Hyperkeratosis Of The Nipple And Areola: Causes & Treatment
Explore the causes, symptoms, diagnosis, and management of hyperkeratosis of the nipple and areola, a benign yet uncommon skin condition.
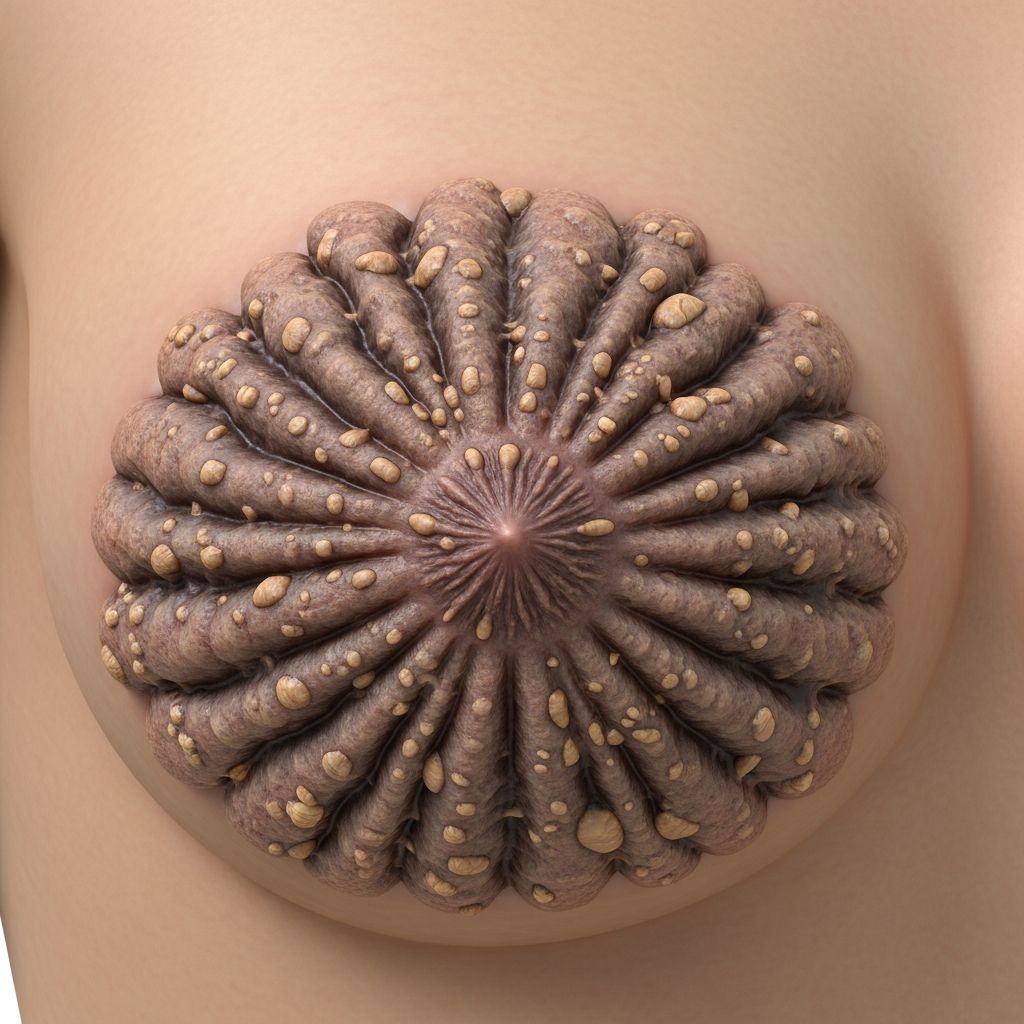
Hyperkeratosis of the nipple and areola is a rare dermatological condition characterized by warty, pigmented thickening of the skin on the nipples, areolae, or both. This benign disorder can be primary (idiopathic or nevoid) or secondary to underlying conditions, often presenting without pain or discharge but sometimes with pruritus.
