Labial Adhesion in Prepubertal Girls
Understanding labial adhesion: causes, symptoms, diagnosis, and effective treatments in young girls before puberty.
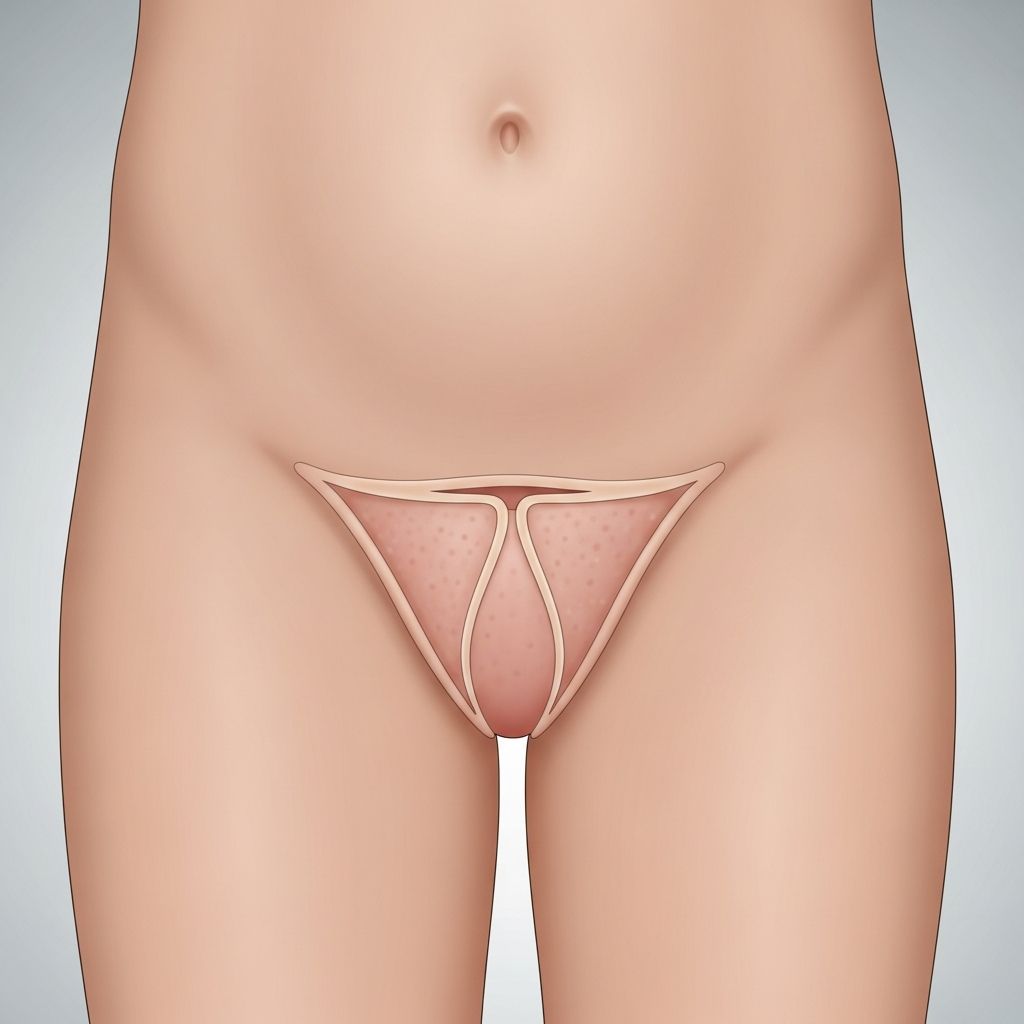
Labial adhesion, also known as labial fusion or synechia of the vulva, is a common benign condition affecting prepubertal girls. It involves the adherence of the labia minora in the midline, often due to low estrogen levels and local irritation. This condition typically occurs between 3 months and 6 years of age and is usually asymptomatic, resolving spontaneously at puberty with rising estrogen levels.
What is labial adhesion?
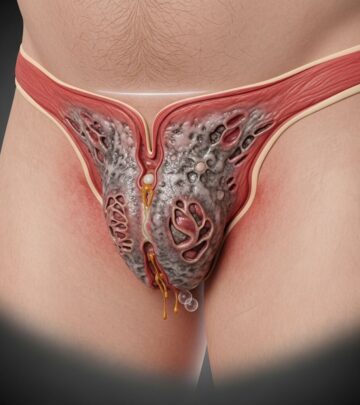
Labial adhesion refers to the fusion of the inner lips of the vulva (labia minora) along the midline, creating a white or gray membrane-like structure. This fusion partially or completely covers the vaginal opening and sometimes the urethral meatus. It is an acquired condition, not present at birth, resulting from the apposition of irritated mucosal surfaces in a low-estrogen environment typical of infancy and childhood.
The thin, fragile labia minora become inflamed from irritants such as urine, feces, soaps, or infections, leading to raw surfaces that stick together during healing. Without sufficient estrogen to promote thicker, more resilient epithelium, the adhesion persists.
Who gets labial adhesion?
Labial adhesion primarily affects prepubertal girls, with peak incidence between 13 months and 48 months of age. Studies estimate prevalence at 1-11% in this population, often discovered incidentally during routine exams or diaper changes.
- Common in girls aged 3 months to 6 years due to low systemic estrogen post-infancy.
- Risk factors include poor hygiene, recurrent vulvovaginitis, diaper dermatitis, and inflammatory skin conditions.
- More noticeable in non-circumcised settings or with bubble baths/perfumed products irritating the area.
Rarely seen in post-pubertal females unless associated with conditions like lichen sclerosus, trauma, or post-surgical states.
What causes labial adhesion?
