Herniated Disk: Causes, Symptoms & Treatment
Complete guide to herniated disks: understand symptoms, diagnosis, and effective treatment options.
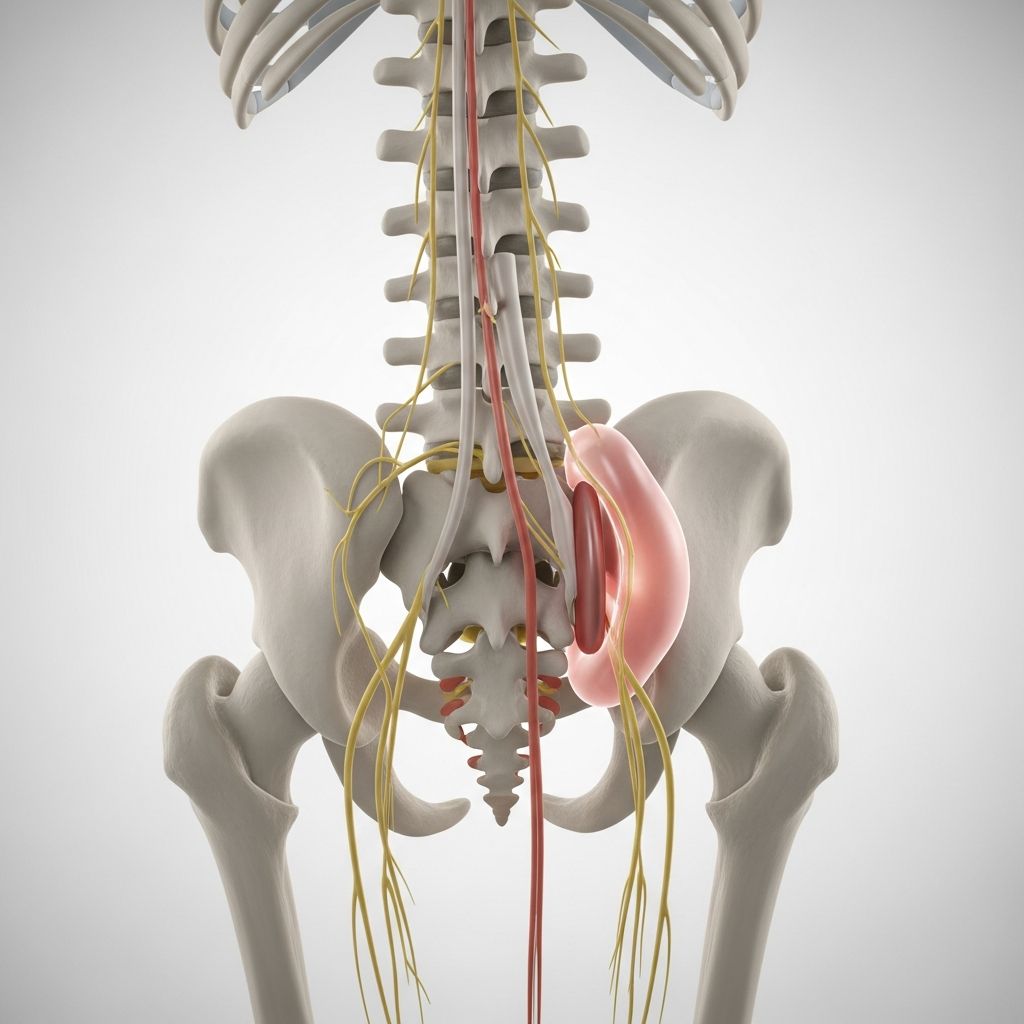
Understanding Herniated Disks
A herniated disk, also commonly referred to as a slipped disk or bulging disk, occurs when the soft inner material of a spinal disk protrudes through the outer layer. This condition can put pressure on nearby nerves and cause pain, numbness, and weakness in the affected area. While herniated disks can sound alarming, the good news is that most cases resolve on their own within four to six weeks with appropriate care.
Your spine consists of vertebrae stacked on top of each other, with cushioning disks between them. These disks absorb shock and allow your spine to flex and bend. When a disk herniates, the inner gel-like substance pushes through cracks in the outer ring, potentially irritating nearby nerves. This condition can occur anywhere along the spine, from the neck to the lower back, affecting your quality of life and daily activities.
Causes and Risk Factors
Herniated disks can develop suddenly from a specific injury or gradually over time due to wear and tear on your spine. Several factors contribute to your risk of developing a herniated disk:
- Age-related degeneration of disks
- Repetitive strain or poor lifting techniques
- Sedentary lifestyle with weak core muscles
- Smoking, which reduces disk nutrition
- Obesity, which increases spine stress
- Sudden traumatic injuries or accidents
- Genetic predisposition to disk problems
Understanding these risk factors can help you take preventive measures to protect your spine health and reduce the likelihood of developing a herniated disk.
