Naevi with Special Features: Dermoscopy Images
Explore dermoscopic images and clinical insights into combined, halo, cockade, Meyerson, and recurrent naevi for accurate diagnosis.
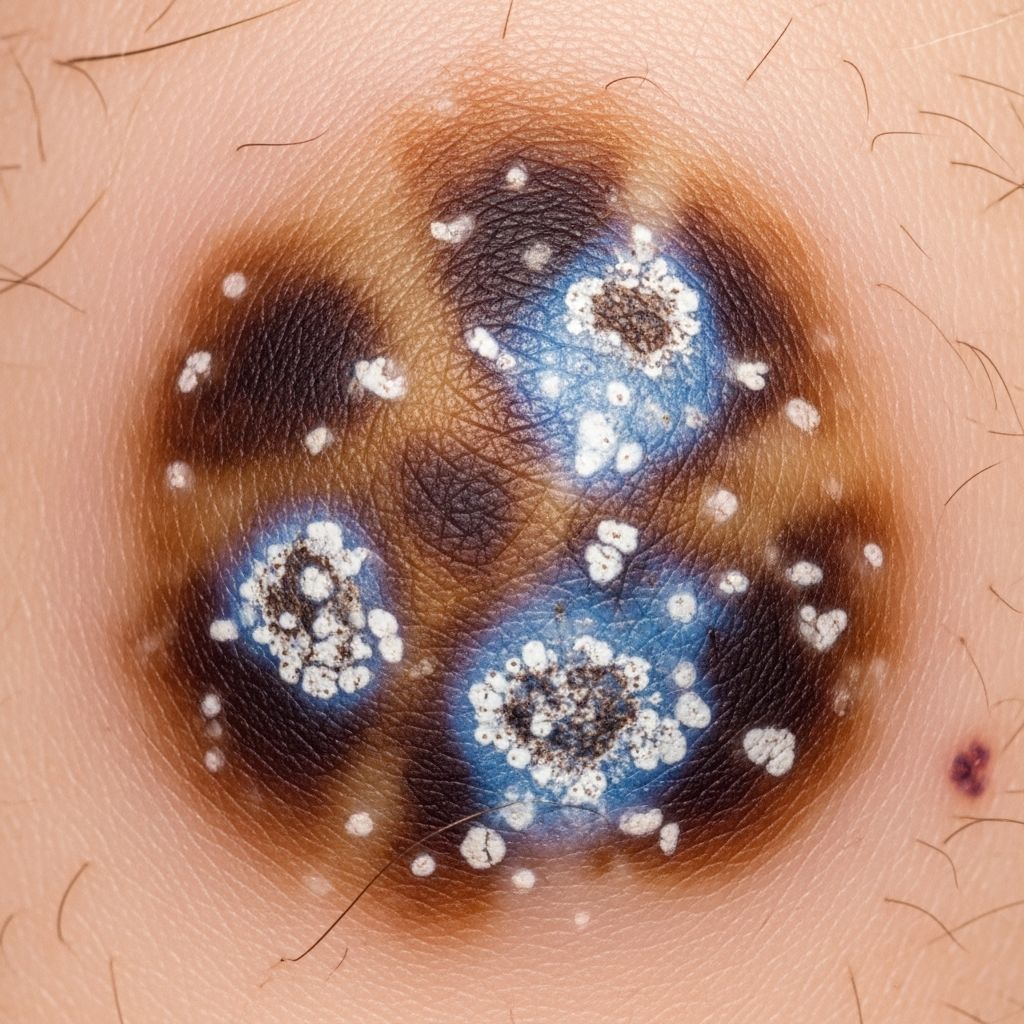
Naevi with Special Features Images
This comprehensive image gallery showcases the clinical and dermoscopic appearances of naevi exhibiting special features. These lesions often present diagnostic challenges due to their atypical patterns, which can mimic melanoma. Dermoscopy plays a crucial role in distinguishing benign naevi from malignant lesions by revealing specific pigment networks, globules, and structural arrangements. Understanding these patterns enhances diagnostic accuracy and guides appropriate management.
Combined Naevi
Combined naevi represent the juxtaposition or merger of two distinct naevus types, typically a reticular (acquired) component alongside a globular (congenital) or blue naevus element. Clinically, they appear as asymmetrical lesions with varied pigmentation and topography—flat macular areas adjacent to elevated papular components. These naevi arise in both children and adults, often on the trunk or limbs.
Dermoscopically, combined naevi display two coexisting patterns: a peripheral reticular network of thin lines forming meshes, juxtaposed with central globular aggregates of roundish structures or homogenous blue pigmentation. The transition between patterns is sharp, without blending, which is a key diagnostic clue. This dual-pattern feature arises from the histological superposition of junctional melanocytic nests (reticular) over dermal melanocytes (globular/blue).
- Clinical images: Multiple examples show brown-black macules with superimposed darker papules, measuring 5-15 mm, symmetrical borders, and uniform colour within components.
- Dermoscopy images: Clear demarcation between reticular periphery (brown lines on white background) and central globules (pigmented dots/clods) or blue homogenous areas. No atypical features like irregular streaks or polymorphous vessels.
Histologically confirmed benign, these naevi require excision only if changing or atypical. Regular dermoscopic monitoring is recommended for patients with multiple lesions. Approximately 10-20% of adult naevi exhibit combined features, emphasizing their clinical relevance.
Halo Naevi
Halo naevi are characterised by a central melanocytic naevus surrounded by a symmetrical rim of depigmentation, resulting from a lymphocytic immune reaction targeting nevus cells. Most common in adolescents and young adults, they frequently appear on the trunk and spontaneously regress over 1-8 years. The halo represents vitiligo-like hypopigmentation without scarring.
