Lichen Simplex of the Scrotum
Understanding the causes, symptoms, diagnosis, and effective treatments for lichen simplex chronicus affecting the scrotal skin.
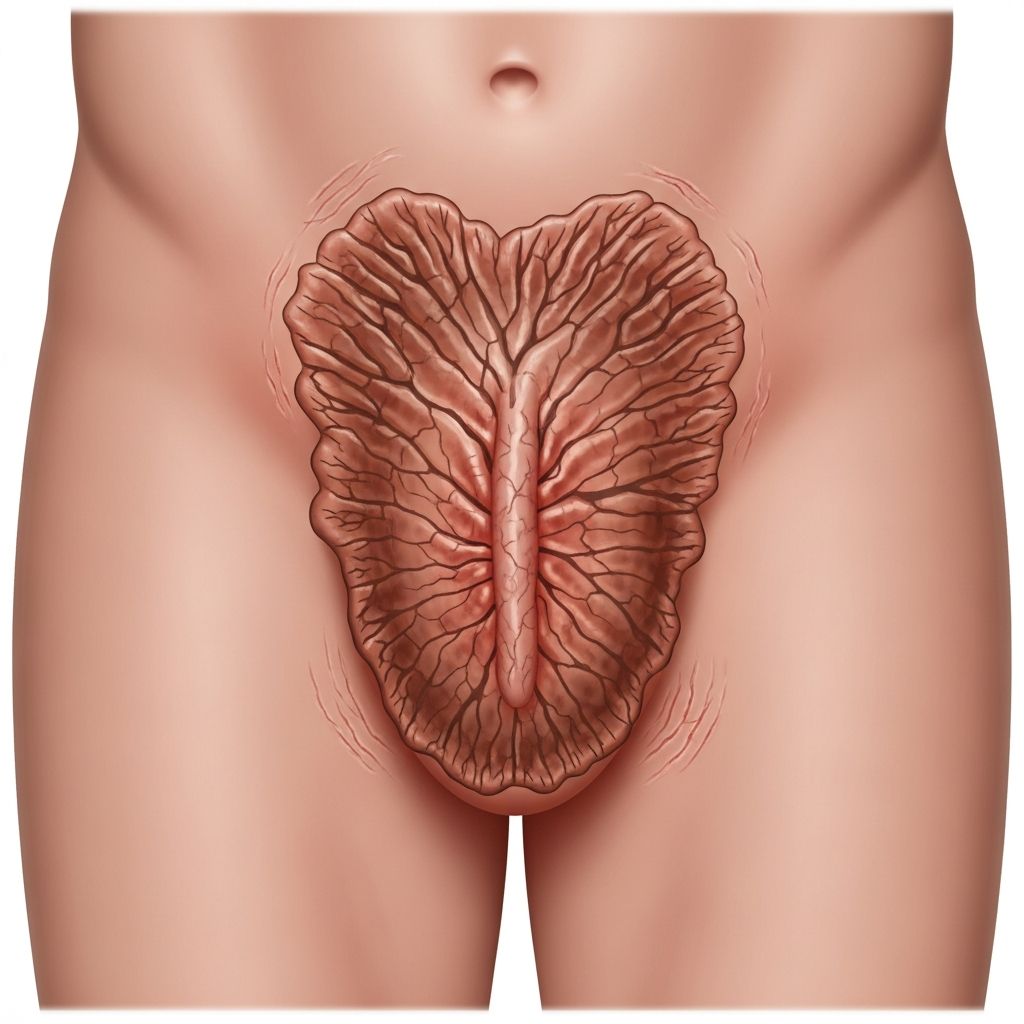
Lichen simplex of the scrotum, also known as lichen simplex chronicus or neurodermatitis in the genital area, represents a common dermatological condition characterized by localized, well-defined plaques of thickened skin resulting from habitual scratching or rubbing. This benign but often persistent disorder primarily affects the scrotal skin due to its thin, sensitive nature and propensity for itchiness. The condition arises from a vicious cycle where an initial itch prompts scratching, which in turn thickens the skin (lichenification), intensifying the itch further. While not life-threatening, it can significantly impair quality of life due to discomfort, embarrassment, and sleep disruption from nocturnal pruritus.
What is Lichen Simplex of the Scrotum?
