Leptospirosis Explained
Understand leptospirosis: causes, symptoms, prevention, and treatment of this bacterial infection from contaminated water and animals.
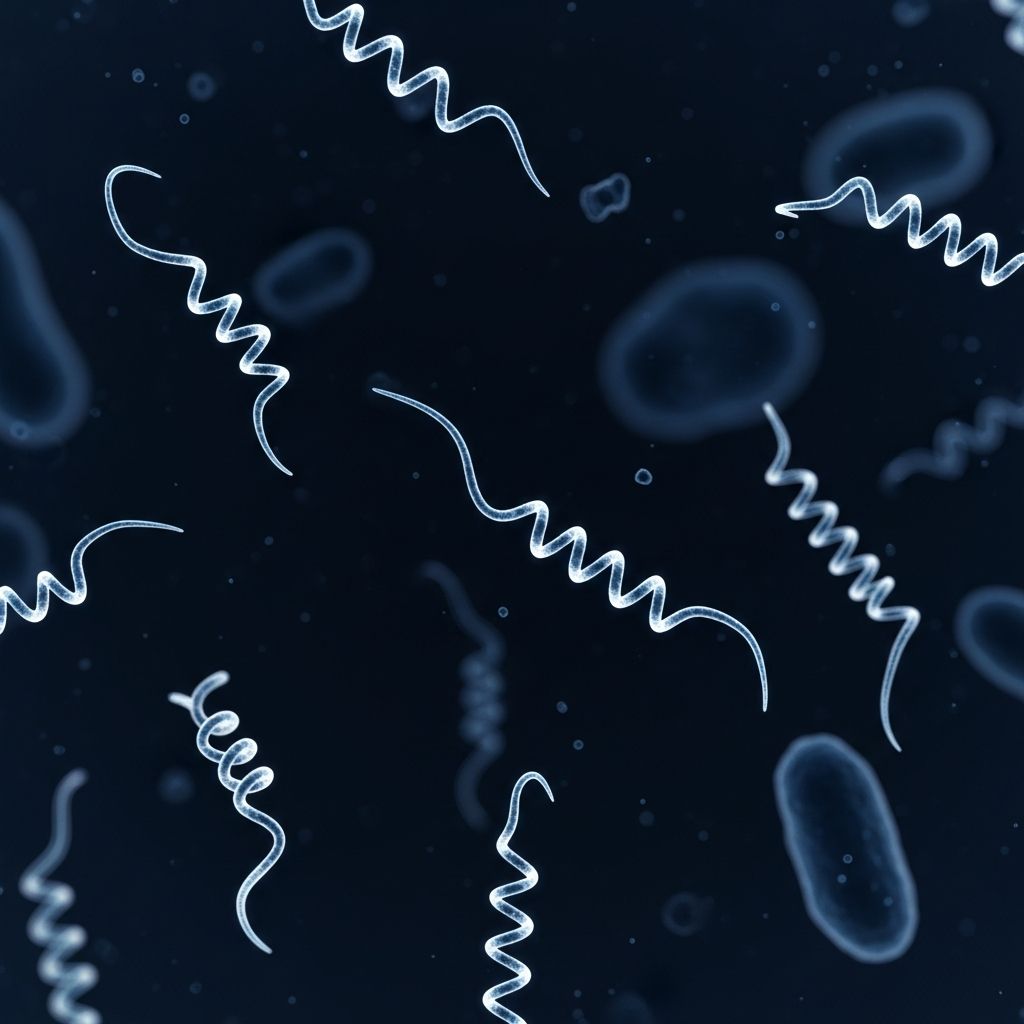
Leptospirosis represents a significant global health concern, caused by bacteria from the genus Leptospira. This zoonotic infection spreads primarily through contact with water, soil, or food contaminated by infected animal urine, affecting over 1 million people annually worldwide.
The Nature of Leptospira Bacteria
Leptospira species are spiral-shaped, motile bacteria thriving in warm, moist environments. Over 300 serovars exist, with common pathogens like L. interrogans responsible for human cases. These microbes survive outside hosts for weeks in favorable conditions, particularly in tropical regions or after heavy rains.
Rodents, dogs, cattle, and pigs serve as primary reservoirs, shedding bacteria in urine without showing symptoms. Humans act as accidental hosts, acquiring infection through skin abrasions or mucous membranes.
How Infection Spreads
Transmission occurs via direct or indirect exposure to infected urine. Common scenarios include wading in floodwaters, farming in wet fields, or handling wildlife. Urban outbreaks link to rat-infested sewers during monsoons.
- Contaminated recreational water like rivers or lakes
- Agricultural work involving soil or livestock
- Veterinary care without protection
- Adventure activities such as kayaking or canyoning
- Pet contact, especially unvaccinated dogs
Person-to-person spread is rare, except via breastfeeding or sex in severe cases.
Recognizing Early Symptoms
After exposure, symptoms emerge 2-30 days later, averaging 5-14 days. Initial presentation mimics influenza: high fever, chills, severe headache, and muscle pain, particularly in calves and back.
