Granuloma Gluteale Infantum: Diagnosis And Treatment Guide
Rare napkin dermatitis in infants causing reddish-purple nodules in diaper area due to irritation.
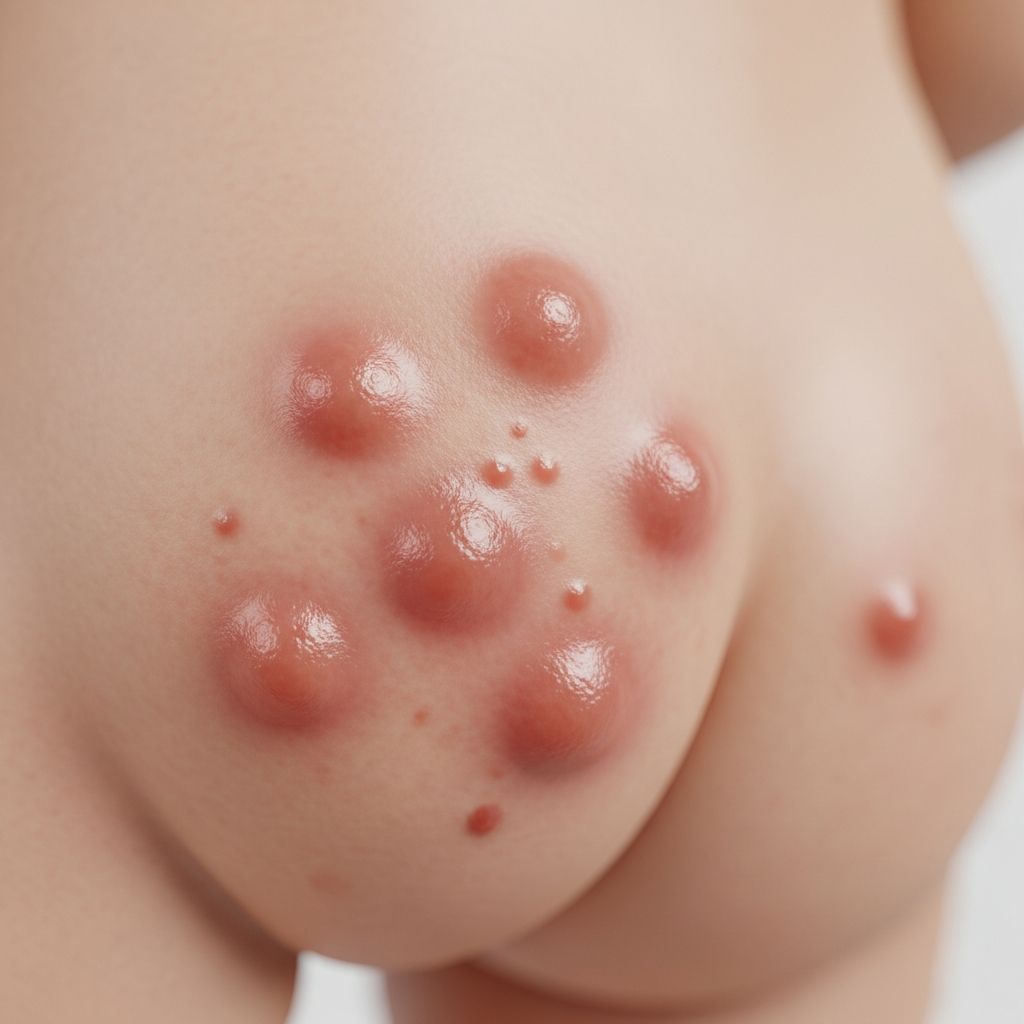
Granuloma Gluteale Infantum
Granuloma gluteale infantum is a rare cutaneous condition characterized by the development of reddish-purple nodules in the diaper area of infants, typically arising as a complication of irritant contact dermatitis or napkin dermatitis. First described in 1891 as ‘vegetating bromidism’ due to its association with bromide-containing ointments, this condition remains uncommon but distinctive in pediatric dermatology. It primarily affects infants during their first year of life, presenting challenges in management due to its resistance to standard diaper rash treatments.
Introduction
Granuloma gluteale infantum manifests in the anogenital region as multiple asymptomatic, firm, erythematous or violaceous nodules amid primary irritant contact dermatitis. The condition is often overlooked, especially when it follows the misuse of topical treatments for initial diaper rashes. Understanding its etiology, clinical presentation, and management is crucial for dermatologists and pediatricians to avoid unnecessary interventions and promote healing. This article synthesizes key insights from clinical reports and reviews to provide comprehensive guidance on this underrecognized entity.
Demographics
Granuloma gluteale infantum predominantly occurs in infancy, with the average age of onset between 9 and 12 months. It is most commonly observed during the diaper-wearing phase, typically in the first two years of life. There is no reported gender predilection, making it equally likely in male and female infants. The condition is rare globally, with cases documented across various regions, including Saudi Arabia, highlighting its universal but infrequent occurrence. Infants with prolonged exposure to occlusive diapers are at higher risk, emphasizing the role of environmental factors in susceptible populations.
Causes
Several predisposing factors contribute to the development of granuloma gluteale infantum, primarily revolving around chronic irritation in the diaper area. Key causative elements include:
- Prolonged exposure to urine and feces, creating a high-pH environment due to urea breakdown by fecal urease.
- Use of nondisposable cloth diapers, plastic pants, or occlusive coverings that trap moisture.
- Irritants such as baby wipes, laundry detergents, starch, talc powder, or topical benzocaine.
- Prolonged or inappropriate use of fluorinated topical corticosteroids, which can exacerbate the condition.
- Secondary candidiasis, often complicating irritant diaper dermatitis.
