Lichen Simplex Of The Vulva: A Comprehensive Clinical Guide
Understanding lichen simplex of the vulva: causes, symptoms, diagnosis, and effective treatments for this chronic itchy condition.
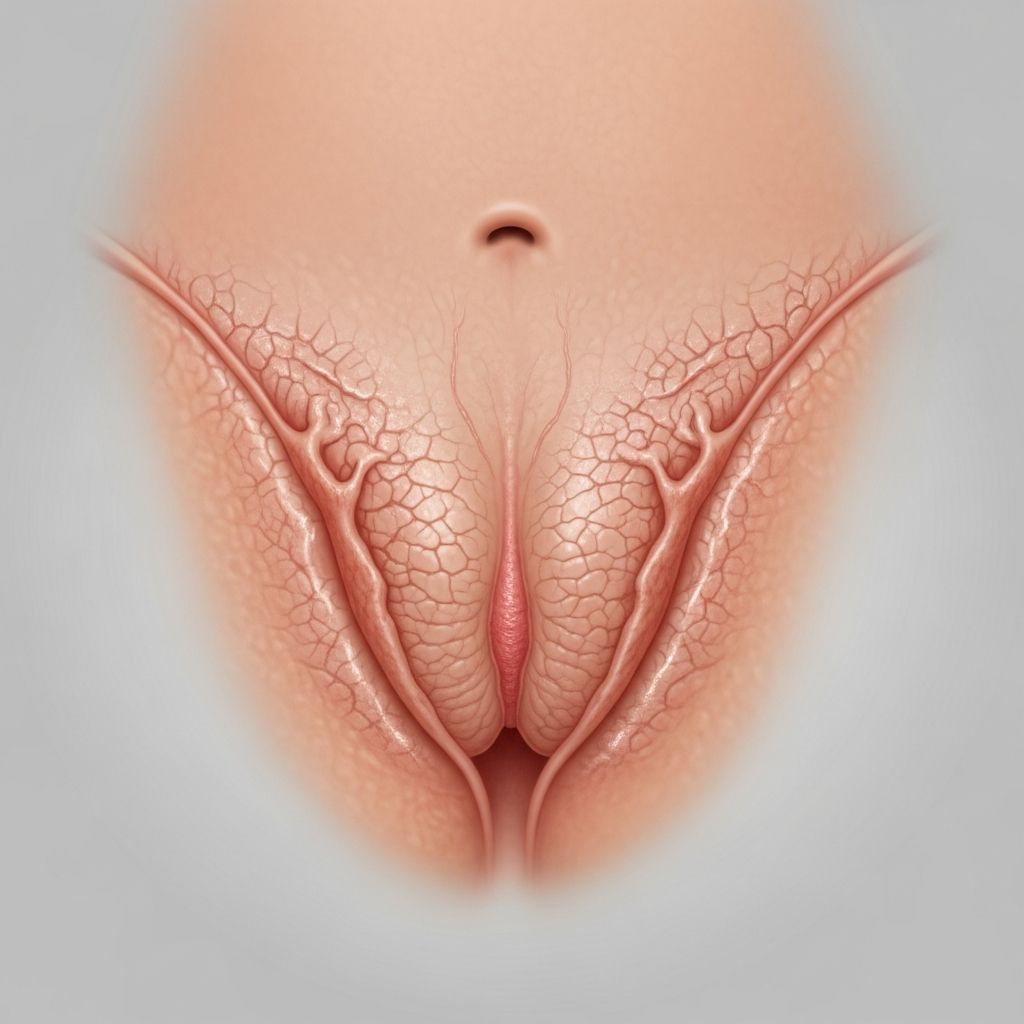
Lichen simplex of the vulva is a chronic pruritic dermatitis characterised by excessive scratching or rubbing, resulting in well-demarcated, thickened plaques on the vulvar skin.
