Infantile Digital Fibromatosis: Pathology & Clinical Overview
Comprehensive guide to IDF pathology, diagnosis, and management in infants and children.
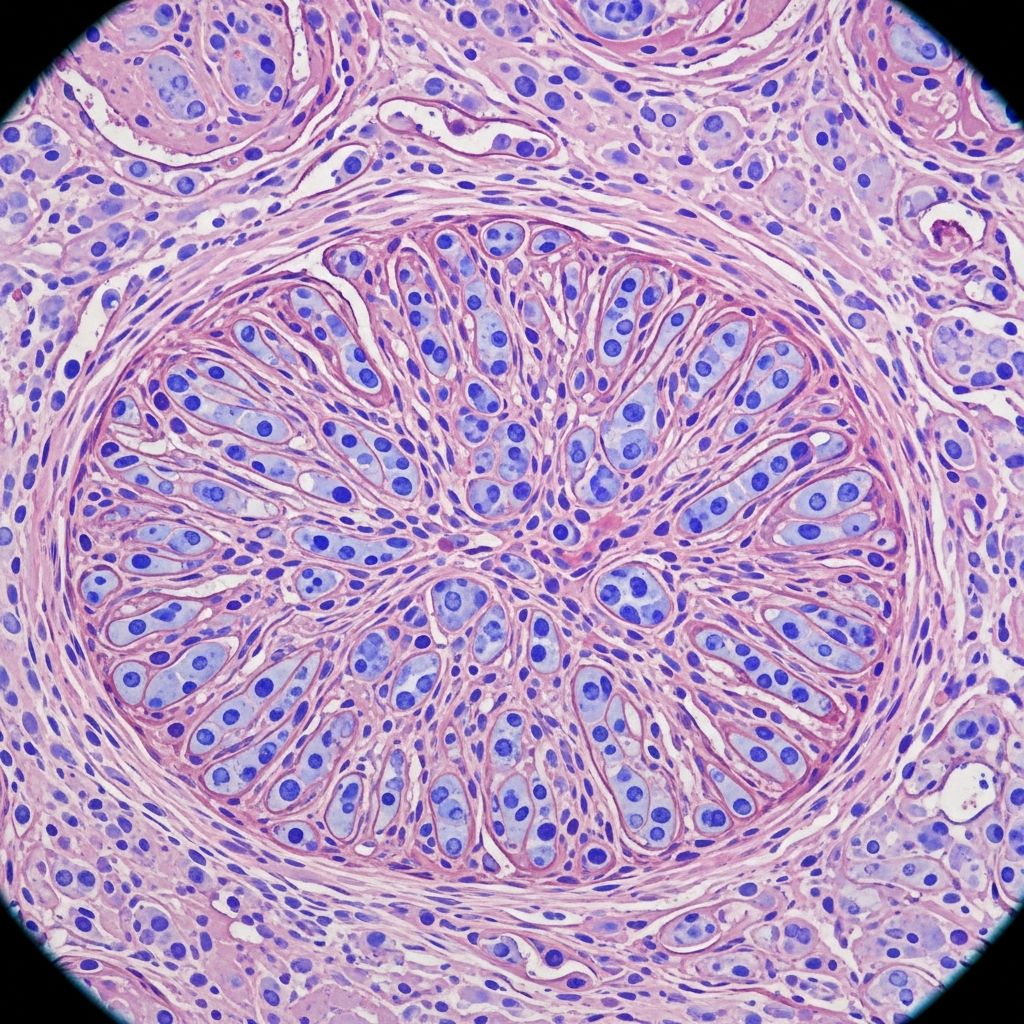
Infantile Digital Fibromatosis: Pathology and Clinical Overview
Introduction
Infantile digital fibromatosis (IDF), also known as inclusion body fibromatosis or Reye’s tumor, is a rare benign tumor that typically presents as a small, asymptomatic nodule in the dermis of fingers or toes in infants and young children. With approximately 200 documented cases in medical literature, IDF remains an uncommon diagnosis that many clinicians encounter infrequently. This condition is characterized by distinctive pathological features, including spindle-shaped cells with characteristic inclusion bodies that aid in differentiation from other fibrous skin diseases.
Originally described by Reye in 1965, IDF has since been recognized as a distinct entity with well-characterized clinical and histopathological features. Understanding the pathology, clinical presentation, and diagnostic criteria of IDF is essential for accurate diagnosis and appropriate management of affected children.
Definition and Nomenclature
Infantile digital fibromatosis is defined as a benign proliferative tumor composed of spindle-shaped cells with characteristic paranuclear inclusion bodies. The condition has multiple synonyms in the medical literature, reflecting its historical confusion with other fibrous proliferations:
- Inclusion body fibromatosis
- Reye’s tumor
- Multiple hyaline fibromatosis
- Infantile dermal fibromatosis
- Subdermal fibromatosis tumor of infancy
- Juvenile dermatofibroma
The nomenclature reflects evolving understanding of the disease. IDF was previously considered a subtype of infantile myofibromatosis (IMF), though it is now recognized as a distinct entity with unique pathological and clinical features.
