Myasthenia Gravis: Causes, Symptoms & Treatment
Understanding myasthenia gravis: autoimmune muscle weakness that worsens with activity and improves with rest.
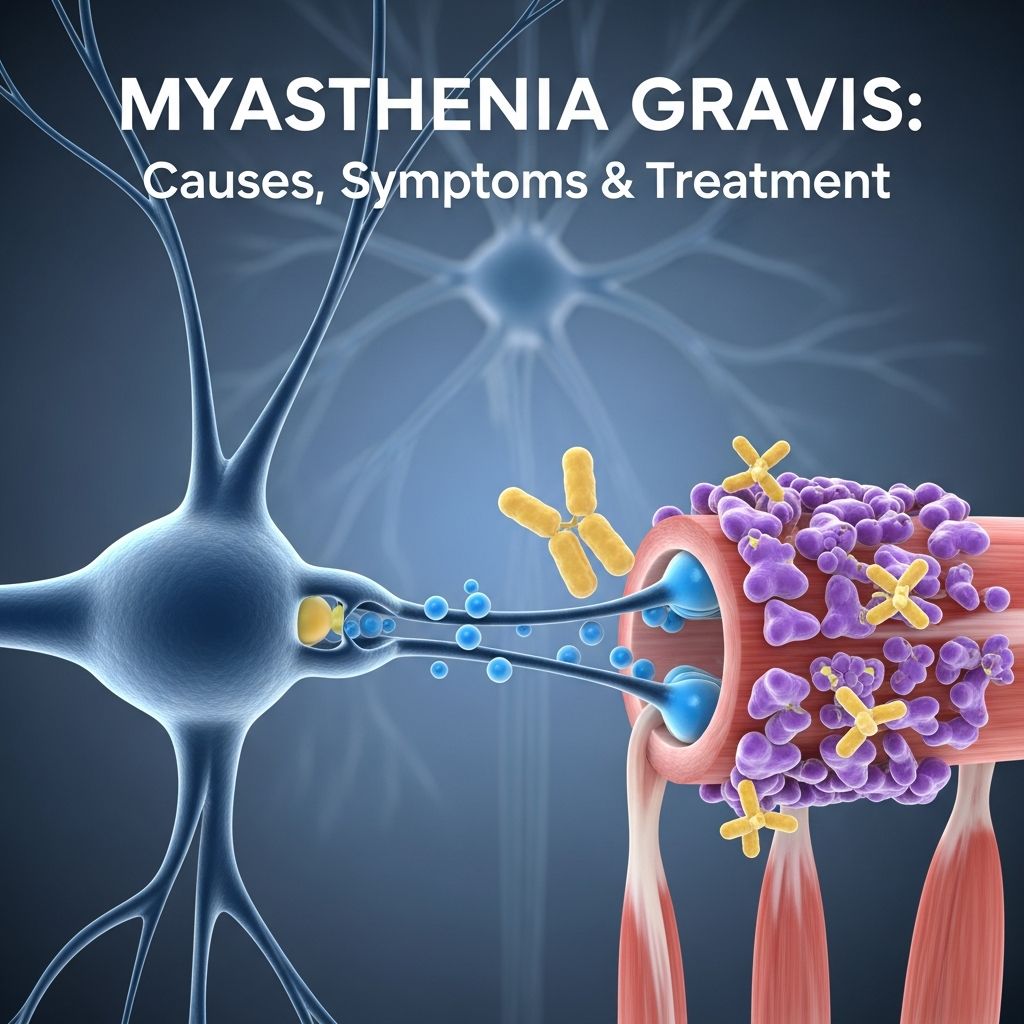
What is Myasthenia Gravis?
Myasthenia gravis (MG) is a chronic autoimmune neuromuscular disorder characterized by skeletal muscle weakness that typically worsens with activity and improves with rest. This condition occurs when the immune system attacks the neuromuscular junction, the point where nerve signals transmit to muscles, disrupting normal muscle contraction. Unlike other muscle diseases, myasthenia gravis does not cause permanent muscle damage, though symptoms can significantly impact daily functioning and quality of life.
The disease has an estimated prevalence of less than 1 per 10,000 individuals, making it a relatively rare condition. However, when properly diagnosed and managed, most patients experience significant improvement in symptoms and can maintain active, productive lives. Understanding this condition is essential for patients, caregivers, and healthcare providers to ensure timely diagnosis and appropriate treatment.
Causes and Risk Factors
Myasthenia gravis is fundamentally an autoimmune disease where the body’s immune system mistakenly attacks acetylcholine receptors or related proteins at the neuromuscular junction. These receptors normally receive chemical signals from nerve endings to trigger muscle contraction. When the immune system damages these receptors, the transmission of signals between nerves and muscles becomes impaired, resulting in muscle weakness and fatigue.
