Harlequin Ichthyosis: What Parents Need To Know
Rare genetic skin disorder causing thick, cracking plates in newborns; intensive care improves survival and quality of life.
Author: Dermatological Society (inferred from high-credibility sources) | Last reviewed: January 2026
What is harlequin ichthyosis?
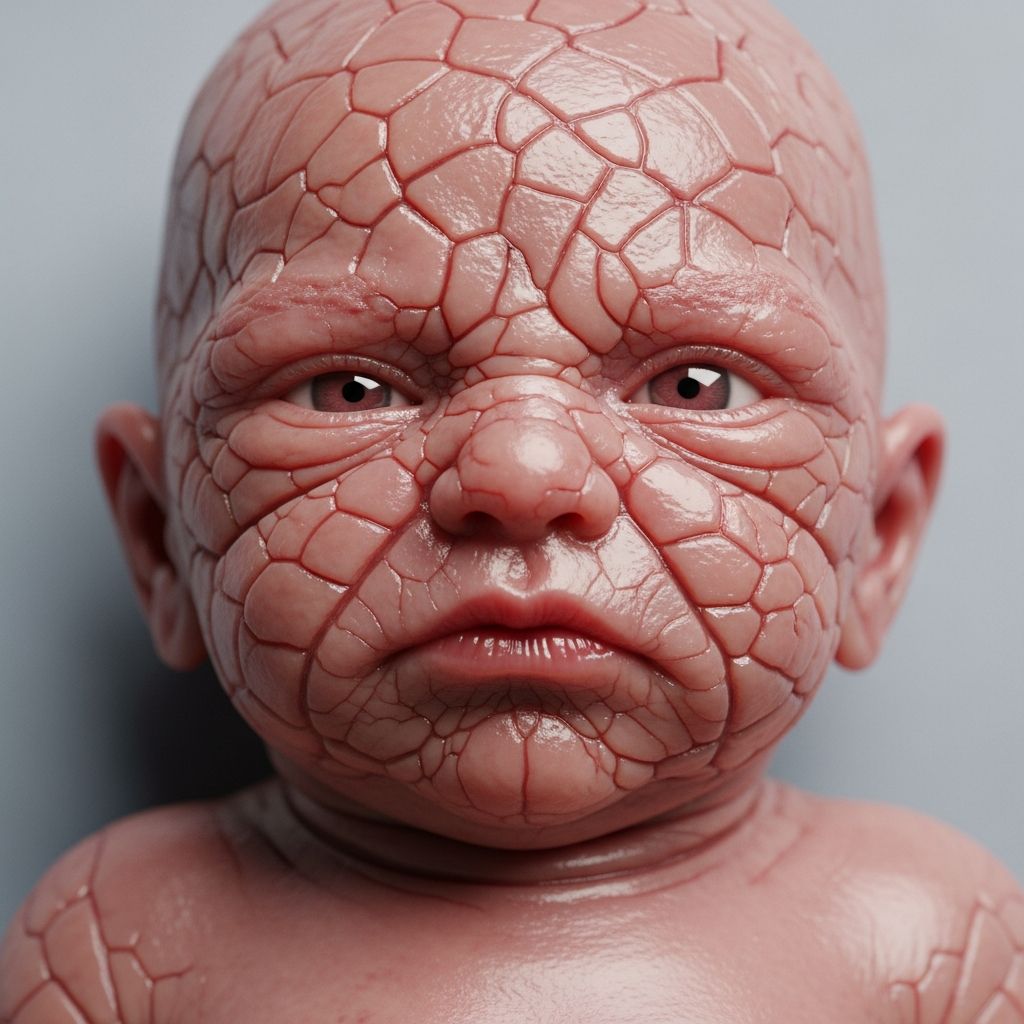
Harlequin ichthyosis (HI), also known as harlequin baby syndrome or ichthyosis congenita gravis, is the most severe phenotype of autosomal recessive congenital ichthyosis (ARCI). It is a rare genetic skin disorder characterized by thick, armour-like plates of skin (hyperkeratosis) that cover the body at birth, resembling the costume of a harlequin clown due to the diamond-shaped fissures and erythematous cracks. Newborns with HI face life-threatening complications from restricted movement, breathing difficulties, and susceptibility to infections, but advances in neonatal intensive care have dramatically improved survival rates from near-zero historically to over 50% reaching adulthood.
