Heel Spurs: Symptoms, Causes, and Treatment
Complete guide to understanding heel spurs, their causes, symptoms, and effective treatment options.
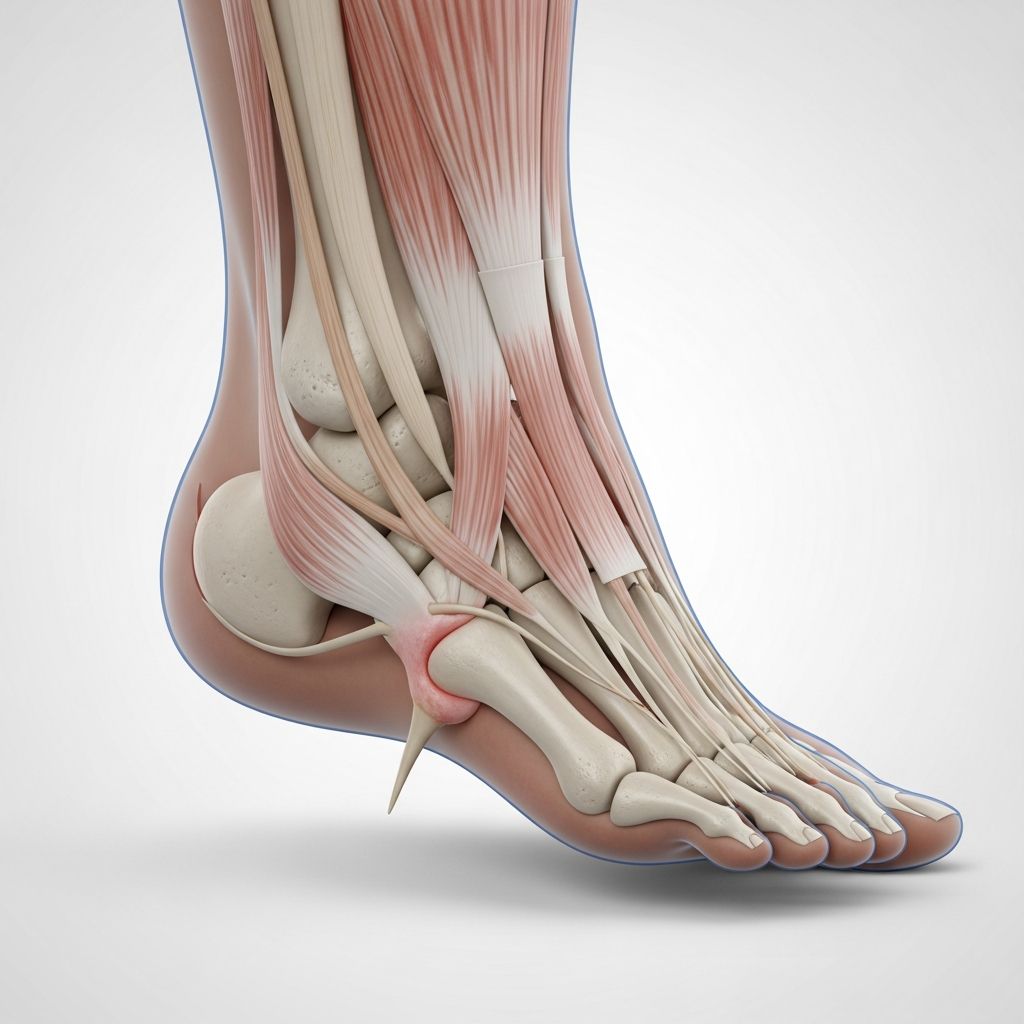
What Are Heel Spurs?
A heel spur is a bony growth that develops on the underside or back of your heel bone, protruding into the surrounding tissue. These growths, medically known as calcaneal spurs or osteophytes, form through the gradual accumulation of calcium deposits on the heel bone. Heel spurs typically develop over time as a result of repetitive stress and strain placed on the plantar fascia—the ligament that runs along the bottom of your foot connecting your toes to your heel bone.
