Internal Hemorrhoids Explained: Symptoms, Causes & Treatments
Learn about internal hemorrhoids: symptoms, causes, diagnosis, treatments, and prevention strategies for effective relief.
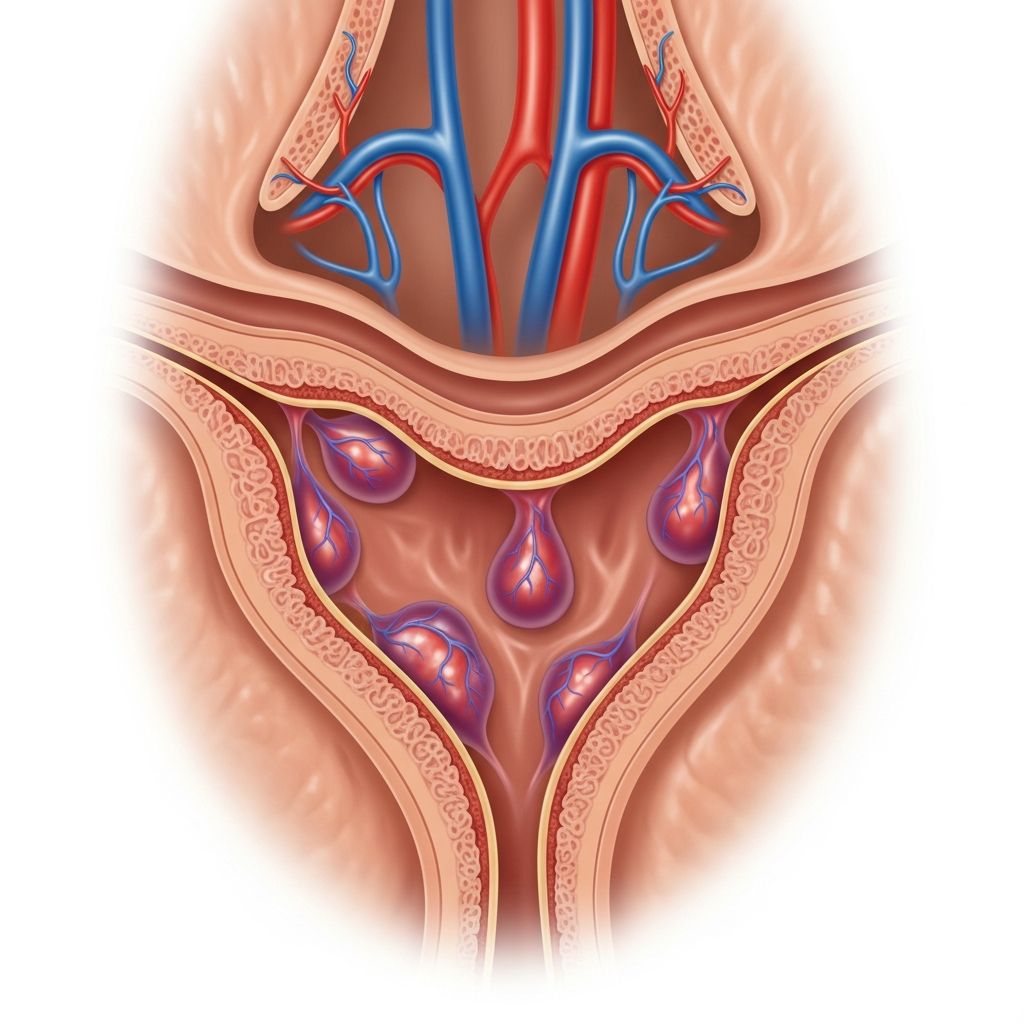
Internal hemorrhoids are swollen veins located inside the rectum, above the dentate line, and often cause painless rectal bleeding during bowel movements. These normal anatomical structures can become symptomatic due to various factors, leading to common issues like bright red blood on toilet paper or in the stool.
What Are Internal Hemorrhoids?
