Hidradenocarcinoma Pathology: Clinical, Histology, IHC Guide
Detailed pathology of hidradenocarcinoma, a rare aggressive sweat gland carcinoma with diagnostic challenges and metastasis risks.
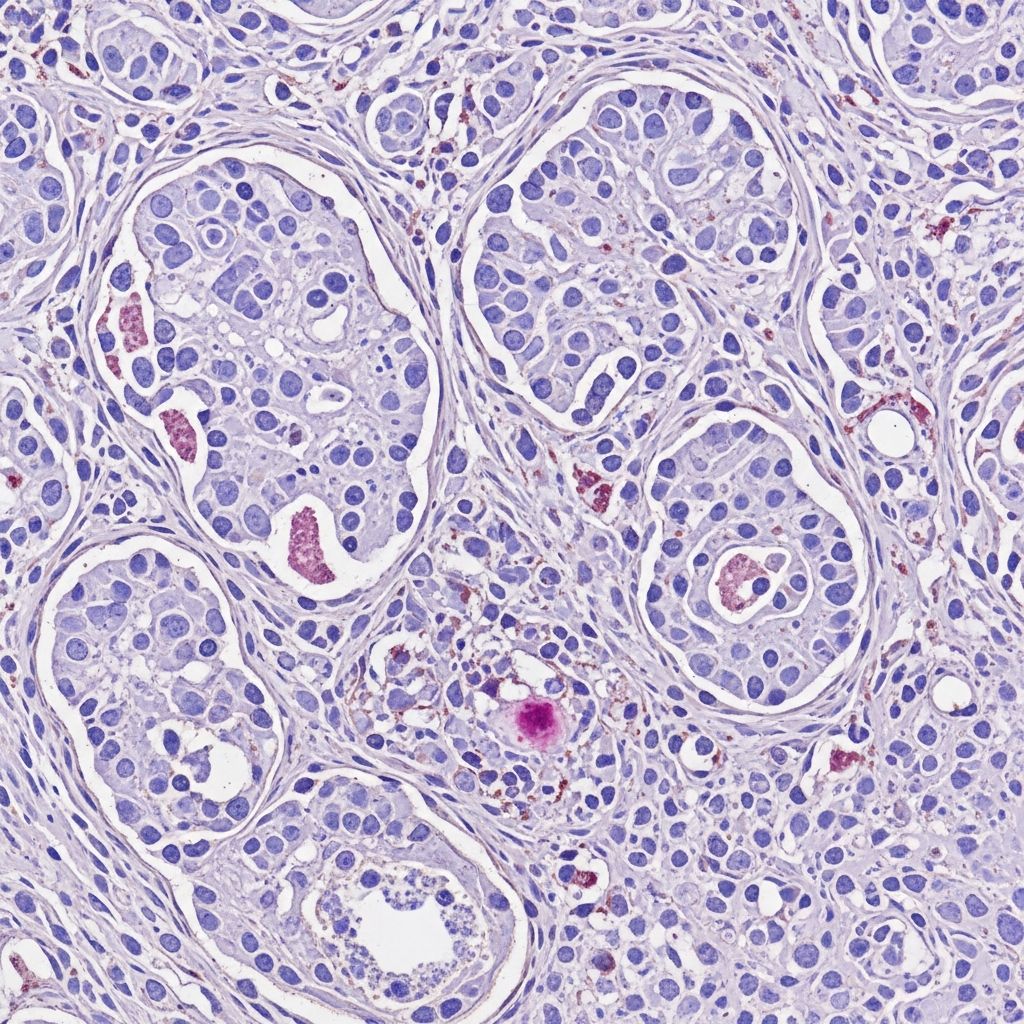
Hidradenocarcinoma pathology
Hidradenocarcinoma is a rare and aggressive sweat gland carcinoma originating from eccrine or apocrine glands, affecting a wide age range and various anatomic sites, often presenting diagnostic challenges due to its similarity to benign lesions.
Clinical features
Hidradenocarcinomas typically manifest as large, nodular, dermally based tumours, often exceeding 1-5 cm in size, with a firm, subcutaneous feel that may ulcerate or show telangiectasia. These lesions can arise de novo or from pre-existing hidradenomas, mimicking benign solitary skin nodules, erythematous plaques, or fleshy red-violet growths with slow circumferential expansion. Common sites include the head and neck, though extremities and trunk involvement occurs; patients may remain asymptomatic despite aggressive behaviour, including local invasion into subcutaneous fat and dermis. Metastasis to regional lymph nodes precedes distant spread to lungs, bones, or viscera in up to 60% of cases, with nodal involvement in 39% and visceral in 28%. Incidence is low, around 0.05% of skin cancers or 1 in 13,000 dermatopathology biopsies, making it <0.01% of all cutaneous malignancies.