The formation of a heel spur occurs when your body responds to consistent tension and micro-tears in the fascia by depositing calcium to reinforce the area. While many people with heel spurs never experience symptoms, others may develop significant pain that interferes with daily activities. It’s important to note that many individuals don’t discover they have a heel spur until they seek medical attention for heel pain, as the spur itself is often identified incidentally during imaging studies.
Understanding the Relationship Between Heel Spurs and Plantar Fasciitis
Heel spurs and plantar fasciitis are closely related but distinct conditions that frequently occur together. Understanding the connection between these two conditions is essential for proper treatment and management. Plantar fasciitis is an inflammation of the plantar fascia caused by excessive stress on this fibrous tissue. When plantar fasciitis develops, your body often responds by creating a heel spur as part of its natural healing process.
Research indicates that approximately 50 percent of people with plantar fasciitis develop heel spurs. However, a critical point to understand is that the heel spur itself is not usually the source of pain. Instead, the pain typically originates from the inflammation of the plantar fascia. This distinction is crucial because it means that while a heel spur may be visible on X-rays, removing it surgically may not always alleviate the underlying pain if inflammation persists. Both conditions respond well to conservative treatment approaches focused on reducing inflammation and stress on the foot.
Symptoms of Heel Spurs
Interestingly, not everyone who has a heel spur experiences symptoms. Some heel spurs remain completely asymptomatic and are discovered accidentally during imaging for unrelated reasons. However, when symptoms do develop, they can significantly impact quality of life and mobility.
Common symptoms of heel spurs include:
- Sharp or stabbing pain in the heel, particularly on the underside of the foot
- Pain that is often worse with the first few steps after waking or after prolonged periods of sitting
- Chronic pain that may develop gradually over time
- Tenderness in the affected heel area
- A visible or palpable bump on the bottom or back of the heel
- Pain that worsens with activities involving running, jumping, or prolonged standing
- Difficulty walking or participating in physical activities
The pain pattern is often characteristic: individuals typically experience the most intense discomfort during the initial weight-bearing steps after a period of rest. As the day progresses and the foot warms up, pain may temporarily decrease, only to return or intensify with additional activity or after rest.
Causes of Heel Spurs
Heel spurs develop as a direct response to mechanical stress and strain on the heel bone and surrounding tissues. The primary cause is the gradual accumulation of calcium deposits at sites of repetitive stress or minor injury to the plantar fascia. This process typically occurs over months or years.
Several specific factors contribute to heel spur formation:
- Repetitive impact activities: Running, jogging, and jumping on hard surfaces like concrete place repeated stress on the heel
- Occupational factors: Jobs requiring extended periods of standing or walking increase heel stress
- Improper footwear: Shoes lacking adequate cushioning or support fail to absorb shock effectively
- Gait abnormalities: Unusual walking patterns that place extra pressure on specific heel areas
- Foot structure issues: Abnormally high arches or flat feet alter weight distribution
- Systemic factors: Obesity, diabetes, and inflammatory conditions increase susceptibility
- Age-related changes: Natural deterioration of tissues and reduced elasticity occur with aging
The underlying mechanism involves chronic tension on the plantar fascia causing small tears and inflammation. Your body’s healing response involves depositing calcium at the injury site, gradually building up the characteristic bony spur over time.
Risk Factors for Developing Heel Spurs
Several factors increase your likelihood of developing heel spurs. Understanding these risk factors can help you take preventive measures to reduce your risk or catch the condition early.
| Risk Factor Category | Specific Risk Factors |
|---|---|
| Activity-Related | Repeated running or jumping on hard surfaces, short frequent bursts of high-impact exercise |
| Occupational | Jobs requiring extended standing or walking throughout the day |
| Biomechanical | Abnormal gait, high arches, flat feet, tight calf muscles |
| Footwear-Related | Non-supportive shoes, inadequate cushioning, high heels |
| Personal Health Factors | Overweight or obesity, increasing age, diabetes, rheumatoid arthritis |
Age is a particularly significant risk factor, with heel spurs becoming increasingly common in individuals over 40 years old. People with diabetes face an elevated risk for developing heel spurs in addition to other foot complications. Similarly, those carrying excess body weight place additional stress on their heels with every step, accelerating spur formation.