Symptoms of a Herniated Disk
The symptoms of a herniated disk vary depending on the location of the herniation and which nerves are affected. Some people experience minimal symptoms, while others may have significant pain and discomfort. Common symptoms include:
- Sharp or burning pain in the affected area
- Numbness or tingling sensations radiating down the leg or arm
- Muscle weakness in the legs or arms
- Pain that worsens with certain movements or positions
- Difficulty walking or maintaining balance
- Muscle spasms in the back
Pain from a herniated disk can radiate down your leg if the herniation occurs in the lumbar spine, a condition called sciatica. In cervical herniated disks affecting the neck, pain may radiate down your arm. These radiating symptoms occur because the herniated disk material is pressing on nerve roots that extend into these areas.
Diagnosis and Physical Examination
Your healthcare provider will conduct a comprehensive evaluation to diagnose a herniated disk. The diagnostic process begins with taking a detailed medical history and performing a thorough physical examination. During this evaluation, your provider will:
- Assess your pain level and its location
- Test your muscle reflexes and strength
- Evaluate sensation in affected areas
- Perform specific orthopedic tests
The Straight Leg Raise Test
One specific diagnostic test your provider may perform is the straight leg raise test. During this test, you lie on your back while your provider raises one leg straight in the air. If you experience pain radiating down your leg during this maneuver, it suggests a herniated disk is pressing on a nerve. This simple yet effective test helps confirm the presence of nerve compression and can indicate which nerve root is affected.
Imaging and Diagnostic Tests
To confirm the diagnosis and determine the exact location and severity of the herniation, your healthcare provider may order imaging tests: These imaging studies provide detailed views of your spine and help guide treatment decisions.
| Imaging Test | Purpose | Advantages |
|---|---|---|
| MRI (Magnetic Resonance Imaging) | Provides detailed images of soft tissues, disks, and nerves | Non-invasive, excellent for visualizing disk herniations and nerve compression |
| CT Scan | Creates cross-sectional images of the spine | Useful for evaluating bone structures and severity of herniation |
| X-rays | Shows bone alignment and overall spinal structure | Quick, readily available, helps assess spinal curvature |
| Myelogram | Involves injecting contrast dye to visualize nerves | Provides detailed nerve pathway visualization when other tests are unclear |
Your provider may also perform a neurological exam to test your nerve function and determine how the herniated disk is affecting your nervous system. These diagnostic tools work together to create a complete picture of your condition.
Conservative Treatment Options
Most people with herniated disks improve with conservative, non-surgical treatment. In fact, about 60% to 90% of people recover well from nonsurgical approaches. The goal of conservative treatment is to manage pain, reduce inflammation, and allow your disk to heal naturally.
Pain Management at Home
Initially, you can treat herniated disk pain at home with several strategies: These approaches are effective for most people and should be your first line of defense.
- Over-the-counter pain relievers such as ibuprofen or naproxen
- Ice packs or heat therapy applied to the affected area
- Rest and activity modification
- Gentle stretching and mild movement
- Proper ergonomics and body mechanics
Physical Therapy and Exercise
Despite initial pain, maintaining gentle movement is crucial for recovery. Staying completely immobilized can actually worsen stiffness and prolong healing. Your healthcare provider may recommend specific stretches and exercises designed to improve flexibility, strengthen core muscles, and reduce pressure on the affected disk. Physical therapy should be tailored to your specific condition and pain level, gradually increasing intensity as you improve.
Advanced Conservative Treatments
When home treatment isn’t sufficient, your healthcare provider may recommend advanced non-surgical options:
- Prescription-strength anti-inflammatory medications
- Epidural steroid injections to reduce inflammation around the nerve
- Nerve blocks to temporarily relieve pain
- Specialized physical therapy programs
- Chiropractic care or manipulation therapy
Epidural steroid injections are particularly effective for herniated disks, as they deliver anti-inflammatory medication directly to the area where the disk is pressing on the nerve. These injections can provide significant pain relief, allowing you to participate more effectively in physical therapy.
Surgical Treatment Options
Surgery is recommended only when conservative treatments fail to provide relief after six weeks or longer, or when symptoms are severe and significantly impacting your quality of life. Your provider might recommend surgical intervention if you experience:
- Persistent, unbearable pain despite conservative treatment
- Significant difficulty walking or performing daily activities
- Bladder or bowel dysfunction
- Severe numbness or progressive muscle weakness
Microdiskectomy
The most common surgical procedure for herniated disks is called a microdiskectomy. This minimally invasive spine surgery involves making a small incision through the skin near the affected disk. Your surgeon will insert a microscope and small specialized tools through the incision to precisely remove the herniated portion of the disk that is pressing on the nerve. The beauty of this approach is that only the damaged portion of the disk is removed, preserving the healthy disk material. This minimally invasive technique results in less tissue damage, reduced blood loss, and faster recovery compared to traditional open surgery.
