Kidney Failure: Symptoms, Causes, Stages, and Treatment
Comprehensive guide to kidney failure: Understand symptoms, causes, stages, diagnosis, and life-saving treatments for better health outcomes.
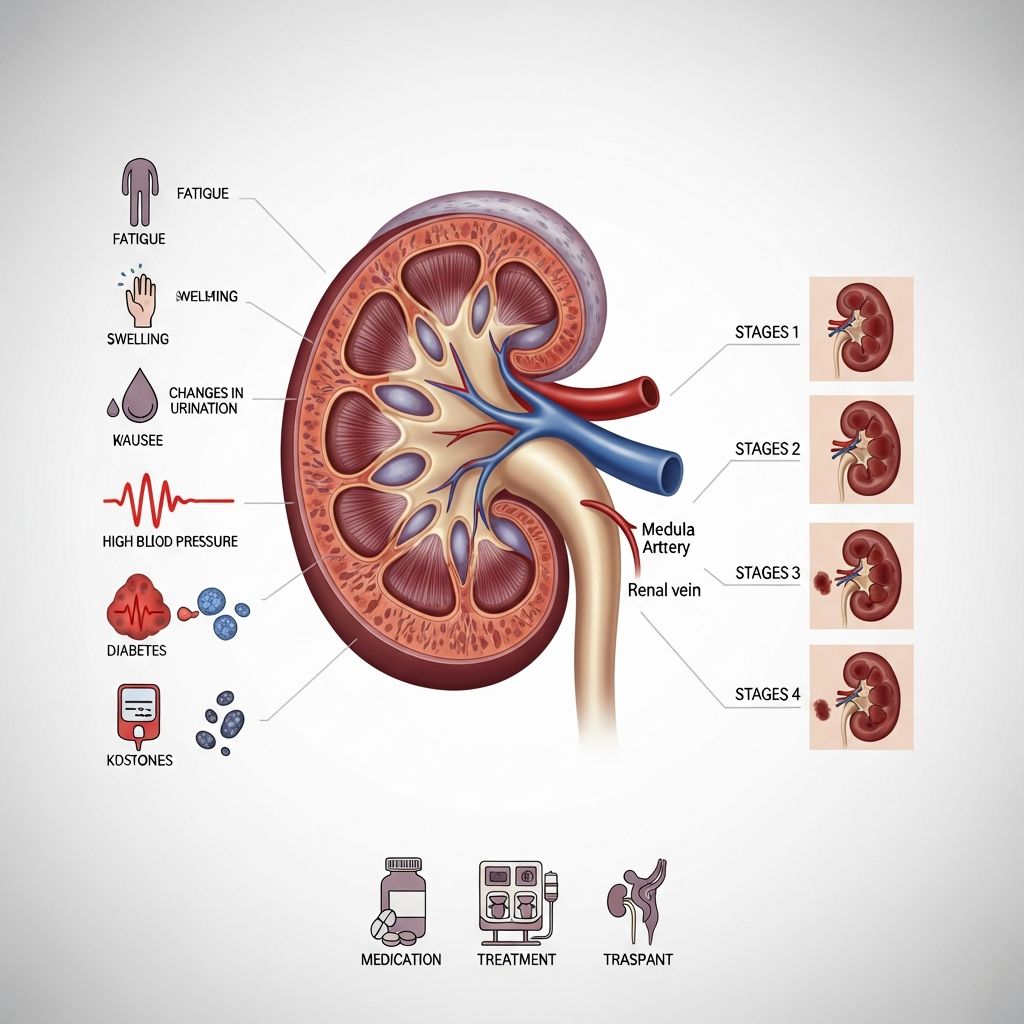
The kidneys are vital organs responsible for filtering waste from the blood, regulating fluid balance, and maintaining electrolyte levels. When they fail, toxins build up, leading to serious health complications. Kidney failure, also known as renal failure, occurs when the kidneys lose their ability to filter effectively. There are two main types: acute kidney injury (AKI), which is sudden and often reversible, and chronic kidney disease (CKD), which progresses slowly over time and can lead to end-stage renal disease (ESRD).
Understanding kidney failure is crucial, as early detection can slow progression. According to the National Kidney Foundation, over 37 million adults in the U.S. have CKD, with millions undiagnosed. This article covers symptoms, causes, stages, diagnosis, treatment, prevention, and more.
What Is Kidney Failure?
Kidney failure happens when the glomeruli—tiny filters in the kidneys—can no longer adequately remove waste and excess fluids from the bloodstream. Healthy kidneys filter about 200 liters of fluid daily, producing 1-2 liters of urine. In failure, this process falters, causing dangerous buildup of urea, creatinine, and other toxins.
Acute kidney injury (AKI) develops rapidly, often within hours or days, due to sudden insults like dehydration or infection. It affects up to 7% of hospitalized patients and can resolve with prompt care. Chronic kidney disease (CKD), however, worsens gradually over months or years, primarily from diabetes or hypertension damaging nephrons irreversibly.
ESRD represents stage 5 CKD, where kidneys function at less than 15% capacity, necessitating dialysis or transplant for survival. Globally, CKD causes 1.2 million deaths annually, per WHO data.
Symptoms of Kidney Failure
Early kidney failure often presents no symptoms, making routine screening essential for at-risk individuals. As damage advances, signs emerge:
- Fatigue and weakness: Toxin accumulation impairs red blood cell production, causing anemia.
- Swelling (edema): Fluid retention leads to puffiness in legs, ankles, face, or hands.
- Changes in urination: Foamy urine (proteinuria), blood in urine (hematuria), reduced output (oliguria), or frequent nighttime urination (nocturia).
- Nausea, vomiting, loss of appetite: Uremia disrupts digestion.
- Itchy skin and rashes: Phosphorus buildup irritates the skin.
