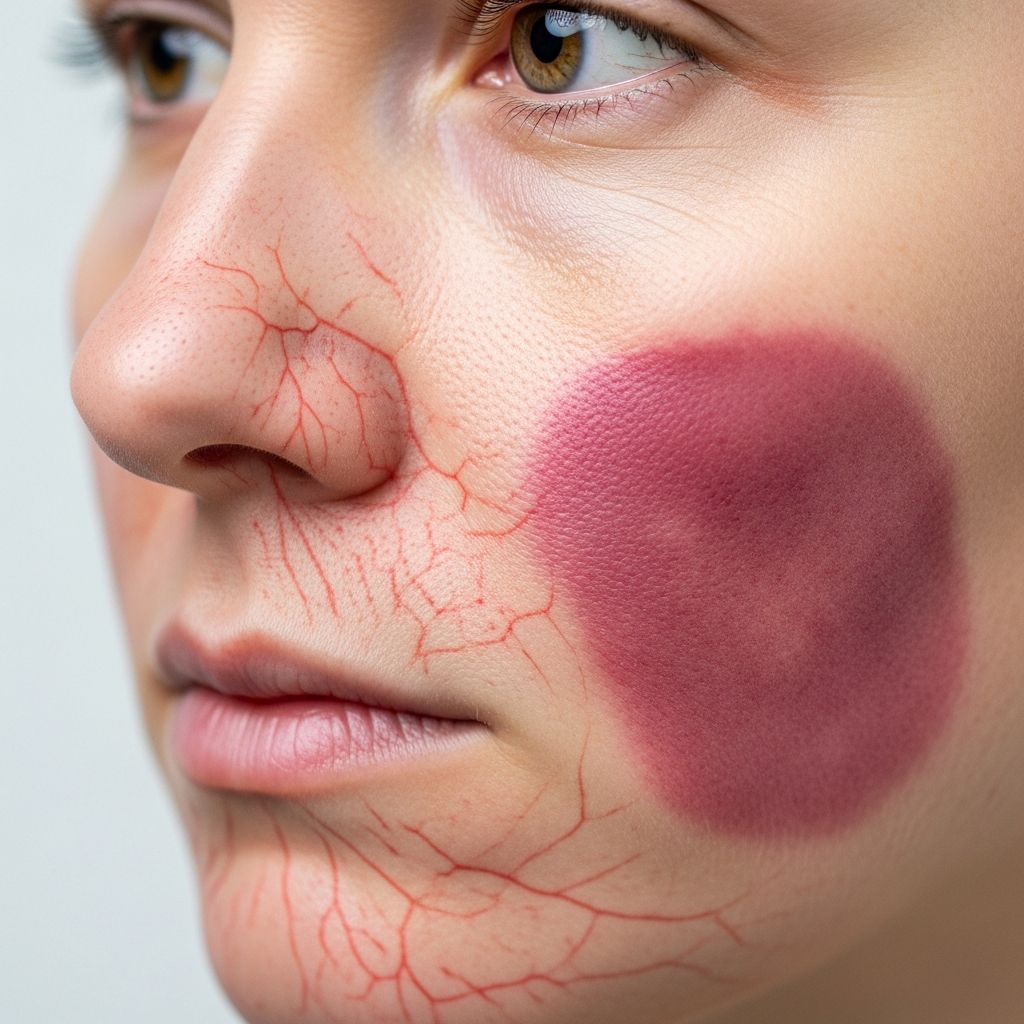
Facial red veins, known as telangiectasia, and vascular birthmarks like port wine stains are common dermatological conditions treatable with advanced laser therapies. These treatments target dilated blood vessels to reduce redness and improve appearance, often requiring multiple sessions for optimal results.
What are they?
Facial red veins or
telangiectasia
are small, dilated blood vessels visible on the skin’s surface, appearing as fine red lines or webs, particularly on the cheeks, nose, and chin. They result from chronic dilation of capillaries and venules near the skin surface.**Vascular birthmarks** include capillary vascular malformations (port wine stains), which are flat, pink to red to purple patches present at birth due to malformed dilated blood vessels. Unlike haemangiomas, which grow and regress, port wine stains persist and may darken over time.
These conditions can affect appearance, causing cosmetic concerns, and in some cases, associate with syndromes like Sturge-Weber or Klippel-Trénaunay.
Who gets them?
Telangiectasia commonly affects fair-skinned individuals, especially women over 30, due to factors like rosacea, sun damage, genetics, or skin aging. They may appear after acne, temperature extremes, or topical steroids.
Port wine stains occur in about 0.3% of newborns, equally in both sexes, often on the face or neck. They grow proportionally with the child and rarely fade spontaneously.
