Leiomyosarcoma Pathology: Histology, Diagnosis, and Clinical Features
Understanding leiomyosarcoma pathology: histological features, immunohistochemical markers, and differential diagnosis.
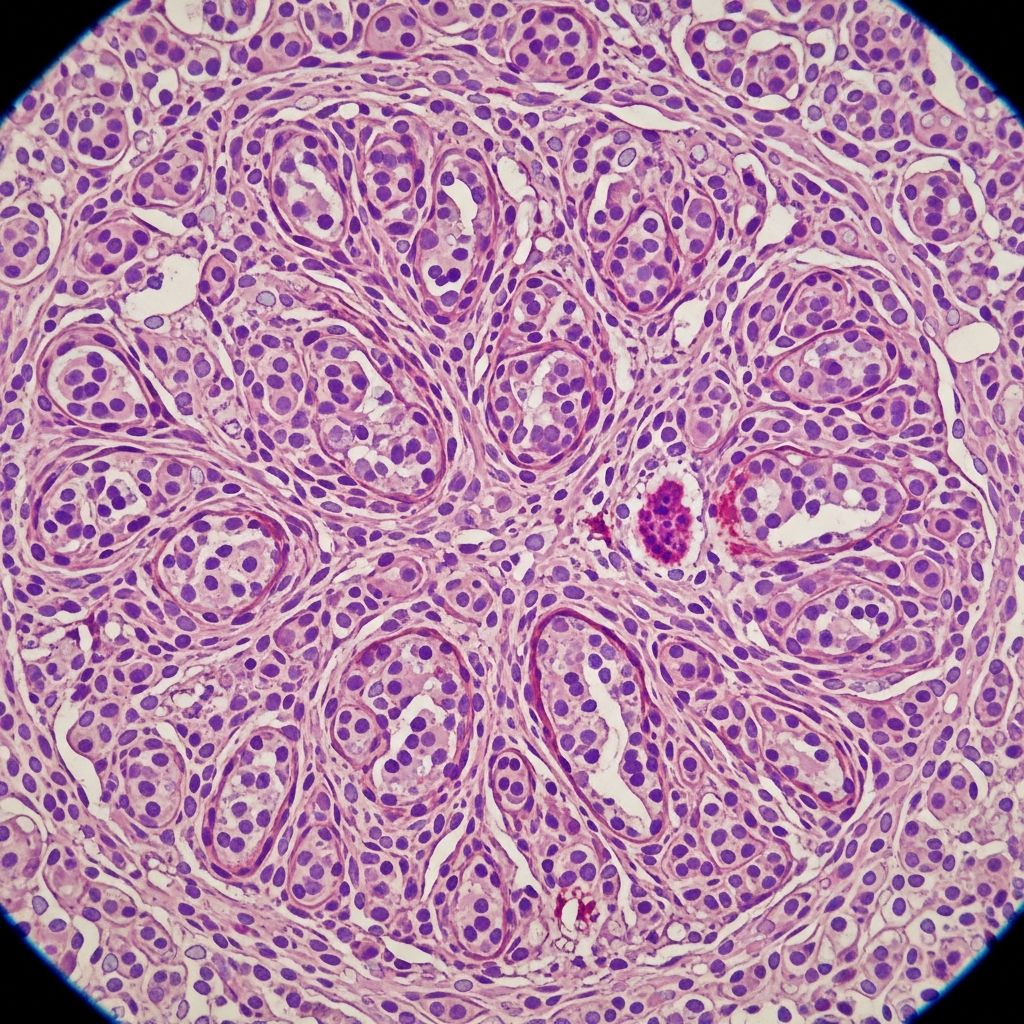
Leiomyosarcoma Pathology: Understanding the Malignant Smooth Muscle Tumor
Leiomyosarcoma is a malignant tumor of smooth muscle that rarely affects the skin, representing one of the most uncommon cutaneous malignancies encountered in dermatopathology. This aggressive neoplasm originates from smooth muscle cells or their mesenchymal precursors and can arise from various anatomical locations, including the dermis and subcutaneous tissue. The rarity of cutaneous leiomyosarcoma and its similar appearance to other spindle cell tumors frequently leads to preoperative misdiagnosis, making a comprehensive understanding of its pathological features essential for accurate diagnosis and appropriate patient management.
