Liver Disease: Signs, Symptoms, Causes & Treatment
Comprehensive guide to understanding liver disease: causes, symptoms, stages, and evidence-based treatment options.
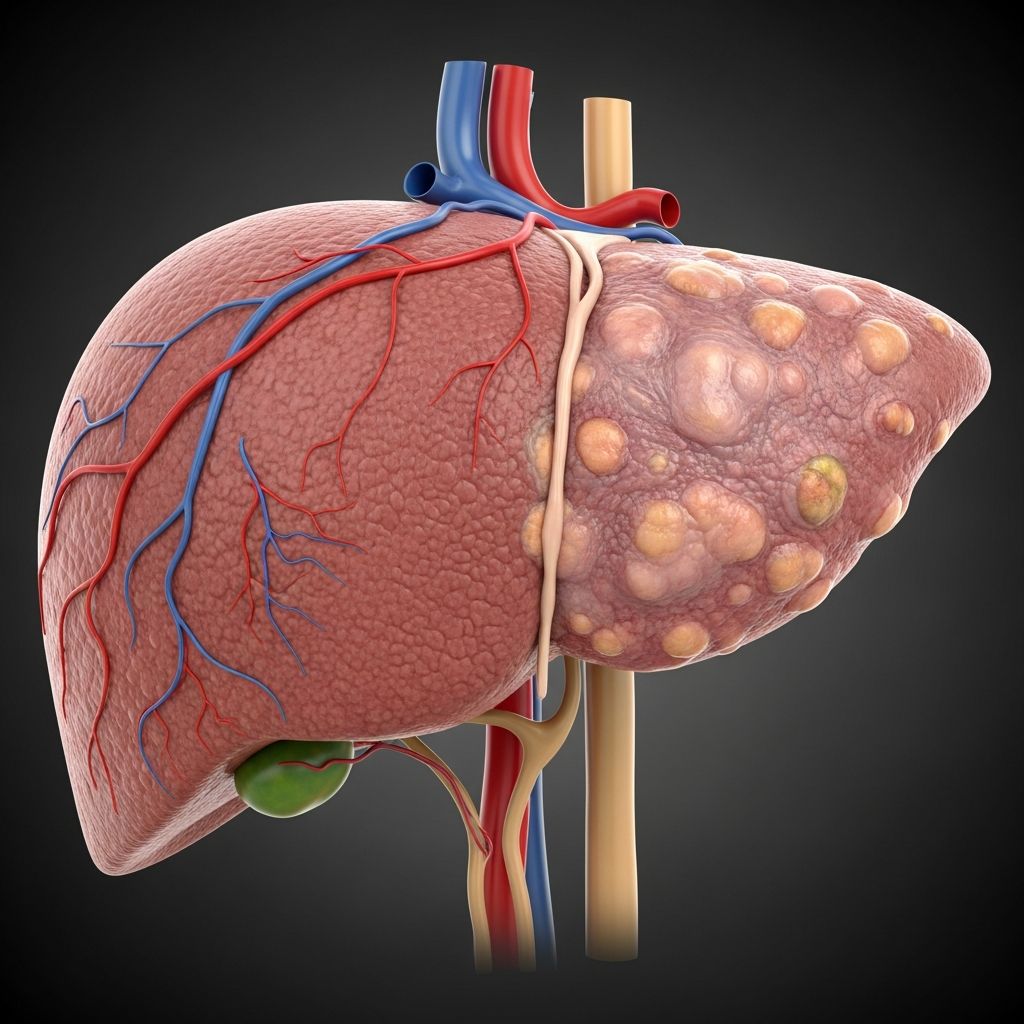
Understanding Liver Disease
The liver is one of your body’s most vital organs, performing over 500 essential functions including filtering blood, producing bile, storing vitamins, and regulating blood sugar levels. When liver disease develops, these critical functions become compromised, affecting your overall health and wellbeing. More than 100 types of liver disease have been identified, each with distinct characteristics and treatment approaches. The common thread among all liver diseases is damage to the liver tissue that disrupts its ability to function normally and maintain your body’s metabolic balance.
Liver disease can develop gradually over many years, often without noticeable symptoms in its early stages. This silent progression makes understanding the signs, causes, and available treatments essential for early detection and intervention. Whether caused by viral infections, alcohol consumption, genetic factors, or autoimmune conditions, liver disease requires comprehensive medical management and lifestyle modifications to prevent progression to more severe conditions like cirrhosis or liver failure.
