Lung Cancer Causes: 7 Major Risk Factors And Prevention Tips
Unraveling the primary causes and risk factors of lung cancer, from smoking to environmental exposures.
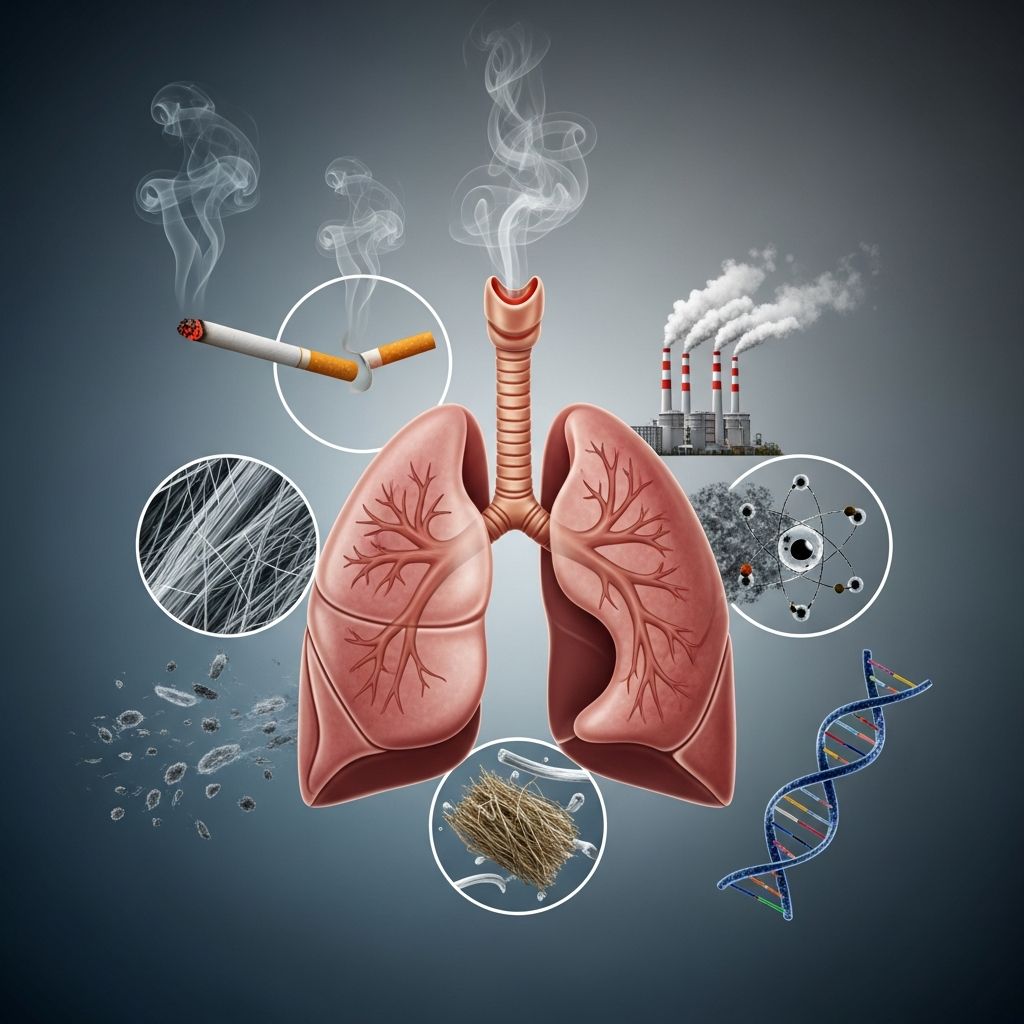
Lung Cancer Causes
Lung cancer typically develops when lung cells acquire DNA mutations that cause them to grow uncontrollably and form tumors. While the precise triggers vary, cigarette smoking remains the predominant cause, accounting for 80-90% of cases in the United States. Other factors like radon gas, secondhand smoke, and occupational exposures significantly contribute to risk.
What Is Lung Cancer?
Lung cancer originates in the lungs, two spongy organs responsible for oxygen exchange during breathing. It arises from uncontrolled growth of abnormal cells that can form tumors, invade nearby tissues, and metastasize to distant sites via blood or lymph systems. There are two primary types: non-small cell lung cancer (NSCLC), which comprises about 80-85% of cases and grows more slowly, and small cell lung cancer (SCLC), which is aggressive and strongly linked to smoking.
Globally, lung cancer is the leading cause of cancer deaths, claiming more lives than breast, prostate, and colorectal cancers combined. In 2026, projections indicate over 2.4 million new cases worldwide, with smoking as the top attributable factor. Even non-smokers face risks from environmental and genetic influences.
How Does Lung Cancer Develop?
Lung cancer begins with genetic changes in lung cells’ DNA, disrupting normal growth, division, and death cycles. Healthy cells follow DNA instructions to multiply at a regulated rate and self-destruct (apoptosis) when damaged. Cancer cells ignore these signals, proliferating rapidly and forming masses that impair lung function.
Carcinogens, such as those in tobacco smoke, damage lung lining cells immediately upon inhalation. Initial repairs may occur, but repeated exposure leads to cumulative mutations. Over time, these alterations enable cells to evade natural safeguards, potentially progressing to invasive cancer. Tumors can remain localized initially but often spread, complicating treatment.