- Hereditary predisposition in fair complexions.
- Sun exposure and rosacea exacerbate telangiectasia.
- Port wine stains linked to GNAQ gene mutations.
What causes them?
Telangiectasia arises from weakened vessel walls due to:
- Acne rosacea or chronic photodamage.
- Hormonal influences, pregnancy, or corticosteroids.
- Genetic factors or trauma.
Port wine stains stem from genetic abnormalities in vascular development, particularly GNAQ mutations on chromosome 9q21, leading to permanent dilation without spontaneous resolution.
What do they look like?
Telangiectasia presents as thin red lines, spider veins, or diffuse redness on the face.
Port wine stains are pink-red patches at birth, potentially thickening or purpling with age, sometimes with nodules.
How are they diagnosed?
Diagnosis is clinical via visual inspection and dermoscopy. For birthmarks, ultrasound confirms vascular nature; MRI or angiography assesses deeper involvement in complex cases.
Treatment of facial red veins
Laser therapy is first-line for telangiectasia and diffuse redness. Key options include:
- Vascular lasers: Nd-YAG laser heats and destroys vessels with minimal surrounding damage.
- Pulsed dye laser (PDL): Targets haemoglobin effectively for superficial veins.
- Intense pulsed light (IPL) and electrosurgery for smaller lesions.
Treatments deliver energy in pulses, often creating temporary circles of lighter skin. 3 sessions typically suffice, repeatable as needed.
Treatment of vascular birthmarks
Port wine stains respond best to
pulsed dye laser (PDL)
, achieving 75% improvement in 40-45% of cases after 5-25 sessions. Early treatment in infancy yields better results before thickening occurs.Other lasers like Nd-YAG treat deeper lesions; V-beam PDL reduces purpura with cooling.
- Infants may need general anesthesia for large areas.
- Limb lesions respond less than facial ones.
- Investigational: Oral sirolimus for severe cases.
What is the treatment technique?
Laser light targets oxyhaemoglobin, coagulating vessels. Dynamic cooling protects skin. Sessions last minutes, spaced 4-8 weeks apart. Initial treatments may show patterned lightening, evening out over time.
| Condition | Laser Type | Sessions Needed | Response Rate |
|---|---|---|---|
| Telangiectasia | Nd-YAG, PDL | 3 | High, repeatable |
| Port Wine Stain | PDL | 5-25 | 40-45% >75% fade |
| Deeper Lesions | Nd-YAG | 4-6 | Improvement, not cure |
Post-treatment care
Avoid sun exposure, makeup, aspirin, or contact sports for 1 week post-treatment to prevent bruising or damage. Use sunscreen; fragile skin may show demarcation lines.
Complications
Common: Temporary redness, bruising, swelling.
Rare: Scarring (more in birthmarks), pigmentation changes (resolve with sun protection, higher risk in darker skin).
- Purpura with older PDL, reduced by V-beam.
- Non-response in resistant cases.
Frequently asked questions
Are facial red veins permanent?
They recur due to ongoing causes like rosacea but laser reduces visibility effectively.
When should port wine stains be treated?
Early, ideally before school age, for best cosmetic outcomes with PDL.
Does treatment hurt?
Mild discomfort like sunburn; numbing creams or anesthesia for children.
Will birthmarks completely disappear?
Improvement common, full clearance less so; multiple sessions needed.
Who performs these treatments?
Dermatologists or specialists in vascular laser centres.
Related topics
- Capillary vascular malformation (port wine stain)
- Lasers and lights in dermatology
- Telangiectasia
- Vascular skin problems
References
- Vascular Laser Treatment — Adelaide Skin and Eye Centre. Accessed 2026. https://asec.net.au/dermatology/vascular-laser-treatment/
- Capillary vascular malformation (red birthmarks, port wine stain) — DermNet NZ. Accessed 2026. https://dermnetnz.org/topics/capillary-vascular-malformation
- Vascular birthmarks — Skin Health Info (BAD Patient Hub). Accessed 2026. https://www.skinhealthinfo.org.uk/condition/vascular-birthmarks/
- Port Wine Stain: Causes, Complications & Treatment — Cleveland Clinic. 2023-10-27. https://my.clevelandclinic.org/health/diseases/24389-port-wine-stain
- Which Kinds of Birthmarks Can be Treated with Lasers? — Celibre Medical. Accessed 2026. https://celibre.com/which-kinds-of-birthmarks-can-be-treated-with-lasers/
- Lasers in dermatology — DermNet NZ. Accessed 2026. https://dermnetnz.org/topics/lasers-in-dermatology
Read full bio of medha deb












