Fatty Liver Disease Symptoms: Key Signs At Every Stage
Recognizing the signs of fatty liver disease early can prevent serious complications like cirrhosis and liver cancer.
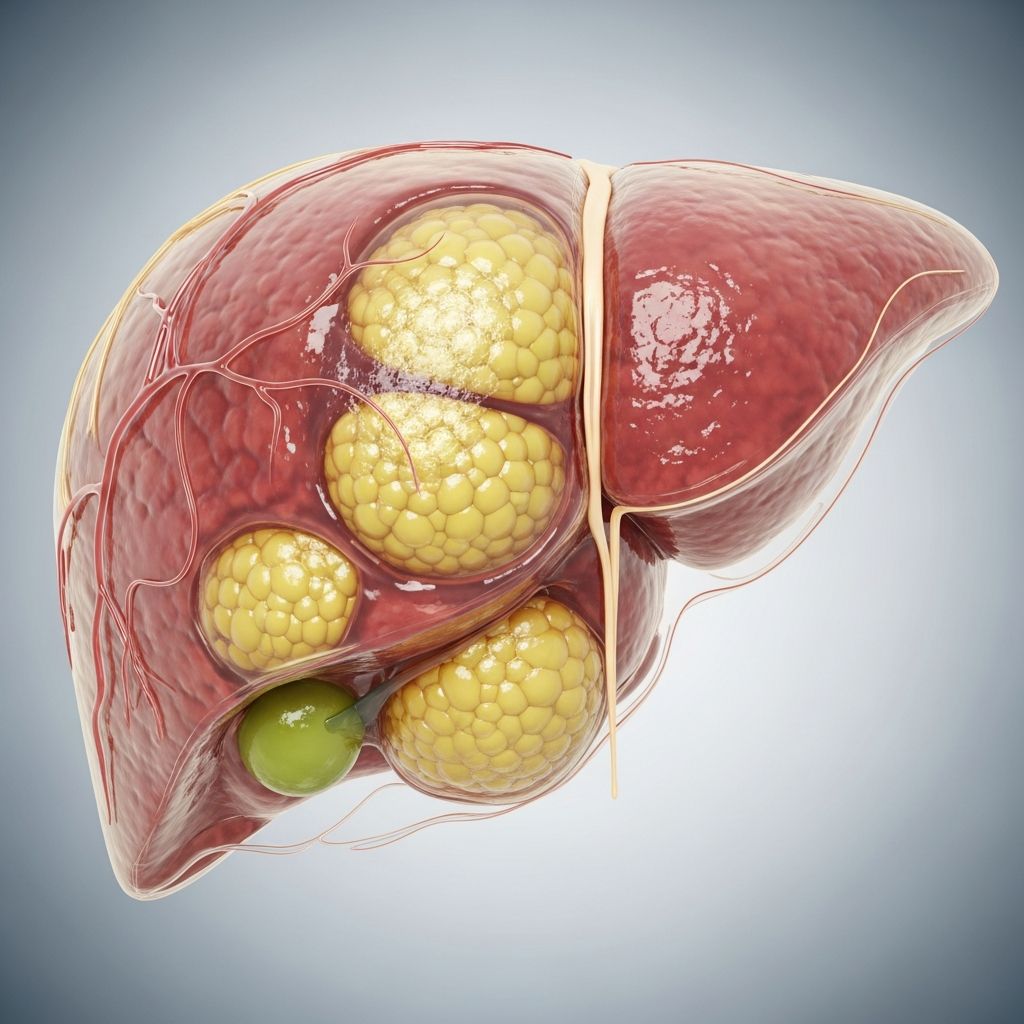
Fatty liver disease, now primarily referred to as metabolic dysfunction-associated steatotic liver disease (MASLD), involves excess fat buildup in the liver and affects millions worldwide, particularly those with obesity or metabolic conditions.
This condition often progresses silently without noticeable signs, but recognizing subtle symptoms early is crucial to prevent advancement to more severe stages like metabolic dysfunction-associated steatohepatitis (MASH), cirrhosis, or liver cancer.
What Is Fatty Liver Disease?
Fatty liver disease occurs when fat accumulates in liver cells, exceeding 5% of the liver’s weight or volume, a condition known as hepatic steatosis. Previously called nonalcoholic fatty liver disease (NAFLD), MASLD is the most common liver disorder globally, driven by rising obesity rates in Western and Middle Eastern populations.
MASLD ranges from simple steatosis, which may not cause harm, to MASH (formerly NASH), involving inflammation and liver cell damage that can lead to fibrosis, cirrhosis, and hepatocellular carcinoma. Another variant, metabolic-associated liver disease (MetALD), incorporates moderate alcohol use alongside metabolic risks.
The liver, the body’s largest internal organ located in the upper right abdomen, filters blood, processes nutrients, and detoxifies substances. Excess fat impairs these functions over time.
Symptoms of Fatty Liver Disease
**MASLD is frequently asymptomatic,** earning its nickname as a ‘silent disease.’ When symptoms appear, they are often vague and include:
- Fatigue: Persistent tiredness or feeling very tired (fatigue), even after rest.
- Malaise: A general sense of not feeling well.
- Right upper quadrant discomfort: Dull pain or ache in the upper right belly, where the liver resides.
In advanced stages like MASH or cirrhosis, symptoms intensify and may include:
- Itchy skin from bile salt buildup.
