Postnasal Drip: How To Get Rid Of It With Proven Remedies
Effective remedies and treatments for postnasal drip relief, from home strategies to medical interventions.
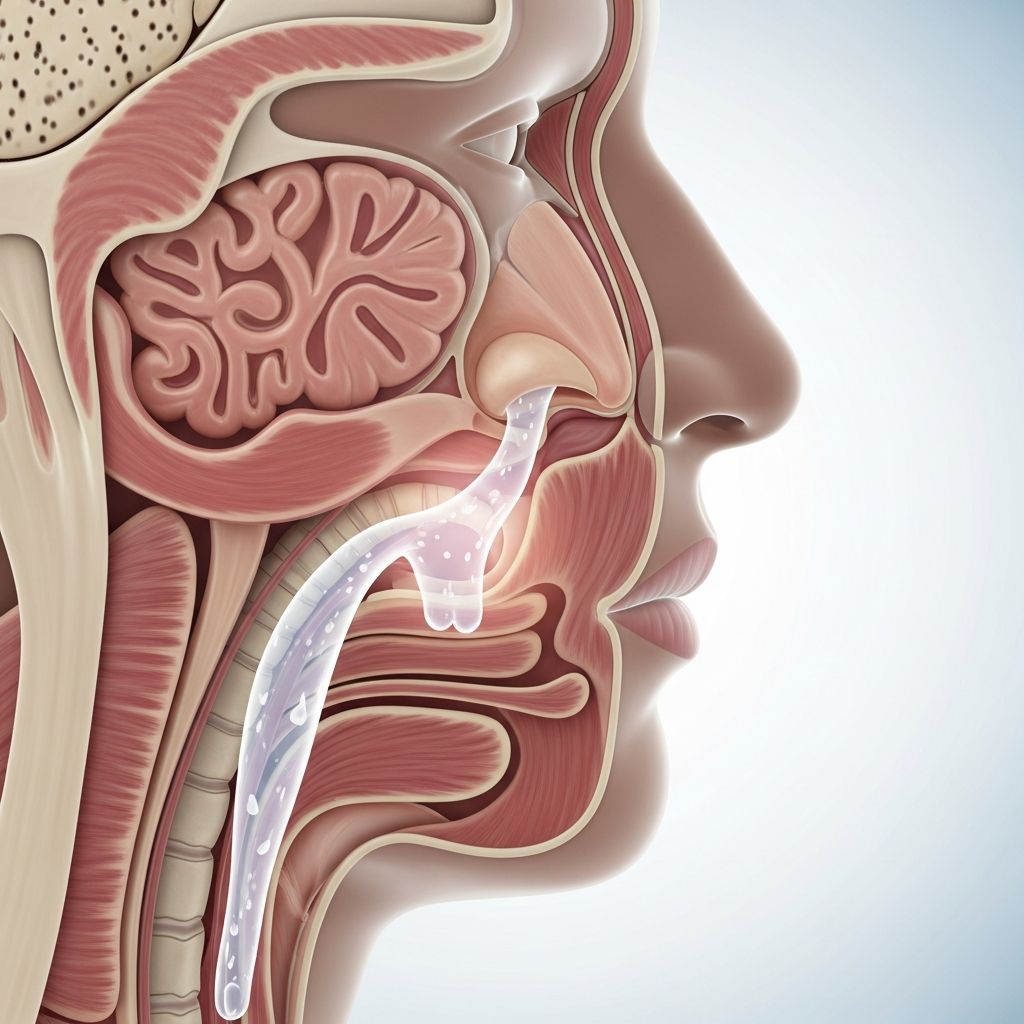
How to Get Rid of Postnasal Drip
Postnasal drip occurs when excess mucus from the nose and sinuses drips down the back of the throat, causing irritation, frequent throat clearing, and discomfort. This common condition affects millions and can stem from various triggers like allergies, infections, or environmental factors.
What Is Postnasal Drip?
Postnasal drip refers to the sensation of mucus drainage into the pharynx, often due to obstruction of normal nasal drainage or increased secretion from the paranasal sinuses. It is characterized by a feeling of mucus dripping from the back of the nose into the throat, leading to frequent swallowing, throat clearing, raspy speech, and a sore throat. The mucus can vary in viscosity—serous (thin and watery) or mucoid (thicker)—and is associated with symptoms like rhinorrhea or throat discomfort.
Normally, mucus produced by the nasal lining, sinuses, and throat keeps these areas moist and filters breathed air. However, excess or thickened mucus becomes problematic, making swallowing difficult and prompting coughs or throat clearing, especially at night, which disrupts sleep. Discolored or foul-smelling mucus may indicate sinusitis.
Symptoms of Postnasal Drip
Common symptoms include:
- Feeling of mucus drainage into the throat
- Frequent need to swallow or clear the throat
- Raspy or gurgling speech
- Sore, irritated throat or sensation of a lump
- Cough, particularly chronic or nighttime cough
- Rhinorrhea (runny nose)
- Nasal stiffness or postnasal pruritus (itching)
- Throat discomfort, worsened by viscous mucus
In chronic idiopathic postnasal drip (CIPND), patients may experience persistent symptoms without a clear underlying diagnosis, with 30.3% reporting cough—a rate higher than the general population—and accompanying symptoms like nasal stiffness linked to higher recurrence. Swelling of throat tissues without infection can exacerbate discomfort.
