Myelodysplastic Syndrome: Symptoms, Diagnosis & Treatment
Understanding MDS: A comprehensive guide to symptoms, diagnosis, and modern treatment options.
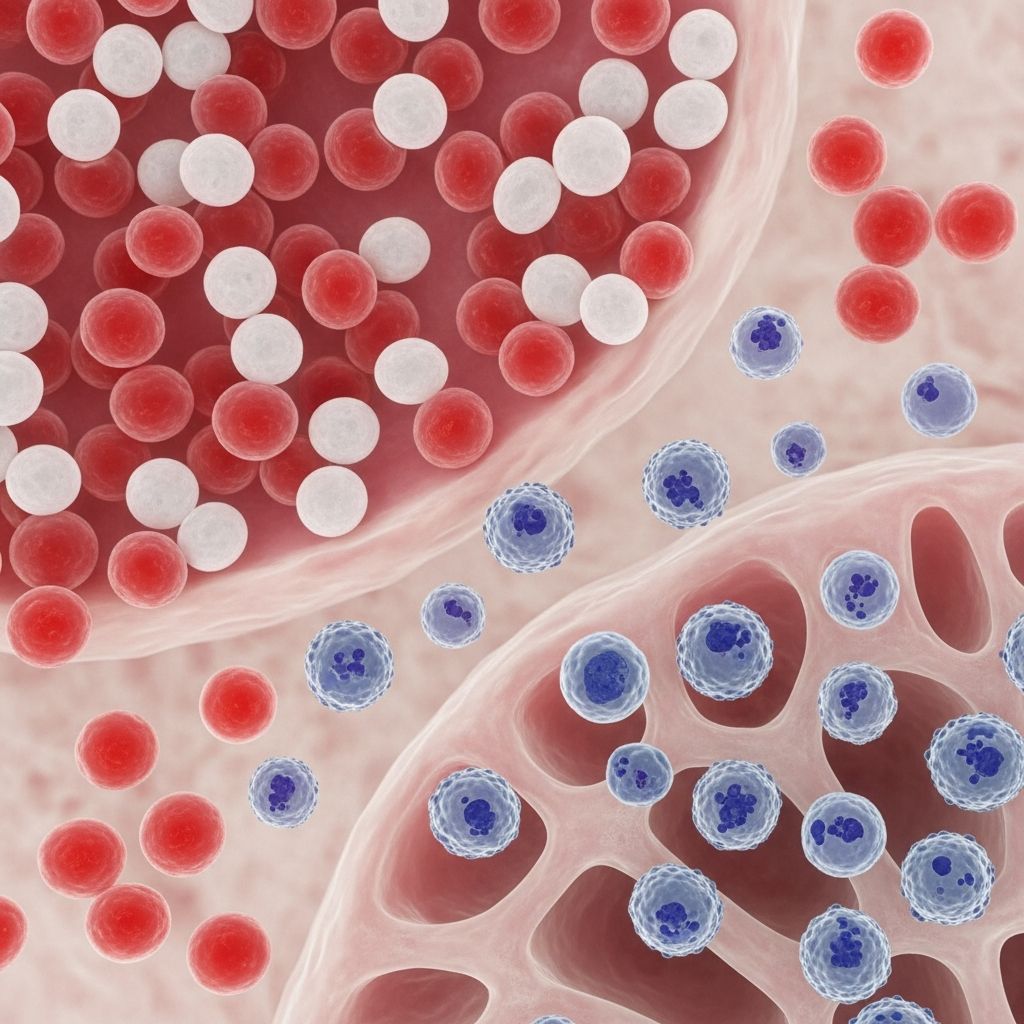
Myelodysplastic Syndrome: Understanding a Complex Blood Disorder
Myelodysplastic syndrome, commonly known as MDS or myelodysplasia, is a group of clonal bone marrow disorders that impair the production of healthy blood cells. Unlike healthy bone marrow that produces adequate quantities of functional blood cells, MDS disrupts this process, leading to cytopenias—a deficiency of one or more types of blood cells. This condition affects stem cells in the bone marrow and can progress to acute myeloid leukemia (AML) in some patients. MDS is now recognized as the most common myeloid malignancy in the United States, predominantly affecting older adults. The heterogeneous nature of MDS means that patients can present with widely varying disease severity and prognosis, requiring individualized diagnostic approaches and treatment strategies.
What Is Myelodysplastic Syndrome?
Myelodysplastic syndrome represents a spectrum of bone marrow disorders characterized by abnormal development and maturation of blood cells. In MDS, the bone marrow produces blood cells ineffectively, resulting in insufficient quantities of red blood cells, white blood cells, or platelets—or combinations thereof. This underproduction occurs despite the bone marrow often appearing hypercellular (containing numerous cells) on microscopic examination. The fundamental problem lies in the quality and function of the cells produced rather than simply their quantity.
