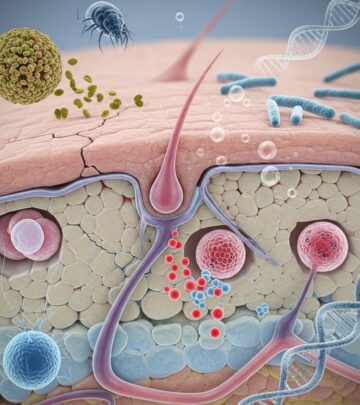
Lebrikizumab: 5 Key Benefits For Atopic Dermatitis Relief
IL-13 inhibitor biologic for moderate-to-severe atopic dermatitis: efficacy, safety, dosing, and patient guidance.
Lebrikizumab
Authoritative facts about lebrikizumab from DermNet New Zealand, updated with recent clinical trial data.
What is lebrikizumab?
Lebrikizumab is a humanized monoclonal antibody that selectively binds to interleukin-13 (IL-13), a key cytokine driving the inflammation in
atopic dermatitis (AD)
, commonly known as eczema. By neutralizing IL-13, lebrikizumab prevents it from binding to its receptors (IL-13Rα1 and IL-4Rα), thereby blocking downstream signaling pathways that promote skin inflammation, barrier dysfunction, and itch. This targeted mechanism restores skin barrier integrity by enhancing production of proteins and lipids essential for hydration and protection against irritants and allergens.Approved as
Ebglyss (lebrikizumab-lbkz)
, it is indicated for adults and adolescents aged 12 years and older weighing at least 88 pounds (40 kg) with moderate-to-severe AD whose disease is not adequately controlled with topical prescription therapies or when those therapies are not advisable. Unlike broad immunosuppressants like ciclosporin or methotrexate, lebrikizumab’s specificity to IL-13 results in a more favorable side effect profile.Who is it for?
Lebrikizumab is prescribed for patients with
moderate-to-severe atopic dermatitis
who have failed or cannot tolerate topical treatments such as corticosteroids or calcineurin inhibitors. Clinical eligibility often includes:- Eczema Area and Severity Index (EASI) score ≥16
- Investigator’s Global Assessment (IGA) score ≥3
- Inadequate response to ≥1 topical medication
- Age ≥12 years and weight ≥40 kg
It is particularly beneficial for those experiencing severe itch (pruritus), sleep disturbance, and quality-of-life impairment due to widespread lesions. Preliminary data suggest potential in combination with topical corticosteroids for enhanced efficacy.
How does lebrikizumab work?
In atopic dermatitis, the immune system overproduces IL-13 in response to triggers like allergens, leading to Th2-driven inflammation, epidermal barrier disruption, and intense itching. Lebrikizumab binds IL-13 with high affinity, inhibiting its interaction with receptors and halting signaling that:
- Induces keratinocyte proliferation and chemokine release
- Impairs filaggrin and lipid synthesis, causing dry, cracked skin
- Amplifies itch via neuronal sensitization
This results in rapid reduction of inflammation (erythema, excoriations), improved skin barrier function, and itch relief as early as 2 days post-injection. Long-term use sustains skin clearance and patient-reported outcomes.
Evidence from clinical trials
Phase 3 trials (ADvocate1, ADvocate2, ADjoin) enrolled over 800 adults and adolescents with moderate-to-severe AD. Key findings at week 16:
| Trial | Lebrikizumab IGA 0/1 (≥2-pt reduction) | Placebo | EASI-75 | Placebo EASI-75 |
|---|---|---|---|---|
| ADvocate1 | 43.1% | 12.7% | 58.8% | 16.2% |
| ADvocate2 | 33.2% | 10.8% | 52.1% | 18.1% |
43-74% achieved IGA 0/1, 52-79% EASI-75, and 79% pruritus improvement vs placebo (p<0.001). Maintenance through week 52 showed sustained responses in 70-80% of initial responders. A meta-analysis confirmed lebrikizumab's efficacy comparable to dupilumab for signs/symptoms but with slightly lower binary success rates. Itch and sleep interference improved within 1-2 weeks.