Overview of Leiomyosarcoma
Leiomyosarcoma is classified as one of the most common subtypes of soft tissue sarcoma, though cutaneous presentation is exceptionally rare. The tumor exhibits aggressive biological behavior with significant potential for local recurrence and distant metastasis. Unlike its benign counterpart, leiomyoma, which is a common benign smooth muscle tumor, leiomyosarcoma demonstrates malignant characteristics both histologically and clinically. The distinction between these two entities is critical, as management and prognosis differ substantially.
Histological Features of Leiomyosarcoma
Architectural Characteristics
On scanning power examination, leiomyosarcoma demonstrates a poorly circumscribed tumor nodule that may be located in either the dermis (dermal leiomyosarcoma) or deeply infiltrating into the subcutaneous tissue (subcutaneous leiomyosarcoma). This infiltrative growth pattern distinguishes leiomyosarcoma from benign leiomyomas, which typically exhibit well-defined, non-infiltrating borders. The tumor architecture consists of a spindle cell proliferation organized into rough bundles and fascicles, reminiscent of normal smooth muscle but with abnormal features.
Grossly, leiomyosarcomas are typically solitary, well-circumscribed lesions that frequently demonstrate areas of cystic degeneration and necrosis. The presence of necrosis is a critical feature in establishing malignancy. The infiltrative borders and lack of encapsulation distinguish malignant tumors from their benign counterparts.
Cytological Features
High-power microscopy reveals spindle cells with characteristic cigar-shaped nuclei displaying prominent cytologic atypia and numerous mitotic figures. The nuclei demonstrate irregular membranes, coarse chromatin, and conspicuous nucleoli. The presence of significant nuclear atypia is a hallmark finding that helps differentiate leiomyosarcoma from benign smooth muscle proliferations.
Mitotic activity is substantially elevated in malignant lesions, with leiomyosarcoma typically showing greater than 5 to 10 mitoses per high-power field (HPF). This high mitotic rate, particularly when accompanied by atypical mitotic figures, supports a diagnosis of malignancy. The combination of nuclear atypia, increased mitotic activity, and tumor necrosis comprises the diagnostic triad for leiomyosarcoma.
Histological Subtypes
Leiomyosarcomas can be further subdivided based on cellular morphology and architectural patterns. The classic spindle cell type represents the most common form, characterized by spindle-shaped cells arranged in intersecting fascicles. Epithelioid leiomyosarcoma, comprising more than 50% epithelial-appearing cells, can be particularly challenging diagnostically as it may mimic carcinoma. Myxoid variants display hypocellular areas with basophilic stroma and represent a less common presentation. These histological variations underscore the morphological heterogeneity within this tumor category.
Immunohistochemical Profile
Muscle-Specific Markers
Immunoperoxidase staining is positive for multiple muscle-specific markers that confirm smooth muscle differentiation. The standard panel includes:
- Smooth muscle actin (SMA) — consistently positive in leiomyosarcoma
- HHF35 (pan muscle actin) — demonstrates broad muscle cell positivity
- h-caldesmon — highly specific for smooth muscle differentiation
- Desmin — typically positive, though negative staining occurs infrequently
The consistent expression of these muscle markers is essential for confirming the diagnosis of leiomyosarcoma and differentiating it from other spindle cell malignancies.
