Leg Ulcer: Expert Guide To Causes, Diagnosis, And Treatment
Comprehensive guide to causes, diagnosis, and management of leg ulcers for effective treatment and prevention.
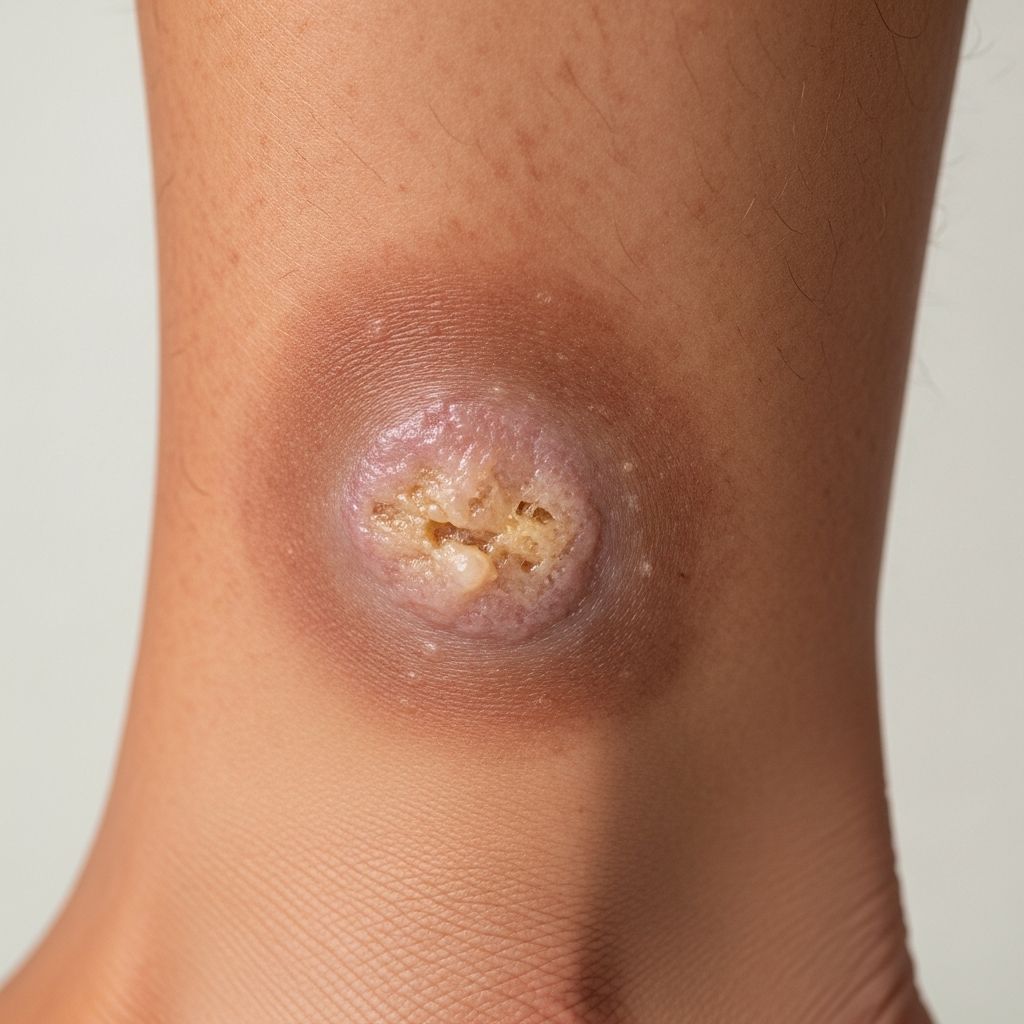
Leg ulcer
A
leg ulcer
is defined as a full-thickness skin loss on the leg or foot due to any cause. Approximately 1% of the middle-aged and elderly population is affected by leg ulceration, often precipitated by minor injury. Leg ulcers occur in association with a range of disease processes, most commonly chronic venous disease, but also arterial, neuropathic, and pressure-related issues.What is a leg ulcer?
