Heel Pain and Plantar Fasciitis: Causes, Symptoms & Treatment
Understanding plantar fasciitis: Learn about symptoms, causes, and effective treatment options for heel pain relief.
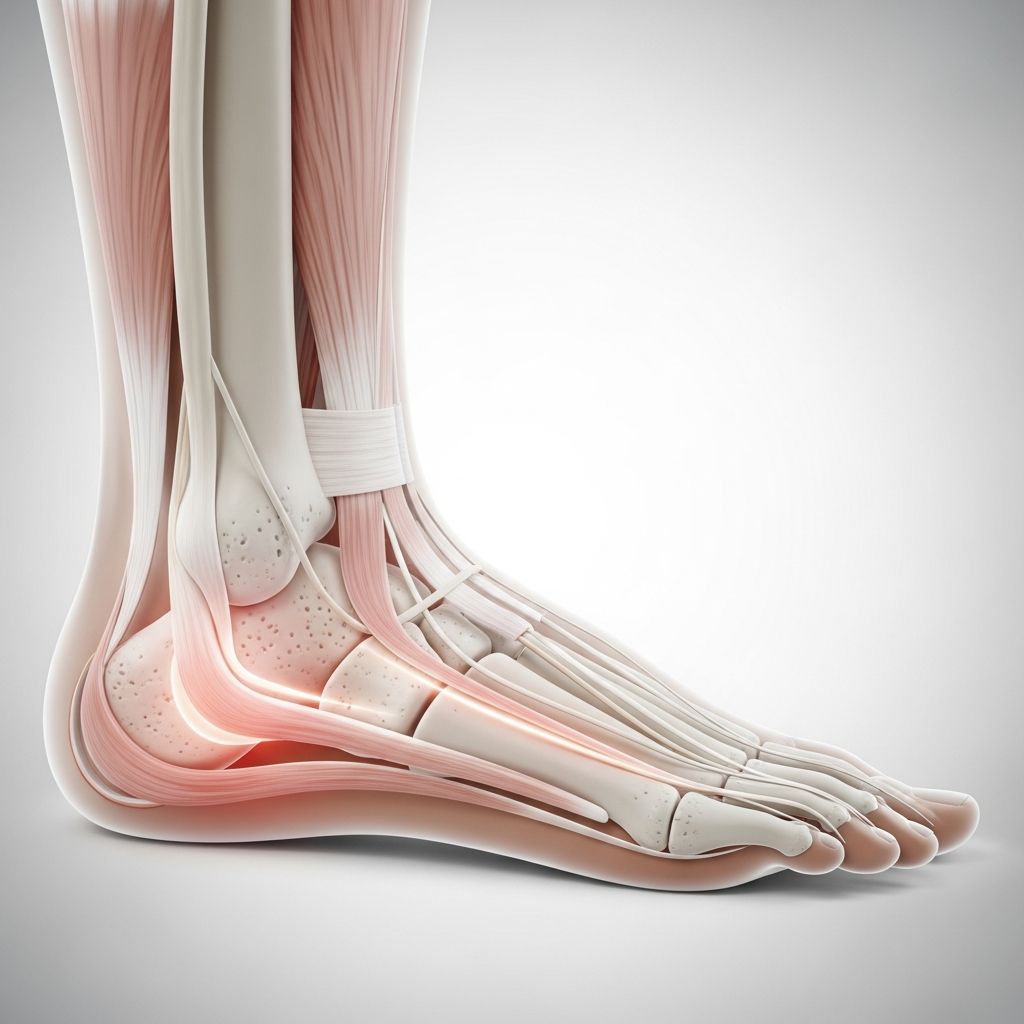
Understanding Heel Pain and Plantar Fasciitis
Heel pain is one of the most common foot complaints affecting millions of people each year. Among the various causes of heel pain, plantar fasciitis stands out as one of the most prevalent conditions. This condition occurs when the plantar fascia—a thick band of tissue running along the bottom of your foot from your heel bone to your toes—becomes inflamed and irritated. Understanding this condition is essential for effective management and relief.
What Is Plantar Fasciitis?
The plantar fascia is a strong, fibrous tissue that plays a crucial role in foot mechanics. It acts like a shock absorber, supporting the arch of your foot and helping to distribute your body weight evenly across your feet when you walk, run, or stand. When this tissue becomes damaged or strained, it triggers inflammation and pain, leading to the condition known as plantar fasciitis.
Interestingly, despite its name ending in “-itis” (which typically indicates inflammation), research shows that plantar fasciitis is characterized by degenerative changes rather than true inflammation. The condition involves microtears and degeneration at the attachment point where the plantar fascia connects to the heel bone. This distinction is important for understanding how the condition develops and progresses over time.