Common Types of Liver Disease
Understanding the different types of liver disease helps identify your risk factors and appropriate treatment strategies. The most prevalent forms include:
Viral Hepatitis
Viral hepatitis represents inflammation of the liver caused by viral infection. Three primary forms exist: Hepatitis A, Hepatitis B, and Hepatitis C. Hepatitis A typically causes acute infection that resolves on its own, while Hepatitis B and C can develop into chronic infections requiring long-term management. These viral infections can be transmitted through contaminated food and water, blood exposure, or sexual contact, depending on the virus type. Without proper treatment, chronic viral hepatitis can progress to cirrhosis and liver cancer over time.
Fatty Liver Disease
Fatty liver disease occurs when excessive fat accumulates in liver cells, comprising more than five percent of the liver’s weight. This condition exists in two forms: non-alcoholic fatty liver disease (NAFLD) and alcoholic fatty liver disease (AFLD). Non-alcoholic fatty liver disease is increasingly common due to obesity, diabetes, and metabolic syndrome, while alcoholic fatty liver disease results from excessive alcohol consumption. Early-stage fatty liver disease is often reversible through weight loss, dietary changes, and lifestyle modifications.
Alcoholic Liver Disease
Chronic alcohol consumption directly damages liver cells, leading to inflammation, fatty accumulation, and scarring. Alcoholic liver disease progresses through stages of fatty liver, alcoholic hepatitis, and cirrhosis. Even moderate to heavy drinking can cause significant liver damage over time. The extent of damage depends on individual factors including genetics, nutritional status, and concurrent health conditions.
Autoimmune Liver Disease
Autoimmune liver diseases occur when the body’s immune system attacks liver cells, causing chronic inflammation and damage. These conditions include autoimmune hepatitis, primary biliary cholangitis, and primary sclerosing cholangitis. Autoimmune liver diseases typically require immunosuppressive medications to control the immune response and prevent progressive liver damage.
Genetic Liver Disease
Inherited genetic conditions affect liver function through various mechanisms. Hemochromatosis causes excessive iron accumulation in the liver, while Wilson’s disease leads to dangerous copper buildup. Other genetic conditions include alpha-1 antitrypsin deficiency and progressive familial intrahepatic cholestasis. Genetic liver diseases often require specialized treatment protocols targeting the underlying metabolic defect.
Recognizing Symptoms by Disease Stage
Early-Stage Liver Disease
Early-stage liver disease often produces no noticeable symptoms, which is why many people remain unaware they have the condition. When symptoms do appear in early stages, they are typically mild and nonspecific, including fatigue, weakness, abdominal discomfort, and mild digestive upset. Some individuals may notice slight nausea or loss of appetite. During this stage, liver enzymes may be elevated on blood tests despite minimal symptoms, making regular health screenings important for high-risk individuals.
Intermediate-Stage Liver Disease
As liver disease progresses, symptoms become more pronounced and noticeable. Patients often experience increased fatigue that interferes with daily activities, persistent abdominal pain or swelling, and changes in appetite. Digestive symptoms may include diarrhea or constipation. Weight loss or gain may occur, and some individuals develop swelling in the legs and feet due to fluid retention. Cognitive changes such as difficulty concentrating or mild confusion may develop as toxins accumulate in the bloodstream.
Late-Stage Liver Disease
Late-stage liver disease produces severe, debilitating symptoms requiring urgent medical attention. Jaundice develops as bile accumulates in the skin and eyes, causing yellow discoloration. Severe itching becomes difficult to manage and significantly impacts quality of life. Portal hypertension leads to variceal bleeding, presenting as vomiting blood or passing black tar-like stools. Hepatic encephalopathy causes notable brain impairment including confusion, memory problems, and personality changes. Fluid accumulation results in abdominal swelling (ascites) and leg edema. At this stage, liver failure becomes imminent without intervention, and liver transplantation may be necessary for survival.
Understanding Liver Disease Progression
Liver disease typically progresses through identifiable stages, each characterized by increasing tissue damage and functional decline. Understanding this progression helps explain why early intervention is crucial.
Stage 1: Inflammation
The liver becomes inflamed in response to harmful agents such as viruses, alcohol, or immune attacks. Inflammation is the body’s attempt to protect and heal itself, but chronic inflammation causes progressive damage. At this stage, liver function may still be relatively normal, and symptoms are often absent or minimal.
Stage 2: Fibrosis
Chronic inflammation triggers scar tissue formation within the liver. This fibrosis represents the liver’s attempt to repair itself, but excessive scarring impairs normal function. Blood flow through the liver becomes restricted, and the organ becomes stiffer and less flexible. Fibrosis is often reversible with appropriate treatment and lifestyle changes during this stage.
