Folliculitis: Causes, Symptoms, And Treatments Explained
Comprehensive guide to understanding, diagnosing, and treating folliculitis – inflammation of hair follicles.
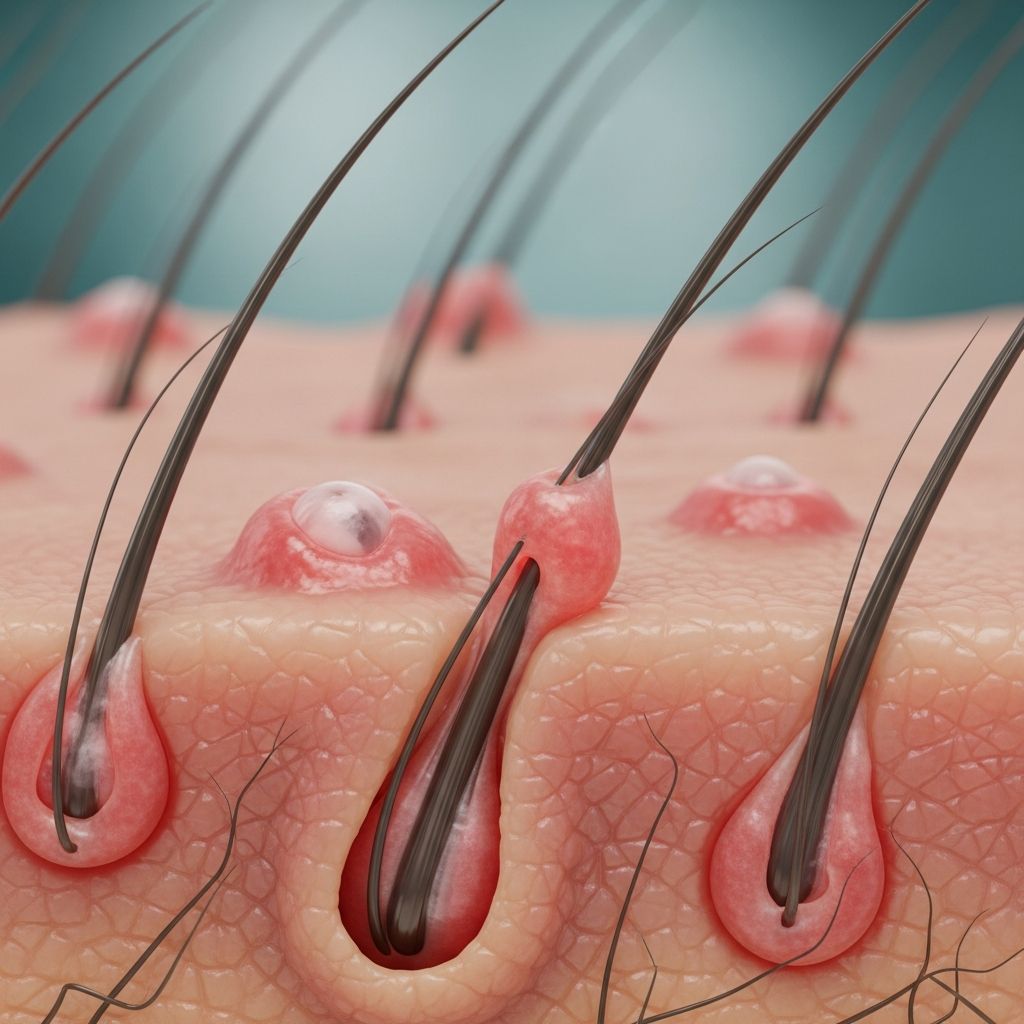
Folliculitis
Folliculitis is a common, generally harmless condition where hair follicles become inflamed, often due to bacterial or fungal infection, friction, or blockage. It manifests as small red bumps or pus-filled pimples around hair follicles, typically on the face, scalp, chest, back, arms, or legs, causing itching, burning, or tenderness.
What is folliculitis?
Folliculitis occurs when hair follicles – the tiny pockets in the skin from which hair grows – become irritated or infected. This inflammation can be superficial, affecting only the upper part of the follicle, or deep, involving the entire follicle and potentially leading to painful nodules or scarring. While most cases are mild and self-limiting, persistent or severe folliculitis may require medical intervention to prevent complications like permanent hair loss or scarring.
The condition is prevalent in areas prone to friction from shaving, tight clothing, or sweating, such as beards, pubic areas, or thighs. It affects people of all ages and skin types but is more noticeable on darker skin tones due to post-inflammatory hyperpigmentation.
Who gets folliculitis?
Folliculitis can affect anyone, but certain groups are at higher risk:
- Individuals who frequently shave, wax, or use depilatory products, leading to razor burn or ingrown hairs.
- People engaging in activities causing sweat and friction, like athletes or those in hot, humid environments.
- Those with compromised immune systems, such as people living with HIV/AIDS, diabetes, or on immunosuppressive drugs.
