Osteoarthritis Of The Hip: Diagnosis, Treatment, Exercise Guide
Understand hip osteoarthritis symptoms, causes, diagnosis, and effective treatments to manage pain and improve mobility.
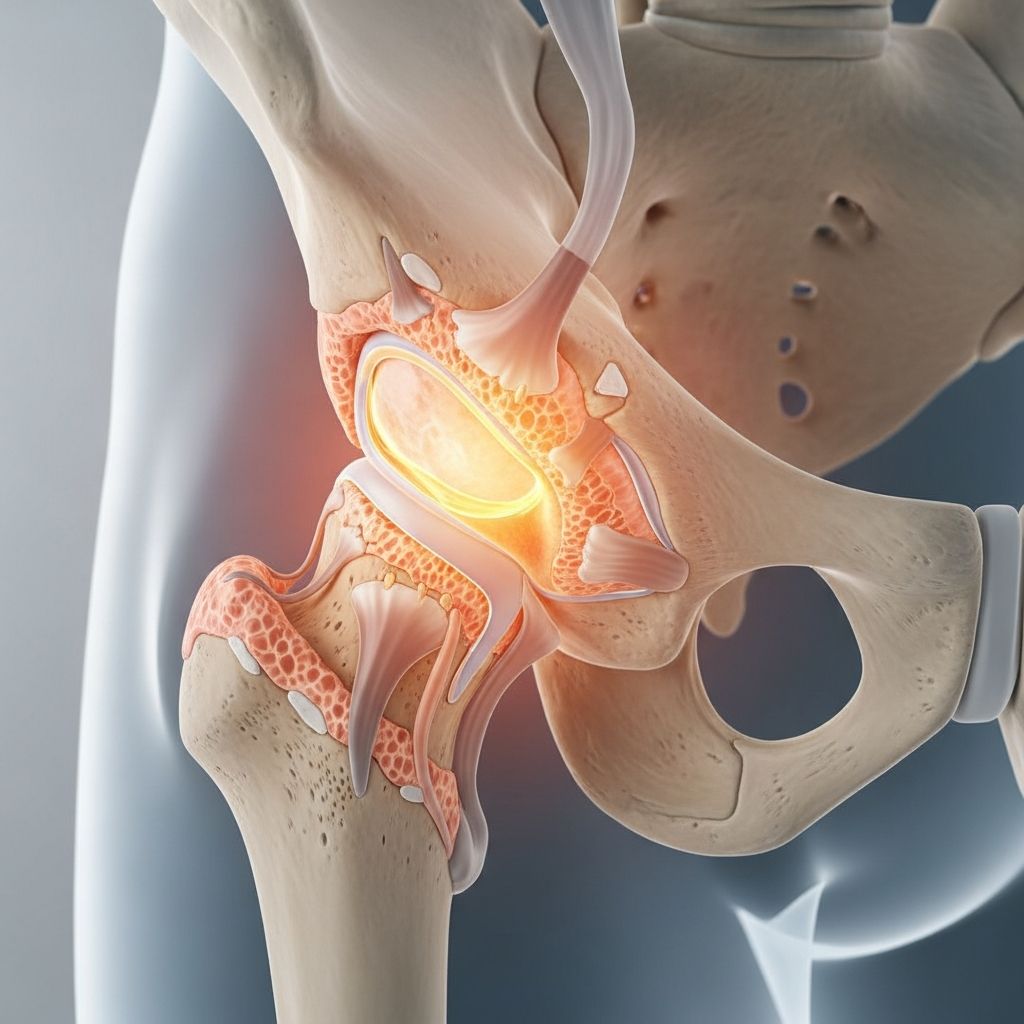
Hip osteoarthritis (OA) is a degenerative joint disease where the protective cartilage in the hip joint wears away over time, leading to bone-on-bone friction, pain, and reduced mobility. While there is no cure, a combination of lifestyle changes, therapies, medications, and surgery can significantly ease symptoms and improve quality of life.
What is Osteoarthritis of the Hip?
The hip is the body’s second-largest weight-bearing joint, after the knee. It functions as a ball-and-socket structure, with the ball at the top of the femur (thigh bone) fitting into the acetabulum socket of the pelvis. Smooth cartilage covers these surfaces, enabling frictionless movement and absorbing shock during activities like walking or running.
In hip OA, this cartilage gradually deteriorates. The joint space narrows, bone ends become rough, and bone spurs (osteophytes) form. This causes inflammation, pain, and mechanical issues like grinding or locking. OA is the most common form of arthritis, affecting millions, and hip involvement often limits daily activities such as climbing stairs or tying shoes.
Risk factors include age (most common over 50), obesity (extra weight stresses the joint), previous hip injuries, genetics, and structural issues like hip dysplasia or femoroacetabular impingement (FAI). Women are more prone due to wider pelvises altering joint mechanics.
Symptoms of Hip OA
Symptoms develop gradually and intensify over time, often worsening after inactivity like morning stiffness lasting 30 minutes or more.
- Pain: Primarily in the groin, but can radiate to the thigh, buttocks, or knee. Activity-related pain is common, easing with rest initially but persisting later.
- Crepitus: Grinding, clicking, or catching sensations during movement due to roughened surfaces.
- Stiffness: Reduced flexibility, making bending, walking, or putting on socks difficult.
- Limited Range of Motion: Leads to limping, altered gait, and muscle weakness from disuse.