MDS is classified as a clonal disorder, meaning it arises from a single abnormal cell that continues to divide and perpetuate the disease. The condition occupies a middle ground between normal bone marrow function and acute leukemia. While some patients with lower-risk MDS experience stable disease for years, others progress rapidly to acute myeloid leukemia. This variable progression pattern underscores the importance of accurate risk stratification at the time of diagnosis.
Common Symptoms and Clinical Presentations
The symptoms of myelodysplastic syndrome vary depending on which blood cell types are affected and the severity of the deficiency. Many patients are discovered to have MDS during routine blood work ordered for other reasons, as primary care physicians and geriatricians are often the first to recognize abnormal blood counts.
Anemia-Related Symptoms
When red blood cells are affected—the most common presentation—patients typically experience symptoms associated with anemia. These include:
- Fatigue and weakness
- Shortness of breath, particularly with exertion
- Pallor (pale skin)
- Pale conjunctiva (the membrane covering the whites of the eyes)
- Tachycardia (increased heart rate)
- Dizziness or lightheadedness
- Headaches
- Reduced exercise tolerance
Infection and Immunity Issues
When white blood cells are affected, patients have increased susceptibility to infections due to neutropenia (abnormally low neutrophil counts). Recurrent infections, fever, or infections that are slow to resolve may indicate white blood cell deficiency.
Bleeding and Clotting Problems
Platelet deficiency leads to thrombocytopenia, which can cause unusual bruising, bleeding gums, blood in stool or urine, or prolonged bleeding from minor cuts.
Understanding Risk Stratification
Unlike many cancers that are “staged,” myelodysplastic syndromes are classified using prognostic systems that predict the risk of transformation to acute myeloid leukemia and overall survival. These classifications guide treatment decisions and help establish realistic expectations for patients and their families.
Lower-Risk MDS
Patients with lower-risk MDS typically have a median survival of 3 to 7 years. These patients often benefit from supportive care and monitoring strategies. Lower-risk disease may progress slowly or remain stable for extended periods. Treatment in these cases is often conservative, focusing on maintaining quality of life and managing symptoms.
Higher-Risk MDS
Higher-risk MDS is pathobiologically similar to acute myeloid leukemia in older adults. Approximately 25% of newly diagnosed MDS patients and 15% to 20% of those with established disease have higher-risk disease. These patients typically develop acute myeloid leukemia or die of complications within an average of 1.5 years, making prompt intervention critical. Higher-risk patients should almost always be followed by a hematologist or medical oncologist, with therapy initiated immediately regardless of blood counts.
Factors Influencing Prognosis
Several factors are considered when determining prognosis:
- The number of myeloblasts (immature cells) in the bone marrow
- The degree and number of cytopenias
- Cytogenetic abnormalities (acquired genetic mutations), found in approximately half of MDS patients
- Specific molecular mutations
- Patient age and overall health status
- Comorbidities such as coronary artery disease, COPD, or chronic kidney disease
Diagnostic Approaches
Accurate diagnosis of myelodysplastic syndrome requires a comprehensive evaluation combining clinical history, physical examination, and specialized testing. Primary care providers often initiate the diagnostic workup by recognizing cytopenia on routine blood tests.
Complete Blood Count (CBC)
The initial diagnostic step involves a complete blood count, which reveals the number and types of blood cells present in the peripheral blood. Multilineage cytopenia—low counts across multiple cell lines—almost always suggests MDS or a related disorder.
Bone Marrow Aspiration and Biopsy
The bone marrow aspiration and biopsy are central to MDS diagnosis. These procedures evaluate the morphology of bone marrow cells and determine the cytogenetic profile. The bone marrow biopsy provides crucial information about cell architecture and allows assessment of fibrosis (scarring) within the marrow. Specific characteristics of peripheral blood and bone marrow findings distinguish MDS from other disorders and help classify the disease according to established criteria.
Cytogenetic and Molecular Testing
Cytogenetic analysis identifies acquired genetic abnormalities in the neoplastic clone. Additional specialized tests may include assessment of antiplatelet antibodies, protein electrophoresis, and fluorescence in situ hybridization to evaluate for specific clonal disorders. Mutation testing is increasingly being incorporated into diagnostic algorithms to help identify earlier disease entities and predict whether MDS will behave as lower-risk or higher-risk disease.
Treatment Options
Myelodysplastic syndrome treatment options are heterogeneous and complex, ranging from supportive care to intensive chemotherapy and allogeneic stem cell transplantation. The choice of treatment depends on disease severity (lower- versus higher-risk), prognosis, patient age, overall health status, availability of therapeutic options, and patient preferences.
Treatment for Lower-Risk Disease
Patients with lower-risk MDS typically receive supportive care as the primary approach. This includes:
- Red blood cell transfusions to manage anemia
- Platelet transfusions to prevent bleeding complications
- Growth factor support to boost blood cell production
- Antibiotics for infections as needed
- Regular monitoring with blood counts and bone marrow evaluations
Once treatment goals and plans are established, patients with lower-risk disease often continue follow-up with their primary care provider, with periodic consultation with a hematologist.