HI disrupts the normal lipid barrier of the skin, leading to excessive scaling, dehydration, and impaired thermoregulation. It affects approximately 1 in 300,000 births worldwide, with no ethnic predisposition, though consanguinity increases risk. The condition persists lifelong, transitioning from thick plates in infancy to erythroderma and fine scales in survivors.
Who gets harlequin ichthyosis?
Harlequin ichthyosis manifests at birth, primarily affecting premature infants. It occurs equally in males and females. There is no racial predilection, but higher incidence is noted in populations with high rates of consanguineous marriages, such as certain Middle Eastern and South Asian communities. All cases are genetic, with parents being asymptomatic carriers.
- Incidence: Extremely rare; fewer than 300 cases reported globally.
- Age: Present from birth; symptoms evolve over weeks.
- Sex: Affects both sexes equally.
What causes harlequin ichthyosis?
Harlequin ichthyosis results from biallelic mutations in the ABCA12 gene on chromosome 15q22.31, which encodes an ATP-binding cassette transporter critical for lipid transport in keratinocytes. Over 80 mutations have been identified, including nonsense, frameshift, and splice-site variants, leading to absent or dysfunctional ABCA12 protein. This impairs lamellar granule formation, causing defective intercellular lipid lamellae, hyperkeratosis, and skin fragility.
Inheritance is autosomal recessive: both parents must carry one mutated allele. Carrier frequency is estimated at 1 in 200 600. Prenatal diagnosis is possible via genetic testing of amniocentesis or chorionic villus sampling (CVS) after molecular confirmation in affected families.
| Mutation Type | Protein Impact | Skin Phenotype Severity |
|---|---|---|
| Nonsense/Frameshift | Complete loss (null alleles) | Severe classic HI |
| Missense | Partial function | Milder or atypical HI |
| Splice-site | Reduced expression | Variable |
What are the clinical features of harlequin ichthyosis?
At birth
Newborns with HI are often premature (32 636 weeks) and appear as ‘collodion babies’ encased in a taut, shiny membrane that splits into large, yellow-white diamond-shaped plates separated by deep, red fissures. Ectropion (everted eyelids) and eclabium (everted lips) are universal, exposing corneal and oral mucosa. The nose and ears are rudimentary or flattened; limbs are fixed in extension due to constricting skin bands. Chest restriction causes hypoplastic lungs and respiratory distress, often requiring intubation.
- Skin: Thick plates (1 63 cm), deep fissures prone to infection.
- Face: Ectropion, eclabium, flattened nose/ears.
- Limbs: Contractures, pseudocontractures, digit ectropion.
- Systemic: Hypoventilation, dehydration, hypothermia, electrolyte imbalance.
Neonatal period (first 4 66 weeks)
The rigid casing sheds progressively, revealing erythematous, desquamating skin with fine scales. Complications peak: sepsis (commonest cause of death), hypernatremia, hyperthermia, feeding intolerance. Intensive care in humidified incubators (80 690% humidity) is essential.
Childhood and beyond
Survivors develop lamellar ichthyosis-like skin: generalized erythroderma, large adherent scales (thickest on flexures), palmoplantar keratoderma. Ectropion may persist or recur, risking keratitis/strabismus. Other features include sparse hair, dental anomalies, nail dystrophy. Growth retardation, recurrent infections, and failure to thrive are common but improve with age.
| Stage | Skin Appearance | Complications |
|---|---|---|
| Birth | Armour-like plates, fissures | Respiratory failure, ectropion |
| Neonatal | Shedding, erythroderma | Sepsis, dehydration |
| Childhood | Scales, hyperkeratosis | Infections, ectropion recurrence |
| Adulthood | Stable erythroderma | Pruritus, vitamin D deficiency |
Diagnosis of harlequin ichthyosis
Diagnosis is primarily clinical at birth based on characteristic morphology. Confirmed by:
- Genetic testing: Targeted ABCA12 sequencing (pathogenic variants in 90% cases).
