Gingivitis and Periodontitis: Essential Prevention & Care Guide
Understanding gum inflammation from gingivitis to severe periodontitis: causes, symptoms, risks, and effective treatments.
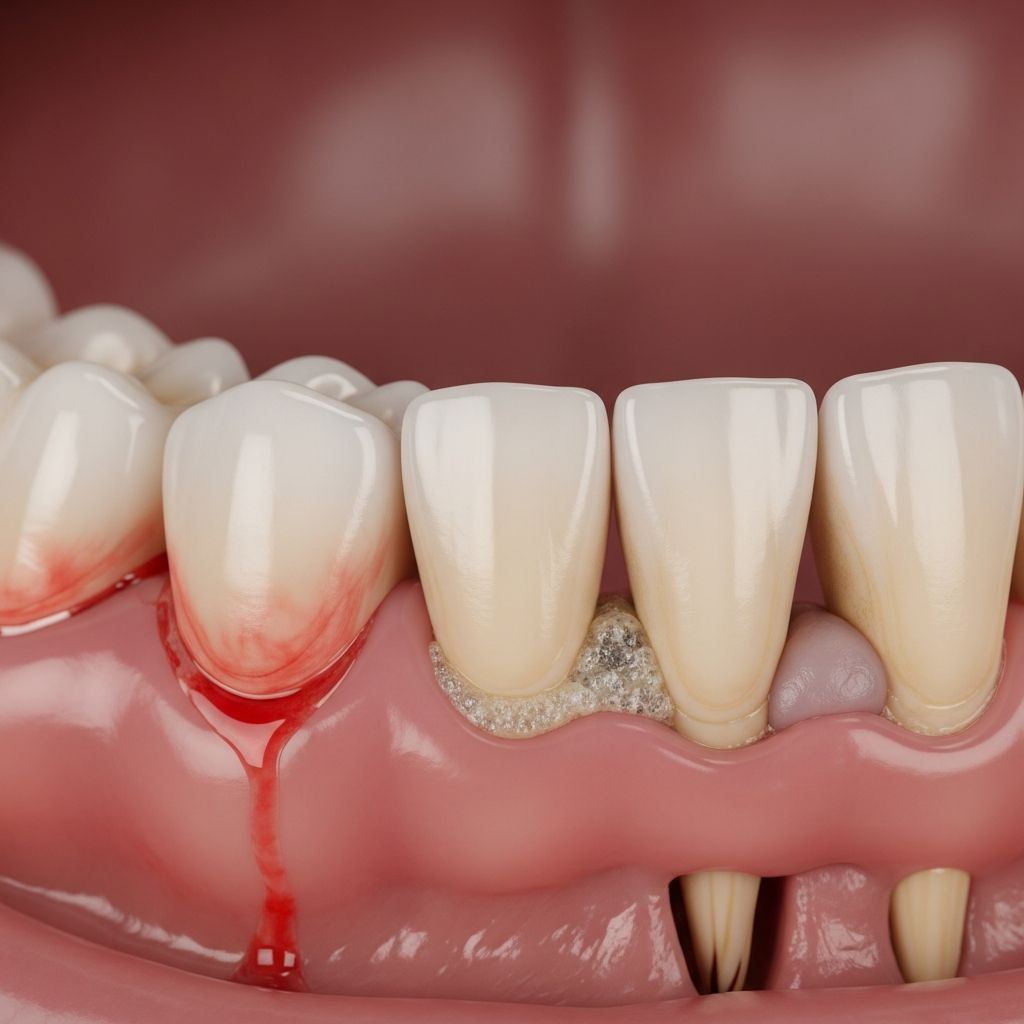
Gingivitis and Periodontitis
Gingivitis is inflammation of the gums (gingiva), the visible mucosa around the teeth. Periodontitis is a chronic, inflammatory disease affecting the gingiva, ligaments, and the underlying alveolar bone, potentially leading to tooth loss if untreated.
Introduction
Gum diseases like gingivitis and periodontitis are among the most prevalent oral health issues worldwide, affecting millions and contributing to systemic health risks. Gingivitis represents an early, reversible stage characterized by gum inflammation due to bacterial accumulation. If ignored, it progresses to periodontitis, involving deeper tissue destruction, pocket formation, and bone resorption. Early intervention is crucial as these conditions are largely preventable through hygiene practices.
These diseases stem primarily from plaque buildup but are influenced by host factors. Globally, severe periodontitis impacts 10-15% of adults, with higher rates in smokers and diabetics. Understanding their progression helps in timely management.
Demographics
Gingivitis affects nearly all individuals at some point, particularly during puberty due to hormonal changes. Periodontitis prevalence increases with age: mild forms in 30-60% of adults over 30, moderate in 7-15%, and severe in about 10%. Men are more affected than women, likely due to poorer hygiene and higher smoking rates. Socioeconomic factors play a role, with higher incidence in lower-income groups due to limited dental access.
- Children: Gingivitis is common but rarely progresses to periodontitis pre-puberty.
- Adults: Peak periodontitis onset in 30-50 age group.
- Elderly: Up to 50% have attachment loss >4mm.
Risk is elevated in developing countries due to malnutrition and poor hygiene.