Causes of Postnasal Drip
Postnasal drip arises from multiple factors:
- Allergies and Rhinitis: Swelling of the nasal lining (rhinitis), often allergy-induced, is a primary cause.
- Infections: Bacterial, viral (colds, flu), leading to thin clear secretions that may thicken and discolor if bacterial sinusitis develops.
- Vasomotor Rhinitis: Overly sensitive nose reacting to non-allergic triggers like temperature changes or pollution.
- Gastroesophageal Reflux: Stomach acid reflux causes nasal and throat swelling, mimicking or worsening drip.
- Medications and Age: Some drugs thicken mucus; age-related changes alter mucus production.
- Chronic Idiopathic Cases: No identifiable cause, potentially linked to anatomical factors or sensory hyper-reactivity, with cough controversy unresolved.
- Other: Nasal polyps, sinusitis (acute/chronic), laryngopharyngeal reflux, or even malignancies in rare cases.
Thin clear secretions often tie to allergies or colds; green/yellow thick mucus signals bacterial infection.
When to See a Doctor for Postnasal Drip
Seek medical attention if symptoms persist beyond 10 days, worsen, or include fever, severe headache, facial pain, bloody mucus, wheezing, or foul-smelling discharge indicating sinusitis. Chronic cases with cough, nasal stiffness, or recurrence after treatment warrant evaluation for underlying issues like allergies or anatomical problems. An ENT specialist may perform endoscopy, allergy testing, or lung exams.
How to Get Rid of Postnasal Drip: Treatment Options
Treatment targets the cause and symptoms. About 71.6% of chronic idiopathic cases respond to first-generation antihistamine-decongestants, though 25.9% recur, especially with nasal stiffness.
Home Remedies and Lifestyle Changes
Start with non-invasive options:
- Nasal Irrigation: Saline nasal rinses (neti pot or squeeze bottle) flush mucus, allergens, and irritants. Use distilled water to avoid infections.
- Humidification: Use a cool-mist humidifier to moisten air, thinning mucus. Clean regularly to prevent mold.
- Hydration: Drink plenty of fluids to thin secretions.
- Elevation: Sleep with head elevated to reduce drainage.
- Steam Inhalation: Breathe steam from hot showers or bowls to loosen mucus.
- Avoid Triggers: Steer clear of allergens, smoke, pollutants, spicy foods, dairy (if sensitizing).
Over-the-Counter Medications
| Medication Type | Examples | Benefits | Notes |
|---|---|---|---|
| Decongestants | Pseudoephedrine | Reduces nasal swelling, improves drainage | May cause rebound congestion; limit to 3 days |
| Antihistamines | First-gen (diphenhydramine); non-sedating (loratadine) | Dries secretions; first-gen effective in 71.6% of idiopathic cases | Sedating types thicken mucus more |
| Nasal Sprays | Steroid (fluticasone), saline | Reduces inflammation | Steroids for allergies; avoid overuse |
| Expectorants | Guaifenesin | Thins mucus | Combine with hydration |
Prescription Treatments
- Steroid Nasal Sprays: For rhinitis/sinusitis.
- Anticholinergic Sprays: Reduce mucus production.
- Oral Steroids: Short-term for severe inflammation.
- Antibiotics: Only for confirmed bacterial sinusitis.
- Immunotherapy: Allergy shots for persistent allergies.
Procedures and Surgery
For refractory cases:
- Inferior Turbinate Reduction: Shrinks swollen nasal tissue.
- Posterior Nasal Nerve Ablation: Disrupts nerves overproducing mucus.
- Endoscopic Sinus Surgery: Clears blocked sinuses if needed.
Anatomical issues like nasal stiffness predict higher recurrence post-medication.
Prevention Tips for Postnasal Drip
- Maintain nasal hygiene with daily saline rinses.
- Manage allergies proactively with avoidance and meds.
- Stay hydrated and use humidifiers in dry environments.
- Elevate head during sleep.
- Control reflux with diet (avoid triggers) and elevation.
- Quit smoking and avoid irritants.
Frequently Asked Questions (FAQs)
What causes postnasal drip at night?
Gravity promotes drainage when lying down; allergies, reflux, or dry air worsen it.
Does postnasal drip cause cough?
Yes, in 30.3% of cases, possibly via sensory hyper-reactivity rather than direct mucus irritation.
How long does postnasal drip last?
Varies by cause: 7-10 days for colds; chronic if untreated. Idiopathic cases may recur.
Is postnasal drip contagious?
Only if caused by infection like a cold; allergy-related is not.
Can dehydration worsen postnasal drip?
Yes, it thickens mucus, intensifying symptoms.
Are antihistamines safe for postnasal drip?
First-generation types help idiopathic cases effectively; consult a doctor for long-term use.
References
- Clinical Aspects of Chronic Idiopathic Postnasal Drip: An Entity Not to be Overlooked — Lee JY et al. PMC. 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC11215627/
- Post-Nasal Drip — American Academy of Otolaryngology—Head and Neck Surgery. 2021. https://www.enthealth.org/wp-content/uploads/2021/09/Post-nasal_Drip_2021.pdf
- Postnasal Drip — Chiu J, Rowan NR. JAMA Otolaryngology–Head & Neck Surgery. 2025-04-17. https://jamanetwork.com/journals/jamaotolaryngology/fullarticle/2830355
Read full bio of Sneha Tete