Common Symptoms of Plantar Fasciitis
Recognizing the symptoms of plantar fasciitis is the first step toward seeking appropriate treatment. The condition presents with several characteristic signs:
- Stabbing heel pain: The primary symptom is a sharp, stabbing pain in the bottom of your foot near the heel. This pain can range from dull to sharp depending on the severity and individual factors.
- Morning pain: Pain is typically worst with the first few steps after awakening, as the plantar fascia tightens overnight. This morning stiffness usually improves after a few minutes of walking.
- Activity-related pain: Pain may worsen after long periods of standing, walking, or running, and often increases as the day progresses. The pain typically worsens after activity rather than during it.
- Heel swelling: Some individuals experience visible swelling in the heel area.
- Sole discomfort: Aching or burning sensations may develop along the sole of your foot, particularly at the arch.
- Stretching pain: Pain may be triggered when stretching the bottom of your foot, such as when raising your toes off the floor or walking up stairs.
What Causes Plantar Fasciitis?
Plantar fasciitis develops through a combination of factors. The primary mechanism involves excessive stress on the plantar fascia, which can damage or tear the tissue. When the body responds to this injury, inflammation develops, resulting in heel pain and stiffness. Multiple risk factors can increase your likelihood of developing this condition:
Biomechanical Factors
- Foot arch issues: Both flat feet (pes planus) and high arches (pes cavus) can contribute to plantar fasciitis. Flat feet increase strain at the origin of the plantar fascia, while high arches prevent effective shock absorption.
- Tight calf muscles: Tightness in the gastrocnemius, soleus, and other posterior leg muscles can alter normal walking biomechanics and increase strain on the plantar fascia.
- Ankle weakness or injury: Previous ankle injuries or underlying weakness can compromise foot stability and increase stress on the plantar fascia.
Activity and Lifestyle Factors
- Sudden increase in activity: Rapidly increasing the intensity or duration of physical activity can overload the plantar fascia.
- Prolonged standing: Spending extended periods on your feet without adequate rest places continuous stress on the tissue.
- High-impact exercise: Activities like running, especially on hard surfaces, can strain the plantar fascia.
- Overweight or obesity: Excess body weight increases the pressure and strain on your heels and the plantar fascia.
Age and Personal Factors
- Age: Plantar fasciitis is more common in people over 40 years old.
- Footwear: Shoes that lack proper cushioning or arch support can contribute to the development of plantar fasciitis.
- Occupations: Jobs requiring prolonged standing or walking increase risk.
Heel Spurs and Their Relationship to Plantar Fasciitis
A heel spur is a bony growth that develops on the heel bone, typically at the point where the plantar fascia attaches. Many people develop heel spurs as a result of prolonged stress and inflammation caused by plantar fasciitis. However, it’s important to note that most people with heel spurs experience no pain at all. The presence of a heel spur doesn’t necessarily indicate that you’ll have symptoms, though when pain does develop from a spur, it typically feels similar to plantar fasciitis pain.
Diagnosis of Plantar Fasciitis
Diagnosing plantar fasciitis typically begins with a physical examination and discussion of your symptoms. Healthcare providers look for characteristic signs such as pain when pressing on the medial calcaneal tubercle (the point where the plantar fascia attaches to the heel bone) and pain that reproduces when passively flexing the foot and toes. Your doctor may also inquire about your daily activities, footwear, and exercise habits to understand contributing factors.
Imaging tests such as X-rays may be used to rule out other causes of heel pain or to identify the presence of a heel spur, though these aren’t always necessary for diagnosis. The clinical presentation and physical examination findings are usually sufficient for confirming plantar fasciitis.
Treatment Options for Plantar Fasciitis
Most cases of plantar fasciitis respond well to conservative, non-surgical treatments. A comprehensive treatment approach typically includes several components working together:
Conservative Management Strategies
- Rest and activity modification: Reducing activities that place stress on the heel allows the tissue time to heal. This doesn’t mean complete immobility but rather avoiding high-impact activities that aggravate symptoms.
- Stretching exercises: Regular stretching of the plantar fascia, calf muscles, and Achilles tendon can improve flexibility and reduce pain. These exercises should be performed gently and consistently.
- Supportive footwear: Wearing shoes with proper arch support and heel cushioning is essential. Supportive shoes help distribute weight more evenly and reduce strain on the plantar fascia.
- Custom orthotics: Specialized shoe inserts or custom orthotic devices can provide additional arch support and heel cushioning tailored to your specific foot mechanics.
- Pain management: Over-the-counter anti-inflammatory medications can help manage pain and swelling, though relief is often temporary. These should be used as directed and discussed with your healthcare provider.
- Ice therapy: Applying ice to the heel for 15-20 minutes several times daily can help reduce inflammation and provide temporary pain relief.
- Weight management: If you’re overweight, losing weight can significantly reduce the stress on your heels and improve symptoms.
Professional Treatment Approaches
- Physical therapy: A physical therapist can design a personalized exercise program focusing on stretching and strengthening muscles that support the foot and ankle.
