Knee Pain and Problems: Causes, Symptoms & Treatment
Comprehensive guide to understanding knee pain causes, symptoms, diagnosis and effective treatment options.
Knee Pain and Problems: A Comprehensive Guide
Knee pain is one of the most common musculoskeletal complaints affecting millions of people worldwide. The knee is a complex joint bearing significant weight during daily activities, making it vulnerable to injuries, degenerative conditions, and chronic pain disorders. Understanding the underlying causes of knee pain is essential for effective management and recovery. This guide provides detailed information about knee pain and problems, their causes, symptoms, diagnosis, and treatment options to help you make informed decisions about your health.
Understanding Knee Anatomy and Function
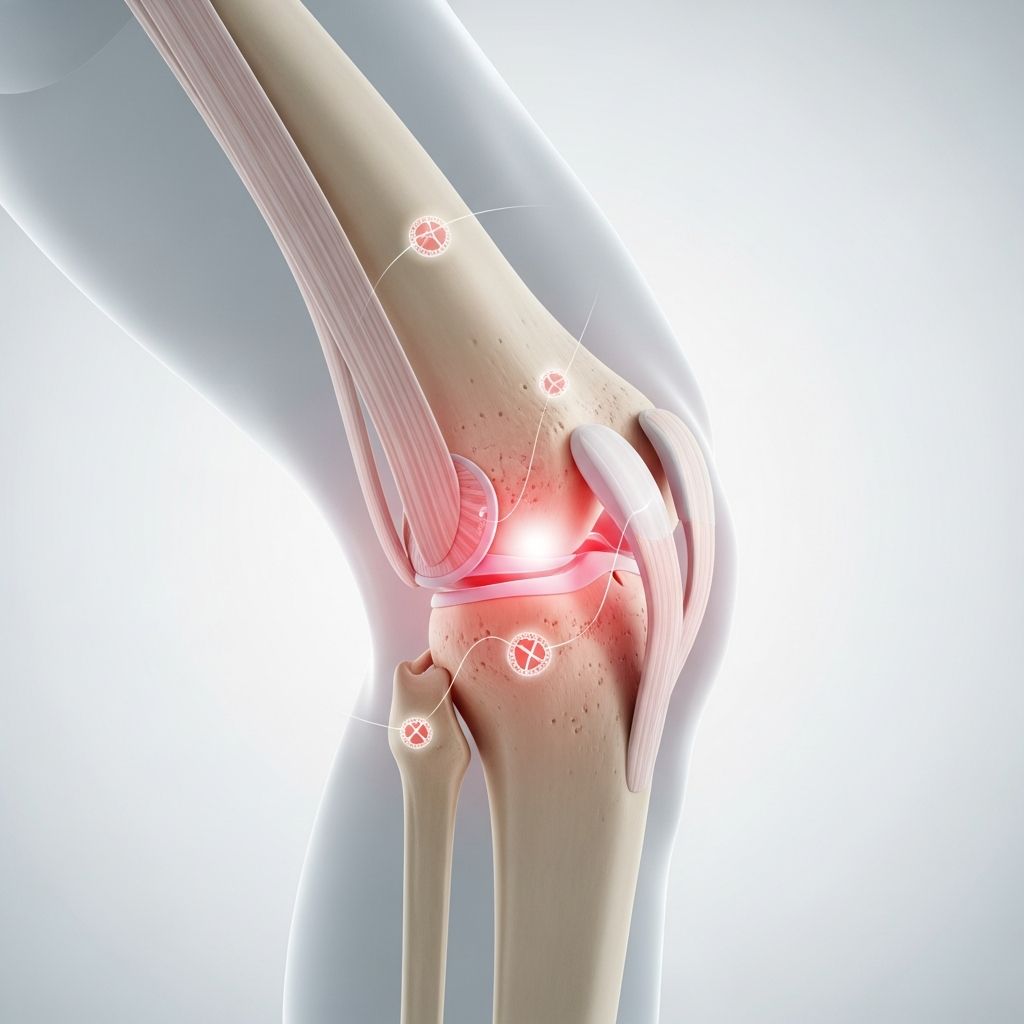
The knee is the largest joint in the human body, connecting the femur (thighbone), tibia (shinbone), and patella (kneecap). This complex structure includes cartilage, ligaments, tendons, and synovial fluid that work together to provide mobility and support. The knee joint allows for bending, straightening, and rotating motions essential for walking, running, and climbing stairs. Several key structures work in concert: the anterior and posterior cruciate ligaments provide stability, the menisci act as shock absorbers, and the articular cartilage cushions the bones. When any of these components become damaged or inflamed, knee pain and dysfunction can result.