- Shortness of breath: Fluid in lungs (pulmonary edema).
- High blood pressure: Kidneys’ role in blood pressure regulation fails.
- Confusion or trouble concentrating: Toxins affect brain function.
In AKI, symptoms like decreased urine output and sudden fatigue appear abruptly. CKD symptoms intensify gradually. Seek immediate care for severe signs like seizures or chest pain.
Causes and Risk Factors
Kidney failure stems from diverse causes, broadly prerenal (reduced blood flow), intrinsic (kidney damage), or postrenal (blockage).
Acute Kidney Injury Causes
- Prenatal: Dehydration, blood loss, heart failure.
- Intrinsic: Infections (sepsis), toxins (contrast dye), glomerulonephritis.
- Postrenal: Enlarged prostate, kidney stones, tumors.
Chronic Kidney Disease Causes
Diabetes (diabetic nephropathy) accounts for 44% of ESRD cases, hypertension 28%, per CDC data. Other contributors include:
- Autoimmune diseases (lupus, vasculitis).
- Polycystic kidney disease (genetic cysts).
- Prolonged NSAID use or antibiotics.
- Repeated urinary tract infections.
Risk factors: Age over 60, family history, obesity, smoking, cardiovascular disease. Black, Hispanic, and Native American populations face higher risks due to genetic and socioeconomic factors.
Stages of Kidney Failure
CKD stages are based on glomerular filtration rate (GFR), measured in mL/min/1.73m²:
| Stage | GFR | Description |
|---|---|---|
| 1 | >90 | Kidney damage with normal function; monitor closely. |
| 2 | 60-89 | Mild loss; manage underlying conditions. |
| 3a/3b | 45-59 / 30-44 | Mild-moderate/severe loss; symptoms may start. |
| 4 | 15-29 | Severe loss; prepare for dialysis/transplant. |
| 5 (ESRD) | <15 | Kidney failure; renal replacement therapy required. |
AKI lacks formal stages but is graded by severity: Risk, Injury, Failure, Loss, End-stage (RIFLE criteria).
Diagnosis of Kidney Failure
Diagnosis combines medical history, physical exams, and tests:
- Blood tests: Serum creatinine, BUN, eGFR. Normal creatinine: 0.6-1.2 mg/dL (men), 0.5-1.1 (women).
- Urine tests: Albumin-to-creatinine ratio (ACR); >30 mg/g indicates damage.
- Imaging: Ultrasound for size/structure, CT/MRI for blockages.
- Biopsy: Samples tissue to identify cause.
Annual screening recommended for high-risk groups per KDIGO guidelines.
Treatment Options for Kidney Failure
Treatment targets underlying cause and symptom management. ESRD requires renal replacement therapy.
Conservative Management
Diet low in sodium, potassium, phosphorus; blood pressure meds (ACE inhibitors); treat anemia with erythropoietin.
Dialysis
- Hemodialysis: Blood filtered via machine 3-4x/week, 3-5 hours/session. Vascular access via fistula.
- Peritoneal dialysis: Dialysate fluid in abdomen exchanges waste; home-based, daily.
Hemodialysis complications: Hypotension, infections; PD: Peritonitis.
Kidney Transplant
Preferred for eligible patients. Living donors yield better outcomes (95% 1-year survival vs. 92% deceased). Immunosuppressants prevent rejection. Waitlists exceed 100,000 in U.S.
Complications of Kidney Failure
- Cardiovascular disease: #1 cause of death in ESRD (50%).
- Anemia and bone disease: From erythropoietin and vitamin D deficiency.
- Infections: Weakened immunity.
- Fluid/electrolyte imbalances: Hyperkalemia risks heart arrhythmia.
Prevention and Living with Kidney Failure
Prevent CKD by controlling diabetes (A1C <7%), hypertension (<130/80 mmHg), healthy weight, no smoking. Stay hydrated, limit NSAIDs.
For diagnosed patients: Follow diet (DAIRY restrictions), exercise, adhere to meds. Quality of life improves with transplant; dialysis patients average 5-10 years survival.
Frequently Asked Questions (FAQs)
What is the life expectancy with kidney failure?
Untreated ESRD: Months. With dialysis: 5-10 years average. Transplant: 15-20+ years. Factors include age, comorbidities.
Can kidney failure be reversed?
AKI often yes, with cause removal. CKD irreversible but progression slowable.
Is kidney failure painful?
Not usually directly; complications like bone disease or gout cause pain.
What foods should be avoided?
High-potassium (bananas, potatoes), phosphorus (dairy, cola), sodium-rich processed foods.
Who is eligible for kidney transplant?
Most under 70 without severe comorbidities; evaluated case-by-case.
References
- Chronic Kidney Disease in the United States, 2023 — Centers for Disease Control and Prevention. 2023-03-01. https://www.cdc.gov/kidneydisease/publications-resources/ckd-national-facts.html
- KDIGO 2024 Clinical Practice Guideline for Chronic Kidney Disease — Kidney Disease: Improving Global Outcomes. 2024-04-01. https://kdigo.org/guidelines/ckd-evaluation-and-management/
- Acute Kidney Injury — National Kidney Foundation. 2023-11-15. https://www.kidney.org/atoz/content/AcuteKidneyInjury
- End-Stage Renal Disease — National Institute of Diabetes and Digestive and Kidney Diseases. 2024-02-20. https://www.niddk.nih.gov/health-information/kidney-disease/end-stage-renal-disease
- Global Burden of Chronic Kidney Disease — World Health Organization. 2023-06-10. https://www.who.int/news-room/fact-sheets/detail/chronic-kidney-disease
- USRDS 2024 Annual Data Report — United States Renal Data System. 2024-07-15. https://usrds.org/annual-data-report/
Read full bio of medha deb