Introduction
Lichen simplex of the vulva represents a pattern of chronic dermatitis driven by the itch-scratch cycle. It manifests as erythematous or hyperpigmented, lichenified plaques typically affecting one or both labia majora. This condition arises secondary to underlying pruritic disorders, where habitual scratching thickens the epidermis (acanthosis) and stratum corneum (hyperkeratosis). Unlike primary inflammatory dermatoses, lichen simplex is a reactive process that perpetuates itself through mechanical trauma. Early intervention is crucial to interrupt this cycle and prevent complications like scarring or secondary infections.
Patients often present with intense vulvar itching, leading to scratching that worsens the skin changes. The vulva’s thin, moist environment exacerbates irritation, making management challenging. This article details the demographics, causes, clinical presentation, complications, diagnosis, differential diagnoses, and comprehensive treatment approaches based on clinical evidence.
Demographics
Lichen simplex chronicus (LSC) of the vulva predominantly affects adult women, particularly those in middle age, though it can occur across all age groups. It is more common in individuals with a history of atopy, such as eczema or psoriasis, which predispose to pruritus. Women with vulvar LSC often report psychological stressors or anxiety, contributing to habitual scratching behaviours. Prevalence data is limited, but it is recognised as one of the most common causes of chronic vulvar pruritus in dermatology and gynaecology clinics. Postmenopausal women may experience exacerbated symptoms due to oestrogen deficiency, leading to skin dryness and fragility. Risk factors include obesity, diabetes, and neurological conditions that heighten itch perception.
Causes
The primary mechanism is the persistent itch–scratch cycle, where initial pruritus from various triggers induces scratching, causing skin thickening that further sensitises nerves, perpetuating itch. Common underlying causes include:
- Infections: Candidiasis (yeast infections) is the most frequent trigger, causing initial inflammation.
- Contact irritants: Harsh soaps, perfumed products, synthetic underwear, or sanitary pads provoke dermatitis.
- Atopic conditions: Eczema, psoriasis, or lichen sclerosus overlay.
- Neuropathic itch: Vulvodynia or nerve irritation without visible skin changes initially.
- Systemic factors: Diabetes, thyroid disease, or generalised pruritus requiring workup.
- Psychiatric contributors: Stress, anxiety, or obsessive-compulsive tendencies amplify scratching.
Identifying and treating the root cause is essential, as LSC is often secondary.
Clinical Features
Characteristic findings include well-demarcated plaques on the labia majora, minora, or perineum, appearing as thickened, leathery skin with exaggerated skin markings (lichenification). Colours range from pink/red to violaceous, hyperpigmented, or hypopigmented, with possible excoriations, fissuring, or crusting. Symptoms are:
- Severe pruritus, worse at night, disrupting sleep.
- Burning or soreness from scratching.
- Dyspareunia (painful intercourse) due to fissuring.
- Swelling and warmth in acute phases.
Skin may feel velvety or rough, with bilateral symmetry common but unilateral cases possible. In advanced stages, fibrosis leads to scarring and architectural distortion.
Complications
Untreated LSC can result in significant morbidity:
- Scarring and fibrosis: Thickened, contracted tissue causing introital narrowing and sexual dysfunction.
- Secondary infections: Bacterial (e.g., Staphylococcus) or fungal superinfections from breaks in skin barrier.
- Psychosocial impact: Chronic itch affects quality of life, sleep, and mental health, potentially leading to anxiety or depression.
- Vulvar distortion: Labial fusion or clitoral burial in severe cases.
- Chronic pain: Post-inflammatory hyperpigmentation or neuropathy.
Early treatment prevents progression to irreversible changes.
Diagnosis
Diagnosis is primarily clinical, based on history of chronic pruritus and examination revealing lichenified plaques. Key steps include:
- Detailed history: Itch triggers, scratching habits, atopy, infections, irritants.
- Vulvoscopy: Magnified view for subtle lichenification or candidiasis.
- Swabs/cultures: For candida, bacteria, or herpes.
- Biopsy: If atypical or refractory, to confirm acanthosis, hyperkeratosis, and rule out malignancy (rare).
- Patch testing: For contact allergy.