Introduction
Also known as nevoid hyperkeratosis or hyperkeratosis areolae mammae naeviformis, this condition involves excessive keratin buildup leading to rough, verrucous plaques. It primarily affects the nipple-areola complex and is typically asymptomatic, though cosmetic concerns and itching may prompt medical attention. Early recognition is crucial to rule out malignancy, especially in unilateral cases with alarming features.
Demographics
Hyperkeratosis of the nipple and areola most commonly affects young adults, with onset often during puberty or pregnancy. It can occur unilaterally or bilaterally, with females more frequently reported, though males on estrogen therapy (e.g., for prostate cancer) are also susceptible. Cases have been documented in patients aged 19 to 62 years, including non-pregnant individuals with regular menstrual cycles.
- Prevalence: Rare, with limited epidemiological data.
- Gender: Predominantly female, but seen in males.
- Age: Puberty onward; pregnancy-associated cases peak in reproductive years.
- Associations: Higher incidence in those with epidermal nevi or on certain medications.
Causes
The exact etiology remains unknown, but several factors are implicated. Primary hyperkeratosis is idiopathic or genetic (nevoid type), while secondary forms link to epidermal nevi, infections, medications, or endocrine changes. No viral DNA has been detected in lesions, ruling out infectious causes like HPV.
- Primary (idiopathic): Sporadic or familial, resembling a nevus.
- Nevoid type: Extension of epidermal nevus to nipple/areola (Levy-Frank type I), often unilateral.
- Secondary causes: Epidermal nevus, ichthyosis hystrix, Darier disease, lichen simplex chronicus, or friction.
- Drug-induced: Estrogens, spironolactone, vemurafenib (BRAF inhibitor for melanoma).
- Pregnancy-associated: Hormonal influences (estrogen, progesterone) cause darkening and thickening, often resolving postpartum.
Histologically, estrogen and genetic factors may play roles, but most experts view it as an independent entity.
Clinical Features
Lesions present as bilateral or unilateral, diffuse verrucous thickening with brown hyperpigmentation of the nipple, areola, or both. The skin appears warty, rough, and thickened without erythema, induration, tenderness, bleeding, or discharge in most cases. Pruritus affects some patients, and in severe instances, scabbing or purulent discharge may occur.
Physical exam reveals:
- Pigmented, thickened nipple-areola complex (~2 cm diameter lesions with clear boundaries).
- Deepened skin texture, protuberant hyperkeratosis.
- No palpable masses or lymphadenopathy typically.
- In males on estrogen: Possible gynecomastia.
Symptoms worsen gradually; pregnancy may exacerbate pigmentation and thickness, potentially complicating breastfeeding.
Complications
While benign and non-malignant, complications include:
- Severe pruritus: Impacts quality of life, leading to psychological distress.
- Cosmetic distress: Visible warty plaques cause embarrassment.
- Breastfeeding difficulty: Significant nipple involvement hinders latching.
- Secondary infection: Rare, from scratching-induced excoriations.
- Misdiagnosis: Delay in care if mistaken for malignancy.
Unilateral cases with pain, ulceration, bleeding, discharge, or nipple retraction warrant urgent cancer investigation.
Diagnosis
Diagnosis relies on clinical presentation, dermoscopy, histopathology, and exclusion of differentials. Biopsy is essential for confirmation, especially in atypical cases.
Histopathology: Key features include orthokeratotic hyperkeratosis, papillomatous hyperplasia, acanthosis, elongated rete ridges, basal layer hyperpigmentation, and mild perivascular lymphoeosinophilic infiltrate. No dyskeratosis or basaloid cells (distinguishing from seborrheic keratosis).
Dermoscopy: Useful for non-invasive assessment; shows subepidermal protuberances, network patterns, and hyperpigmentation.
Laboratory tests (hormones, blood work) are usually normal.
