Necrotizing Periodontal Disease: Causes, Signs, Treatments
Understanding necrotising periodontal disease: causes, symptoms, diagnosis, and effective treatment strategies for this severe gum condition.
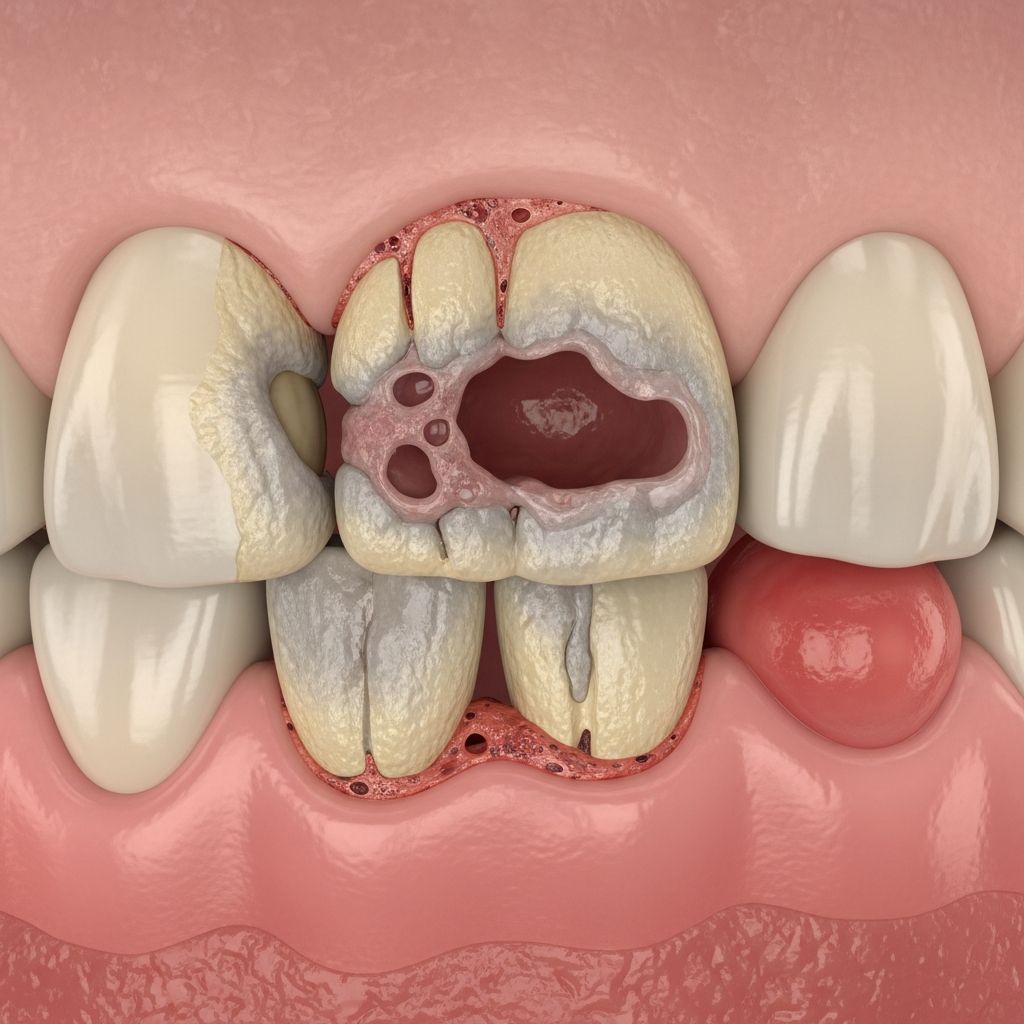
Necrotising Periodontal Disease
Necrotising periodontal disease (NPD), also known as necrotizing ulcerative gingivitis (NUG) or necrotizing periodontitis, is a severe, rapidly progressing infection of the gums characterized by tissue necrosis, intense pain, and potential bone loss. It primarily affects the interdental papillae and can spread if untreated, leading to significant oral morbidity. This condition is opportunistic, arising from bacterial dysbiosis in susceptible hosts, and requires prompt intervention to prevent irreversible damage.