Stage 3: Cirrhosis
Extensive scarring severely damages liver structure and function, creating a permanent condition called cirrhosis. The liver becomes hardened and nodular, unable to perform its normal functions effectively. Cirrhosis causes portal hypertension, where blood pressure increases in the veins supplying the liver, leading to serious complications. Once established, cirrhosis is irreversible, though its progression can be slowed with treatment.
Stage 4: Liver Failure
End-stage liver disease or acute liver failure represents the most severe stage, where the liver can no longer support vital bodily functions. Liver failure can develop acutely over days to weeks or chronically over years. Acute liver failure is a medical emergency requiring immediate hospitalization and intensive care. Chronic liver failure may progress more gradually but ultimately proves fatal without intervention such as liver transplantation.
Diagnostic Tests for Liver Disease
Accurate diagnosis of liver disease requires comprehensive testing to identify the type, severity, and stage of disease. Multiple diagnostic approaches are employed to build a complete clinical picture.
Blood Tests
Liver function tests measure specific enzymes and proteins that indicate liver health. Alanine aminotransferase (ALT) and aspartate transaminase (AST) are liver enzymes that leak into the bloodstream when liver cells are damaged. Alkaline phosphatase and bilirubin levels indicate bile flow and liver’s ability to process waste products. Albumin and prothrombin time (PT/INR) reflect the liver’s synthetic function and ability to produce essential proteins. These tests establish baseline liver function and help monitor disease progression and treatment response.
Hepatitis Serologies
For suspected viral hepatitis, specific serological tests identify the virus type and infection status. Hepatitis A testing distinguishes acute from resolved infection. Hepatitis B testing includes surface antigen, core antibody, and surface antibody to determine infection status and immunity. Hepatitis C testing uses enzyme immunoassay followed by RNA PCR to confirm active infection and determine viral load. Genotyping identifies the hepatitis C genotype, which guides treatment selection and predicts treatment response.
Imaging Studies
Ultrasound, computed tomography (CT), and magnetic resonance imaging (MRI) visualize liver structure and detect abnormalities such as fatty infiltration, cirrhosis, tumors, or portal hypertension. These imaging modalities help stage liver disease and screen for hepatocellular carcinoma in high-risk patients. Elastography measures liver stiffness, providing a noninvasive assessment of fibrosis severity.
Liver Biopsy
In selected cases, liver biopsy provides definitive assessment of liver tissue damage, inflammation severity, and fibrosis stage. A small tissue sample is obtained through needle aspiration under ultrasound guidance. Histopathology examination reveals the degree of inflammation, necrosis, and scarring present. Biopsy remains the gold standard for assessing liver disease severity, though noninvasive alternatives are increasingly used.
Specialized Testing
For suspected genetic liver diseases like Wilson’s disease, specialized testing includes serum ceruloplasmin levels, 24-hour urinary copper measurement, and slit lamp examination to detect Kayser-Fleischer rings in the cornea. Genetic testing confirms specific mutations in conditions with known genetic basis. Autoimmune markers such as antinuclear antibody (ANA) and anti-smooth muscle antibody help diagnose autoimmune hepatitis.
Treatment Approaches for Liver Disease
Lifestyle Modifications
Lifestyle changes form the foundation of liver disease management and can significantly slow or even reverse disease progression, particularly in early stages. Alcohol cessation is absolutely critical for all types of liver disease, as continued alcohol consumption accelerates disease progression regardless of other treatments. Weight loss through balanced nutrition and regular exercise helps reverse fatty liver disease and improves overall metabolic health. Dietary modifications including reduced sodium intake manage fluid retention and portal hypertension complications. Vaccination against hepatitis A and B prevents additional viral infections in susceptible patients.
Medications
Pharmacological treatment varies based on liver disease type and severity. Antiviral medications such as pegylated interferon and ribavirin treat chronic hepatitis C, while newer direct-acting antiviral agents offer improved efficacy and tolerability. Immunosuppressive agents control autoimmune liver diseases. Diuretics manage fluid accumulation and ascites. Medications addressing underlying conditions such as diabetes or hyperlipidemia reduce metabolic strain on the liver. Corticosteroids may be used for severe autoimmune hepatitis or alcoholic hepatitis.