Additional Immunohistochemical Findings
A rare subset of leiomyosarcomas demonstrates cytokeratin or epithelial membrane antigen (EMA) staining, which can create diagnostic confusion, particularly in epithelioid variants. When epithelioid leiomyosarcoma exhibits EMA positivity, additional immunostains including histone deacetylase-8 (HDAC8) and myocardin help confirm smooth muscle origin and exclude carcinoma. Proliferation markers such as Ki-67 demonstrate high indices in malignant lesions compared to benign tumors. Immunopositivity for p16 and p53 with elevated Ki-67 proliferation index has demonstrated high sensitivity and specificity for differentiating leiomyosarcoma from leiomyomas.
Cutaneous Leiomyosarcoma Subtypes
Dermal Leiomyosarcoma
Superficial dermal leiomyosarcoma is believed to originate from arrector pili muscles and sweat gland smooth muscle. This variant typically presents as a relatively superficial lesion confined primarily to the dermis, though it may extend into superficial subcutaneous tissue. Dermal-based leiomyosarcomas are generally smaller at presentation compared to subcutaneous variants and may have somewhat different clinical behavior.
Subcutaneous Leiomyosarcoma
Subcutaneous leiomyosarcoma arises from the vascular smooth muscle of subcutaneous adipose tissue. This variant demonstrates more aggressive biological behavior and is typically diagnosed at a more advanced stage, resulting in larger lesions at presentation. Subcutaneous tumors show substantially higher recurrence rates (50–70%) and increased risk of distant metastases (up to 60%). The deeper location and larger size at diagnosis contribute to worse overall prognosis compared to superficial dermal lesions.
Diagnostic Criteria and Classification
Establishing Malignancy
Reliable criteria for establishing malignancy in cutaneous leiomyosarcomas remain somewhat subjective, though guidelines derived from uterine tumors provide useful reference points. Critical diagnostic features include:
- Tumor size greater than 5.5 cm
- Mitotic count greater than 7 per 10 high-power fields in the presence of significant nuclear atypia
- Presence of tumor cell necrosis
- Significant nuclear pleomorphism and irregularity
- Infiltrative growth pattern
The cumulative assessment of these features supports a diagnosis of leiomyosarcoma rather than a benign or intermediate lesion.
Atypical Leiomyoma
Atypical leiomyoma represents an intermediate category on the spectrum between benign leiomyoma and leiomyosarcoma. These lesions lack definitive criteria for malignancy but demonstrate concerning features. They typically show moderate to significant nuclear atypia but lack tumor necrosis and maintain relatively low mitotic rates (fewer than 5 mitoses per 10 high-power fields).
Mitotically Active Leiomyoma
The category of mitotically active leiomyoma applies to lesions lacking significant nuclear atypia or tumor necrosis but demonstrating elevated mitotic activity between 5 and 15 mitoses per high-power field. These tumors represent an intermediate category distinct from both typical benign leiomyomas and frank leiomyosarcomas, and they require careful clinical follow-up and consideration of adjuvant therapy.
Differential Diagnosis
Spindle cell leiomyosarcoma may mimic several other malignant spindle cell tumors, necessitating careful histological examination and immunohistochemical correlation. Important differential diagnoses include:
- Spindle cell squamous cell carcinoma — typically positive for cytokeratin markers and negative for muscle-specific antigens
- Malignant peripheral nerve sheath tumor (MPNST) — demonstrates S-100 protein positivity and negative muscle markers
- Spindle cell melanoma — positive for melanoma markers (S-100, Melan-A, SOX10) and negative for muscle markers
- Angiosarcoma — demonstrates vascular differentiation with CD31 and CD34 positivity; lacks muscle marker expression
- Atypical fibroxanthoma — typically positive for CD68 and CD10; variable cytokeratin and focal muscle marker staining
Immunoperoxidase staining is typically required to differentiate between these lesions and establish the correct diagnosis of leiomyosarcoma. The specific panel of antibodies used should include muscle-specific markers to confirm smooth muscle origin.