Lichen simplex chronicus is a form of acquired skin thickening secondary to repetitive mechanical trauma from scratching or rubbing. When localized to the scrotum, it manifests as hyperkeratotic, leathery plaques with exaggerated skin markings. The scrotal involvement is particularly common in middle-aged to older men, often linked to underlying factors such as sacral radiculopathy or emotional stress. Patients typically present with one or more discrete, oval or irregular patches on the scrotum that feel rough and exhibit intensified creases. The overlying skin may appear hyperpigmented, especially in darker skin types, and the lesions are notoriously pruritic, worsening at night or with heat and perspiration.
The pathophysiology involves repeated epidermal injury leading to hyperkeratosis, acanthosis, and dermal fibrosis. Neurogenic inflammation plays a key role, with altered sensory nerve processing amplifying itch signals. Individuals with a history of atopy, anxiety disorders, or nonspecific emotional stress are predisposed, as these heighten itch perception.
Who Gets Lichen Simplex of the Scrotum?
This condition predominantly affects adult males, with peak incidence between ages 30 and 60. Risk factors include:
- Atopic background: Patients with eczema, asthma, or hay fever are more susceptible due to inherent skin barrier defects and itch proneness.
- Neurological factors: Sacral sensory neuron radiculopathy, such as from lumbar disc herniation or spinal stenosis, can initiate scrotal itch via referred neuropathic pain.
- Psychological stressors: Anxiety, depression, or chronic stress exacerbate scratching behaviors, perpetuating the itch-scratch cycle.
- Local irritants: Tight clothing, excessive sweating, or poor hygiene can trigger initial pruritus in susceptible individuals.
- Other associations: Rarely linked to insect bites, contact dermatitis, or unresolved scars that serve as itch foci.
Men with scrotal lichen simplex often report a prodromal itch without visible rash, progressing to lichenified plaques over weeks to months. Prevalence is higher in humid climates where perspiration aggravates symptoms.
What Causes Lichen Simplex of the Scrotum?
The primary mechanism is the itch-scratch cycle: an initial pruritic stimulus—whether neuropathic, atopic, psychogenic, or irritant—leads to scratching, causing microtrauma. This induces epidermal hyperplasia and releases inflammatory mediators like substance P and nerve growth factor, sensitizing itch receptors (C-fibers). Over time, central sensitization in the spinal cord amplifies itch perception, making it intractable.
Specific scrotal triggers include:
- Sacral radiculopathy disrupting sensory nerves (S2-S4 dermatomes).
- Hyperhidrosis and frictional irritation from underwear.
- Psychosomatic factors, where stress lowers itch thresholds.
- Secondary infection or superinfection from scratching, though rare.
Unlike generalized dermatitis, scrotal lichen simplex is focal, emphasizing localized perpetuation.
What are the Clinical Features of Lichen Simplex of the Scrotum?
Classic presentation includes:
- Lesion morphology: Solitary or multiple, well-circumscribed, hyperkeratotic plaques 2-10 cm in diameter, with a leathery texture and prominent skin furrows in a criss-cross pattern.
- Color and scaling: Erythematous to hyperpigmented; dry, scaling surface with possible excoriations.
- Symptoms: Intense pruritus, worse nocturnally or post-shower; burning or stinging if eroded.
- Distribution: Central scrotum most common; may extend to perineum or inner thighs.
- Associated signs: Nail biting, fidgeting, or other neurodermatitis sites (e.g., ankles, neck).
Lesions evolve from subtle erythema to thickened plaques over months. Chronic cases show fibrosis, reducing itch but causing cosmetic disfigurement.
Diagnosis
Diagnosis is primarily clinical, based on history of chronic rubbing/scratching and characteristic lichenified plaques. Key diagnostic features:
- History: Insidious onset pruritus leading to habitual scratching.
- Examination: Lichenification with exaggerated folds.
Investigations:
- Skin scraping/biopsy if malignancy suspected: Shows compact hyperkeratosis, acanthosis, elongated rete ridges, thickened basement membrane, and superficial perivascular lymphocytic infiltrate.
- Swabs for bacterial/fungal culture if oozing or pustules present.
- Neurological exam or MRI spine for suspected radiculopathy.
