Gingivitis: Symptoms, Causes, Treatment, Prevention Guide
Understand gingivitis symptoms, causes, treatments, and prevention to protect your gums and avoid serious dental issues.
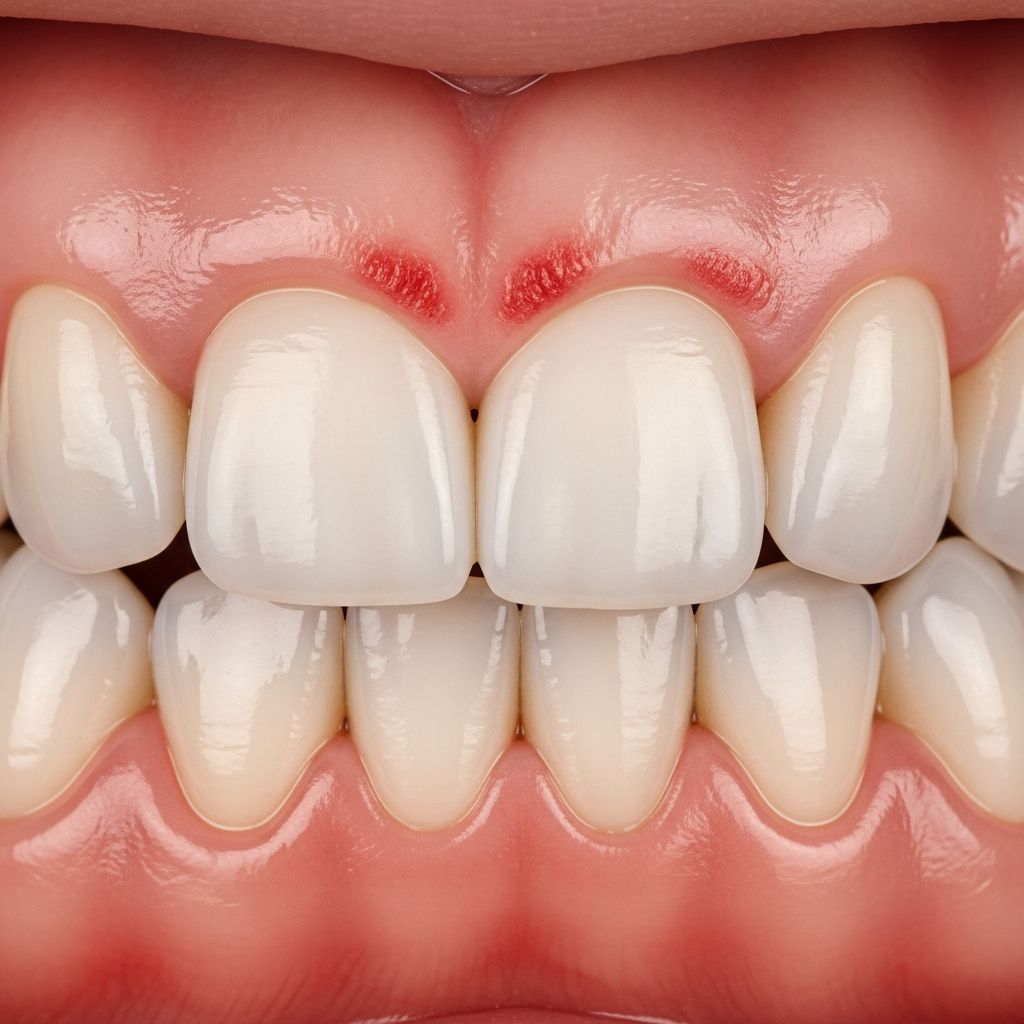
Gingivitis Overview
Gingivitis is the earliest and most common form of gum disease, characterized by inflammation of the gums due to bacterial plaque buildup. It is reversible with proper care but can progress to periodontitis if ignored.
What Is Gingivitis?
Gingivitis, a mild form of periodontal disease, affects the soft tissues surrounding the teeth. It occurs when plaque—a sticky film of bacteria—accumulates along the gumline, triggering an inflammatory response. Healthy gums are firm and pale pink, fitting snugly around teeth; in gingivitis, they become red, swollen, and prone to bleeding.
This condition impacts nearly half of adults over 30 and is often painless in early stages, making it easy to overlook. Unlike advanced gum disease, gingivitis does not involve bone loss, but prompt intervention is crucial to prevent escalation.
Symptoms of Gingivitis
Early gingivitis symptoms are subtle but progressive. Common signs include:
- Bright red, dark red, or purplish gums that appear darker than usual.
- Swollen or puffy gums that feel tender to the touch.
- Gums that bleed easily during brushing, flossing, or even spontaneously.
- Bad breath (halitosis) persisting despite oral hygiene efforts.
- A shiny gum surface or receding appearance in mild cases.
These symptoms often develop gradually over weeks or months. Regular dental checkups can detect gingivitis before noticeable changes occur.
Causes of Gingivitis
Plaque formation is the primary cause of gingivitis. After consuming sugary or starchy foods, bacteria in the mouth produce acids that form this colorless biofilm on teeth. If not removed within 24-48 hours via brushing and flossing, plaque hardens into tartar (calculus) below the gumline, harboring more bacteria and irritating gums.