- Corticosteroid injections: In some cases, injections may be recommended to reduce inflammation and provide pain relief.
- Extracorporeal shock wave therapy (ESWT): This non-invasive procedure uses shock waves to stimulate healing in the affected tissue.
- Night splints: Wearing a splint while sleeping keeps the plantar fascia stretched overnight, potentially reducing morning pain.
Surgical Options
Surgical treatment is considered only when conservative approaches have failed and symptoms persist. Procedures may involve releasing the plantar fascia or removing a heel spur. However, surgery is not commonly needed, as most patients achieve relief through non-surgical methods.
Prevention Strategies
Taking preventive measures can help you avoid developing plantar fasciitis or prevent recurrence:
- Maintain a healthy weight: Excess weight increases pressure on your feet, so weight management is crucial.
- Choose appropriate footwear: Invest in shoes with good arch support, cushioning, and heel protection. Replace worn-out shoes regularly.
- Warm up properly: Before exercise, spend time warming up and stretching your calf muscles and plantar fascia.
- Increase activity gradually: When starting a new exercise routine or sport, increase intensity and duration gradually to avoid overloading the plantar fascia.
- Stretch regularly: Incorporate daily stretching exercises for your calves, Achilles tendon, and plantar fascia into your routine.
- Avoid prolonged standing: Take regular breaks if your job requires standing for extended periods. Sit down and elevate your feet when possible.
- Exercise on appropriate surfaces: Avoid excessive running or high-impact activities on hard surfaces. Choose softer surfaces like grass or a track when possible.
When to Seek Medical Attention
While many cases of heel pain improve with home care, you should consult a healthcare provider if:
- Pain is severe or interferes with daily activities
- Symptoms persist for more than a few weeks despite self-care measures
- You cannot bear weight on the affected foot
- Pain develops suddenly or follows an injury
- You have swelling, redness, or warmth in the heel area
Frequently Asked Questions
Q: How long does it take for plantar fasciitis to heal?
A: Recovery time varies depending on the severity and individual factors. Most people see improvement within a few weeks to months with appropriate conservative treatment. However, some cases may take 6-12 months to fully resolve. Consistency with stretching exercises and activity modification is key to faster recovery.
Q: Can plantar fasciitis be cured permanently?
A: With appropriate treatment and prevention strategies, most people achieve lasting relief from symptoms. However, plantar fasciitis can recur if you return to activities that created the original problem without maintaining preventive measures like stretching and wearing supportive shoes.
Q: Is surgery necessary for plantar fasciitis?
A: Surgery is rarely necessary. Approximately 90% of people with plantar fasciitis respond well to non-surgical treatments including stretching, rest, supportive footwear, and anti-inflammatory measures. Surgery is only considered when conservative treatment fails over an extended period.
Q: What exercises are most effective for plantar fasciitis?
A: Effective exercises include calf stretches, plantar fascia stretches (such as the towel stretch), and strengthening exercises for the intrinsic foot muscles. A physical therapist can demonstrate proper technique to ensure you’re performing exercises correctly and safely.
Q: Can I continue exercising with plantar fasciitis?
A: Yes, but modifications are important. Avoid high-impact activities that aggravate symptoms, and focus on low-impact exercises like swimming or cycling. Always wear supportive footwear and warm up properly before activity.
Q: Are there any complications from untreated plantar fasciitis?
A: Untreated plantar fasciitis can lead to changes in your gait to compensate for heel pain, potentially causing problems in your ankles, knees, hips, and back. Additionally, chronic foot pain may contribute to reduced physical activity and associated health consequences. Early intervention helps prevent these complications.
References
- Plantar Fasciitis — Symptoms and Causes — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/plantar-fasciitis/symptoms-causes/syc-20354846
- Plantar Fasciitis — Treatment, Symptoms and Causes — HealthDirect Australia. 2023. https://www.healthdirect.gov.au/plantar-fasciitis
- Plantar Fasciitis — National Health Service (NHS). 2024. https://www.nhs.uk/conditions/plantar-fasciitis/
- Plantar Fasciitis and Bone Spurs — American Academy of Orthopaedic Surgeons (AAOS). 2024. https://orthoinfo.aaos.org/en/diseases–conditions/plantar-fasciitis-and-bone-spurs
- What is Plantar Fasciitis? Causes, Symptoms, and Treatment — Brown Health. 2024. https://www.brownhealth.org/be-well/what-plantar-fasciitis-causes-symptoms-and-treatment
- Plantar Fasciitis: Symptoms, Causes & Treatment Options — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/14709-plantar-fasciitis
- Plantar Fasciitis — National Center for Biotechnology Information (NCBI). 2024. https://www.ncbi.nlm.nih.gov/books/NBK431073/
Read full bio of Sneha Tete