Additional signs include:
- Conjunctival suffusion (red eyes without discharge)
- Nausea, vomiting, diarrhea
- Photophobia and neck stiffness
- Fatigue and rash
This septicemic phase lasts 3-10 days, sometimes resolving briefly before worsening.
Progression to Severe Disease
Approximately 10% of cases advance to the immune phase, targeting kidneys, liver, and lungs. Weil’s disease, the most severe form, features jaundice, acute kidney injury, and bleeding tendencies.
| Severe Complication | Symptoms | Organs Affected |
|---|---|---|
| Weil’s Syndrome | Yellow skin/eyes, oliguria, hemorrhage | Liver, Kidneys |
| Pulmonary Hemorrhage | Coughing blood, respiratory distress | Lungs |
| Meningitis | Altered mental status, seizures | Brain/Spinal Cord |
| Multi-Organ Failure | Shock, arrhythmias | Heart, Multiple |
In dogs, signs parallel human ones: lethargy, vomiting, jaundice, increased thirst, and potential pulmonary hemorrhage. Untreated, mortality reaches 60,000 yearly, highest in resource-poor settings.
Diagnostic Approaches
Diagnosis combines clinical suspicion, exposure history, and lab tests. Key indicators: fever with conjunctival suffusion post-flood exposure.
Laboratory Methods:
- Microscopic Agglutination Test (MAT): Gold standard, detects antibodies
- PCR: Identifies bacterial DNA in blood/urine early
- Serology: IgM ELISA for immune phase
- Urinalysis: Reveals kidney damage, bacteria
Bloodwork shows elevated creatinine, bilirubin, thrombocytopenia. Chest imaging confirms lung involvement. Differential diagnoses include dengue, malaria, and sepsis.
Treatment Protocols
Early antibiotics like doxycycline or penicillin shorten illness and prevent severity. Severe cases require IV penicillin G or ceftriaxone, plus supportive care: hydration, dialysis for kidney failure, ventilation for respiratory distress.
For dogs, aggressive antibiotics and hospitalization improve outcomes. Recovery spans weeks to months; chronic kidney issues may persist.
Prevention Strategies
Avoiding exposure is paramount. Key measures include:
- Wearing protective footwear and clothing in risk areas
- Avoiding floodwater contact
- Vaccinating pets annually against common serovars
- Doxycycline prophylaxis for high-risk travelers (200mg weekly)
- Rodent control in communities
Public health campaigns emphasize hygiene post-floods.
Leptospirosis in Animals
Dogs suffer most among pets, transmitting to owners via urine. Symptoms: anorexia, abdominal pain, polyuria. Vaccination reduces incidence but doesn’t cover all serovars.
Livestock like cattle shed asymptomatically, posing farm risks. Wildlife reservoirs remain unvaccinable.
Epidemiology and Global Burden
Tropical climates foster outbreaks; Hawaii reports cases yearly from recreation. Over 1 million infections occur globally, with higher fatality in elderly or comorbid patients. Climate change expands mosquito-free flood risks.
FAQs
What is the incubation period for leptospirosis?
Typically 5-14 days, ranging 2-30 days after exposure.
Can leptospirosis spread from person to person?
Rarely; mainly through contaminated environment, not direct contact.
Is there a vaccine for humans?
No universal vaccine; pet vaccines exist but serovar-limited.
How do I know if my dog has leptospirosis?
Look for vomiting, jaundice, lethargy; vet testing confirms.
What should I do after flood exposure?
Monitor for fever; seek care if symptoms appear, consider prophylaxis.
Leptospirosis demands vigilance, especially in wet seasons. Prompt recognition saves lives.
References
- About Leptospirosis — Centers for Disease Control and Prevention. 2023. https://www.cdc.gov/leptospirosis/about/index.html
- Leptospirosis — Hawaii State Department of Health. 2024-01-15. https://health.hawaii.gov/docd/disease_listing/leptospirosis/
- Canine Leptospirosis — Cornell University College of Veterinary Medicine. 2023-05-10. https://www.vet.cornell.edu/departments-centers-and-institutes/riney-canine-health-center/canine-health-topics/canine-leptospirosis
- Leptospirosis Fact Sheet — Pennsylvania Department of Health. 2022-08-22. https://www.pa.gov/content/dam/copapwp-pagov/en/health/documents/topics/documents/diseases-and-conditions/Leptospirosis%20.pdf
- Leptospirosis: Causes, Symptoms, Diagnosis & Treatment — Cleveland Clinic. 2024-03-12. https://my.clevelandclinic.org/health/diseases/24021-leptospirosis
- Leptospirosis: clinical aspects — National Center for Biotechnology Information (PMC). 2022-02-01. https://pmc.ncbi.nlm.nih.gov/articles/PMC8813018/
- Leptospirosis in dogs — American Veterinary Medical Association. 2023-11-05. https://www.avma.org/resources-tools/pet-owners/petcare/leptospirosis
Read full bio of Sneha Tete