Differential Diagnoses
Several conditions mimic hyperkeratosis of the nipple and areola. Pathological exam differentiates them.
| Condition | Key Features | Distinguishing Histology |
|---|---|---|
| Paget disease | Pruritus, burning, erythema, induration, discharge; often unilateral. | Intraepidermal adenocarcinoma cells. |
| Epidermal nevus | Present since birth, verrucous; may extend beyond areola. | Hyperkeratosis, acanthosis (similar but congenital). |
| Acanthosis nigricans | Velvety hyperpigmentation; associated with insulin resistance. | Papillomatosis, minimal hyperkeratosis. |
| Seborrheic keratosis | Sharply demarcated plaques/papules, “stuck-on” appearance. | Basaloid acanthosis, no papillomatosis. |
| Darier disease | Acneiform lesions elsewhere; greasy crusts. | Dyskeratosis, acantholysis. |
| Chronic eczema / Lichen simplex | History of friction/itching; lichenification. | Hypergranulosis, spongiosis. |
| Mycosis fungoides / BCC | Patchy infiltration or pearly nodules. | Lymphocytic infiltrate or basaloid tumor. |
Treatment
No standardized cure exists; management is symptomatic and cosmetic. Options include:
- Topical keratolytics: Urea, salicylic acid, lactic acid, tazarotene to reduce thickening.
- Topical retinoids: Tretinoin or adapalene for hyperkeratosis.
- Corticosteroids: For pruritus (potent topicals short-term).
- Calcipotriol / Vitamin D analogues: Reduce keratinization.
- Laser therapy: CO2, Er:YAG, or pulsed dye for ablation; effective but may recur.
- Cryotherapy / Electrodessication: For localized lesions.
- Surgical excision: Shave or full-thickness for refractory cases.
- Observation: If asymptomatic.
Pregnancy-associated cases often improve postpartum. Discontinue offending drugs if identified.
Outcome
Benign with excellent prognosis; no malignant potential. Recurrence is common post-treatment, especially without addressing underlying causes. Patient education on self-examination and follow-up is key. Regular monitoring advised for unilateral or changing lesions to exclude breast cancer.
Frequently Asked Questions (FAQs)
Q: Is hyperkeratosis of the nipple and areola cancerous?
A: No, it is a benign condition without malignant potential. However, unilateral cases with pain, bleeding, or discharge require investigation for breast cancer.
Q: Does it go away on its own?
A: Primary cases persist lifelong; pregnancy-associated types often improve after delivery. Treatment provides symptomatic relief.
Q: Can it affect breastfeeding?
A: Yes, severe nipple thickening may hinder latching, though it rarely impacts milk production.
Q: What is the best treatment?
A: Topical keratolytics and retinoids are first-line; laser or surgery for persistent cases. Consult a dermatologist.
Q: Who is at risk?
A: Young adults, pregnant women, those on estrogens/spironolactone, or with epidermal nevi.
References
- Severe Bilateral Hyperkeratosis of the Nipples and Areolae — Frontiers in Medicine. 2022-03-15. https://www.frontiersin.org/journals/medicine/articles/10.3389/fmed.2022.781693/full
- Keratotic Lesions on the Nipples and Areolae of a 62-Year-Old Man — American Family Physician (AAFP). 2011-04-15. https://www.aafp.org/pubs/afp/issues/2011/0415/p969.html
- Hyperkeratosis of the Nipple and Areola — MD Searchlight. Recent (post-2022). https://mdsearchlight.com/skin-problems-and-treatments/hyperkeratosis-of-the-nipple-and-areola/
- Dermoscopy and Histopathology of Hyperkeratosis of Nipple and Areola — Dove Press (Clinical, Cosmetic and Investigational Dermatology). Recent (post-2022). https://www.dovepress.com/dermoscopy-and-histopathology-of-hyperkeratosis-of-nipple-and-areola-a-peer-reviewed-fulltext-article-CCID
- Hyperkeratosis of the nipple and areola — DermNet NZ. Recent (post-2022). https://dermnetnz.org/topics/hyperkeratosis-of-the-nipple-and-areola
Read full bio of Sneha Tete