- Systemic workup: Blood tests for diabetes, thyroid if generalised pruritus.
No single test defines LSC; it’s a pattern diagnosis.
Differential Diagnoses
Conditions mimicking vulvar LSC include:
| Condition | Key Features | Differentiator |
|---|---|---|
| Lichen sclerosus | Porcelain-white atrophic plaques, figure-of-8 pattern | Biopsy shows dermal sclerosis; high-potency steroids first-line |
| Lichen planus | Violaceous papules, Wickham striae, erosions | Biopsy; responds to high-potency steroids |
| Psoriasis | Well-defined plaques with silvery scale | Auspitz sign; multifocal |
| Candidiasis | White curdy discharge, satellite lesions | KOH prep positive |
| Vulvodynia | Burning pain without visible changes | Neuropathic; cotton-swab test |
| Contact dermatitis | Diffuse erythema, vesicles | Patch test; resolves with avoidance |
Accurate differentiation guides therapy.
Treatment
Treatment targets breaking the itch-scratch cycle, addressing triggers, and restoring skin barrier. Principles:
- Stop irritants: Use emollients (petroleum jelly, mineral oil), avoid soaps/pads.
- Topical corticosteroids: First-line medium-potency (e.g., triamcinolone 0.1%) twice daily until resolution (2-4 weeks), then taper. Escalate to potent (clobetasol 0.05%) if refractory, short-term.
- Infection control: Antifungals (fluconazole weekly for recurrent yeast), antibiotics as needed.
- Sedating antihistamines: Hydroxyzine or diphenhydramine at night for itch.
- Moisturisers/hormonal: Vaginal oestrogen for postmenopausal atrophy.
- Adjuncts: Calcineurin inhibitors (tacrolimus) for steroid-sparing; intralesional steroids for hypertrophic areas.
- Severe cases: Oral steroids, immunosuppressants, or psychotherapy.
Compliance is key; follow-up monitors response.
Outcome
With prompt treatment, most achieve symptom control and lesion regression. However, recurrence is common if triggers persist, requiring maintenance therapy (low-potency steroid/emollient). Long-term, skin may retain mild lichenification, but scarring is minimised. Patient education on itch hygiene prevents relapse. Prognosis improves with multidisciplinary care (dermatology, gynaecology, psychology).
Frequently Asked Questions (FAQs)
What causes lichen simplex of the vulva?
It stems from an itch-scratch cycle, often triggered by infections like candida, irritants, or atopy.
How is it diagnosed?
Clinically via history and exam; biopsy if needed to exclude mimics.
What is the best treatment?
Medium-potency topical steroids to break the cycle, plus irritant avoidance and emollients.
Can it be cured?
Not always curative, but manageable; recurrence prevented by addressing causes.
Does it lead to cancer?
No increased risk; monitor for changes.
References
- Common Benign Chronic Vulvar Disorders — American Academy of Family Physicians. 2020-11-01. https://www.aafp.org/pubs/afp/issues/2020/1101/p550.html
- Lichen Simplex Chronicus — Dallas Gynecology. 2023. https://dallas-obgyn.com/gynecology/lichen-simplex-chronicus/
- Lichen simplex of the vulva — DermNet NZ. 2024. https://dermnetnz.org/topics/lichen-simplex-of-the-vulva
- Vulvar lichen — Dexeus Midlife. 2023. https://www.dexeus.com/midlife/en/problema/vulvar-lichen/
- Vulvar Lichen Sclerosus et Atrophicus — National Center for Biotechnology Information (PMC). 2017-06-29. https://pmc.ncbi.nlm.nih.gov/articles/PMC5496281/
- Lichen Simplex Chronicus — Joy Women’s Health (PDF). 2021-08. https://joywomenshealth.com.au/wp-content/uploads/2021/08/lichen_simplex_chronicus.pdf
- Lichen Simplex Chronicus — Vulvovaginal Disorders. 2024. https://vulvovaginaldisorders.org/atlas_topic/lichen-simplex-chronicus/
Read full bio of Sneha Tete