What is necrotising periodontal disease?
Necrotising periodontal disease encompasses a spectrum of destructive gingival infections, including necrotizing gingivitis (NG), necrotizing periodontitis (NP), and necrotizing stomatitis. NG is the earliest form, limited to interdental papillae necrosis with a punched-out appearance, reversible if treated early before attachment loss occurs. Progression to NP involves deeper tissue destruction, periodontal ligament involvement, and alveolar bone exposure, often with pseudomembrane formation. In advanced cases, it extends to necrotizing stomatitis, affecting broader oral mucosa and potentially causing facial deformity or life-threatening complications. NPD is classified under Stage III/IV periodontitis in modern systems but distinguished by its acute necrosis and pain. Unlike chronic periodontitis, NPD develops rapidly, often within days, due to synergistic polymicrobial infection under impaired host immunity.
Who gets necrotising periodontal disease?
NPD predominantly affects individuals with predisposing host factors that compromise immune defenses. High-risk groups include those with HIV/AIDS, where it may present as the initial sign of infection, affecting up to 10% of untreated cases. It is also prevalent in malnourished children in developing countries, linked to poor sanitation and vitamin deficiencies. Other vulnerable populations encompass smokers, as tobacco impairs neutrophil function and gingival blood flow; psychologically stressed individuals; those with sleep deprivation; and patients undergoing immunosuppressive therapies or with conditions like leukemia. Poor oral hygiene exacerbates plaque accumulation, but NPD is rare in healthy individuals, occurring in less than 1% of the general population. Acute outbreaks are noted in young adults (18-30 years) amid stressors like military service or exams.
- Immunosuppressed patients (HIV, chemotherapy)
- Smokers and tobacco users
- Malnourished individuals, especially children
- Those with psychological stress or sleep deprivation
- Poor oral hygiene practitioners
Causes of necrotising periodontal disease
The primary cause is bacterial invasion from dental plaque biofilms, dominated by anaerobic fusobacteria (Fusobacterium nucleatum), spirochetes (Treponema spp.), Prevotella intermedia, and Porphyromonas gingivalis. These form a dysbiotic microbiome with reduced diversity, promoting necrosis through synergistic interactions and virulence factors like leukotoxins. Host factors are crucial: immunosuppression allows unchecked proliferation, while smoking induces local hypoxia and inflammation. Malnutrition depletes immune cells and antioxidants, stress elevates cortisol suppressing immunity, and sleep loss impairs cytokine responses. Pre-existing gingivitis can rapidly worsen under these triggers, but NPD requires both microbial and host compromise. Environmental factors like high altitude or poor sleep in outbreaks further contribute.
Clinical features of necrotising periodontal disease
Symptoms onset acutely with severe gingival pain, distinguishing NPD from painless chronic periodontitis. Patients report fetid halitosis, spontaneous bleeding, metallic taste, and eating difficulties leading to malaise or weight loss. Systemic signs like fever, lymphadenopathy, and fatigue occur in 30-50% of cases, especially advanced NP.
Key clinical signs include:
- Punched-out interdental craters with grayish pseudomembrane (fibrin, debris, PMNs)
- Sloughing necrotic tissue, erythema, and edema
- Bleeding on provocation
- In NP: bone exposure, tooth mobility, attachment loss >2mm within days
- Advanced: mucosal necrosis, osteitis, sequestra formation
Lesions favor anterior sextants, multiple sites possible. Pain halts hygiene, worsening infection[20 from 1]. Images typically show cratered papillae with pseudomembrane, progressing to exposed bone.