Differential Diagnosis
| Condition | Key Distinguishing Features |
|---|---|
| Psoriasis | Well-defined plaques with silvery scale; Auspitz sign; nail changes; less pruritic. |
| Lichen planus | Polygonal violaceous papules; Wickham striae; oral involvement; hypertrophic variant similar but Wickham striae on histo. |
| Atopic dermatitis | Diffuse erythema, oozing; flexural distribution; personal/family atopy history. |
| Contact dermatitis | Geometric pattern matching irritant; resolves with avoidance. |
| Mycosis fungoides | Poikilodermatous patches; progression to tumors; epidermotropism on biopsy. |
| Squamous cell carcinoma | Ulcerated, indurated nodule; rapid growth; keratin pearls on biopsy. |
| Fungal infection | Annular lesions; KOH positive; responds to antifungals. |
Biopsy resolves most doubts, especially to exclude neoplasia in longstanding lesions.
Treatment of Lichen Simplex of the Scrotum
Management targets breaking the itch-scratch cycle via itch suppression, skin barrier repair, and behavioral modification. Multidisciplinary approach often required.
General Measures
- Patient education: Explain itch-scratch cycle; encourage itch awareness and alternatives like tapping.
- Hygiene: Gentle cleansing with emollients; loose cotton underwear; avoid irritants.
- Occlusion: Cover lesions with occlusive dressings post-topical application to enhance penetration and prevent scratching.
Topical Therapies
- Corticosteroids: First-line; potent (e.g., clobetasol 0.05%) twice daily for 2-4 weeks under occlusion, then taper. Intralesional triamcinolone for thick plaques.
- Emollients: Frequent application to hydrate and soften lichenified skin.
- Antipruritics: Capsaicin cream (desensitizes nerves); doxepin or menthol preparations.
- Others: Coal tar, ichthyol for anti-pruritic effects; calcineurin inhibitors (tacrolimus) steroid-sparing.
Systemic Therapies
- Sedating antihistamines (e.g., hydroxyzine) at bedtime for nocturnal itch.
- Antibiotics if secondarily infected.
- Gabapentinoids or antidepressants (e.g., doxepin) for neuropathic component.
Advanced Interventions
- Phototherapy: UVB/NB-UVB contraindicated in genitals; consider for extra-genital sites.
- Injections: Botulinum toxin for refractory cases (reduces neurogenic itch).
- Surgery: Cryotherapy or excision for localized, persistent plaques.
- Psychotherapy: CBT or stress management if psychogenic.
Response typically seen in 4-6 weeks; recurrence common without adherence.
Frequently Asked Questions (FAQs)
Q: Is lichen simplex of the scrotum cancerous?
A: No, it is a benign reactive dermatosis. However, longstanding lesions warrant biopsy to exclude squamous cell carcinoma.
Q: How long does treatment take?
A: Initial improvement in 2-4 weeks with potent topicals; full resolution may take months. Maintenance therapy prevents relapse.
Q: Can it spread to other areas?
A: Focal by nature, but multifocal lesions occur in atopics. Treat underlying itch predisposition.
Q: Why does it itch more at night?
A: Reduced distractions amplify sensations; circadian cortisol dip heightens itch. Sedating antihistamines help.
Q: Are there home remedies?
A: Cool compresses, emollients, and distraction techniques aid; consult dermatologist for prescription topicals.
Prognosis
With treatment, most cases improve markedly, though genital sites like scrotum are prone to persistence due to inaccessibility and ongoing irritation. Relapse rates high without behavioral change; early intervention key to preventing fibrosis.
References
- Lichen Simplex Chronicus – StatPearls — James et al., NCBI Bookshelf. 2023-07-17. https://www.ncbi.nlm.nih.gov/books/NBK499991/
- Lichen Simplex Chronicus – Dermatologic Disorders — Merck Manuals Professional Edition. 2024-05-01. https://www.merckmanuals.com/professional/dermatologic-disorders/dermatitis/lichen-simplex-chronicus
- Lichen Simplex Chronicus – MSD Manuals — MSD Manuals Professional Edition. 2024-05-01. https://www.msdmanuals.com/professional/dermatologic-disorders/dermatitis/lichen-simplex-chronicus
- Lichen Simplex: Causes and Treatment — Patient.info. 2023-11-15. https://patient.info/doctor/dermatology/lichen-simplex
- Lichen Simplex Chronicus (Neurodermatitis): Key Facts & Care — Indiana University School of Medicine Dermatology Trials. 2024-02-20. https://dermatrials.medicine.iu.edu/blogs/guide-about-lichen-simplex-chronicus-neurodermatitis
- Lichen Simplex Chronicus (Neurodermatitis) — Cleveland Clinic. 2023-09-12. https://my.clevelandclinic.org/health/diseases/17989-neurodermatitis
Read full bio of medha deb