Key contributing factors include:
- Poor oral hygiene: Inadequate brushing (twice daily for two minutes) or flossing allows plaque persistence.
- Tobacco use: Smoking or chewing tobacco impairs blood flow to gums, reducing healing capacity.
- Improper brushing/flossing techniques: Missing gumlines leaves plaque untouched.
- Misaligned teeth or ill-fitting dental appliances: Creates hard-to-clean areas.
- Hormonal changes: Pregnancy, puberty, or menopause increases gum sensitivity.
- Medications: Dry mouth from drugs like antihistamines reduces saliva’s protective effects.
While bacteria causing gingivitis can spread via saliva, the condition itself is not directly contagious; poor hygiene amplifies risk.
Risk Factors for Gingivitis
Certain factors elevate susceptibility:
- Diabetes: High blood sugar promotes bacterial growth and impairs immunity.
- Genetic predisposition: Some inherit thinner gums or aggressive plaque responses.
- Compromised immunity: Conditions like HIV, leukemia, or cancer treatments weaken defenses.
- Poor nutrition: Vitamin C deficiency hinders gum tissue repair.
- Stress: Elevates cortisol, suppressing oral immunity.
Addressing these through lifestyle changes and professional care significantly lowers incidence.
How Is Gingivitis Diagnosed?
Dentists diagnose gingivitis via clinical exams during routine visits. Key methods include:
- Visual inspection: Checking for redness, swelling, or shine.
- Periodontal probing: Measuring pocket depths between teeth and gums (healthy: 1-3mm; gingivitis: 4mm+).
- Dental X-rays: Rule out bone loss indicating periodontitis.
- Medical history review: Assessing risk factors like medications or smoking.
Early diagnosis is straightforward and non-invasive, often during six-month cleanings.
Treatment for Gingivitis
Gingivitis is fully reversible in its early stage with diligent home care and professional intervention. Nonsurgical treatments include:
- Professional cleaning (scaling): Removes plaque and tartar above/below gumline.
- Root planing: Smooths roots to deter bacterial reattachment.
- Antimicrobial rinses: Prescription chlorhexidine reduces bacteria.
- Antibiotics: Topical gels or oral for severe cases.
Improvements appear within 1-2 weeks of consistent care. Surgery is rare for gingivitis alone.
Prevention and Management Tips
Prevent gingivitis through daily habits:
- Brush twice daily with fluoride toothpaste using a soft-bristled brush at a 45-degree angle.
- Floss daily to clear interdental plaque.
- Use antimicrobial mouthwash (e.g., with essential oils).
- Eat a balanced diet low in sugars; stay hydrated.
- Avoid tobacco; manage chronic conditions like diabetes.
- Visit dentist every 6 months for cleanings.
| Daily Routine | Frequency | Purpose |
|---|---|---|
| Brushing | 2x/day, 2 min | Remove plaque from surfaces |
| Flossing | 1x/day | Clean between teeth |
| Mouthwash | 2x/day | Kill lingering bacteria |
| Dental visits | Every 6 months | Professional removal of tartar |
Complications: Gingivitis vs. Periodontitis
Untreated gingivitis advances to periodontitis in 3-4 stages:
- Early Periodontitis: Pockets deepen (4-5mm); gums recede.
- Moderate: Bone loss begins; pus, pain, bad breath intensify.
- Advanced: Severe bone/tissue destruction; tooth loss.
Periodontitis is irreversible, linking to heart disease, stroke, diabetes complications, and respiratory issues.
Frequently Asked Questions (FAQs)
What does gingivitis look like?
Gingivitis appears as red, swollen gums that bleed easily, often shiny and tender.
Can gingivitis be reversed?
Yes, with improved hygiene and professional cleaning, gums heal within weeks.
Is gingivitis contagious?
Bacteria can spread via saliva, but poor hygiene is the main trigger—not casually contagious.
How long before gingivitis turns into periodontitis?
Weeks to years, depending on care; early treatment halts progression.
Can you have gingivitis without knowing?
Yes, early stages are often painless and symptom-light.
Special Considerations
Pregnancy Gingivitis: Affects 60-75% due to hormones; extra cleanings help.
Trench Mouth (NUG): Rare severe form with ulcers, fever; requires antibiotics.
Children and seniors face higher risks from braces or dry mouth.
References
- What Is Gum Disease: Gingivitis vs Periodontitis Signs & Prevention — Listerine. 2023. https://www.listerine.com/gum-disease-healthy-gums/what-is-gum-disease
- Gingivitis: Symptoms & How To Treat It — Cleveland Clinic. 2023-10-12. https://my.clevelandclinic.org/health/diseases/10950-gingivitis-and-periodontal-disease-gum-disease
- Gingivitis – Symptoms and causes — Mayo Clinic. 2023-11-08. https://www.mayoclinic.org/diseases-conditions/gingivitis/symptoms-causes/syc-20354453
- Overview: Gingivitis and periodontitis — NCBI InformedHealth.org. 2023. https://www.ncbi.nlm.nih.gov/books/NBK279593/
Read full bio of Sneha Tete