Monitoring and Follow-up
Regular monitoring through blood tests, imaging studies, and clinical assessment tracks disease progression and treatment response. Patients with cirrhosis require periodic screening for hepatocellular carcinoma through ultrasound and alpha-fetoprotein measurement. Endoscopic screening identifies esophageal varices requiring prevention strategies. Regular specialist appointments ensure timely adjustment of treatments and early detection of complications.
Liver Transplantation
Liver transplantation offers curative treatment for end-stage liver disease, acute liver failure, and certain liver cancers. Transplantation successfully cures many genetic liver diseases and prevents death from liver failure. The transplantation process includes comprehensive evaluation, surgery, and lifelong immunosuppressive therapy to prevent organ rejection. Outcomes have dramatically improved with modern surgical techniques and immunosuppressive protocols, with five-year survival rates exceeding 80% in many centers.
Frequently Asked Questions
Q: Can liver disease be reversed?
A: Early-stage liver disease, particularly fatty liver disease and mild fibrosis, can often be reversed or significantly improved through aggressive lifestyle modifications, treatment of underlying causes, and medical therapies. However, cirrhosis is generally irreversible, though progression can be slowed with appropriate management.
Q: How often should I be screened for liver disease?
A: Screening frequency depends on individual risk factors. Those with family history of liver disease, chronic hepatitis, cirrhosis, or hepatocellular carcinoma risk should undergo regular screening. Your healthcare provider will recommend appropriate screening intervals based on your specific situation.
Q: Is liver disease always symptomatic?
A: No. Early-stage liver disease is often asymptomatic, with no noticeable symptoms despite ongoing tissue damage. This is why screening is important for high-risk individuals, as early detection and treatment can prevent serious complications.
Q: Can I live normally with liver disease?
A: Many people with early-stage liver disease maintain normal activities with appropriate treatment and lifestyle modifications. Those with compensated cirrhosis may also function well. However, decompensated cirrhosis and liver failure significantly impact quality of life and require intensive management.
Q: What dietary changes help liver disease?
A: Recommended dietary changes include reducing sodium to manage fluid retention, limiting alcohol completely, eating balanced nutrition with adequate protein, maintaining healthy weight, and avoiding raw shellfish and undercooked foods. Your healthcare provider may recommend specific dietary guidelines based on your disease type and severity.
Q: How is liver transplant success measured?
A: Liver transplant success is typically measured by patient survival rates and graft survival (how long the transplanted liver functions). Modern immunosuppressive protocols have achieved five-year survival rates exceeding 80% in many centers, with many transplant recipients living 15-20 years or longer with their new liver.
When to Seek Medical Attention
Prompt medical attention is essential if you develop symptoms suggestive of liver disease or have known risk factors. Seek immediate emergency care if you experience vomiting blood, passing black or tarry stools, severe abdominal pain, confusion, or loss of consciousness. These symptoms indicate serious complications requiring urgent intervention. Schedule an appointment with your healthcare provider if you experience persistent fatigue, jaundice, abdominal swelling, or other symptoms concerning for liver disease. Early diagnosis and treatment significantly improve outcomes and prevent disease progression to life-threatening stages.
Conclusion
Liver disease encompasses numerous conditions affecting this vital organ’s ability to function properly. Understanding the types, symptoms, stages, and available treatments empowers you to make informed decisions about your health. Early detection through appropriate screening and prompt treatment can prevent disease progression and serious complications. While advanced liver disease poses significant challenges, modern medical management and innovative treatments offer hope for improved outcomes. Working closely with experienced liver specialists ensures personalized treatment plans addressing your specific condition and health goals. Making lifestyle modifications, adhering to prescribed treatments, and maintaining regular medical follow-up significantly influence your long-term prognosis and quality of life with liver disease.
References
- Understanding Liver Disease — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/17179-liver-disease
- Common Tests for Liver Disease — Cleveland Clinic. 2024. https://my.clevelandclinic.org/departments/digestive/medical-professionals/hepatology/liver-tests
- Treatment for Liver Disease — Cleveland Clinic. 2024. https://my.clevelandclinic.org/departments/digestive/depts/liver-disease
- Get Treatment for Liver Diseases — Cleveland Clinic. 2024. https://my.clevelandclinic.org/services/liver-disease-treatment
- A guide to managing acute liver failure — Cleveland Clinical Journal of Medicine. 2014. https://www.ccjm.org/content/83/6/453
- Understanding Liver Disease Brochure — Cleveland Clinic Digestive Disease Institute. 2024. https://my.clevelandclinic.org/-/scassets/files/org/digestive/ddc_liver_brochure.pdf
Read full bio of medha deb