Treatment for Higher-Risk Disease
Patients with higher-risk MDS require immediate intervention due to the substantial risk of transformation to acute myeloid leukemia. Treatment options include:
Hypomethylating Agents: Methyltransferase inhibitors such as azacitidine and decitabine are commonly used as first-line therapy for higher-risk MDS. These agents work by altering methylation patterns in cancer cells and can induce differentiation and cell death of leukemic clones. Studies have demonstrated that combination therapy approaches, using hypomethylating agents in combination with other agents, may improve response rates, increase complete remission rates, enhance transfusion independence, and prolong the time to transformation to acute myeloid leukemia.
Cytotoxic Chemotherapy: Similar to chemotherapy used in acute myeloid leukemia, intensive chemotherapy regimens may be considered for selected patients with higher-risk MDS.
Allogeneic Stem Cell Transplantation: For eligible patients, allogeneic stem cell transplantation offers the potential for cure and is one of the most effective treatments for MDS. However, transplantation involves significant risks and benefits must be carefully weighed against patient age and comorbidities.
Emerging Therapies: Clinical trials are continuously evaluating new agents and combination strategies to improve outcomes. Recent research has focused on identifying which mutations predict treatment response and exploring novel agents that can be added to hypomethylating therapy to enhance efficacy.
Factors Affecting Treatment Management
Several factors complicate the management of MDS and may worsen prognosis. Older age itself increases disease complexity. Additionally, comorbidities such as coronary artery disease, chronic obstructive pulmonary disease, and chronic kidney disease make treatment selection more challenging and can negatively impact outcomes. These factors must be carefully considered when developing individualized treatment plans.
Prognostic Models and Classification Systems
Several classification schemes and prognostic models guide the selection of appropriate therapy. These systems integrate information about myeloblast counts, cytopenia degree, and cytogenetic abnormalities to provide risk stratification and guide treatment decisions. The most widely used prognostic systems have been established by international working groups and are regularly updated as new data emerge regarding mutation patterns and treatment responses.
Key Clinical Considerations
Life expectancy at the time of diagnosis depends on the types of cells affected and the disease risk category. Supportive and disease-altering options are available to improve outcomes and quality of life. Prompt referral to a hematologist or oncologist is essential for confirmation of diagnosis and initiation of an appropriate treatment plan.
Frequently Asked Questions
Q: What is the difference between MDS and acute myeloid leukemia?
A: Myelodysplastic syndrome is a disorder of blood cell underproduction that can transform into acute myeloid leukemia. AML is characterized by an excess of immature blood cells in the bone marrow and blood, whereas MDS involves ineffective production of blood cells. While MDS can progress to AML, they are distinct entities with different treatment approaches.
Q: How often do patients with MDS require monitoring?
A: Monitoring frequency depends on disease risk category. Lower-risk patients may have less frequent evaluations, while higher-risk patients require close monitoring and more frequent blood tests and bone marrow studies to assess disease progression and treatment response.
Q: Can MDS be cured?
A: While some lower-risk MDS patients experience stable disease for years with supportive care, cure is most likely achieved through allogeneic stem cell transplantation. For higher-risk patients, the goal is to delay progression to acute myeloid leukemia and maintain quality of life.
Q: What role do genetic mutations play in MDS treatment?
A: Specific genetic mutations help predict disease behavior (lower- versus higher-risk), guide treatment selection, and predict response to therapy. Mutation testing is increasingly incorporated into diagnostic and prognostic algorithms to provide more personalized treatment recommendations.
Q: Is age a barrier to receiving treatment?
A: While older age itself presents challenges in MDS management, age alone should not be a barrier to appropriate treatment. Rather, overall health status, comorbidities, and functional status should be considered when selecting therapies.
References
- Myelodysplastic syndromes: A practical approach to diagnosis and treatment — Cleveland Clinic Journal of Medicine. 2010-01-15. https://www.ccjm.org/content/ccjom/77/1/37.full.pdf
- The myelodysplastic syndromes — PubMed/National Institutes of Health. 2007. https://pubmed.ncbi.nlm.nih.gov/17309328
- In-Depth Diagnostic Testing in Older Patients with Myelodysplastic Syndromes — Cleveland Clinic. 2024. https://consultqd.clevelandclinic.org/in-depth-diagnostic-testing-in-older-patients-with-myelodysplastic-syndromes
- Clinical Management of Myeloid Malignancies in an Era of Novel Therapeutics — Cleveland Clinic Medical Education. 2024. https://www.clevelandclinicmeded.com/online/clinical-management-myeloid/
- Myelodysplastic Syndrome (MDS): Symptoms, Diagnosis & Treatment — Cleveland Clinic Patient Education. 2024. https://my.clevelandclinic.org/health/diseases/6192-myelodysplastic-syndrome-myelodysplasia
- Current and Emerging Therapies for Myelodysplastic Syndromes — Blood Cancer United. 2024. https://bloodcancerunited.org/article/current-and-emerging-therapies-myelodysplastic-syndromes-mds
Read full bio of medha deb