- Other Signs: Swelling, instability, or pain at night.
In advanced stages, constant pain and severe mobility loss may necessitate interventions like joint replacement.
Diagnosing Hip OA
Diagnosis starts with a medical history and physical exam. Doctors assess:
- Range of motion in multiple directions.
- Signs of injury or tenderness.
- Crepitus or grinding during movement.
- Gait abnormalities, like limping.
- Pain on hip pressure or rotation.
Imaging confirms the diagnosis:
- X-rays: Show joint space narrowing, bone spurs, and sclerosis.
- MRI: Detects soft tissue damage, cartilage loss, or labral tears, useful for early or atypical cases.
Blood tests rule out inflammatory arthritis like rheumatoid arthritis (RA), which symmetrically affects both hips.
Treatments for Hip OA
Treatment focuses on symptom relief, function preservation, and delaying progression. Options span non-drug, medications, and surgery.
Non-Drug Treatments
Self-care forms the foundation:
- Weight Management: Losing 5-10% body weight reduces joint load significantly.
- Exercise: Strengthens supporting muscles (glutes, core), improves flexibility, and reduces pain. Water aerobics, swimming, cycling, and tai chi are ideal low-impact options.
- Physical/Occupational Therapy: Customized programs enhance stability and daily function.
- Assistive Devices: Canes, walkers, or shoe lifts improve gait and offload the joint.
- Hot/Cold Therapy: Heat relaxes muscles; ice reduces inflammation.
- Complementary Therapies: Acupuncture, massage, topical capsaicin/CBD creams.
Studies show 12-week exercise programs reduce pain by 30%, boost strength by 20%, and improve mobility.
Medications
For moderate pain:
- Acetaminophen: First-line for mild pain.
- NSAIDs: Ibuprofen or naproxen reduce inflammation (oral/topical).
- Corticosteroid Injections: Provide temporary relief (3-6 months).
- Hyaluronic Acid Injections: Lubricate the joint, though evidence is mixed.[10]
Always consult a doctor for personalized regimens, considering risks like GI issues with NSAIDs.[10]
Surgical Options
For severe, unresponsive cases:
| Procedure | Description | Best For |
|---|---|---|
| Hip Resurfacing | Caps damaged bone with metal shell; preserves more bone. | Younger, active patients. |
| Total Hip Replacement (Arthroplasty) | Replaces socket and femoral head with metal/plastic/ceramic implants. | Advanced OA; over 300,000/year. |
| Osteotomy | Cuts/shaves bones to realign joint. | Rare; younger patients with malalignment. |
Pre-surgery (‘pre-hab’) exercises don’t significantly improve outcomes, but post-op rehab is crucial.
Exercise Benefits for Hip OA
Regular activity is vital. Goals: Strengthen hip stabilizers (gluteus medius), enhance aerobic fitness, and increase flexibility.
- Strengthening: Bridges, clamshells, side leg raises target deep rotators.
- Aerobic: Walking, elliptical, aquatics (buoyancy unloads joints).
- Flexibility: Gentle stretches for hip flexors, hamstrings.
A 2017 Finnish study: 12 weeks of exercise cut pain 30%, improved strength 20%, ROM 30%. A 2016 trial: Better pain/mobility vs. controls.
Aquatic therapy excels: Shoulder-deep water supports weight while building resistance.
Living with Hip OA
Manage flares with rest, ice, and meds. Ongoing research via Arthritis Foundation’s HipOA/FastOA identifies rapid progressors (e.g., post-dysplasia surgery) using MRI biomarkers and risk calculators.
Stem cell therapies show promise for cartilage repair, potentially delaying replacements.
Frequently Asked Questions (FAQs)
Q: How does hip OA differ from RA?
A: OA is degenerative (wear-and-tear); RA is autoimmune, symmetric, with more swelling.
Q: Can exercise worsen hip OA?
A: Low-impact no; high-impact yes. Start slow with PT guidance.
Q: When is hip replacement needed?
A: Severe pain limiting daily life despite conservative treatments.
Q: Does weight loss help?
A: Yes, reduces joint stress dramatically.
Q: Are injections a cure?
A: No, temporary relief only.[10]
References
- Osteoarthritis of the Hip — Arthritis Foundation. 2021-10-15. https://www.arthritis.org/health-wellness/about-arthritis/understanding-arthritis/hip-osteoarthritis
- When Hip Pain May Mean Arthritis — Arthritis Foundation. N/A. https://www.arthritis.org/health-wellness/about-arthritis/where-it-hurts/when-hip-pain-may-mean-arthritis
- Exercise Benefits for Hip Osteoarthritis — Arthritis Foundation. N/A. https://www.arthritis.org/health-wellness/healthy-living/physical-activity/getting-started/exercise-benefits-for-hip-osteoarthritis
- HipOA Awards Advance Osteoarthritis Research — Arthritis Foundation. 2025-09-25. https://www.arthritis.org/news/news-and-events/hipoa-awards-advance-osteoarthritis-research
- Osteoarthritis: Symptoms, Diagnosis, and Treatment — Arthritis Foundation. N/A. https://www.arthritis.org/diseases/osteoarthritis
- Physical Therapy for Hip Arthritis — Arthritis Foundation. N/A. https://www.arthritis.org/health-wellness/treatment/complementary-therapies/physical-therapies/physical-therapy-for-hip-arthritis-how-to-exercise
Read full bio of Sneha Tete