- Skin biopsy: Orthokeratotic hyperkeratosis, absent lamellar bodies on electron microscopy.
- Prenatal: Ultrasonography (polyhydramnios, fetal akinesia); 3D US shows ‘shiny’ skin; genetic testing on fetal DNA.
Treatment of harlequin ichthyosis
There is no cure; management is supportive and multidisciplinary (dermatology, neonatology, ophthalmology, nutrition, physiotherapy). Goals: prevent infection, maintain barrier function, support nutrition/growth.
Neonatal intensive care
- Humidified incubator (80 690% RH, 32 6346C).
- Petroleum jelly/emollients q4 66h to fissures.
- Antibiotics for suspected sepsis.
- Mechanical ventilation if needed.
- NG feeding; monitor electrolytes.
Retinoids
Oral retinoids (acitretin 0.5 61 mg/kg/day or etretinate) accelerate shedding in severe cases but reserved due to toxicity (hypercalcemia, pseudotumor cerebri). Topical retinoids (tazarotene 0.1%) for localized hyperkeratosis.
Long-term care
- Daily emollients (e.g., white soft paraffin).
- Keratolytics (urea 10 620%, lactic acid).
- Exfoliation gloves for scales.
- Vitamin D supplementation (deficiency common).
- Ophthalmic lubricants; surgery for severe ectropion.
- Hand splinting/fasciotomy for digit necrosis.
Surgical interventions
Indicated for recurrent ectropion (tarsorrhaphy, grafts), digit constriction (fasciotomy), nasal patency. Pre-op retinoids/skin prep reduce complications.
What is the prognosis for harlequin ichthyosis?
Historically fatal in days/weeks from sepsis/respiratory failure; now ~60% survive infancy with NICU care. Long-term: improved quality of life, though chronic issues persist (pruritus, infections, scarring). Puberty often brings cosmetic improvement. Life expectancy into adulthood possible with compliance.
How can harlequin ichthyosis be prevented?
Genetic counseling for carrier families. Prenatal testing (non-invasive cfDNA or invasive) allows informed decisions. Preimplantation genetic diagnosis (PGD) in IVF.
Emerging therapies
Gene therapy targeting ABCA12 restoration and lipid supplementation show promise in models. mRNA therapy and topical cholesterol/ceramides under investigation.
Frequently asked questions (FAQs) on harlequin ichthyosis
Q: Is harlequin ichthyosis curable?
A: No, it is a genetic condition without cure, but symptoms are manageable with lifelong skincare and medical support.
Q: Can babies with harlequin ichthyosis survive?
A: Yes, survival has improved to over 50% into adulthood due to NICU interventions, retinoids, and infection control.
Q: What does a harlequin baby look like?
A: At birth, covered in thick, cracking skin plates with everted eyes/lips, resembling a harlequin costume.
Q: Is harlequin ichthyosis hereditary?
A: Yes, autosomal recessive inheritance via ABCA12 mutations; both parents are carriers.
Q: How is harlequin ichthyosis treated?
A: Neonatal: incubator, emollients, antibiotics. Long-term: moisturizers, keratolytics, retinoids, surgery as needed.
References
- Harlequin Ichthyosis (HI): Causes, Symptoms & Treatment — Cleveland Clinic. 2023-10-15. https://my.clevelandclinic.org/health/diseases/harlequin-ichthyosis
- DI 23022.188 – Harlequin Ichthyosis – Child — Social Security Administration (gov). 2024-01-01. https://secure.ssa.gov/apps10/poms.nsf/lnx/0423022188
- Harlequin Ichthyosis — National Organization for Rare Disorders (NORD). 2023-05-20. https://rarediseases.org/rare-diseases/ichthyosis-harlequin-type/
- Management of Harlequin Ichthyosis: A Brief Review of the Recent… — PMC/NCBI (peer-reviewed). 2022-06-10. https://pmc.ncbi.nlm.nih.gov/articles/PMC9221756/
- Harlequin Ichthyosis: Causes, Symptoms & Treatments — WebMD. 2024-02-14. https://www.webmd.com/children/what-is-harlequin-ichthyosis
Read full bio of medha deb