Molecular and Genetic Features
Leiomyosarcomas are primarily associated with mutations in tumor suppressor genes, particularly RB1 and PTEN. RB1 gene mutations are observed in approximately 90% of patients with leiomyosarcoma, representing the most common genetic abnormality. The cytogenetic and molecular changes in leiomyosarcoma are complex and inconsistent, contributing to the tumor’s biological heterogeneity. Additionally, leiomyosarcoma is characterized by complex and unbalanced karyotypes with severe genomic instability resulting in multiple genetic aberrations.
Clinical Presentation and Location
Cutaneous leiomyosarcoma most commonly presents on the extremities and trunk, with the proximal arm being a frequently reported site. Patients typically present with a solitary nodule or mass that may have been enlarging gradually. Unlike benign leiomyomas, which are often painful, leiomyosarcomas may be relatively asymptomatic. The clinical presentation varies depending on the tumor’s location within the skin layers and its size at presentation.
Prognosis and Prognostic Factors
Prognosis in leiomyosarcoma depends on multiple factors including tumor location, size, histological grade, and depth of invasion. Superficial dermal leiomyosarcomas generally have better prognosis than subcutaneous variants, though local recurrence rates remain substantial at 30–50% for dermal lesions and 50–70% for subcutaneous tumors. Distant metastases occur in up to 60% of subcutaneous cases. Tumor grade significantly impacts overall survival, with higher-grade lesions associated with increased risk of distant metastasis. Age and patient performance status also influence treatment decisions and outcomes.
Frequently Asked Questions (FAQs)
Q: How is leiomyosarcoma distinguished from benign leiomyoma on histology?
A: Key distinguishing features include infiltrative growth pattern, significant nuclear atypia, mitotic rate exceeding 5-10 per high-power field, tumor necrosis, and lack of a well-defined capsule. Leiomyomas demonstrate well-circumscribed borders, minimal cytologic atypia, and low mitotic activity.
Q: What is the role of immunohistochemistry in diagnosing leiomyosarcoma?
A: Immunohistochemistry confirms smooth muscle differentiation through positivity for muscle-specific markers (SMA, HHF35, h-caldesmon, and Desmin) and helps differentiate leiomyosarcoma from other spindle cell malignancies that typically show different staining patterns.
Q: Are cutaneous leiomyosarcomas often misdiagnosed initially?
A: Yes, preoperative misdiagnosis is common because cutaneous leiomyosarcoma is a rare malignant tumor. The diagnosis is definitively established through histopathological and immunohistochemical studies rather than clinical examination alone.
Q: What is the difference between dermal and subcutaneous leiomyosarcoma?
A: Dermal leiomyosarcoma originates from arrector pili muscles and sweat glands, is typically smaller, and has lower recurrence rates (30–50%). Subcutaneous leiomyosarcoma arises from vascular smooth muscle, is usually larger, diagnosed at advanced stages, and demonstrates higher recurrence (50–70%) and metastasis rates (up to 60%).
Q: What immunostains should be used when epithelioid leiomyosarcoma is suspected?
A: When epithelioid leiomyosarcoma shows EMA positivity mimicking carcinoma, additional immunostains including HDAC8, myocardin, p16, and p53 along with Ki-67 proliferation index help confirm smooth muscle origin and exclude carcinoma.
References
- Primary leiomyosarcoma of the skin. A histological and immunohistochemical study — PubMed/NCBI. https://pubmed.ncbi.nlm.nih.gov/8103264/
- Leiomyosarcoma pathology — DermNet New Zealand. https://dermnetnz.org/topics/leiomyosarcoma-pathology
- Leiomyosarcoma — StatPearls — National Center for Biotechnology Information Bookshelf. 2025. https://www.ncbi.nlm.nih.gov/books/NBK551667/
- A rare cutaneous soft tissue neoplasm: Clinicopathologic Features of Cutaneous Leiomyosarcoma — Esculapio Medical. https://esmed.org/MRA/mra/article/view/6437
- Leiomyoma — DermNet — DermNet New Zealand. https://dermnetnz.org/topics/leiomyoma
Read full bio of Sneha Tete