Common Causes of Knee Pain
Osteoarthritis
Osteoarthritis (OA) is the most common form of knee arthritis and develops when the cartilage protecting the bones gradually wears away over time. Research from Johns Hopkins indicates that knee pain from osteoarthritis tends to be poorly correlated to the degree of cartilage loss, suggesting that other factors related to knee OA, including bone marrow edema and synovitis, may be more significant determinants of pain in knee osteoarthritis. Synovitis, or inflammation of the joint lining, is usually quite limited in knee OA and difficult to quantify on physical examination, though magnetic resonance imaging provides more sensitive assessment. This progressive condition typically affects older adults and those with risk factors such as obesity, previous knee injury, or muscle weakness.
Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune disease causing inflammation in the knee joint lining. Unlike osteoarthritis, which develops from wear and tear, rheumatoid arthritis occurs when the immune system attacks the synovial membrane. This leads to pain, swelling, and eventual cartilage and bone damage if left untreated.
Acute Injuries
Traumatic injuries can cause immediate knee pain and long-term complications. Common acute injuries include anterior cruciate ligament (ACL) tears, posterior cruciate ligament (PCL) tears, meniscal tears, and patellar dislocation. These injuries often result from sudden movements, falls, or sports-related activities. The severity ranges from mild sprains to complete ligament ruptures requiring surgical intervention.
Chronic Pain Mechanisms
Chronic knee pain can develop through complex pain mechanisms involving neuroplasticity and central sensitization. According to clinical research, sensitization represents neuroplasticity where heightened pain intensity, spreading of pain, and impaired ability to inhibit pain become clinical features of chronic pain conditions. Central sensitization can occur with repetitive input to the nervous system or from a single intense noxious event, characterized by increased excitability of pain pathways. Understanding these mechanisms is crucial for developing targeted interventions that address the specific pain mechanisms rather than simply treating symptoms.
Overuse and Repetitive Strain
Activities involving repetitive knee motion can cause inflammation and pain. Conditions like runner’s knee, patellar tendinitis, and IT band syndrome develop from overuse without adequate recovery. These conditions commonly affect athletes and individuals who engage in high-impact activities without proper conditioning.
Symptoms of Knee Problems
Knee problems present with various symptoms that may develop suddenly or gradually. Common symptoms include:
Pain and Discomfort: Patients may experience localized pain on specific areas of the knee or diffuse pain across multiple regions. The intensity varies from mild discomfort to severe debilitating pain that limits activities. Pain patterns can indicate the location and nature of the underlying problem.
Stiffness: Morning stiffness or stiffness when first rising is particularly common in arthritic knees. This typically improves as the joint begins moving through its range of motion during the day.
Swelling: Knee swelling indicates inflammation within the joint and may develop acutely after injury or gradually with chronic conditions. Swelling reduces mobility and may feel uncomfortable or tight.
Crepitus: A crunching or clicking sound when bending and straightening the knee is called crepitus and often indicates cartilage damage or joint surface irregularities.
Catching and Locking: Patients may experience the knee suddenly catching or locking during movement, limiting their ability to fully extend or bend the joint.
Instability: A sensation that the knee is giving way or feeling unstable during walking or standing activities suggests ligament damage or neuromuscular weakness.
Deformity: Over time, progressive knee arthritis can cause visible changes in knee alignment, resulting in more bow-legged or knock-kneed appearance.
