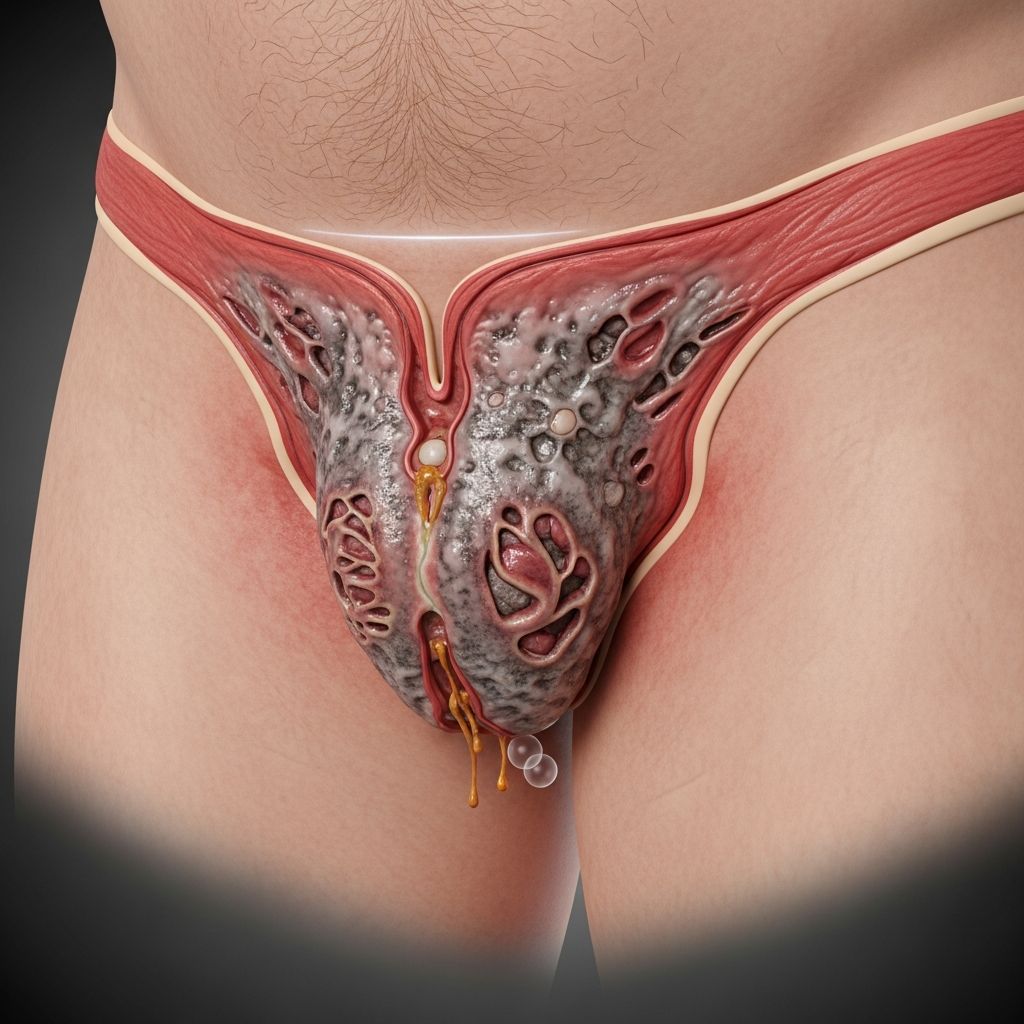
Fournier Gangrene
A life-threatening necrotizing fasciitis of the perineum requiring urgent surgical intervention and antibiotics.
Author: Dermatological Society | Updated: 2025
What is Fournier gangrene?