Leg ulcers represent a significant burden on healthcare systems worldwide, affecting quality of life due to pain, immobility, and risk of infection. They are chronic wounds that fail to heal within 6 weeks and persist beyond 3 months in many cases. Full-thickness loss means the ulcer extends through the epidermis and dermis, sometimes reaching subcutaneous tissue. Common sites include the gaiter area (lower third of the leg, around the medial malleolus for venous ulcers) and distal areas for arterial types.
Who gets leg ulcers?
Leg ulcers primarily affect older adults, with prevalence increasing with age. Risk factors include:
- Age over 60 years
- History of varicose veins or deep vein thrombosis
- Obesity and sedentary lifestyle
- Smoking and peripheral arterial disease
- Diabetes mellitus leading to neuropathy
- Previous leg injury or surgery
- Family history of venous insufficiency
Women are more commonly affected by venous leg ulcers, while arterial ulcers show no strong gender bias. In populations with diabetes, neuropathic ulcers add to the complexity.
What causes leg ulcers?
Leg ulcers result from underlying vascular, neurological, or pressure-related pathologies that impair normal wound healing.
Venous leg ulcers
The most common type (70-90% of cases), venous leg ulcers arise from chronic venous insufficiency. High venous pressure (ambulatory venous hypertension) damages microcirculation, leading to skin changes like lipodermatosclerosis and eventual ulceration. Precipitating factors include superficial or deep venous reflux, often post-thrombotic.
Arterial leg ulcers
Caused by ischaemia from peripheral arterial disease, these ulcers (10-20% of cases) occur due to inadequate blood supply. Risk factors include atherosclerosis, smoking, and diabetes. Ulcers are typically distal on toes, feet, or shins.
Mixed aetiology leg ulcers
Approximately 15-20% of ulcers have both venous and arterial components, complicating management. Compression must be cautiously applied.
Neuropathic leg ulcers
Common in diabetes, these result from loss of sensation leading to repetitive trauma. They often occur on pressure points like the plantar surface.
Pressure ulcers
Develop from prolonged pressure on skin, especially in immobile patients. Stage 4 involves extensive necrosis affecting muscle and bone.
Other causes
Rare causes include vasculitis, pyoderma gangrenosum, sickle cell disease, malignancy (e.g., squamous cell carcinoma in chronic ulcers), and infections like tuberculosis or syphilis.
Clinical features of leg ulcers
Diagnosis relies on history, examination, and investigations. Key features vary by aetiology:
| Type | Location | Appearance | Edge | Base | Pain | Surrounding Skin |
|---|---|---|---|---|---|---|
| Venous | Medial malleolus, gaiter area | Shallow, irregular | Sloping | Granulating, exuding | Mild-Moderate, worse on dependency | Pigmented, varicosities, oedema |
| Arterial | Toes, feet, lateral malleolus | “Punched out”, deep | Vertical/undermined | Pale, necrotic | Severe, burning | Pale, shiny, hairless, cool |
| Neuropathic | Plantar surface | Callused edges | Well-defined | Yellow slough | Painless | Thickened skin |
| Pressure | Sacrum, heels | Deep, necrotic | Undermined | Eschar/slough | Painful if sensation intact | Macerated |
Venous ulcers often have haemosiderin pigmentation and eczema; arterial ulcers show absent pulses and claudication.
Diagnosis of leg ulcers
Take a complete medical history and thorough examination. Assess for comorbidities like diabetes or heart failure.
- Vascular studies: Ankle-brachial pressure index (ABPI) – normal 0.9-1.3; arterial <0.9; venous >0.8. Doppler ultrasound for venous reflux.
- Blood tests: Full blood count, glucose, lipids, inflammatory markers.
- Biopsy: If atypical, non-healing, or suspicious for malignancy.
- Wound swab: Only if clinical infection (pain, erythema, pus).
ABPI is mandatory before compression; values <0.8 contraindicate standard compression.