Hemorrhoids consist of clusters of vascular tissue, smooth muscle, and connective tissue arranged in three columns along the anal canal. They serve as cushions that help maintain continence in healthy individuals. Internal hemorrhoids, specifically located above the dentate line, are covered by columnar epithelium innervated by visceral nerve fibers, which means they typically do not cause pain unless prolapsed.
When asymptomatic, hemorrhoids are normal structures, but the term ‘hemorrhoids’ commonly refers to a pathologic process involving enlargement or inflammation. Internal hemorrhoids are graded from I to IV based on prolapse extent: Grade I show no prolapse, Grade II prolapse but reduce spontaneously, Grade III require manual reduction, and Grade IV remain prolapsed.
Symptoms of Internal Hemorrhoids
Symptoms commonly attributed to internal hemorrhoids include rectal bleeding, prolapse, mucus discharge, fecal seepage, pruritus (itching), and occasionally pain if thrombosed or prolapsed. The most frequent symptom is painless bright red bleeding on toilet paper or dripping into the toilet bowl, often noticed during or after defecation.
- Bleeding: Bright red blood coating stool or toilet paper, rarely causing anemia unless chronic and severe.
- Prolapse: Tissue protruding from the anus, which may retract or require manual pushing back.
- Mucus discharge: Leading to anal irritation, soiling, or itching.
- Pain: Unusual for non-prolapsed internal hemorrhoids but occurs with thrombosis or external involvement.
Research indicates these symptoms occur equally in patients with and without hemorrhoids, highlighting the need for proper diagnosis to rule out other conditions like colorectal cancer.
Causes and Risk Factors
Internal hemorrhoids develop when normal hemorrhoidal cushions enlarge due to increased pressure or structural weakness. Common causes include chronic constipation, straining during bowel movements, prolonged sitting, and low-fiber diets leading to hard stools.
- Straining: Increases intra-abdominal pressure, engorging veins.
- Pregnancy: Hormonal changes and uterine pressure contribute.
- Obesity and sedentary lifestyle: Promote venous congestion.
- Collagen abnormalities: Elevated matrix metalloproteinases and reduced collagen stability may play a role, as seen in conditions like Ehlers-Danlos syndrome.
Other factors include aging, which weakens supporting tissues, and heavy lifting. Increased resting anal pressure is common but likely secondary, not causal.
How Are Internal Hemorrhoids Diagnosed?
Diagnosis begins with a thorough medical history focusing on bleeding patterns, diet, bowel habits, and family history of colorectal issues. Physical exam includes visual inspection and digital rectal exam (DRE) to assess for masses, fissures, or prolapse.
For internal hemorrhoids, an anoscope provides direct visualization above the dentate line. If bleeding is significant or risk factors for cancer exist (age >45, weight loss, change in bowel habits), colonoscopy or sigmoidoscopy is recommended to exclude malignancy. Visits for hemorrhoids exceed those for colon cancer or IBS, underscoring diagnostic vigilance.
| Diagnostic Tool | Purpose | When Used |
|---|---|---|
| Digital Rectal Exam | Palpate for tenderness, masses | Initial assessment |
| Anoscopy | Visualize internal hemorrhoids | Suspected internal disease |
| Colonoscopy | Rule out proximal pathology | Age >45 or alarm symptoms |
Treatment Options for Internal Hemorrhoids
Treatment escalates from conservative measures to office-based procedures and surgery based on grade and symptoms. Goals are symptom relief, prolapse reduction, and recurrence prevention.
Conservative (Home) Treatments
First-line for Grade I-II: High-fiber diet (25-30g/day), stool softeners, and hydration soften stools, reducing straining. Topical creams with hydrocortisone or witch hazel provide symptomatic relief but lack strong evidence for curing hemorrhoids.
- Increase fiber intake gradually to avoid bloating.
- Sitz baths (warm water soaks) 2-3 times daily for 10-15 minutes soothe irritation.
- Avoid prolonged toilet sitting; use footstool to optimize defecation posture.
Fiber supplementation shows inconsistent results in trials, with mild gastrointestinal side effects; methodological issues limit confidence.