- Abdominal swelling (ascites) due to fluid accumulation.
- Leg swelling (edema).
- Shortness of breath from fluid around the lungs.
- Spider angiomas: Visible spiderlike blood vessels under the skin.
- Enlarged spleen (hypersplenism).
- Palmar erythema: Reddened palms.
- Jaundice: Yellowing of skin and eyes from bilirubin buildup.
Cirrhosis symptoms can further involve confusion, sleepiness, slurred speech (hepatic encephalopathy), esophageal varices, and end-stage liver failure.
Causes and Risk Factors
Fatty liver disease stems from metabolic dysfunction rather than alcohol in MASLD cases. Key causes include:
- Obesity: Especially abdominal obesity, leading to insulin resistance and fat influx to the liver.
- Type 2 diabetes: High blood sugar promotes fat storage in hepatocytes.
- High cholesterol and triglycerides: Dyslipidemia contributes to lipid accumulation.
- Insulin resistance: Impairs fat metabolism, increasing intrahepatic triglycerides (IHTG).
- Metabolic syndrome: Combination of hypertension, high blood sugar, excess waist fat, and abnormal lipids.
Other risks: Rapid weight loss, certain medications, viral hepatitis, and genetics. For alcoholic fatty liver, heavy drinking (>140g/week women, >210g/week men) is primary. In obese individuals with NAFLD, hepatic de novo lipogenesis (DNL) and visceral fat lipolysis significantly contribute to IHTG.
Stages of Fatty Liver Disease
Fatty liver progresses in stages:
| Stage | Description | Potential Complications |
|---|---|---|
| Simple Steatosis (MASLD) | Fat buildup >5% without inflammation. | Usually benign, but monitor. |
| MASH (formerly NASH) | Fat + inflammation + hepatocyte damage. | Fibrosis, hepatomegaly. |
| Fibrosis | Scarring from ongoing injury. | Progresses to cirrhosis. |
| Cirrhosis | Advanced scarring, liver enlargement/discoloration. | Ascites, varices, cancer, failure. |
Mitochondrial dysfunction and impaired fatty acid oxidation exacerbate progression in NAFLD.
Diagnosis of Fatty Liver Disease
Diagnosis starts with blood tests showing elevated liver enzymes (ALT, AST). Providers check for risk factors during exams, palpating for hepatomegaly or jaundice signs.
Imaging includes:
- Ultrasound: Detects fat (bright liver echo).
- CT/MRI: Quantifies fat.
- FibroScan: Measures stiffness/fibrosis.
Liver biopsy confirms inflammation, fibrosis, or steatosis via histology, though less common due to risks.
Treatment and Management
No FDA-approved drugs specifically for MASLD exist, but management focuses on lifestyle:
- Weight loss: 7-10% body weight reduces fat (diet + exercise).
- Diet: Mediterranean-style, low sugar/fat, high fiber.
- Exercise: 150 min/week aerobic + resistance.
- Control comorbidities: Manage diabetes, lipids with meds like statins, metformin.
- Limit alcohol: Even in MASLD.
Emerging: GLP-1 agonists (e.g., semaglutide) show promise for weight loss and liver fat reduction. For cirrhosis, treat complications.
Prevention Strategies
Prevent MASLD by:
- Maintaining healthy weight (BMI <25).
- Eating balanced diets rich in fruits, veggies, whole grains.
- Exercising regularly.
- Avoiding sugary drinks and processed foods.
- Monitoring metabolic health annually.
Early intervention can reverse steatosis and halt progression.
When to See a Doctor
Seek care if you have risk factors plus fatigue, right upper pain, or abnormal liver tests. Urgent for jaundice, ascites, or confusion.
Frequently Asked Questions (FAQs)
What is the main cause of fatty liver disease?
Metabolic factors like obesity, type 2 diabetes, and insulin resistance are primary causes for MASLD.
Can fatty liver disease be reversed?
Yes, early MASLD often reverses with 7-10% weight loss via diet and exercise.
Does fatty liver always lead to cirrhosis?
No, simple steatosis may not progress, but 20-30% advance to MASH and potential cirrhosis.
Is fatty liver disease linked to liver cancer?
Yes, advanced MASH/cirrhosis increases hepatocellular carcinoma risk.
How is fatty liver diagnosed without biopsy?
Blood tests, ultrasound, and FibroScan suffice for most cases.
Fatty liver disease underscores the importance of metabolic health. Routine check-ups and lifestyle changes are key to safeguarding your liver.
References
- Fatty liver disease (MASLD) – Symptoms and causes — Mayo Clinic. 2023. https://www.mayoclinic.org/diseases-conditions/fatty-liver-disease-masld/symptoms-causes/syc-20354567
- Fatty Liver Disease — MedlinePlus (U.S. National Library of Medicine). 2023. https://medlineplus.gov/fattyliverdisease.html
- Steatotic (Fatty) Liver Disease: Symptoms & Treatment — Cleveland Clinic. 2023. https://my.clevelandclinic.org/health/diseases/15831-fatty-liver-disease
- Obesity and Nonalcoholic Fatty Liver Disease — National Center for Biotechnology Information (PMC). 2013-04-01. https://pmc.ncbi.nlm.nih.gov/articles/PMC3575093/
Read full bio of medha deb