- Users of hot tubs or public pools exposed to Pseudomonas aeruginosa (hot tub folliculitis).
- Individuals with oily skin or using occlusive cosmetics that trap bacteria.
Children and adults alike can develop it, though bacterial folliculitis is common in adolescents due to shaving practices.
What causes folliculitis?
Folliculitis has infectious and non-infectious causes:
Infectious causes
- Bacterial: Most common is Staphylococcus aureus, entering via cuts or abrasions. Gram-negative bacteria like Pseudomonas cause hot tub folliculitis.
- Fungal: Yeasts like Malassezia (pityrosporum folliculitis) or dermatophytes thrive in warm, moist areas.
- Viral: Rare, from herpes simplex virus.
Non-infectious causes
- Mechanical irritation from shaving, tape, or clothing (pseudofolliculitis barbae).
- Chemical irritation from oils, tar, or adhesives.
- Occlusion by tight clothes or heavy moisturizers.
- Drugs like EGFR inhibitors (sterile folliculitis).
| Type | Cause | Common Sites |
|---|---|---|
| Bacterial | S. aureus | Beard, buttocks, thighs |
| Hot tub | Pseudomonas | Trunk, limbs |
| Pityrosporum | Malassezia yeast | Upper trunk, face |
| Pseudofolliculitis barbae | Shaving irritation | Beard area |
What are the clinical features of folliculitis?
Symptoms appear 1-2 days after triggering factors:
- Small red bumps (papules) or white-headed pimples (pustules) centered around hairs.
- Itching, burning, soreness, or tenderness.
- Pus-filled blisters that may crust or form collarettes of scale.
- In deep forms: painful nodules, abscesses, or furuncles (boils).
- Severe cases: swelling, fever, scarring, or hair loss.
Superficial folliculitis resembles acne; deep forms mimic furunculosis. Hot tub folliculitis is pruritic with symmetric trunk involvement.
Diagnosis
Diagnosis is primarily clinical via history and examination. Key questions include recent shaving, hot tub use, immunosuppression, or recurrence.
For confirmation:
- Skin swab or scraping for microscopy/culture to identify bacteria, fungi, or yeast.
- Biopsy for atypical cases or scarring alopecia.
- Wood lamp or fungal culture for specific infections.
Treatment of folliculitis
Treatment varies by type, severity, and cause. Mild cases often resolve with self-care.
Self-care
- Gently cleanse twice daily with antibacterial soap (e.g., benzoyl peroxide wash).
- Apply warm compresses to drain pustules.
- Use over-the-counter antibiotic ointment or hydrocortisone for itch.
- Avoid irritants: loose clothing, no shaving until healed.
Medical treatments
| Type | Topical | Oral | Other |
|---|---|---|---|
| Bacterial | Mupirocin, clindamycin | Cephalexin, dicloxacillin (severe) | Drainage |
| Fungal | Ketoconazole shampoo/cream | Fluconazole, itraconazole | – |
| Pseudofolliculitis | Topical steroids | – | Laser hair removal |
| Hot tub | – | Ciprofloxacin (if severe) | Self-resolves |
For eosinophilic folliculitis (HIV-associated), antiretroviral therapy or steroids. Recurrent cases may need culture-guided antibiotics or laser therapy.
Complications
- Scarring or cicatricial alopecia.
- Cellulitis or abscess if untreated.
- Post-inflammatory pigmentation.
Prevention of folliculitis
- Maintain hygiene: shower after sweating, dry skin thoroughly.
- Shave properly: use sharp razor, shave with grain, moisturize.
- Avoid sharing razors/towels; clean hot tubs with chlorine.
- Use non-comedogenic products; wear breathable fabrics.
Frequently Asked Questions
Q: Is folliculitis contagious?
A: Bacterial and fungal types can spread via shared items; practice good hygiene.
Q: How long does folliculitis last?
A: Mild cases resolve in 7-10 days; severe may take weeks with treatment.
Q: Can folliculitis cause hair loss?
A: Deep, scarring types can lead to permanent alopecia; seek early treatment.
Q: When to see a doctor for folliculitis?
A: If persistent >2 weeks, worsening, fever, or spreading.
References
- Folliculitis Treatment — Fairview Dermatology. 2023. https://fairviewderm.com/medical-dermatology/folliculitis-treatment/
- Folliculitis – Diagnosis & treatment — Mayo Clinic. 2024-01-15. https://www.mayoclinic.org/diseases-conditions/folliculitis/diagnosis-treatment/drc-20361662
- Best Folliculitis Treatment Near Me — HMGS Dermatology. 2023. https://hmgsderm.com/adult-dermatology/folliculitis/
- Folliculitis — Penn Medicine. 2024. https://www.pennmedicine.org/conditions/folliculitis
- Folliculitis – causes and treatment — healthdirect (Australian Government). 2024. https://www.healthdirect.gov.au/folliculitis
Read full bio of Sneha Tete