Diagnosis of Knee Problems
Physical Examination
The diagnostic process begins with a thorough physical examination. Your healthcare provider will assess the knee for swelling, tenderness, range of motion, and stability. Special tests help identify specific injuries such as ACL tears or meniscal damage. Pain location during examination provides valuable diagnostic information—very localized pain on the inside of the knee suggests arthritis in one compartment, while diffuse pain around the knee indicates multi-compartment involvement.
Imaging Studies
Imaging techniques provide detailed visualization of knee structures. X-rays show bone alignment and cartilage loss associated with arthritis. Magnetic resonance imaging (MRI) offers superior soft tissue detail, clearly showing ligament tears, meniscal damage, and cartilage conditions. MRI is particularly useful for assessing synovitis in knee osteoarthritis with greater sensitivity than physical examination. Ultrasound provides real-time visualization of dynamic structures and can guide injections.
Laboratory Tests
Blood tests may be ordered when autoimmune conditions like rheumatoid arthritis are suspected. Tests measuring inflammatory markers and specific antibodies help confirm diagnosis and guide treatment selection.
Treatment Options
Conservative Treatment Approach
Activity Modification: Patients with knee arthritis benefit significantly from avoiding twisting and high-impact activities such as running, jumping, and basketball. These activities cause irritation and exacerbate swelling and pain. The goal is transitioning to lower-impact activities easier on the knee rather than complete inactivity. Walking, swimming, and cycling offer excellent alternatives for maintaining fitness while protecting the joint.
Weight Management: Excess body weight increases stress on weight-bearing joints like the knee. Weight loss programs combining dietary modification and exercise improve symptoms and slow disease progression. Both upper extremity and lower extremity exercises prove helpful in these situations, and bariatric surgery may be considered as a surgical weight loss option when other approaches prove insufficient.
Walking Aids: Using a cane or walker helps offload the knee joint by transmitting weight to the assistive device, significantly reducing symptoms.
Physical Therapy and Rehabilitation
Physical therapy plays a central role in knee pain management. Modern approaches emphasize pain mechanism-based interventions targeting specific factors contributing to pain rather than treating symptoms alone. Therapy programs include strength training to improve supporting muscles, flexibility exercises to maintain range of motion, and proprioceptive training to enhance stability. Addressing factors like sleep disorders that impair pain inhibition becomes part of comprehensive management. Physical therapists design individualized programs based on patient presentation and underlying pathology.
Medications
Pharmacological management varies based on condition type and severity. Acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs) provide pain relief and reduce inflammation for many patients. These medications offer initial symptom control, though long-term use requires medical monitoring. Prescription medications may be necessary for more severe conditions.
Injectable Treatments
Corticosteroid Injections: Cortisone or steroid injections provide excellent pain relief for many patients, particularly with first injection, often delivering relief lasting several months. These injections can be repeated up to every three months or approximately four times yearly, making them valuable for managing acute pain flares while pursuing other treatment options.
Viscosupplementation: Viscosupplementation injections contain hyaluronic acid that supplements synovial fluid, functioning as a biological treatment agent. This approach works particularly well for patients with osteoarthritis.
Surgical Interventions
When conservative measures fail to provide adequate relief, surgical options become appropriate. Knee arthroscopy addresses specific structural problems like meniscal tears or loose bodies. Arthroscopic debridement removes damaged cartilage fragments and cleans the joint. Osteotomy realigns the knee to reduce stress on damaged cartilage. Knee replacement becomes necessary for patients with end-stage arthritis affecting multiple knee compartments or those with severe ligament instability requiring full knee replacement.
Determining Treatment Stages
Treatment progression follows a staged approach. Stage one emphasizes conservative measures including activity modification, weight management, and walking aids. When patients experience inadequate symptom relief after appropriate conservative therapy, progression to stage two incorporating physical therapy and medications is indicated. If these interventions prove insufficient, progression to stage three with injection therapy provides additional relief options. Surgical intervention represents the final stage when all other approaches have been exhausted.