Causes
The primary cause of both conditions is dental plaque, a biofilm of bacteria on teeth. Poor oral hygiene allows plaque to mineralize into tartar (calculus), irritating gums.
Gingivitis Causes
- Bacterial plaque accumulation from inadequate brushing/flossing.
- Hormonal fluctuations (pregnancy, puberty).
- Medications (e.g., anticonvulsants, immunosuppressants).
- Systemic diseases (e.g., diabetes, vitamin C deficiency).
Gingivitis is reversible upon plaque removal.
Periodontitis Causes
Tartar buildup forms periodontal pockets filled with bacteria, leading to chronic infection. Key pathogens include Porphyromonas gingivalis, Tannerella forsythia, and Treponema denticola. Progression involves host immune response destroying supporting structures.
Risk Factors
Beyond plaque, modifiable and non-modifiable factors increase susceptibility:
- Poor oral hygiene: Primary driver.
- Smoking/tobacco use: Doubles periodontitis risk by impairing immunity.
- Diabetes: Poor glycemic control worsens severity.
- Genetics: Familial aggregation noted.
- Obesity, stress, poor diet: Contribute via inflammation.
- Immunosuppression (HIV, chemotherapy): Predisposes to necrotizing forms.
Children in malnourished populations face higher necrotizing risks.
Clinical Features
Gingivitis
Often asymptomatic early on, but progresses to:
- Red, swollen, shiny gums.
- Bleeding on brushing/probing.
- Bad breath (halitosis).
- No bone/attachment loss.
Localized (around specific teeth) or generalized.
Periodontitis
Advanced signs include:
- Persistent bleeding gums.
- Gum recession (“long teeth”).
- Deep periodontal pockets (>4mm).
- Tooth mobility, drifting.
- Pus discharge, pain on chewing.
- Abscesses, bone loss on x-rays.
Symptoms may be absent until advanced.
Complications
Untreated gingivitis leads to periodontitis. Periodontitis complications:
- Tooth loss: Due to bone/support loss.
- Systemic links: Increased cardiovascular disease, diabetes complications, rheumatoid arthritis, preterm birth risks. Mechanisms involve bacteremia and chronic inflammation.
- Necrotizing forms: Rapid tissue death in immunocompromised.
- Halitosis, aesthetic issues.
Links to chronic conditions are associative, not fully causal.
Diagnosis
Clinical exam is cornerstone:
- Visual inspection of gums/teeth.
- Periodontal probing for pocket depths (normal <3mm).
- Attachment loss measurement.
- Bleeding index.
- Radiographs for bone loss.
No lab tests routine; cultures for refractory cases. Staging: I-IV based on severity, extent, complexity.
| Parameter | Gingivitis | Periodontitis |
|---|---|---|
| Pocket Depth | <4mm | >4mm |
| Bone Loss | None | Present |
| Attachment Loss | None | Present |
Treatment
Gingivitis
- Professional scaling/polishing.
- Enhanced home care: brushing 2x/day, flossing, antiseptics (chlorhexidine).
- Address causes (e.g., stop smoking).
Resolution in days-weeks.
Periodontitis
Multistage:
- Nonsurgical: Scaling/root planing to remove subgingival deposits. Adjuncts: antibiotics, lasers.
- Surgical: Flap surgery, grafts for pockets >5mm, regeneration.
- Maintenance: 3-6 monthly recalls.
Systemic antibiotics for aggressive cases. Treat underlying conditions.
For necrotizing: Debridement, pain relief, antibiotics (metronidazole).
Prevention
- Daily brushing (soft brush, fluoride paste), flossing/interdental aids.
- Regular dental visits (6-12 months).
- Balanced diet, no smoking, diabetes control.
- Antiseptic mouthwashes.
Plaque control prevents 80% cases.
Frequently Asked Questions (FAQs)
Q: Can gingivitis be reversed?
A: Yes, with improved hygiene and professional cleaning, gingivitis resolves quickly without permanent damage.
Q: Does periodontitis always cause tooth loss?
A: Not always if treated early, but advanced cases risk loss; maintenance prevents progression.
Q: Is smoking the worst risk factor?
A: Smoking significantly worsens outcomes and healing; quitting is vital.
Q: How often should I see a dentist?
A: Twice yearly, or more for high-risk individuals.
Q: Can diabetes cause gum disease?
A: Diabetes impairs immunity, increasing susceptibility; control both conditions.
This comprehensive overview emphasizes prevention’s role in averting progression from gingivitis to debilitating periodontitis. Consult professionals for personalized advice.
References
- Gingivitis and Periodontitis — DermNet NZ. 2023. https://dermnetnz.org/topics/gingivitis-and-periodontitis
- Necrotising Periodontal Disease — DermNet NZ. 2023. https://dermnetnz.org/topics/necrotising-periodontal-disease
- Pathogenesis of Gingivitis and Periodontal Disease in Children — American Academy of Pediatric Dentistry. 2003. https://www.aapd.org/globalassets/media/publications/archives/ranney-03-s1.pdf
- Overview: Gingivitis and Periodontitis — NCBI Bookshelf (InformedHealth.org). 2023. https://www.ncbi.nlm.nih.gov/books/NBK279593/
Read full bio of Sneha Tete