Non-Small Cell Lung Cancer Prognosis: Stage-By-Stage Guide
Understanding NSCLC prognosis: survival rates, staging, treatments, and factors influencing outcomes for better management.
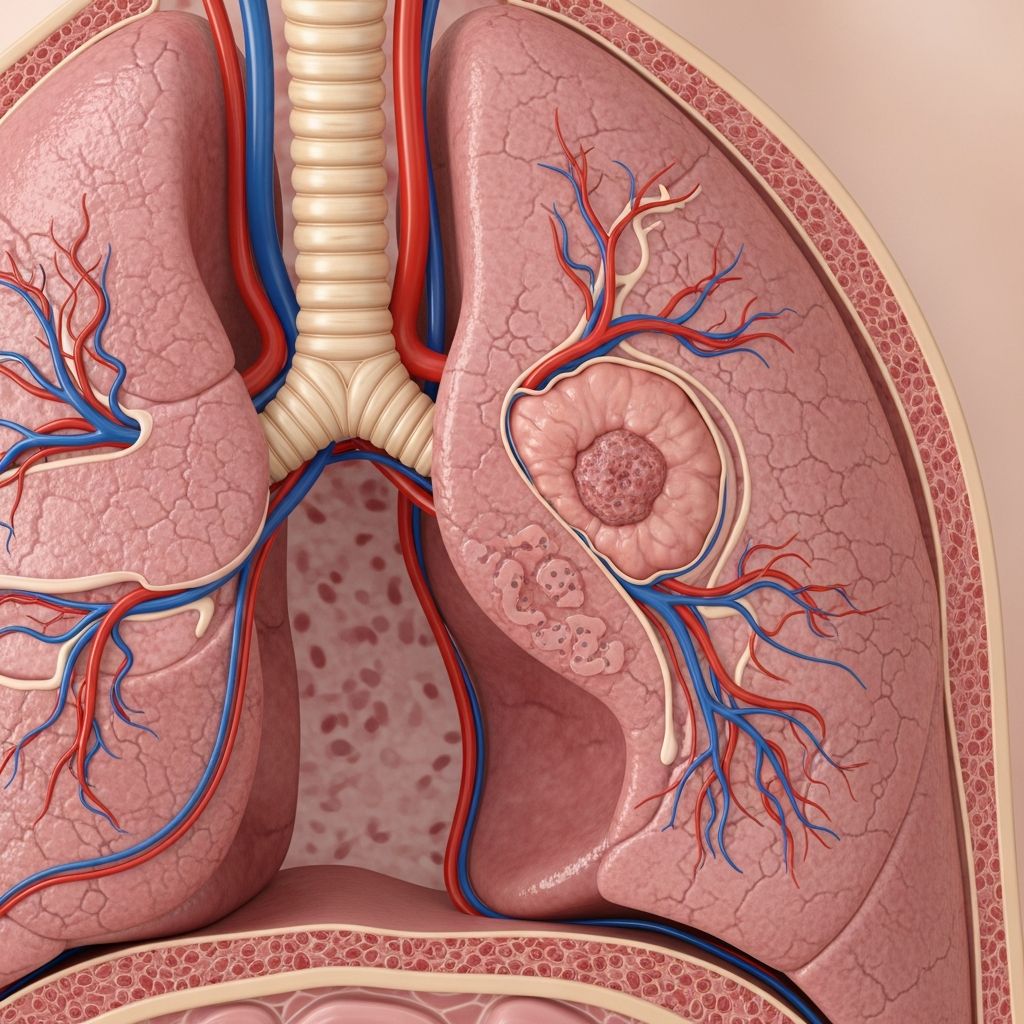
Non-small cell lung cancer (NSCLC) prognosis varies widely based on stage at diagnosis, tumor characteristics, patient health, and treatment advances, with an overall 5-year survival rate of approximately 28-32%.
Receiving an NSCLC diagnosis prompts critical questions about life expectancy, treatment options, and quality of life. While statistics provide general guidance, individual outcomes depend on multiple factors. This article examines NSCLC types, staging, survival rates, prognostic influencers, and emerging therapies that are enhancing prognoses.
What Is Non-Small Cell Lung Cancer?
**Non-small cell lung cancer (NSCLC)** accounts for about 80-85% of all lung cancer cases and develops when lung cells mutate and grow uncontrollably. Unlike small cell lung cancer, NSCLC grows and spreads more slowly but is often diagnosed at advanced stages due to subtle early symptoms.
NSCLC originates in the lungs’ epithelial cells and includes several subtypes:
- Adenocarcinoma: The most common type (40% of cases), often starting in mucus-producing cells on the lung’s outer edges. It affects smokers and non-smokers alike.
- Squamous cell carcinoma: Comprises 25-30% of cases, linked to central airways and heavy smoking.
- Large cell carcinoma: Makes up 5-10%, growing rapidly with large, abnormal cells.
- Rarer subtypes include adenosquamous and sarcomatoid carcinomas.
Risk factors include smoking (85% of cases), radon exposure, asbestos, air pollution, family history, and genetic mutations like EGFR or ALK. Early detection remains challenging as symptoms like persistent cough, shortness of breath, chest pain, or unexplained weight loss often appear late.
NSCLC Staging: Key to Prognosis
Staging determines how far cancer has spread, guiding treatment and prognosis. The TNM system (Tumor size, Node involvement, Metastasis) classifies NSCLC into stages 0-IV.
