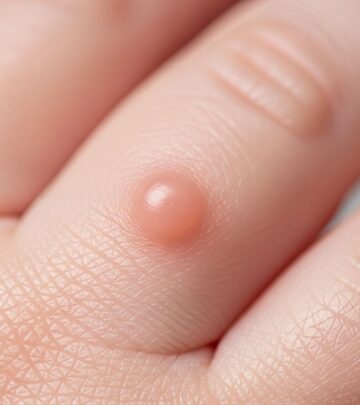
Infantile Papular Acrodermatitis Images: 5 Clinical Photos
Comprehensive visual guide to Gianotti-Crosti syndrome with clinical images, symptoms, causes, and management in children.
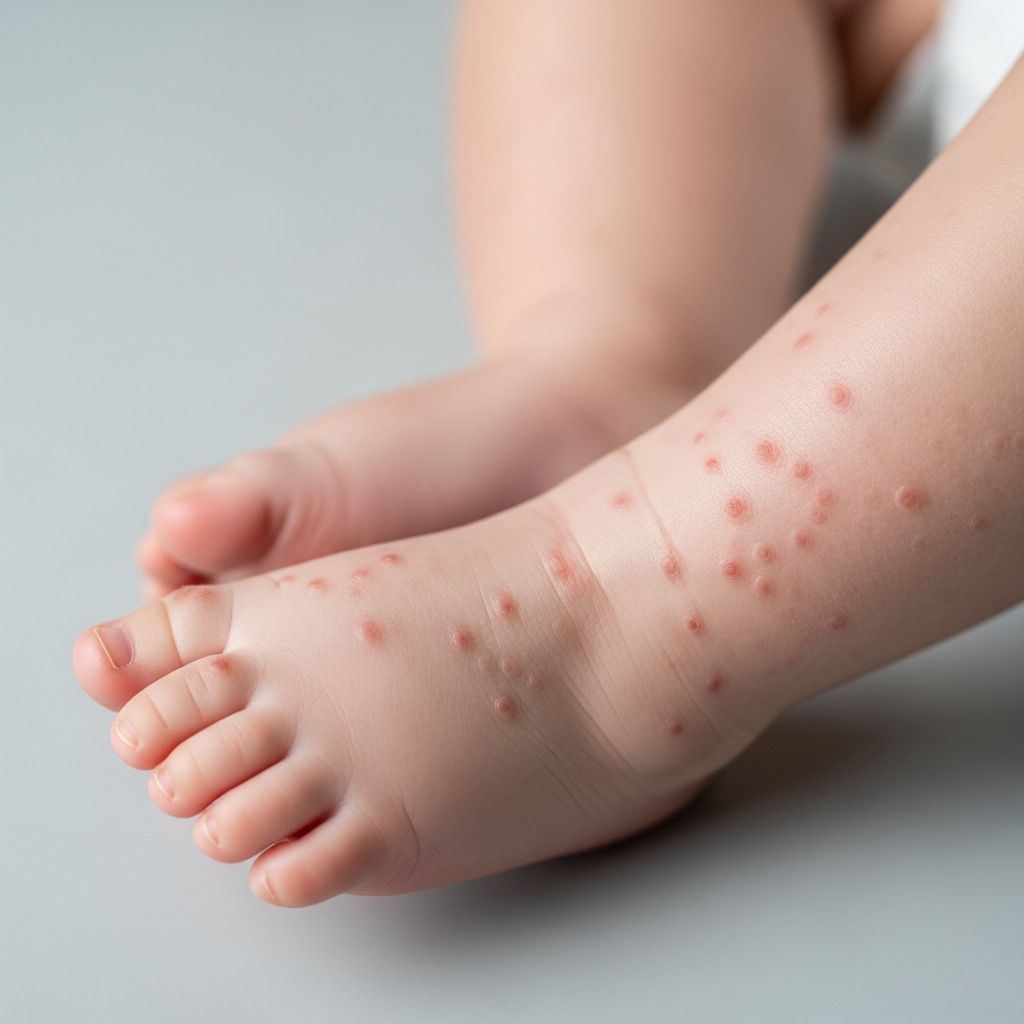
Infantile Papular Acrodermatitis Images
Also known as Gianotti-Crosti syndrome or papular acrodermatitis of childhood, this benign self-limiting rash primarily affects young children following viral infections or vaccinations.
What is Infantile Papular Acrodermatitis?
Infantile papular acrodermatitis, commonly referred to as
Gianotti-Crosti syndrome (GCS)
, is a distinctive dermatological condition characterized by a symmetric eruption of monomorphic papules predominantly distributed on the acral surfaces of the extremities. First described in the 1950s, it was initially associated with hepatitis B virus (HBV) in endemic regions, but contemporary understanding reveals it as an immunologically mediated response to a broad spectrum of viral triggers and occasionally vaccinations. This condition typically manifests in children between 3 months and 15 years of age, with peak incidence around 1-3 years, and is remarkably self-resolving within 2-3 months without long-term sequelae.The hallmark of GCS is its acute onset of flat-topped, firm papules measuring 1-10 mm, which are flesh-colored to erythematous and often pruritic. These lesions spare the trunk and flexures, concentrating on extensor surfaces of limbs, buttocks, and face. Accompanying features may include mild lymphadenopathy, particularly cervical and inguinal, low-grade fever, and malaise, underscoring its post-infectious etiology.
Who Gets Infantile Papular Acrodermatitis (Epidemiology)?
GCS predominantly affects infants and young children, with 90% of cases occurring under 6 years and equal distribution between genders. There is no strong racial predilection, though it appears more frequently in atopic individuals or those with family history of atopy, suggesting an immune predisposition. In non-endemic HBV areas like the United States, viral exanthems rather than HBV predominate, with Epstein-Barr virus (EBV) being the most implicated.