Clinically, the central lesion is a typical globular or reticular naevus (3-10 mm) encircled by a white halo 5-15 mm wide. Multiple halo naevi may occur simultaneously, and associated vitiligo or melanoma risk elevation is noted in some patients.
Dermoscopy reveals a central naevus pattern (globules, network, or homogenous brown) with sharp peripheral hypopigmentation lacking pigment network or structures. White dots or structureless white areas may appear in evolving halos. Vessels, if present, are regular dotted or linear, distinguishing from regressing melanoma’s atypical polymorphic vasculature.
- Clinical images: Round central mole with expanding white rim; early stages show faint halo, mature stages complete achromia.
- Dermoscopy images: Symmetrical white rim abutting central pigmentation; no blue-white veil or peppering typical of melanoma regression.
Halo naevi indicate immune surveillance and are generally reassuring, though central atypical features warrant biopsy.
Cockade Naevi
Cockade (targetoid) naevi feature a distinctive ‘bull’s-eye’ appearance with central hypopigmentation surrounded by a peripheral pigmented ring, primarily on the limbs of young individuals (10-30 years). They are benign, recurrent, and may represent a variant of recurrent naevi post-trauma.
Clinically, these 4-8 mm lesions display a pale center, brown ring, and sometimes an outer hypopigmented halo, evoking a cockade badge.
Dermoscopy shows a central white structureless area encircled by a sharp brown ring network, often with peripheral globules or homogenous pigmentation. The pattern is highly symmetrical, aiding differentiation from melanoma’s asymmetrical pigmentation.
- Clinical images: Target-like lesions on arms/legs; multiple per patient possible.
- Dermoscopy images: Concentric rings: white center, brown network ring, optional outer pigmentation.
Rare but pathognomonic, cockade naevi require no intervention unless atypical evolution.
Meyerson Naevi (Eczematous Halo)
Meyerson naevi exhibit an eczematous reaction overlying or surrounding a pre-existing naevus, presenting as itchy, scaling plaques. Common in children and young adults, they resolve spontaneously but may recur. The eczema is benign, possibly autoimmune-mediated.
Clinically: Central brown naevus (globular/reticular) covered by yellow crusts, vesicles, and scaling erythema, 5-12 mm size.
Dermoscopy: Obscured central naevus pattern under dotted vessels, white/yellow crusts, and orange scaling. Scale removal reveals underlying benign globules/network. Regression shows fading eczema with naevus persistence or halo formation.
- Clinical images: Inflamed, crusted moles on trunk/extremities.
- Dermoscopy images: Polymorphous vessels (dotted, glomerular) over obscured pigmentation; post-scale benign pattern.
Biopsy rarely needed; topical steroids suffice. Distinguish from inflamed melanoma via short history and resolution.
Recurrent Naevi
Recurrent naevi arise at previous biopsy/excision sites, showing repigmentation within scars. They mimic local recurrence of melanoma, necessitating dermoscopy for differentiation. Most occur 6-12 months post-procedure on sun-exposed sites.
Clinically: Irregular brown-black macule within hypopigmented scar, often centrifugal spread.
Dermoscopy: Central white scar (structureless fibrosis) surrounded by peripheral irregular network, globules, or streaks confined to scar edges. No radial streaming or blue-white areas beyond scar limits, unlike melanoma.
- Clinical images: Pigment islands in pale surgical scars.
- Dermoscopy images: Abrupt pigment edge at scar border; benign internal patterns.
Observation preferred; excision if expanding beyond scar.
Diagnostic Table: Key Dermoscopic Features
| Type | Clinical | Dermoscopy | Management |
|---|---|---|---|
| Combined | Dual topography | Reticular + globular/blue | Monitor |
| Halo | Depigmented rim | Central pattern + white halo | Observe |
| Cockade | Targetoid | Central white + ring network | Reassure |
| Meyerson | Eczematous | Vessels + crusts over naevus | Topical Rx |
| Recurrent | In scar | Pigment confined to scar | Monitor/biopsy if atypical |
Frequently Asked Questions (FAQs)
Q: How does dermoscopy differentiate halo naevi from regressing melanoma?
A: Halo naevi show symmetrical white rim without blue-white veil, peppering, or atypical vessels; central pattern remains benign.
Q: When should combined naevi be excised?
A: Only if changing (size, colour, symptoms) or dermoscopically atypical (asymmetry, irregular streaks).
Q: Do Meyerson naevi indicate underlying malignancy?
A: No, they are reactive and resolve; short history <3 months and scale-stripping revealing benign pattern confirm.
Q: What is the prognosis for recurrent naevi?
A: Benign if pigment stays within scar; 95%+ are non-malignant with dermoscopic confinement.
Q: Are cockade naevi associated with melanoma risk?
A: No increased risk; they are rare benign variants, symmetrical and stable.
References
- Melanocytic naevi: new classification — DermNet NZ. 2008 (updated). https://dermnetnz.org/cme/dermoscopy-course/melanocytic-naevi-new-classification
- Dermoscopy of atypical naevi — DermNet NZ. 2008 (updated). https://dermnetnz.org/cme/dermoscopy-course/dermoscopy-of-atypical-naevi
- Melanocytic naevus — DermNet NZ. 2023-10-01. https://dermnetnz.org/topics/melanocytic-naevus
- Naevi with special features images — DermNet NZ. 2008 (updated). https://dermnetnz.org/cme/dermoscopy-course/naevi-with-special-features-images
- Dermoscopy of benign melanocytic lesions — DermNet NZ. 2008 (updated). https://dermnetnz.org/cme/dermoscopy-course/dermoscopy-of-benign-melanocytic-lesions
Read full bio of medha deb