Fournier gangrene is a rare but aggressive form of necrotizing fasciitis, a rapidly progressive bacterial infection that leads to extensive tissue necrosis in the perineal, genital, and perianal regions. First described by Jean Alfred Fournier in 1883, it affects the subcutaneous tissues and fascia while sparing the underlying muscle in early stages. The infection is polymicrobial, involving both aerobic and anaerobic bacteria, and spreads swiftly along fascial planes, causing thrombosis of blood vessels and subsequent tissue death. Without prompt intervention, it can lead to sepsis, multi-organ failure, and death, with mortality rates historically ranging from 20-40% despite modern treatments.
This condition is considered a urological and surgical emergency, often requiring multidisciplinary management involving urologists, general surgeons, infectious disease specialists, and plastic surgeons. It predominantly affects adults, particularly males aged 50-60, but cases occur in females and children. Risk factors include diabetes mellitus, immunosuppression, obesity, alcoholism, and trauma.
Who gets Fournier gangrene?
Fournier gangrene primarily affects middle-aged to older adults, with a strong male predominance (male-to-female ratio of 10:1) due to the anatomical vulnerability of the scrotum and perineum. Globally, over 1,800 cases have been reported since 1950, though underdiagnosis may occur in resource-limited settings.
Key risk factors include:
- Diabetes mellitus: Present in 40-60% of cases; hyperglycemia impairs immune response and wound healing.
- Immunosuppression: From HIV, chemotherapy, steroids, or organ transplantation.
- Chronic alcoholism: Leads to malnutrition and liver dysfunction.
- Obesity: Promotes skin folds and moisture, fostering bacterial growth.
- Local trauma or procedures: Urethral catheterization, circumcision, perineal abscesses, or colorectal surgery.
- Urinary or gastrointestinal pathology: Diverticulitis, appendicitis, or urinary tract infections.
Women may develop it postpartum or after episiotomy, while pediatric cases are linked to neglect or congenital anomalies.
What causes Fournier gangrene?
The infection typically originates from breaches in the perineal skin or mucosa, allowing entry of endogenous flora. It is polymicrobial, with common pathogens including Escherichia coli, Bacteroides fragilis, Clostridium species, Staphylococcus aureus, Streptococcus species, and anaerobes. Synergistic bacterial action produces toxins, enzymes, and gas, leading to thrombosis, ischemia, and necrosis.
Common portals of entry:
- Perirectal or perianal abscesses (30-40% of cases).
- Urinary tract infections or instrumentation (20-30%).
- Trauma, insect bites, or skin ulcers.
- Colorectal pathology like diverticulitis or cancer.
In 20-30% of cases, no clear source is identified (idiopathic).
What are the clinical features of Fournier gangrene?
| Stage | Symptoms and Signs |
|---|---|
| Prodromal (1-7 days) | Lethargy, malaise, low-grade fever, mild genital discomfort. |
| Acute | Severe pain out of proportion to exam findings, swelling, erythema, warmth in perineum/genitals. |
| Advanced | Dusky/紫色 skin, bullae, crepitus (gas in tissues), foul-smelling discharge, fever, tachycardia, hypotension. |
| Septic | Sepsis, shock, organ failure, exposed testes in males. |
Pain is intense and progressive, often described as throbbing. Crepitus is pathognomonic, felt as subcutaneous emphysema. Systemic signs like tachycardia and fever indicate toxemia. In females, it involves labia and vagina; in males, scrotum and penis.
How is Fournier gangrene diagnosed?
Diagnosis is primarily clinical, based on rapid progression, pain, crepitus, and necrosis in the perineum. High suspicion in at-risk patients with disproportionate pain is key—delays increase mortality.
Investigations:
- Laboratory: Leukocytosis (>15,000/mm³), elevated CRP, lactate, creatinine kinase; metabolic acidosis, thrombocytopenia.
- Imaging: CT shows gas in soft tissues (sensitivity 80-90%), fascial thickening; X-ray for gas; ultrasound limited.
- Cultures: Blood, wound, urine to guide antibiotics.