Potential Complications of Heel Spurs
While heel spurs themselves may seem like a minor issue, untreated or inadequately managed heel spurs can lead to several complications that affect overall health and quality of life.
Gait abnormalities and secondary pain: Attempting to avoid heel pain often causes people to alter their walking pattern, shifting weight to other areas of the foot. This compensation mechanism can lead to pain and dysfunction in the ankle, knee, hip, and lower back. Chronic gait abnormalities may result in long-term musculoskeletal problems requiring additional treatment.
Reduced activity and fitness decline: Heel pain frequently causes people to avoid walking, running, and other physical activities. This reduction in activity can lead to weight gain, deconditioning, and increased risk of cardiovascular disease and metabolic disorders.
Quality of life impact: Chronic pain significantly affects psychological well-being, sleep quality, and social participation. Many people with heel spurs report reduced enjoyment of leisure activities and difficulty maintaining their previous activity levels.
Surgical complications: When conservative treatments fail and surgery becomes necessary, potential surgical risks include increased pain, infection, blood clots, excessive bleeding, and nerve damage. It’s essential to consult with an experienced foot surgeon to thoroughly discuss both benefits and risks before pursuing surgical intervention.
Diagnosis of Heel Spurs
Diagnosis typically begins with a clinical evaluation by a healthcare provider, including a thorough medical history and physical examination. Your provider will assess your pain pattern, examine your foot structure, and evaluate your gait. Imaging studies, particularly X-rays, confirm the presence of a heel spur and help determine its size and exact location. Sometimes heel spurs are discovered incidentally when imaging is performed for other reasons.
Advanced imaging like ultrasound or MRI may be ordered to evaluate associated soft tissue inflammation, particularly if plantar fasciitis is suspected. A systematic diagnostic approach helps differentiate heel spurs from other causes of heel pain.
Treatment Options for Heel Spurs
Good news: more than 90 percent of people with painful heel spurs improve with non-surgical treatments. Healthcare providers recommend conservative approaches as the first line of treatment before considering surgery.
Non-Surgical Treatment Approaches
Rest and activity modification: Reducing high-impact activities and avoiding activities that worsen pain allows inflammation to subside. This doesn’t mean complete immobility but rather modifying activities to lower stress on the heel.
Ice therapy: Applying ice for 15-20 minutes several times daily reduces inflammation and pain. Ice should be wrapped in a towel to protect skin.
Footwear modifications: Wearing shoes with adequate cushioning, proper arch support, and heel cups distributes pressure more evenly. Orthotics and custom insoles can provide additional support and shock absorption, specifically designed for your foot structure.
Stretching exercises: Gentle stretching of the calf muscles and plantar fascia improves flexibility and reduces tension. Physical therapy programs teach proper stretching techniques and strengthening exercises.
Pain management: Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can reduce pain and inflammation. Prescription medications may be considered in some cases.
Corticosteroid injections: Injected directly into the affected area, corticosteroids reduce inflammation and provide pain relief lasting several weeks to months.
Plantar fascia strapping: Special taping techniques provide support and reduce stress on the fascia during activity.
Surgical Treatment Options
Surgery is reserved for cases where conservative treatments have failed after several months of dedicated effort. Two main surgical approaches are available:
Plantar fascia release: This procedure involves partially cutting or releasing the plantar fascia to reduce tension and allow the tissue to heal in a lengthened position. This addresses the underlying inflammation causing pain.