Pathological Features
Microscopic Histopathology
Microscopic examination of appropriately stained IDF tissues reveals characteristic pathological findings. The tumor typically appears as a non-encapsulated lesion composed of bundles of uniform spindle-shaped cells arranged in an organized pattern within a collagen-rich background.
The spindle cells demonstrate hybrid features combining characteristics of both fibroblasts and myofibroblasts. Myofibroblasts are contractile, spindle-shaped cells identifiable by their expression of α-smooth muscle actin. These cells form interlacing fascicles throughout the dermis, extending from the papillary dermis into the subcutaneous tissue in many cases.
Characteristic Inclusion Bodies
The most distinctive pathological feature of IDF is the presence of paranuclear inclusion bodies within the cytoplasm of spindle cells. These inclusions are composed of densely packed vimentin and actin filaments, which represent the hallmark feature distinguishing IDF from other fibrous skin diseases.
The inclusions appear as eosinophilic structures on standard histological staining and can be confirmed through immunofluorescence staining when necessary. However, demonstration of these filaments through immunofluorescence is not mandatory for diagnosis if the clinical picture and other histological findings are consistent with IDF.
Immunohistochemical Profile
IDF demonstrates a characteristic immunohistochemical profile that supports diagnosis:
- α-smooth muscle actin (α-SMA) – consistently expressed by myofibroblasts in the tumor
- Desmin – positive in the spindle cells
- Calponin – expressed by myofibroblastic components
- Vimentin – prominent in inclusion bodies
- Actin – primary component of paranuclear inclusions
Findings of small lesions centered in the dermis composed of spindle-shaped cells expressing α-smooth muscle actin, desmin, and calponin proteins strongly support an IDF diagnosis.
Clinical Presentation
Typical Presentation
IDF typically presents as a solitary, painless, smooth, dome-shaped nodule with flesh-colored to red appearance. The lesion is usually small and firm, though clinical presentation can vary. The majority of cases present in infancy and early childhood, with most occurring in the first two years of life, and approximately one-third of cases having lesions present since birth.
Location and Distribution
IDF classically affects specific sites with characteristic sparing patterns:
| Location Feature | Details |
|---|---|
| Most Common Sites | Lateral and dorsal aspects of the last four digits (fingers and toes) |
| Typically Spared | Thumb and great toe |
| Rare Locations | Non-digital sites including hands, feet, arms, and other body areas |
| Multiple Lesions | Rare; documented cases range from solitary lesions to up to 74 lesions in exceptional cases |
Size and Characteristics
Most IDF lesions are typically smaller than 2 cm in maximum diameter. However, rare cases of larger tumor-sized lesions, reaching up to 4.5 cm, have been documented. The lesions are usually painless and nonpruritic, though larger lesions may cause pain and compromise function of nearby joints and digits.
In rare instances, lesions may invade the periosteum and erode nearby bone, requiring imaging evaluation to determine the extent of involvement.
Clinical Course and Natural History
IDF characteristically follows an indolent course with spontaneous resolution. The typical progression includes:
- Initial indolent growth phase lasting months to years
- Rapid growth phase occurring over several months in some cases
- Stabilization of tumor size
- Spontaneous regression and resolution without scarring
- Average regression time of 2-3 years, with a range of 1-10 years
Recurrence is common after surgical excision, occurring in a significant proportion of treated cases. This high recurrence rate has led many clinicians to favor conservative management with observation rather than immediate surgical intervention.
Diagnosis and Diagnostic Criteria
Clinical Diagnosis
Diagnosis of IDF is usually based on its characteristic presentation in newborns or young infants combined with histopathological findings. The clinical context—a small, painless nodule on a finger or toe of an infant—provides important diagnostic clues.
Biopsy and Histopathological Analysis
Confirmation of IDF diagnosis requires biopsy or fine needle aspirate analysis of tumor pathology. These analyses should demonstrate the presence of spindle-shaped cells bearing eosinophilic paranuclear inclusions composed of actin and vimentin filaments.
Key diagnostic findings include:
- Non-encapsulated tumor composed of bundles of uniform spindle cells
- Cells combining features of fibroblasts and myofibroblasts
- Collagen fiber-rich background
- Paranuclear inclusions with characteristic appearance
- Positive immunostaining for α-smooth muscle actin, desmin, and calponin
Imaging Considerations
X-ray imaging may be necessary to determine if the lesion involves bone or to assess the extent of involvement, particularly for larger lesions or those with suspected periosteal invasion. Ultrasonographic examination can help characterize soft-tissue involvement and exclude other conditions such as arteriovenous malformations.