Diagnosis of necrotising periodontal disease
Diagnosis is clinical, based on history of acute pain, risk factors, and pathognomonic signs: interdental necrosis, ulceration, bleeding, and rapid progression. Differential includes herpetic gingivitis (vesicles, no necrosis), agranulocytosis (systemic), or acute leukemias (petechiae). HIV testing recommended if risk present.
Investigations:
- Intraoral exam: confirm necrosis extent
- Periapical radiographs: assess bone loss (vertical defects in NP)
- Microbiology: confirm fusospirochetal flora (phase contrast microscopy)
- Blood tests: CBC for neutropenia, HIV serology, nutritional markers
Staging: NG (papillae only), NP (attachment/bone loss), stomatitis (extensive). Early detection prevents progression.
Treatment of necrotising periodontal disease
Treatment is phased: acute management, supportive care, resolution, and maintenance. Outpatient for mild-moderate; hospitalization for systemic involvement.
Acute phase (first visit):
- Pain relief: Paracetamol, NSAIDs (avoid aspirins)
- Debridement: Gentle supragingival scaling under local anesthesia; remove pseudomembrane with 0.12% chlorhexidine-soaked pellet. Avoid aggressive subgingival till pain subsides
- Antiseptics: Chlorhexidine 0.12-0.2% rinse (bid), hydrogen peroxide 1.5% (tid, diluted)
- Antibiotics: Metronidazole 400mg tid x 3-7 days ± amoxicillin 500mg tid if non-responders
Supportive: hydration, nutrition (vit C/B, zinc if deficient), smoking cessation, stress reduction. Symptoms resolve in 24-48h with therapy.
Resolution phase (3-5 days post-acute):
- Full debridement, root planing
- Oral hygiene instruction: soft brush, rinses
- Address risk factors
Repair phase (weeks later):
- Surgery if defects: gingivectomy/oplasty for fibrosis, bone grafts for defects
Maintenance:
3-monthly recalls; high recurrence risk.
| Phase | Interventions |
|---|---|
| Acute | Debridement, CHX, H2O2, analgesics, antibiotics |
| Resolution | Full cleaning, OHI |
| Repair | Surgery if needed |
| Maintenance | Regular recalls |
Prevention of necrotising periodontal disease
Prevention targets risk modification: optimal oral hygiene (brushing, flossing, professional cleans), smoking cessation, balanced nutrition, stress/sleep management. High-risk patients (HIV, post-transplant) need vigilant monitoring. Early intervention at pain/bleeding onset prevents progression. Population measures in endemic areas include malnutrition programs.
Frequently Asked Questions
What causes necrotising periodontal disease?
Anaerobic bacteria from plaque in hosts with poor immunity, smoking, malnutrition, or stress.
Is necrotising periodontal disease contagious?
No, but poor hygiene spreads bacteria; it’s host-dependent.
How serious is necrotising periodontal disease?
Very; untreated leads to tooth loss, bone destruction, systemic spread.
Can necrotising periodontal disease be cured?
Yes, early treatment reverses NG; NP needs ongoing care to halt damage.
What does necrotising gum disease look like?
Punched-out gum craters with gray pseudomembrane, bleeding, bad breath.
Does smoking cause NPD?
Strong risk factor; cessation is key to treatment success.
References
- Necrotizing Periodontal Diseases — StatPearls Publishing. 2023-05-01. https://www.ncbi.nlm.nih.gov/books/NBK557417/
- Necrotizing Periodontal Diseases | Point of Care — StatPearls. 2023-05-01. https://www.statpearls.com/point-of-care/34402
- Necrotizing Periodontal Disease — Ada Health. 2023. https://ada.com/conditions/necrotizing-periodontal-disease/
- Necrotising periodontal disease — DermNet NZ. 2023. https://dermnetnz.org/topics/necrotising-periodontal-disease
- Necrotizing Periodontal Diseases: Epidemiology, Clinical Features — J Periodontal Res. 2023. https://onlinelibrary.wiley.com/doi/10.1111/jre.70028
Read full bio of Sneha Tete