Office-Based Procedures
For persistent Grade I-III symptoms, minimally invasive options offer high success with low cost.
- Rubber Band Ligation (RBL): Most effective office therapy; band placed at hemorrhoid base causes necrosis and sloughing in 5-7 days. Success 70-90% for Grade II, lower recurrence than alternatives. Mild pain or bleeding common.
- Infrared Coagulation (IRC): Probe delivers infrared heat for coagulation and fibrosis. Quick, painless for Grade I-II; multiple sessions may be needed.
- Sclerotherapy: Inject sclerosant (e.g., phenol) at base induces inflammation and shrinkage. Effective for Grade I-II but risks include ulceration or rare serious complications like abscess.
RBL is guideline-recommended as superior for efficacy.
Surgical Treatments
Reserved for Grade III-IV, failures of office therapy, or complications like thrombosis. Options include hemorrhoidectomy (excision) and stapled hemorrhoidopexy (mucopexy with arterial ligation).
- Conventional Hemorrhoidectomy: Gold standard for low recurrence but painful recovery with complications like bleeding (2-6%).
- Stapled Procedure: Less pain, faster return to work, but higher recurrence.
- Other: LigaSure™, Harmonic® scalpel reduce complications; transanal hemorrhoidal dearterialization (THD) minimizes pain.
A meta-analysis of 98 trials showed surgery has lowest recurrence but more pain/complications than THD or vessel-sealing devices.
| Treatment | Efficacy | Pain/Complications | Recurrence |
|---|---|---|---|
| Rubber Band Ligation | High (Grade I-III) | Low | Low |
| IRC/Sclerotherapy | Moderate | Very Low | Moderate |
| Hemorrhoidectomy | Very High | High | Very Low |
Complications of Untreated Internal Hemorrhoids
Rare but include thrombosis (painful clot), strangulation (irreducible prolapse with ischemia), anemia from chronic bleeding, and secondary infection. Prolapse can lead to ulceration or incontinence if severe.
Prevention Tips
- Maintain high-fiber diet and hydration.
- Exercise regularly to prevent constipation.
- Respond promptly to urge to defecate.
- Avoid straining and heavy lifting when possible.
When to See a Doctor
Seek care for first-time rectal bleeding, prolapse, severe pain, or symptoms lasting >1 week. Alarm signs: black/tarry stools, weight loss, abdominal pain—prompt colonoscopy essential.
Frequently Asked Questions (FAQs)
What causes rectal bleeding in internal hemorrhoids?
Bleeding occurs when fragile rectal veins rupture during straining, producing bright red blood.
Do internal hemorrhoids go away on their own?
Mild cases may resolve with conservative care, but persistent symptoms require intervention to prevent progression.
Is rubber band ligation painful?
Mild discomfort or cramping post-procedure is common, resolving in days; superior to surgery for pain.
Can diet alone cure hemorrhoids?
Dietary fiber reduces symptoms but evidence is inconsistent for complete cure; combine with other measures.
How long does recovery take after hemorrhoid surgery?
1-2 weeks for office procedures; 2-4 weeks for hemorrhoidectomy with pain management.
References
- Rethinking What We Know About Hemorrhoids — Orso Schouten, MD, et al. National Library of Medicine, National Center for Biotechnology Information. 2020-03-25. https://pmc.ncbi.nlm.nih.gov/articles/PMC7075634/
- Hemorrhoids: Diagnosis and Treatment Options — American Society of Colon and Rectal Surgeons. 2023-05-15. https://fascrs.org/patients/diseases-and-conditions/a-z/hemorrhoids-expanded-version
- Clinical Practice Guidelines for Hemorrhoids — American College of Gastroenterology. 2022-11-01. https://journals.lww.com/ajg/fulltext/2022/11000/acg_clinical_guideline__management_of_hemorrhoids.13.aspx
- Haemorrhoids: Modern Perspectives — National Institute for Health and Care Excellence (NICE). 2024-02-20. https://www.nice.org.uk/guidance/ng148
Read full bio of medha deb