Differential Diagnosis
Several conditions should be considered in the differential diagnosis of IDF:
- Infantile myofibromatosis (IMF) – similar presentation but distinct pathological and clinical features; IDF was once considered a subtype of IMF
- Exostosis – bony lump that may be confused clinically; imaging helps differentiate
- Neurofibromatosis – may present with multiple lesions requiring histopathological distinction
- Arteriovenous malformation – can be excluded through imaging studies
- Proteus syndrome – rare genetic condition with multiple tumors
- Other fibrous proliferations – dermatomyositis-associated fibromatosis and other fibroblastic tumors
Age of Presentation and Demographic Features
IDF typically develops during the first year of life, with the majority of cases presenting as sporadic occurrences. The majority of cases (more than 80%) are present in infancy. However, the condition demonstrates variable presentations:
- Congenital onset is rare but documented
- Cases have been reported in children up to age 10
- One case was reported in a 52-year-old adult
- The condition affects both males and females equally
- No clear racial or ethnic predilection has been established
Etiology and Pathogenesis
The cause of infantile digital fibromatosis remains unknown. The tumor appears to arise de novo without clear environmental triggers or hereditary predisposition in most cases. The characteristic inclusion bodies and hybrid myofibroblastic-fibroblastic cell type suggest a unique developmental or proliferative pathway distinct from other fibromatoses.
No consistent genetic mutations or chromosomal abnormalities have been identified in most cases, though ongoing research continues to investigate the molecular basis of this condition.
Management and Treatment Approaches
Management of IDF varies based on clinical presentation, lesion size, and functional impact:
Observation
Conservative management with observation is often recommended given the benign nature of the condition and tendency for spontaneous resolution. This approach avoids the risks of surgical intervention and high recurrence rates associated with excision.
Intralesional Corticosteroid Injections
Intralesional corticosteroid injections represent a minimally invasive treatment option for lesions causing functional impairment or cosmetic concerns.
Surgical Resection
Complete surgical resection is a treatment option, though high recurrence rates following excision should be considered when determining candidacy for surgery.
Complications and Functional Impact
Most IDF lesions remain harmless and do not cause symptoms unless they rub on neighboring digits or footwear. Potential complications and functional impacts include:
- Pain with larger lesions
- Functional impairment of affected digits or joints
- Cosmetic concerns for parents and caregivers
- Rare ulceration of overlying skin
- Periosteal invasion and bone erosion in exceptional cases
Functional deformities are rare, and most children tolerate the condition well with conservative management.
Frequently Asked Questions
Q: What is the difference between infantile digital fibromatosis and infantile myofibromatosis?
A: While IDF was once considered a subtype of infantile myofibromatosis (IMF), they are now recognized as distinct entities. Both present with benign tumors in fingers and toes of infants, but they differ in pathological features, clinical behavior, and immunohistochemical profiles. IDF specifically features characteristic paranuclear inclusion bodies composed of vimentin and actin filaments.
Q: Will my child’s infantile digital fibromatosis lesion go away on its own?
A: Yes, spontaneous resolution without scarring is characteristic of IDF. Most lesions regress over an average of 2-3 years, though the range can extend from 1-10 years. This predictable natural history supports conservative management with observation in most cases.
Q: Is infantile digital fibromatosis inherited or genetic?
A: The majority of IDF cases are sporadic with no clear hereditary predisposition. Genetic factors have not been consistently identified, and most cases appear to arise de novo without family history of similar lesions.
Q: Can infantile digital fibromatosis occur outside of fingers and toes?
A: While IDF classically affects the fingers and toes (excluding thumb and great toe), non-digital involvement has been documented, though this is rare. Lesions may occasionally occur on hands, feet, arms, or other body locations.
Q: What is the recurrence rate after surgical removal of infantile digital fibromatosis?
A: Recurrence after surgical excision is common, which is an important consideration when deciding between surgery and conservative management. This high recurrence rate has led many clinicians to favor observation rather than immediate surgical intervention.
Q: How is infantile digital fibromatosis diagnosed definitively?
A: Definitive diagnosis requires histopathological analysis through skin biopsy. The characteristic finding is spindle-shaped cells with paranuclear inclusion bodies composed of vimentin and actin filaments, along with positive immunostaining for α-smooth muscle actin, desmin, and calponin.
Conclusion
Infantile digital fibromatosis is a rare benign tumor with distinctive pathological features characterized by spindle-shaped myofibroblasts containing paranuclear inclusion bodies. Understanding the pathology, clinical presentation, and natural history of IDF enables accurate diagnosis and appropriate management. While the condition typically presents as a solitary painless nodule on fingers or toes of infants, awareness of atypical presentations and rare complications is important for comprehensive patient care. Most cases resolve spontaneously without intervention, supporting a conservative approach to management in the majority of affected children.
References
- Infantile Digital Fibromatosis — Wikipedia. 2024. https://en.wikipedia.org/wiki/Infantile_digital_fibromatosis
- Infantile Digital Fibromatosis/Inclusion Body Fibromatosis — National Institutes of Health, National Center for Biotechnology Information (PMC). 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC9827721/
- Infantile Digital Fibromatosis: A Rare Case Report — National Institutes of Health, National Center for Biotechnology Information (PMC). 2015. https://pmc.ncbi.nlm.nih.gov/articles/PMC4817457/
- Infantile Digital Fibroma (Fibromatosis) — DermNet. 2004. https://dermnetnz.org/topics/infantile-digital-fibroma
Read full bio of Sneha Tete