Benefits of lebrikizumab
- Rapid onset: Itch reduction in 2 days; meaningful skin improvement by week 2
- Sustained efficacy: >70% maintain clearance at 1 year
- Quality of life gains: Reduced sleep loss, better daily functioning
- Targeted action: Fewer systemic effects than broad immunosuppressants
- Combination potential with topicals
Dosage and administration
Lebrikizumab is self-administered via subcutaneous injection using pre-filled syringes (250 mg/2 mL).
- Induction: 250 mg every 2 weeks for first 3 doses
- Maintenance: 250 mg every 2 weeks or every 4 weeks based on response
Inject into thigh, abdomen (avoid 5 cm around navel), or upper arm (assisted). Rotate sites; no refrigeration needed post-first use (store ≤30°C up to 21 days).
What are the side effects of lebrikizumab?
Lebrikizumab is well-tolerated; most adverse events are mild. Common (>1%):
- Conjunctivitis (7-10%; herpetic or bacterial)
- Nasopharyngitis (6%)
- Herpes infections (2-4%)
- Headache (3%)
Rare: Injection site reactions, hypersensitivity. No increased malignancy or serious infections vs placebo. Monitor eyes; discontinue if severe. Limited drug interaction data.
Pre-treatment work-up
Before starting:
- TB screening (Quantiferon or PPD)
- Recent infections/hepatitis serology
- Baseline eye exam if conjunctivitis history
- Confirm EASI/IGA eligibility
Follow-up and monitoring
Assess at weeks 16, 20, then every 16-24 weeks:
- EASI, IGA, pruritus NRS
- Eye symptoms
- Infection signs
- Adjust dosing if inadequate response
Discontinue if no improvement by week 16.
Interactions of concern
No major interactions identified; limited data. Use caution with live vaccines or strong CYP450 inducers (theoretical).
Alternative treatments
For moderate-severe AD:
| Biologic | Target | EASI-75 (Wk16) |
|---|---|---|
| Dupilumab | IL-4/13 | ~45-70% |
| Tralokinumab | IL-13 | ~25-33% |
| Abrocitinib | JAK1 | ~40-60% |
| Lebrikizumab | IL-13 | 52-79% |
Lifestyle: Emollients, trigger avoidance essential adjuncts.
Investigations underway
Ongoing trials (NCT02340234): Pediatric <12 years, long-term safety, combination therapies.
Frequently Asked Questions
Q: How quickly does lebrikizumab work?
A: Itch relief starts in 2 days; 50-60% achieve EASI-75 by week 16.
Q: Is lebrikizumab safe for long-term use?
A: Yes, 52-week data show sustained efficacy with mild, mostly ocular side effects.
Q: Can I self-inject lebrikizumab?
A: Yes, after training; pre-filled syringes for subcutaneous use every 2-4 weeks.
Q: What if I miss a dose?
A: Administer ASAP; resume schedule. If >7 days late, consult prescriber.
Q: Does insurance cover lebrikizumab?
A: Varies; prior authorization often required for moderate-severe AD.
References
- Lebrikizumab — National Eczema Society. 2023. https://eczema.org/lebrikizumab/
- Lebrikizumab effective in treating moderate-to-severe atopic dermatitis — 2 Minute Medicine. 2023. https://www.2minutemedicine.com/lebrikizumab-effective-in-treating-moderate-to-severe-atopic-dermatitis/
- The role of lebrikizumab in the treatment of atopic dermatitis — PubMed (DOI: 10.1111/1756-185X.14902). 2023-07-04. https://pubmed.ncbi.nlm.nih.gov/37401345/
- Lebrikizumab — DermNet NZ. 2024. https://dermnetnz.org/topics/lebrikizumab
- Lebrikizumab — British Association of Dermatologists Patient Hub. 2024. https://www.skinhealthinfo.org.uk/condition/lebrikizumab/
- Systemic Immunomodulatory Treatments for Atopic Dermatitis — JAMA Dermatology. 2024. https://jamanetwork.com/journals/jamadermatology/fullarticle/2821284
- Lebrikizumab for Atopic Dermatitis: 52-Week Efficacy Review — HCPLive (YouTube). 2024. https://www.youtube.com/watch?v=TKV-juerDoQ
Read full bio of Sneha Tete