Heel spur removal: During fascia release surgery, the surgeon may completely remove the heel spur itself. Heel spur removal procedures are relatively rare today, performed only when the spur is particularly large or symptomatic. The surgeon makes either one large incision or several smaller incisions, using specialized surgical instruments to remove the bony deposit.
Both procedures can be performed using open surgery with one larger incision or endoscopic surgery with smaller incisions. Recovery typically requires several months, with vigorous exercise resumable after approximately three months. Shock-absorbing shoe insoles and orthopedic supports aid recovery.
Prevention Strategies
Several evidence-based strategies help prevent heel spur development:
- Maintain a healthy body weight to reduce pressure on heels
- Wear supportive, well-cushioned shoes with adequate arch support
- Perform regular calf and plantar fascia stretches
- Avoid repetitive high-impact activities on hard surfaces
- Use shock-absorbing orthotics during exercise
- Gradually increase exercise intensity rather than sudden changes
- Manage underlying conditions like diabetes and arthritis
- Consider custom orthotics if you have structural foot abnormalities
Frequently Asked Questions About Heel Spurs
Q: Are heel spurs always painful?
A: No. Many people with heel spurs experience no symptoms whatsoever. Some spurs are discovered incidentally during imaging for unrelated issues. Not everyone with a radiographic heel spur develops pain.
Q: Is a heel spur the same as plantar fasciitis?
A: No, they are related but distinct conditions. A heel spur is a bony growth that may develop in response to plantar fasciitis, but the pain typically comes from fascia inflammation, not the spur itself. About 50 percent of plantar fasciitis patients develop heel spurs.
Q: Can heel spurs go away on their own?
A: The bony spur itself doesn’t disappear, but associated pain can resolve with proper treatment and management. Conservative treatments address the inflammation causing pain rather than the spur itself.
Q: How long does recovery take after heel spur surgery?
A: Full recovery typically requires several months. Most people can resume vigorous exercise approximately three months after surgery, though complete healing and return to pre-injury activity levels may take longer.
Q: What percentage of people need surgery for heel spurs?
A: More than 90 percent of people with heel spurs improve with conservative non-surgical treatments. Surgery is reserved for the small percentage of cases where extensive non-surgical treatment has failed.
Q: Can I prevent heel spurs?
A: While you cannot guarantee prevention, you can significantly reduce your risk by maintaining healthy weight, wearing supportive shoes, performing regular stretches, avoiding excessive high-impact activities, and using orthotics when needed.
Q: What types of shoes should I wear if I have heel spurs?
A: Look for shoes with excellent cushioning in the heel area, proper arch support, and shock-absorbing soles. Many people benefit from using custom or over-the-counter orthotic inserts. Avoid high heels and flat shoes without support.
Q: Are heel spurs more common in athletes?
A: Heel spurs are more common in people who engage in repetitive high-impact activities like running and jumping, but they develop in many non-athletes due to occupational factors, age, weight, and foot structure.
References
- Heel Spurs: Symptoms, Causes, and Treatment — Cleveland Clinic. 2021-10-19. https://my.clevelandclinic.org/health/diseases/21965-heel-spurs
- Heel Spur: Symptoms, Causes, Risk Factors & Treatment — Healthgrades. https://resources.healthgrades.com/right-care/foot-health/heel-spur
- Heel Spur Surgery: Procedure Benefits, Risks, Recovery, and Cost — Healthline. https://www.healthline.com/health/heel-spur-surgery
- Heel Spur Removal — EBSCO Research Starters. https://www.ebsco.com/research-starters/health-and-medicine/heel-spur-removal
- Heel Pain: Diagnosis and Treatment, Step by Step — Cleveland Clinic Journal of Medicine, Vol. 73, No. 5. 2006. https://www.ccjm.org/content/73/5/465
- Get Bone Spur Treatment — Cleveland Clinic. https://my.clevelandclinic.org/services/bone-spur-treatment
Read full bio of medha deb