While the exact cause of why the immune system begins attacking neuromuscular junctions remains unclear, researchers have identified several contributing factors. Genetic predisposition plays a role, as the condition sometimes runs in families. Additionally, certain environmental triggers, infections, or other autoimmune conditions may precipitate the development of myasthenia gravis in susceptible individuals. The condition can develop at any age, though it shows a bimodal distribution with peaks in the third and eighth decades of life.
Symptoms of Myasthenia Gravis
Myasthenia gravis symptoms often develop gradually and can be easily mistaken for signs of other health conditions, making early recognition challenging. The hallmark characteristic is muscle weakness that worsens with activity and improves with rest. Symptoms vary significantly among patients depending on which muscles are affected and the severity of the condition.
Common Symptoms Include:
- Weakness in the arms and legs
- Excessive fatigue and tiredness
- Drooping eyelids (ptosis)
- Double vision (diplopia)
- Slurred or nasal speech
- Difficulty swallowing and chewing
- Shortness of breath or respiratory weakness
- Facial weakness affecting smiling or frowning
Symptoms often fluctuate throughout the day, typically worsening toward evening and improving after rest. Physical exertion, stress, illness, or certain medications can trigger or exacerbate symptoms. Some patients experience myasthenic crisis, a life-threatening condition where respiratory muscles become severely weakened, requiring immediate medical intervention and hospitalization.
Diagnosis of Myasthenia Gravis
Diagnosing myasthenia gravis requires a comprehensive approach combining detailed clinical history, physical examination, and specialized diagnostic testing. Because symptoms can mimic other neurological conditions, working with healthcare providers familiar with myasthenia gravis is crucial for accurate and timely diagnosis.
Initial Evaluation
The diagnostic process begins with a thorough medical history where healthcare providers ask about symptom onset, duration, triggers, and progression. A detailed physical examination focuses on identifying muscle weakness patterns, particularly in the ocular and bulbar muscles. Neurologists perform specific tests, such as evaluating eye closure strength and observing for fatigue with sustained muscle use.
Diagnostic Tests
Several specialized tests help confirm a myasthenia gravis diagnosis:
Blood Tests: These measure the presence of acetylcholine receptor antibodies and muscle-specific kinase (MuSK) antibodies. Approximately 85% of patients with generalized MG and 50% with ocular MG test positive for acetylcholine receptor antibodies.
Edrophonium (Tensilon) Test: This test involves administering a short-acting anticholinesterase medication intravenously to observe whether symptoms temporarily improve, suggesting a neuromuscular junction disorder.
Ice Pack Test: A simple, non-invasive test where applying ice to affected muscles temporarily relieves symptoms in myasthenia gravis patients, providing diagnostic support.
Electromyography (EMG): This nerve conduction study measures electrical activity in muscles and can show the characteristic pattern of decreased muscle response with repeated stimulation.
Repetitive Nerve Stimulation (RNS): This test stimulates nerves repeatedly to demonstrate the decremental response typical in myasthenia gravis, showing progressive weakening of muscle response.
Single Fiber Electromyography (SFEMG): The most sensitive diagnostic test, capable of detecting neuromuscular junction dysfunction even when other tests are negative. This specialized test measures “jitter,” the variability in time intervals between action potentials of muscle fiber pairs.
Imaging Studies: Computed tomography (CT) scans and magnetic resonance imaging (MRI) of the chest help identify thymoma or thymic abnormalities, as approximately 10-15% of myasthenia gravis patients have thymic tumors.
Treatment Options for Myasthenia Gravis
Treatment approaches for myasthenia gravis are highly individualized, depending on disease severity, symptom distribution, patient age, overall health status, and response to initial therapy. When diagnosed promptly, most patients improve significantly with appropriate treatment. The goal is to achieve complete remission or minimal symptomatic manifestation, allowing patients to resume normal activities.
Medications
Cholinesterase Inhibitors: Pyridostigmine (Mestinon) is typically the first-line medication, working by increasing acetylcholine levels at the neuromuscular junction. This medication often provides symptomatic relief but does not alter disease progression.
Corticosteroids: Medications like prednisone suppress the immune system and reduce antibody production. While effective, long-term corticosteroid use requires careful monitoring due to potential side effects.
Immunosuppressants: Medications including azathioprine, mycophenolate mofetil, cyclosporine, methotrexate, and tacrolimus reduce immune system activity and are often used as steroid-sparing agents or for patients who don’t respond adequately to cholinesterase inhibitors alone.
Immunological Therapies
Intravenous Immunoglobulin (IVIG): This therapy provides healthy antibodies from donor blood administered through a vein, helping modulate immune responses. Benefits typically last several weeks.
Subcutaneous Immunoglobulin (SCIG): A newer alternative to IVIG where immunoglobulin is injected through the skin, absorbing more slowly and allowing for home administration.
Plasmapheresis (Plasma Exchange): This procedure removes antibodies from the bloodstream, providing temporary symptom relief typically lasting 4-6 weeks. It’s particularly useful during myasthenic crisis or as a bridge therapy while waiting for longer-acting treatments to take effect.
Monoclonal Antibodies: Rituximab, which targets B cells producing antibodies, and eculizumab, a complement inhibitor, represent newer therapeutic options for patients with inadequate response to conventional treatments.