HistoPathology
Grossly, hidradenocarcinomas appear as well-circumscribed superficial skin nodules, but microscopy reveals irregular infiltration into surrounding dermis and subcutaneous fat. Tumour cells exhibit pleomorphic morphology: epithelioid with clear cell changes, basaloid patterns, or eosinophilic cytoplasm; darker fusiform/spindle cells with atypical mitoses and nuclear pleomorphism coexist with larger clear cells. Key malignant features include:
- Infiltrative growth pattern with tumour cords invading peripherally
- Ductal and squamous differentiation, cystic spaces, and apocrine features
- Necrosis, vascular/perineural/lymphovascular invasion, and deep extension
- Loss of circumscription, high mitotic activity (especially in clear cells), and remnants of nodular hidradenoma.
Not all cases show universal infiltration; some remain deceptively bland, complicating diagnosis. Metastatic deposits, such as in lung tissue, mirror primary histology with epithelioid cells and ductal foci.
Cytology description
Cytologically, aspirates or imprints display cohesive clusters of epithelioid cells with eosinophilic or clear cytoplasm, vesicular nuclei, prominent nucleoli, and atypical mitoses; background may include necrosis or myxoid stroma. Ductal lumina and tubular structures are evident, distinguishing from purely squamous or basaloid neoplasms.
Histopathology images
- Figure 1: Large nodular dermal tumour invading subcutaneous fat with eosinophilic cells.
- Figure 2: Irregular dermal infiltration, squamous differentiation, and duct formation.
- Figure 3: Epithelioid cells with clear cell changes.
- Figure 4: Areas of tumour necrosis.
- Figure 5: Metastatic deposit in lung parenchyma.
Immunohistochemistry
Hidradenocarcinomas are typically positive for CK7, epithelial markers like pankeratin (AE1/AE3), and ductal markers such as CEA highlighting lumina; partial positivity for EMA and CK15 is common. p63 expression favours primary adnexal origin, while D2-40 positivity aids in distinguishing from metastases. Negative or variable staining for S100, SOX10, and GCDFP-15 differentiates from other adnexal or metastatic tumours; Ki67 proliferation index is high.
Differential diagnosis
Distinguishing hidradenocarcinoma from mimics requires integrating clinical size (>1 cm), invasion, and IHC:
| Entity | Key Differentiators from Hidradenocarcinoma |
|---|---|
| Nodular hidradenoma | Benign, circumscribed, no invasion/subcutis involvement, low mitoses; recommend excision due to malignant potential. |
| Clear cell acrospiroma | Epidermal connection, less pleomorphism, no deep invasion. |
| Digital papillary adenocarcinoma | Acral location, prominent papillary ducts, S100+. |
| Metastatic carcinoma | p63-, known primary, organ-specific IHC (e.g., TTF1 lung). |
| Epithelioid sarcoma | SMARCB1 loss, proximal/subungual sites, less ductal differentiation. |
Malignancy is favoured by subcutis invasion, lymphovascular invasion, infiltrative borders, and large size; absence of some features does not exclude diagnosis.
Treatment and prognosis
Wide local excision with 2 cm margins is mainstay, often including sentinel lymph node biopsy due to >50% recurrence and 60% metastasis risk; adjuvant radiotherapy (50-70 Gy) improves local control, though controversial. Chemotherapy (5-FU/capecitabine) or targeted therapies (EGFR inhibitors, PI3K/Akt/mTOR) are considered for advanced disease, but no standardized guidelines exist owing to rarity. Prognosis is guarded: high locoregional recurrence; long-term follow-up with imaging (CT/MRI/PET) essential.
Frequently Asked Questions
What is hidradenocarcinoma?
A rare, aggressive sweat gland malignancy arising from eccrine/apocrine ducts, often mimicking benign hidradenoma.
How is hidradenocarcinoma diagnosed?
Via histopathology showing invasion/mitoses and IHC (CK7+, p63+, CEA ductal+); imaging rules out metastasis.
What are the common sites and symptoms?
Head/neck most frequent; presents as asymptomatic nodule/plaque, may ulcerate; metastasis to nodes/lungs.
Is hidradenoma always benign?
No, it may transform; excise all due to ~50% recurrence risk if malignant.
What is the treatment?
Wide excision ± lymph node dissection, radiotherapy; chemotherapy for metastatic cases.
This article synthesizes pathology insights, emphasizing early recognition for better outcomes in this underdiagnosed entity. (Word count: 1678)
References
- Hidradenocarcinoma pathology — DermNet New Zealand. 2023. https://dermnetnz.org/topics/hidradenocarcinoma-pathology
- Current management approach to hidradenocarcinoma: a comprehensive review of the literature — ecancer (de A Soni et al.). 2015-06-01. https://ecancer.org/es/journal/article/517-current-management-approach-to-hidradenocarcinoma-a-comprehensive-review-of-the-literature
- Hidradenocarcinoma — Anais Brasileiros de Dermatologia (AA de Lima et al.). 2021. https://www.anaisdedermatologia.org.br/en-hidradenocarcinoma-articulo-S0365059621000210
Read full bio of medha deb