The primary cause is a combination of hypoestrogenism and vulvar irritation. Prepubertal girls have thin, sensitive vulvar epithelium lacking estrogen’s protective thickening effect.
- Irritants: Urine dribbling, fecal contamination, harsh soaps, bubble baths, or synthetic underwear.
- Infections/Inflammation: Vulvovaginitis, candidiasis, or bacterial overgrowth.
- Mechanical factors: Diaper friction or poor perineal hygiene leading to chronic moisture.
- Once fused, the adhesion prevents normal cleaning, perpetuating irritation and increasing UTI risk.
It is not congenital and does not indicate sexual abuse or endocrine disorders.
What are the symptoms and signs of labial adhesion?
Most cases (up to 80%) are asymptomatic, noticed as a thin midline membrane during exams. Symptomatic cases present with:
- Vulvar soreness or discomfort.
- Post-void dribbling or urinary retention.
- Recurrent urinary tract infections (UTIs) from urethral obstruction.
- Rare severe complications: acute urinary retention or hydronephrosis from complete occlusion.
The appearance is a smooth, white/gray raphe bridging the labia minora, varying from thin (<1mm) to thick/complete occlusion.
How is labial adhesion diagnosed?
Diagnosis is clinical via visual inspection of the external genitalia in a frog-leg position. No imaging or labs are routinely needed unless complications suspected.
- Key finding: Midline fusion of labia minora with normal clitoris and surrounding skin.
- Differentiate from imperforate hymen (covers entire vestibule) or congenital anomalies.
- If symptomatic: Urinalysis for UTI; rarely, renal ultrasound for hydronephrosis.
Biopsy or further tests unnecessary unless atypical features like bleeding or asymmetry.
What is the treatment of labial adhesion?
Conservative management (asymptomatic)
For thin, asymptomatic adhesions, observation is recommended. Spontaneous resolution occurs in 75-90% by puberty due to endogenous estrogen.
- Hygiene: Gentle cleaning with water; avoid irritants.
- Emollients: Daily petroleum jelly (Vaseline) to prevent worsening.
Topical therapies (symptomatic)
Treatment indicated for symptoms, thick adhesions, or parental concern. Success rates 50-90%.
Topical estrogen cream
First-line: Conjugated estrogen (0.01%) or estradiol cream.
- Dose: Pea-sized amount twice daily to midline.
- Duration: 2-4 weeks; taper if separating.
- Side effects: Transient pigmentation, rare breast budding or spotting.
Mechanism: Mimics pubertal estrogen to mature epithelium and separate tissues.
Topical corticosteroid
Alternative, especially for recurrence or estrogen intolerance: Betamethasone 0.05% ointment.
- Dose: Thin layer twice daily for 4-6 weeks.
- Side effects: Mild telangiectasia or atrophy (rare, reversible).
- May have lower recurrence vs. estrogen.
Maintenance and prevention
Post-separation: Apply emollient (Vaseline) daily for 4-8 weeks to prevent re-adhesion.
- Hygiene education: Front-to-back wiping, cotton underwear.
- Avoid irritants: No bubble baths, perfumed wipes.
Manual or surgical separation
Rare (<5%): For complete occlusion failing medical therapy. Performed under anesthesia by specialist; follow with topical estrogen.
Complications of labial adhesion
Usually benign, but untreated severe cases risk:
- UTIs: Stagnant urine promotes infection.
- Urinary obstruction: Retention, dribbling, or hydronephrosis.
- Vulvovaginitis: Trapped debris causes secondary infection.
- Psychological distress for parents mistaking for trauma.
Prevention of labial adhesion
Proactive measures reduce incidence:
- Daily emollient barrier creams during diaper phase.
- Mild soap-free cleansing; pat dry thoroughly.
- Prompt treatment of diaper rash or infections.
- Breathable cotton clothing; frequent changes.
Labial adhesion in adult women
Rare post-puberty; associated with hypoestrogenism (post-menopause), lichen sclerosus, or scarring from trauma/SJS. Management similar but investigate underlying cause.
Follow-up and when to refer
Reassess 4-6 weeks post-treatment. Refer to pediatric gynecology if:
- Failed 2+ medical trials.
- Thick/complete occlusion with symptoms.
- Atypical features or diagnostic uncertainty.
Prognosis excellent; >95% resolve without long-term issues.
Frequently asked questions about labial adhesion
Is labial adhesion painful?
Typically painless unless secondarily infected or obstructing.
Does labial adhesion require surgery?
Rarely; medical therapy suffices in 90%+ cases.
Can labial adhesion cause infertility?
No; resolves before reproductive years.
How long does treatment take?
2-6 weeks for separation; maintenance 1-2 months.
Is it related to sexual abuse?
No; common benign finding unrelated to trauma.
References
- Labial Adhesions in Children: Diagnosis & Treatment Guide — Hippo Education. 2023. https://home.hippoed.com/blog/labial-adhesions-in-children-diagnosis-treatment-guide-hippo-education
- Labial Adhesion: Evaluation and Management — Nationwide Children’s Hospital. 2022-10-01. https://www.nationwidechildrens.org/-/media/nch/for-medical-professionals/practice-tools-new/labial-adhesion.pdf
- Labial Adhesion: Causes, Diagnosis & Treatment — Cleveland Clinic. 2024-05-15. https://my.clevelandclinic.org/health/diseases/16435-labial-adhesions
- Labial adhesions — Better Health Channel (Victorian Government). 2023. https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/labial-adhesions
- Labial Adhesions — Children’s Hospital of Philadelphia (CHOP). 2024. https://www.chop.edu/conditions-diseases/labial-adhesions
Read full bio of Sneha Tete