Management of leg ulcers
Treatment targets the underlying cause while promoting healing. Multidisciplinary approach is ideal.
Wound bed preparation
Cleanse: Use saline or surfactant solutions to remove debris. Avoid cytotoxic antiseptics routinely.
Debridement: Essential to remove necrotic tissue, slough, and biofilm. Methods include:
- Autolytic (hydrogels, films)
- Sharp surgical
- Enzymatic
- Biological (larval therapy)
- Mechanical
Debridement converts chronic to acute wounds, stimulating healing.
Dressings
Occlusive/moist dressings promote healing by maintaining a moist environment. Change frequency: weekly for clean ulcers; more often if exuding. Options include foams, alginates, hydrocolloids, and honey-impregnated. Avoid frequent changes to preserve healthy cells.
Compression therapy (venous ulcers)
Gold standard, healing 40-70% within 12 weeks. Options:
- Multi-layer bandaging (4-layer: wool, crepe, elastane, cohesive)
- Compression hosiery (Class 1-3 based on ankle pressure)
- Unna boot
Highest pressure at ankle, graduated upwards. Monitor ABPI regularly.
Other measures
- Pain management: Analgesics, elevation.
- Infection control: Systemic antibiotics for cellulitis (e.g., flucloxacillin); avoid topical.
- Nutrition: Protein, iron, vitamin C, zinc supplements if deficient.
- Skin grafts/flaps: For large, clean ulcers.
- Surgery: Vein ablation, arterial revascularization.
Arterial ulcer management
Revascularization (angioplasty, bypass), avoid compression, wound care, and pain control.
Prevention of pressure ulcers
Reposition every 2 hours, pressure-relieving mattresses, skin inspection.
Prevention of leg ulcers
- Weight management and exercise to improve calf pump.
- Compression hosiery for at-risk venous disease.
- Smoking cessation.
- Diabetes control and foot care.
- Skin moisturizing and emollient use.
Investigations
As detailed under diagnosis: ABPI, duplex ultrasound, biopsy, bloods.
Complications
Infection, cellulitis, osteomyelitis, malignant transformation (Marjolin ulcer), recurrence (60-70%), lymphoedema.
Recurrent leg ulcers
Common due to persistent venous hypertension. Lifelong compression hosiery post-healing is crucial.
Healing of leg ulcers
Requires optimal wound bed (TIME: Tissue, Infection, Moisture, Edge). Monitor with photography and tracing.
Frequently asked questions
What is the most common cause of leg ulcers?
Venous insufficiency accounts for 70-90% of cases.
Can leg ulcers be cured?
Many heal with appropriate treatment, but recurrence is common without maintenance therapy.
Is compression safe for all ulcers?
No; ABPI must be >0.8. Contraindicated in arterial disease.
How long do leg ulcers take to heal?
Venous ulcers: 12 weeks with compression; others vary.
Should I use topical antibiotics?
Avoid due to resistance and allergy risk; use systemic if infected.
References
- Leg ulcers – Wound healing – DermNet — DermNet NZ. 2023. https://dermnetnz.org/cme/wound-healing/leg-ulcers-cme
- Leg ulcers | Better Health Channel — Better Health Channel (VIC Gov). 2023-01-01. https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/leg-ulcers
- Leg ulcers – DermNet — DermNet NZ. 2024. https://dermnetnz.org/topics/leg-ulcer
- A complete guide to managing venous leg ulcers — Essity. 2023. https://medical-images.essity.com/images-c5/971/556971/original/a-complete-guide-to-managing-venous-leg-ulcers.pdf
- Australian and New Zealand Clinical Practice Guideline for Prevention and Management of Venous Leg Ulcers — Australian Wound Management Association. 2011-01-01. https://www.nzwcs.org.nz/images/luag/2011_awma_vlug.pdf
- Arterial ulcer – DermNet — DermNet NZ. 2024. https://dermnetnz.org/topics/arterial-ulcer
Read full bio of medha deb