Other Surgical Approaches
Depending on your specific condition and the location of the herniation, your surgeon may recommend alternative surgical options:
- Diskectomy: Removal of part or all of the herniated disk
- Laminectomy: Removal of part of the vertebra to create more space for the nerve
- Anterior Cervical Diskectomy and Fusion (ACDF): Removal of the disk followed by fusion of the vertebrae to stabilize the spine
- Open diskectomy: Traditional approach with a larger incision for direct access to the spine
Your surgeon will choose the most appropriate technique based on your imaging results, the location and severity of the herniation, and your overall health status. A diskectomy typically takes one to two hours, depending on the complexity of your case.
Recovery and Long-term Management
Recovery from a herniated disk varies depending on whether you pursue conservative or surgical treatment. With conservative care, most people experience significant improvement within four to six weeks. Post-surgical recovery typically involves a gradual return to normal activities over several weeks to months.
Following your healthcare provider’s recommendations is essential for optimal recovery. This may include continuing physical therapy exercises, maintaining proper posture, gradually increasing activity levels, and following any activity restrictions your provider recommends.
Prevention Strategies
While it’s not always possible to prevent a herniated disk, you can significantly reduce your risk by implementing healthy lifestyle habits:
- Maintain proper lifting techniques, bending at the knees and keeping your back straight
- Stay physically active with regular exercise to strengthen core muscles
- Maintain a healthy weight to reduce stress on your spine
- Practice good ergonomics when sitting, standing, and working
- Avoid smoking, which can weaken disk material
- Take regular breaks during prolonged sitting or repetitive activities
- Sleep on a supportive mattress with proper pillow alignment
- Manage stress effectively, as tension can contribute to muscle tightness
When to See a Healthcare Provider
While many herniated disks resolve on their own, you should see a healthcare provider if:
- Pain persists beyond four to six weeks
- Symptoms are getting worse rather than improving
- You experience severe pain that significantly affects your daily activities
- You develop numbness or weakness in your legs or arms
- You have difficulty walking or maintaining balance
- You experience bladder or bowel dysfunction
- Pain radiates down your leg or arm
Early evaluation and intervention can prevent complications and help you return to your normal activities more quickly.
Frequently Asked Questions
Q: How long does it take for a herniated disk to heal?
A: Most herniated disks heal on their own within four to six weeks with appropriate conservative treatment. However, some cases may take longer, and symptoms may persist if the herniation is severe or affecting multiple nerves. Your healthcare provider can give you a more specific timeline based on your individual condition.
Q: Can a herniated disk heal without surgery?
A: Yes, approximately 60% to 90% of people recover completely from a herniated disk without surgery. Conservative treatment including rest, physical therapy, anti-inflammatory medications, and activity modification is successful for most cases. Surgery is reserved for persistent cases that don’t respond to conservative treatment.
Q: What should I avoid if I have a herniated disk?
A: Avoid heavy lifting, repetitive bending, prolonged sitting in one position, high-impact activities, and smoking. Don’t remain completely immobilized, as gentle movement and stretching are beneficial. Follow your healthcare provider’s specific recommendations for activity restrictions.
Q: Is it safe to exercise with a herniated disk?
A: Yes, gentle exercise and stretching are actually recommended and beneficial. Staying active helps maintain muscle strength and flexibility, which supports healing. However, you should follow your healthcare provider’s recommendations and avoid movements that increase pain. Physical therapy can guide you through safe, therapeutic exercises.
Q: Can a herniated disk cause permanent damage?
A: Most herniated disks do not cause permanent damage when treated appropriately. However, if a herniated disk causes prolonged nerve compression without treatment, it could potentially lead to permanent nerve damage. This is why seeking timely medical attention is important, especially if you experience progressive weakness or numbness.
Q: What questions should I ask my healthcare provider?
A: Consider asking about the location and severity of your herniation, the expected timeline for healing, which activities to avoid, what exercises are safe for your condition, whether imaging studies are necessary, when to follow up, and what warning signs should prompt immediate medical attention. Understanding your condition helps you make informed decisions about your care.
References
- Herniated Disk (Slipped or Bulging Disk) — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/12768-herniated-disk
- Diskectomy: What It Is, Purpose, Procedure & Recovery — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/procedures/discectomy
- Herniated Disc Symptoms & Treatment — Cleveland Clinic Abu Dhabi. 2024. https://www.clevelandclinicabudhabi.ae/en/health-hub/health-resource/diseases-and-conditions/herniated-disc
- A Guide to Herniated Discs: Symptoms, Diagnosis, and Treatment — SIOrthopedic. 2024. https://siortho.com/blog/spine/herniated-disc-treatment-options/
- Minimally Invasive Spine Surgery: Procedure, Risks & Benefits — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/treatments/17235-minimally-invasive-spine-surgery
- Healing a Herniated Disk: Causes, Treatment & Prevention — Cleveland Clinic Health Essentials Podcast. 2024. https://my.clevelandclinic.org/podcasts/health-essentials/healing-a-herniated-disk-dr-dominic-pelle
Read full bio of Sneha Tete