When to Seek Medical Attention
Immediate medical evaluation is warranted for sudden severe knee pain, inability to bear weight on the affected leg, visible deformity, signs of infection including fever and warmth, or knee pain following significant trauma. Persistent knee pain lasting more than two weeks despite conservative self-care measures also warrants professional evaluation. Additionally, if your knee feels unstable or you experience functional limitations affecting daily activities, consulting a healthcare provider is important.
Prevention Strategies
Several strategies help prevent knee problems and reduce injury risk. Maintaining appropriate body weight decreases joint stress. Regular strength and flexibility training keeps supporting muscles strong and maintains range of motion. Warming up before exercise and cooling down afterward prepare tissues for activity and promote recovery. Using proper technique during sports and recreational activities prevents injury. Wearing supportive footwear and using protective equipment when appropriate further reduces injury risk. Gradually increasing activity levels prevents overuse injuries.
Living with Knee Problems
Managing chronic knee problems requires a multifaceted approach combining multiple strategies. Most patients experience significant improvement with appropriate conservative treatment. Maintaining consistency with physical therapy, following activity recommendations, and managing weight prove essential for long-term success. Regular communication with healthcare providers allows treatment adjustments as needed. Many patients successfully return to desired activities with proper management, though some may require permanent activity modification.
Frequently Asked Questions
Q: What is the difference between knee pain and knee arthritis?
A: Knee pain is a symptom that can result from various conditions including injury, inflammation, or overuse. Arthritis specifically refers to joint inflammation, with osteoarthritis being the most common form involving cartilage degeneration. While arthritis causes knee pain, not all knee pain results from arthritis.
Q: How long does it take for conservative treatment to work?
A: Response to conservative treatment varies by individual and condition severity. Many patients notice improvement within 2-4 weeks of consistent therapy and activity modification. However, some conditions require several months of treatment before substantial improvement occurs. Patience and compliance with treatment recommendations are essential.
Q: Can knee pain resolve without treatment?
A: Minor knee injuries may resolve spontaneously with rest and conservative care. However, significant injuries and chronic conditions typically require active treatment. Delaying appropriate treatment may allow conditions to worsen and lead to chronic pain patterns.
Q: Is surgery necessary for all knee problems?
A: No, most knee problems respond well to conservative treatment. Surgery is typically reserved for specific structural problems not responding to conservative care, severe arthritis affecting multiple compartments, or ligament injuries causing instability.
Q: Can physical therapy alone treat knee osteoarthritis?
A: Physical therapy is an important component of osteoarthritis management, but optimal outcomes typically result from combining physical therapy with activity modification, weight management, and appropriate medication. A comprehensive, multifaceted approach produces the best results.
Q: What activities should I avoid with knee pain?
A: Activities involving high impact like running and jumping, twisting motions, and heavy lifting should typically be avoided during acute pain flares. However, complete inactivity is counterproductive—transitioning to lower-impact activities like swimming, cycling, or walking maintains fitness while protecting the joint.
Q: How does weight affect knee pain?
A: Excess weight increases stress on weight-bearing joints like the knee. Each pound of weight adds approximately four pounds of stress to the knee joint. Weight loss significantly reduces pain and can slow progression of degenerative conditions.
References
- Pain Mechanisms Associated with Chronic Knee Osteoarthritis — Johns Hopkins Department of Physical Medicine and Rehabilitation. 2018-05-15. https://www.hopkinsmedicine.org
- Knee Pain from Osteoarthritis Related to Synovitis and Bone Marrow Edema — Johns Hopkins Arthritis Center. 2024. https://www.hopkinsarthritis.org
- Management of Knee Arthritis: Diagnosis and Treatment Options — Johns Hopkins Medicine, Department of Orthopaedic Surgery. 2021-11-15. https://www.hopkinsmedicine.org
- Knee Osteoarthritis: Using Biology to Optimize Exercise Treatment Paradigm — Johns Hopkins Medicine. 2023. https://www.hopkinsmedicine.org
Read full bio of medha deb