- Localized (Stage I-II): Cancer confined to lung/nearby lymph nodes.
- Regional (Stage III): Spread to nearby structures or distant lymph nodes.
- Distant (Stage IV): Metastatic to distant organs like brain, bones, or liver.
Imaging (CT, PET scans), biopsies, and bronchoscopy confirm staging post-diagnosis. Accurate staging is crucial: early-stage NSCLC offers curative potential, while advanced stages focus on control and palliation.
Non-Small Cell Lung Cancer Prognosis and Survival Rates
The
5-year relative survival rate
for NSCLC is 28-32% overall, meaning people with NSCLC are 28-32% as likely as the general population to survive 5 years post-diagnosis. These rates, from SEER data (2015-2021 diagnoses), vary significantly by stage:| SEER Stage | 5-Year Relative Survival Rate (NSCLC) |
|---|---|
| Localized | 67% |
| Regional | 40% |
| Distant (Metastatic) | 9-12% |
| All Stages Combined | 32% |
These figures are estimates and do not predict individual outcomes. Factors like age, comorbidities, and response to therapy influence results. Notably, rates are improving due to novel treatments not reflected in older data.
Factors Affecting NSCLC Prognosis
Several elements beyond stage impact prognosis:
- Tumor Biology: Mutations (e.g., EGFR, ALK, KRAS) allow targeted therapies, improving survival in 10-30% of cases.
- Patient Health: Better performance status (ability to perform daily activities) correlates with superior outcomes.
- Age and Comorbidities: Younger, healthier patients fare better; COPD or heart disease worsens prognosis.
- Smoking Status: Continued smoking reduces treatment efficacy and survival.
- Treatment Access: Timely intervention with surgery, radiation, chemo, or immunotherapy enhances longevity.
Genomic profiling identifies actionable mutations, shifting some advanced cases toward chronic management.
Treatments for NSCLC and Their Impact on Prognosis
Treatment is stage-specific and multimodal:
- Early-Stage (I-II): Surgery (lobectomy) offers cure rates up to 65-90%; adjuvant chemo boosts survival by 5-15%.
- Locally Advanced (III): Chemoradiation followed by immunotherapy (e.g., durvalumab) improves 5-year survival to 40-50%.
- Advanced/Metastatic (IV): Systemic therapies including chemotherapy, targeted agents (osimertinib for EGFR), and immunotherapy (pembrolizumab) extend median survival from 10-12 months to 2+ years in responders.
**Targeted Therapy** attacks specific mutations, with drugs like alectinib for ALK yielding 70-80% response rates.
Immunotherapy
(PD-1/PD-L1 inhibitors) activates immune response, doubling survival in PD-L1-positive cases. Combinations are standard, per NCCN guidelines.Advances have markedly improved outcomes: a 2020 NEJM study showed lung cancer mortality declining due to these innovations. Supportive care (palliative radiation, symptom management) further enhances quality of life.
Can NSCLC Be Cured?
Yes, in early stages: Stage I surgery cures 80-90% of patients. Most diagnoses (60%) occur at stages III-IV, where cure is unlikely but long-term control is achievable with modern therapies—some metastatic patients now survive 5+ years.
Even incurable cases can be managed as chronic conditions, emphasizing multidisciplinary care.
Living with NSCLC: Quality of Life and Support
Beyond survival, prognosis includes quality of life. Treatments like immunotherapy have fewer side effects than traditional chemo. Lifestyle (quitting smoking, nutrition, exercise) and psychosocial support mitigate impacts.
Clinical trials offer access to cutting-edge options, potentially improving personal prognosis.
Frequently Asked Questions (FAQs)
What is the average survival time for NSCLC?
Overall 5-year survival is 28-32%, but stage-specific: 67% localized, 9-12% metastatic. Median survival for untreated metastatic is 4-6 months; treated, 12-24+ months.
Does NSCLC prognosis differ by subtype?
Adenocarcinoma often has better prognosis due to targetable mutations; squamous cell is more aggressive.
How do new treatments affect NSCLC survival?
Targeted therapies and immunotherapy have increased metastatic survival by 50-100% in eligible patients.
Can lifestyle improve NSCLC prognosis?
Yes, smoking cessation, exercise, and healthy weight improve treatment tolerance and outcomes.
What if NSCLC recurs after treatment?
Prognosis depends on site/time; salvage therapies like re-irradiation or new agents can extend life.
References
- Non-Small Cell Lung Cancer Prognosis: What to Expect with NSCLC — GoodRx. 2024. https://www.goodrx.com/conditions/lung-cancer/nsclc-prognosis
- Non-Small Cell Lung Cancer (NSCLC): Symptoms & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/6203-non-small-cell-lung-cancer
- 5-Year Survival Rates for Lung Cancer — American Cancer Society. 2024. https://www.cancer.org/cancer/types/lung-cancer/detection-diagnosis-staging/survival-rates.html
- Non-small cell lung cancer: current treatment and future advances — National Center for Biotechnology Information (PMC). 2016-07-12. https://pmc.ncbi.nlm.nih.gov/articles/PMC4931124/
- Non-small cell lung cancer treatment (PDQ®)–patient version — National Cancer Institute. 2024. https://www.cancer.gov/types/lung/patient/non-small-cell-lung-treatment-pdq
Read full bio of Sneha Tete