These factors collectively lead to persistent inflammation, culminating in the characteristic nodular lesions. While the exact etiology remains unclear, the interplay of occlusion, irritation, and sometimes iatrogenic interventions like potent steroids is central.
Clinical Features
The hallmark of granuloma gluteale infantum is the presence of asymptomatic, well-demarcated, firm, round-to-oval, red to purple papules or nodules in the diaper region. Lesions typically measure 0.5 to 4 cm in diameter, with surfaces that may be smooth, lichenified, eroded, or ulcerated depending on the stage. They preferentially locate on the convexities of the gluteal surfaces, perianal area, inguinal folds, and occasionally the scrotum or medial thighs, sparing deeper skin folds in some cases.
Nodules are often ovoid, with their long axis parallel to skin-fold lines, and some may be friable with crusting or erosion. The lesions arise in the context of underlying irritant diaper dermatitis, which may initially present as erythema before progressing to nodules. Systemic symptoms are absent, and the condition remains localized to the napkin area.
Complications
Although granuloma gluteale infantum is benign and self-limiting, potential complications include postinflammatory hyperpigmentation and atrophic scarring. Residual brown macules or depressed scars may persist after resolution, as observed in treated cases. Rarely, secondary bacterial or fungal infections can occur if hygiene is suboptimal. Prolonged cases may lead to discomfort from eroded lesions, though pain is not a primary feature. Early intervention mitigates these risks, emphasizing the importance of prompt recognition.
Diagnosis
Diagnosis is primarily clinical, based on the infant’s history of diaper dermatitis and characteristic nodular lesions in the napkin area. Key diagnostic features include the location, morphology, and absence of systemic involvement. Swabs for bacterial culture and microscopy for fungi (e.g., 10% potassium hydroxide) help rule out infections.
Histological confirmation reveals acanthosis, hyperkeratosis, spongiosis, parakeratosis, and a dense dermal perivascular infiltrate of lymphocytes, neutrophils, histiocytes, plasma cells, and eosinophils. Periodic acid-Schiff (PAS) stain excludes fungal elements, and no true granulomas are typically seen despite the name. Biopsy is reserved for atypical or recalcitrant cases to differentiate from mimics.
Differential Diagnoses
Several conditions mimic granuloma gluteale infantum, necessitating careful differentiation:
| Condition | Key Distinguishing Features |
|---|---|
| Jacquet’s erosive diaper dermatitis | Punched-out erosions and vesicles; more ulcerative. |
| Candidal diaper dermatitis | Satellite pustules, involves folds; responds to antifungals. |
| Infantile acropustulosis | Vesicopustules on hands/feet; pruritic. |
| Infantile Langerhans cell histiocytosis | Crusted, purpuric papules; systemic signs possible. |
| Pediatric bullous pemphigoid | Blisters and urticarial plaques; immunofluorescence positive. |
Other considerations include irritant contact dermatitis without nodules, psoriasis, or histiocytosis. Clinical context and histopathology resolve most ambiguities.
Treatment and Outcome
First-line management focuses on conservative measures: meticulous cleaning, frequent diaper changes, and keeping the area dry using superabsorbent disposable diapers. Application of barrier creams like zinc oxide is recommended to protect the skin. Treat coexisting Candida albicans with topical antifungals such as nystatin or clotrimazole.
Lesions are resistant to topical steroids, barrier creams alone, or antifungals without addressing irritation. Avoid fluorinated corticosteroids, as they may worsen the condition. Nodules typically regress spontaneously within 1–2 months, often leaving atrophic scars or hyperpigmentation.
For recalcitrant cases, topical calcineurin inhibitors like tacrolimus 0.03% ointment twice daily have shown success, leading to complete resolution in 6 weeks without recurrence. This approach is supported by limited case reports as a steroid-sparing alternative. No systemic therapy is usually required.
Frequently Asked Questions (FAQs)
Q: What is granuloma gluteale infantum?
A: It is a rare skin condition in infants causing reddish-purple nodules in the diaper area due to irritant dermatitis.
Q: How is it treated?
A: Keep the area clean and dry, use barrier creams, treat Candida if present, and consider tacrolimus for persistent cases.
Q: Does it go away on its own?
A: Yes, nodules often regress in 1–2 months with proper hygiene, though scars may remain.
Q: Can topical steroids help?
A: No, fluorinated steroids may worsen it; avoid their prolonged use.
Q: Is biopsy always needed?
A: Not routinely; it’s clinical, but useful for confirmation or differentials.
This comprehensive overview equips caregivers and clinicians with evidence-based strategies. Early recognition prevents complications and unnecessary treatments.
References
- Successful Treatment of Recalcitrant Granuloma Gluteale Infantum with Topical Tacrolimus in an Infant — Al-Fouzan AF et al. 2021-06-14. https://pmc.ncbi.nlm.nih.gov/articles/PMC8203409/
- Granuloma gluteale infantum — Wikipedia. Accessed 2026. https://en.wikipedia.org/wiki/Granuloma_gluteale_infantum
- A forgotten complication of diaper dermatitis: granuloma gluteale infantum — Al-Dhafiri S et al. 2011-01-01. https://pmc.ncbi.nlm.nih.gov/articles/PMC3045094/
- Granuloma gluteale infantum – DermNet — DermNet NZ. Accessed 2026. https://dermnetnz.org/topics/granuloma-gluteale-infantum
- Granuloma gluteale infantum – Knowledge and References — Taylor & Francis. Accessed 2026. https://taylorandfrancis.com/knowledge/Medicine_and_healthcare/Dermatology/Granuloma_gluteale_infantum/
- Granuloma Gluteale Infantum: A Case Report — De Zeeuw R et al. 2000-05-01. https://onlinelibrary.wiley.com/doi/10.1046/j.1525-1470.2000.01734.x
Read full bio of Sneha Tete