Surgical Treatment
Thymectomy, surgical removal of the thymus gland, is recommended for patients with thymoma and can benefit those without thymoma, particularly younger patients with generalized myasthenia gravis. Approximately 30-40% of patients achieve remission following thymectomy, with additional patients experiencing significant symptom reduction.
Managing Myasthenia Gravis
Beyond medical treatment, several strategies help patients manage their condition effectively:
- Pacing activities to avoid excessive fatigue
- Taking frequent rest breaks during physically demanding tasks
- Scheduling important activities when energy levels are highest
- Using adaptive equipment for eating, writing, or other activities
- Applying eye patches or using prism glasses for double vision
- Avoiding known triggers such as heat, stress, or infections
- Maintaining regular communication with healthcare providers
- Participating in rehabilitation therapy for optimal function
When First-Line Treatments Don’t Work
For the 5-20% of patients with generalized myasthenia gravis who don’t respond adequately to initial therapies like pyridostigmine and corticosteroids, alternative treatment strategies become necessary. These patients benefit from early escalation to combination immunosuppressive therapy or newer biologic agents. Close collaboration between neuromuscular specialists and other experts ensures appropriate treatment selection based on individual patient characteristics and disease presentation.
Specialized Care at Leading Centers
Receiving care from specialized myasthenia gravis programs offers significant advantages. Multidisciplinary teams including neuromuscular specialists, neuro-ophthalmologists, thoracic surgeons, and rehabilitation specialists provide comprehensive evaluation and personalized treatment plans. These centers maintain expertise in diagnosing complex cases, managing treatment-resistant disease, and providing access to cutting-edge therapeutic options including clinical trial participation.
Frequently Asked Questions
Q: Is myasthenia gravis hereditary?
A: While myasthenia gravis is not strictly hereditary, genetic factors increase susceptibility. Approximately 5% of patients have a family history of the condition. Identical twins show higher concordance rates than the general population, suggesting genetic contribution. Environmental triggers likely play an important role in disease development.
Q: Can myasthenia gravis be cured?
A: While not traditionally “cured,” myasthenia gravis can be managed effectively with appropriate treatment. Many patients achieve complete remission or minimal symptoms with therapy. Thymectomy offers potential for long-term remission in some patients, particularly younger individuals with generalized disease.
Q: How does pregnancy affect myasthenia gravis?
A: Pregnancy effects vary among patients. Some experience improvement, others notice worsening symptoms, and many remain stable. Careful monitoring and coordination between obstetric and neuromuscular specialists is essential. Most medications used for myasthenia gravis are considered safe during pregnancy.
Q: What is myasthenic crisis?
A: Myasthenic crisis is a life-threatening condition where respiratory muscles become severely weakened, potentially requiring mechanical ventilation. It can be triggered by infections, medication changes, surgery, or stress. This medical emergency requires immediate hospitalization and intensive care management.
Q: Can myasthenia gravis cause permanent muscle damage?
A: Myasthenia gravis itself does not cause permanent muscle damage or degeneration. The underlying muscle tissue remains normal. With appropriate treatment, muscle strength can be fully restored, distinguishing it from progressive neuromuscular degenerative diseases.
Q: Are there lifestyle modifications that help manage symptoms?
A: Yes, several lifestyle adjustments help manage myasthenia gravis. These include pacing activities, avoiding heat exposure, minimizing stress, preventing infections through vaccinations, maintaining regular sleep schedules, and working closely with rehabilitation specialists to optimize functional abilities.
References
- Myasthenia Gravis Program – Cleveland Clinic — Cleveland Clinic. Accessed December 1, 2025. https://my.clevelandclinic.org/departments/neurological/depts/neuromuscular/myasthenia-gravis-program
- Get Myasthenia Gravis Treatment | Cleveland Clinic — Cleveland Clinic. Accessed December 1, 2025. https://my.clevelandclinic.org/services/myasthenia-gravis-treatment
- Myasthenia gravis: An update for internists — Cleveland Clinic Journal of Medicine. 2021. https://www.ccjm.org/content/90/2/72
- Myasthenia gravis: Frequently asked questions — Cleveland Clinic Journal of Medicine. 2021. https://www.ccjm.org/content/90/2/103
- What to Do if First-Line Myasthenia Gravis Treatments Fail? — Cleveland Clinic Consult QD. Accessed December 1, 2025. https://consultqd.clevelandclinic.org/what-are-the-treatment-options-for-myasthenia-gravis-if-first-line-agents-fail
- Myasthenia gravis: Frequently asked questions — PubMed. 2023. https://pubmed.ncbi.nlm.nih.gov/36724914/
- Myasthenia Gravis: What It Is, Causes, Symptoms & Treatment — Cleveland Clinic. Accessed December 1, 2025. https://my.clevelandclinic.org/health/diseases/17252-myasthenia-gravis-mg
Read full bio of Sneha Tete