Smoking and Lung Cancer
Cigarette smoking is the number one risk factor for lung cancer, linked to 80-90% of deaths in the U.S. Tobacco smoke contains over 7,000 chemicals, including at least 70 known carcinogens like benzene, formaldehyde, and polycyclic aromatic hydrocarbons. The risk escalates with pack-years (packs per day multiplied by years smoked); for instance, heavy smokers face up to 30 times higher odds than non-smokers.
Even non-cigarette tobacco products like cigars and pipes increase risk due to similar toxic profiles. Quitting at any age substantially reduces chances, with benefits accruing over time—former smokers who quit 10-15 years prior see risks approach those of never-smokers. Vaping introduces potential carcinogens like heavy metals and flavoring chemicals, though long-term data is emerging; experts caution against it, especially for youth.
Secondhand Smoke Exposure
Secondhand smoke, inhaled passively from others’ tobacco use, elevates lung cancer risk by 20-30% in non-smokers. It contains the same carcinogens as firsthand smoke, damaging lung tissues through sidestream (from burning tobacco) and mainstream (exhaled) emissions. Children and workplace exposure pose particular vulnerabilities, underscoring the need for smoke-free environments.
Radon Gas
Radon, a colorless, odorless radioactive gas from uranium decay in soil, rock, and water, is the second leading cause of U.S. lung cancer, responsible for about 21,000 deaths annually. It seeps into homes via foundations, accumulating to hazardous levels. The EPA estimates 1 in 15 homes exceeds safe limits; smokers exposed to radon face synergistically higher risks—up to 10 times that of non-smokers.
Testing homes with affordable kits and mitigation via ventilation systems can prevent exposure. Radon daughters emit alpha particles that irradiate lung cells, causing DNA damage akin to radiation therapy effects.
Occupational and Environmental Exposures
Workplace carcinogens account for 5-15% of lung cancers, per historical estimates updated for multifactorial etiology. Key agents include:
- Asbestos: Fibrous mineral used in insulation; synergizes with smoking to multiply risk 50-fold.
- Arsenic, Chromium, Nickel: Found in mining, metalworking; inhaled particulates damage DNA.
- Diesel Exhaust and Silica: Common in construction, trucking; linked to dose-dependent risk increases.
Air pollution, particularly fine particulates (PM2.5) from vehicles and industry, raises risk modestly but population-wide. Ionizing radiation (X-rays, gamma rays) from medical procedures or occupational sources like nuclear work contributes via DNA breaks and oxidative stress; alpha particles from radon exemplify this.
Radiation Therapy
Chest radiation for prior cancers (e.g., breast, Hodgkin’s lymphoma) heightens lung cancer risk by 5-10 years post-treatment, as ionizing rays induce mutations in lung tissues. Risk persists lifelong, amplified by smoking. Modern techniques minimize exposure, but survivors require vigilant screening.
Genetics and Family History
A personal or family history of lung cancer elevates risk, potentially due to shared genetics, smoking habits, or environments. Inherited mutations in genes like EGFR or TP53 predispose cells to carcinogen-induced changes, explaining 8-15% of never-smoker cases. Survivors face recurrence risks, emphasizing genetic counseling.
Diet and Other Factors
Dietary influences are under study; beta-carotene supplements increase risk in smokers, while fruits/vegetables may protect via antioxidants. Arsenic in well water correlates with elevated incidence. Obesity and chronic lung diseases like COPD indirectly heighten vulnerability by impairing repair mechanisms.
Prevention Strategies
Key to curbing lung cancer:
- Quit Smoking: Access cessation programs; risk drops immediately.
- Test for Radon: Mitigate high levels promptly.
- Avoid Carcinogens: Use PPE at work; support clean air policies.
- Screening: Low-dose CT for high-risk individuals (ages 50-80, 20+ pack-years).
| Risk Factor | Attributable Risk (% U.S. Deaths) | Prevention Tip |
|---|---|---|
| Smoking | 80-90% | Quit via nicotine replacement, counseling |
| Radon | ~10-15% | Home testing and ventilation |
| Secondhand Smoke | ~3-5% | Smoke-free zones |
| Occupational | 5-15% | Exposure controls, PPE |
Frequently Asked Questions (FAQs)
Can lung cancer occur in non-smokers?
Yes, about 10-20% of cases occur in never-smokers, often due to radon, secondhand smoke, or genetics.
How long after quitting smoking does risk decrease?
Risk halves after 10 years and approaches non-smoker levels after 15-20 years.
Is vaping safe for lungs?
No, vaping exposes users to carcinogens; long-term risks mirror smoking.
How can I test my home for radon?
Use EPA-approved kits; retest every 2 years or post-renovation.
Does family history guarantee lung cancer?
No, but it doubles risk; screening and lifestyle matter.
References
- Lung cancer – Symptoms and causes — Mayo Clinic. 2023-10-05. https://www.mayoclinic.org/diseases-conditions/lung-cancer/symptoms-causes/syc-20374620
- Lung Cancer Risk Factors — Centers for Disease Control and Prevention (CDC). 2024-01-15. https://www.cdc.gov/lung-cancer/risk-factors/index.html
- Lung Cancer: Types, Stages, Symptoms, Diagnosis & Treatment — Cleveland Clinic. 2024-05-20. https://my.clevelandclinic.org/health/diseases/4375-lung-cancer
- Occupational and Environmental Causes of Lung Cancer — National Center for Biotechnology Information (PMC). 2013-10-01. https://pmc.ncbi.nlm.nih.gov/articles/PMC3875302/
Read full bio of medha deb