- Age group: Primarily 6 months to 4 years; rare in neonates or adults.
- Incidence: Exact rates unknown, but commonly encountered in pediatric dermatology practices.
- Risk factors: Recent viral illness, vaccination, atopic background, elevated IgE levels.
Causes of Infantile Papular Acrodermatitis
The etiology of GCS is multifactorial, primarily triggered by viral infections that provoke a delayed hypersensitivity reaction. Historically linked to HBV in Mediterranean and Asian cohorts, HBV association has diminished post-vaccination era. Current triggers encompass a wide array of pathogens:
| Viral Triggers | Common Examples | Notes |
|---|---|---|
| Herpesviruses | EBV, CMV, HHV-6, HSV | EBV most common in US |
| Enteroviruses | Coxsackievirus, Echovirus | Often precedes hand-foot-mouth disease |
| Respiratory Viruses | RSV, Parainfluenza, Influenza, Adenovirus | Post-upper respiratory infection |
| Others | Parvovirus B19, Rotavirus, HIV | Rare but reported |
| Vaccinations | Hep B, Polio, Influenza, MMR | Live or inactivated vaccines |
Pathophysiology involves immune complex deposition or T-cell mediated responses, evidenced by perivascular lymphocytic infiltrates and endothelial swelling on histopathology, though biopsy is rarely needed.
Clinical Features and Images
The eruption evolves over 3-4 days: initial red macules progress to papules, occasionally vesicular or purpuric, migrating centripetally from limbs to face and buttocks. Lesions are discrete, firm, and symmetric, with koebnerization at trauma sites possible. Pruritus varies from mild to moderate.
- Sites: Extensor forearms/legs, cheeks, buttocks; spares trunk, flexures.
- Morphology: 1-5 mm pink-red papules; larger in infants.
- Associated: Lymphadenopathy (60-80%), hepatosplenomegaly (rare), jaundice (if HBV).
Image Descriptions (Clinical Correlations):
- Image 1: Symmetrical pink papules on extensor forearms of a 2-year-old post-EBV, sparing flexures.
- Image 2: Facial involvement with discrete flesh-colored papules on cheeks; trunk spared.
- Image 3: Buttocks and thighs showing confluent papules over pressure points.
- Image 4: Resolution phase: Fading lesions after 4 weeks with post-inflammatory hyperpigmentation.
- Image 5: Rare vesicular variant on palms post-vaccination.
These visual hallmarks aid rapid recognition, distinguishing GCS from more concerning eruptions.
Diagnosis of Infantile Papular Acrodermatitis
Diagnosis is clinical, relying on characteristic morphology, distribution, and recent prodrome. Key differentials include:
| Differential | Distinguishing Features |
|---|---|
| Arthropod bites | Asymmetric, urticarial, trunk involvement. |
| Henoch-Schonlein purpura | Palpable purpura, abdominal pain, arthritis. |
| Pityriasis lichenoides | Polymorphic lesions, prolonged course. |
| EBV rash/amoxicillin | Diffuse morbilliform, not acral. |
| Hand-foot-mouth | Oral ulcers, vesicles on palms/soles. |
Laboratory tests are selective: HBV serology in endemic areas, viral PCR if atypical. Histology shows spongiotic dermatitis with lymphocytic infiltrate, non-diagnostic alone.
Treatment and Management
GCS is self-limited, resolving in 2-8 weeks without scarring. Management is supportive:
- Symptomatic relief: Topical corticosteroids (hydrocortisone 1%), emollients for pruritus.
- Severe cases: Oral antihistamines, short-course oral steroids.
- Avoid: Unnecessary antivirals or antibiotics unless underlying infection confirmed.
- Follow-up: Monitor for resolution; investigate if persistent >3 months.
Parental reassurance is paramount, emphasizing benign prognosis.
Prognosis and Complications
Excellent; full resolution without sequelae in nearly all cases. Rare recurrences or post-inflammatory pigment changes. No increased risk of chronic skin disease.
Frequently Asked Questions (FAQs)
Q: Is Gianotti-Crosti syndrome contagious?
A: No, the rash itself is not contagious; it results from the child’s immune response to a prior infection.
Q: How long does the rash last?
A: Typically 2-3 months, though individual papules resolve faster; full clearance by 8 weeks.
Q: Should I take my child to a doctor?
A: Yes, for confirmation and to exclude mimics, especially if fever, jaundice, or lymphadenopathy present.
Q: Can it recur?
A: Rare, but possible with subsequent viral exposures.
Q: Is biopsy necessary?
A: Rarely; clinical diagnosis suffices in typical cases.
Prevention
No specific prevention beyond routine vaccinations reducing HBV risk. Prompt viral illness management may mitigate triggers.
References
- Papular Acrodermatitis – Gianotti-Crosti Syndrome — StatPearls, NCBI Bookshelf. 2023-10-01. https://www.ncbi.nlm.nih.gov/books/NBK441825/
- What Is Acrodermatitis? Causes, Symptoms, and More — Healthline. 2023-05-15. https://www.healthline.com/health/acrodermatitis
- Gianotti Crosti: Causes and Treatment — Dermatology Consultants. 2018-06-27. https://dermatologyconsultants.com/2018/06/27/gianotti-crosti-causes-and-treatment/
- What Is Gianotti-Crosti Syndrome — WebMD. 2024-02-10. https://www.webmd.com/skin-problems-and-treatments/what-is-gianotti-crosti-syndrome
- Acrodermatitis — Miriam Lieberman MD FAAD. 2022-11-01. https://www.miriamliebermanmd.com/acrodermatitis.php
Read full bio of medha deb