LRINEC score (Laboratory Risk Indicator for Necrotizing Fasciitis) aids differentiation from cellulitis: score ≥6 suggests high risk (sensitivity 90%). Biopsy confirms but is rarely needed emergently.
What is the treatment of Fournier gangrene?
Treatment is urgent: resuscitation, broad-spectrum IV antibiotics, and surgical debridement. Delay beyond 24 hours doubles mortality.
- Resuscitation: IV fluids, vasopressors for shock, correct electrolytes.
- Antibiotics: Triple therapy: carbapenem (e.g., meropenem) + clindamycin + vancomycin (covers gram+, gram-, anaerobes, inhibits toxin production). Duration 2-4 weeks, tailored by cultures.
- Surgery: Radical debridement of all necrotic tissue, often multiple (daily if needed). Colostomy/orchiectomy if source uncontrolled. Average 3.5 procedures.
- Adjuncts: Hyperbaric oxygen (improves oxygenation, antibacterial), IVIG for toxin mediation.
Post-debridement: wound care, nutrition, vacuum-assisted closure.
Complications of Fournier gangrene
Despite treatment, complications are common:
- Sepsis/multi-organ failure: Leading cause of death.
- Chronic pain: In 50% of survivors.
- Sexual dysfunction: Erectile issues, penile curvature.
- Scarring/amputation: Penectomy, scrotectomy rare with early intervention.
- Psychological impact: Body image distress, PTSD.
What is the outcome for Fournier gangrene?
Mortality is 20-30% with optimal care, higher (50-80%) if delayed. Prognostic factors: age >60, diabetes, sepsis at presentation, LRINEC >8. Survivors require 4-8 weeks hospitalization, reconstructive surgery (skin grafts, flaps) after 2-4 weeks granulation. Long-term: 40% report pain/functional impairment. Prevention: glycemic control, hygiene, prompt abscess treatment.
Investigations for Fournier gangrene
- Blood tests: FBC, U&E, CRP, lactate, ABG, blood cultures.
- Urine culture.
- Imaging: CT pelvis preferred.
- Wound swab for Gram stain/culture.
Management of Fournier gangrene
See treatment section; multidisciplinary in ICU setting.
Prevention of Fournier gangrene
- Diabetes management (HbA1c <7%).
- Hygiene in obese/perineal folds.
- Prompt treatment of UTIs, abscesses.
- Avoid trauma in immunocompromised.
Timeline and progression
Progresses in hours-days: pain → swelling → necrosis → sepsis (24-72 hours untreated).
Patient education
Educate on risks, early symptoms, seek immediate care for perineal pain/swelling.
Frequently Asked Questions
Is Fournier gangrene contagious?
No, it arises from endogenous bacteria, not person-to-person.
Can Fournier gangrene be cured?
Yes, with prompt surgery and antibiotics; survival >70% in treated cases.
How fast does Fournier gangrene spread?
Up to 2-3 cm/hour along fascia.
Does diabetes cause Fournier gangrene?
It predisposes via poor immunity; not direct cause.
Related topics
- Necrotizing fasciitis
- Gangrene
- Perineal abscess
- Diabetic ulcers
References
- Fournier’s Gangrene: Treatment, Symptoms, and More — Healthline. 2023. https://www.healthline.com/health/fourniers-gangrene
- Fournier Gangrene — NORD (National Organization for Rare Disorders). 2024-01-15. https://rarediseases.org/rare-diseases/fournier-gangrene/
- Fournier Gangrene — StatPearls, NCBI Bookshelf. 2024-08-12. https://www.ncbi.nlm.nih.gov/books/NBK549821/
- Gangrene – Symptoms & causes — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/gangrene/symptoms-causes/syc-20352567
- Fournier Gangrene: Causes, Symptoms, Treatment, Prevention — WebMD. 2023. https://www.webmd.com/diabetes/what-is-fourniers-gangrene
Read full bio of Sneha Tete