Nosebleeds (Epistaxis): Causes, Treatment & Prevention
Complete guide to understanding, treating, and preventing nosebleeds effectively.
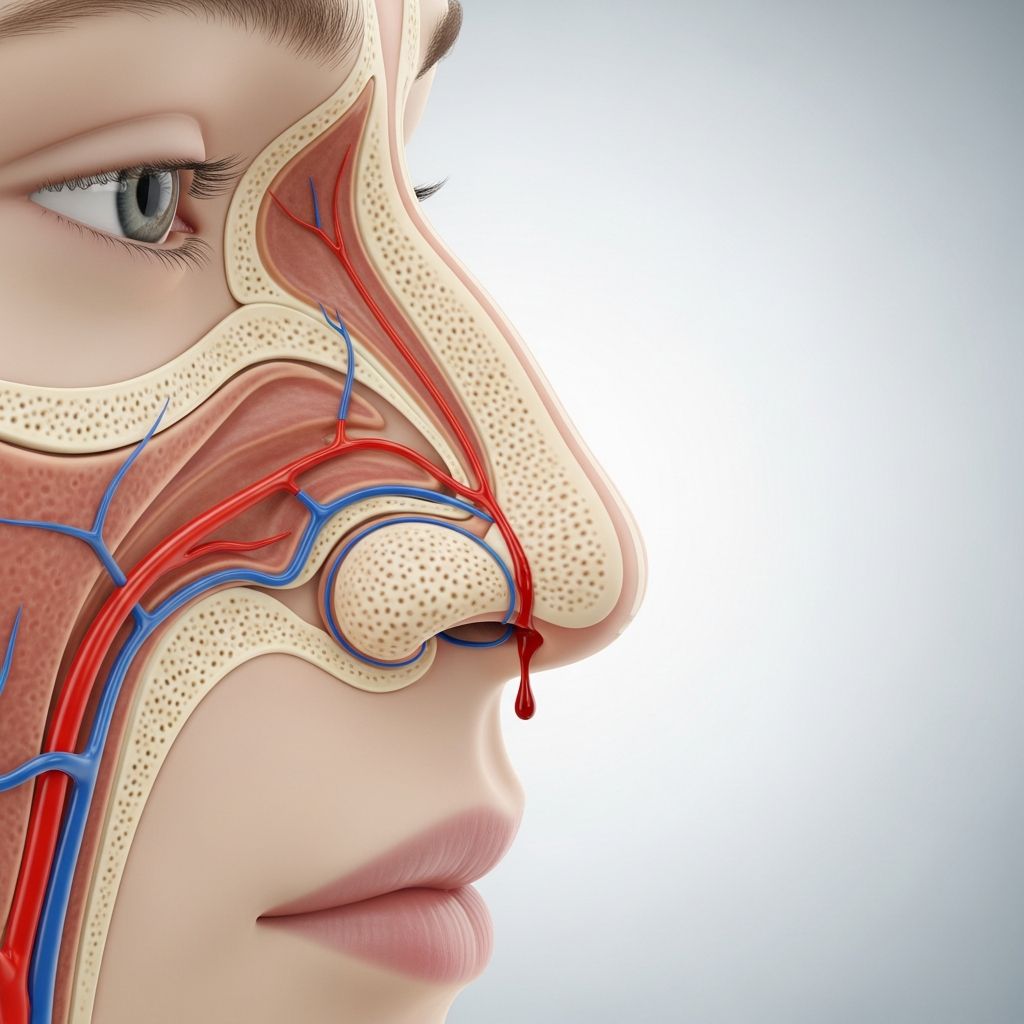
Understanding Nosebleeds (Epistaxis)
Epistaxis is the medical term for a nosebleed, which is a loss of blood from the tissue that lines the inside of your nose. While nosebleeds can be alarming and uncomfortable, they are usually not serious and can often be managed at home with simple first aid measures. However, understanding the causes, proper treatment techniques, and when to seek professional medical care is essential for effectively managing this common condition.
The nasal cavity contains numerous blood vessels that are close to the surface, making the nose particularly susceptible to bleeding. When these blood vessels become irritated, damaged, or ruptured, they can result in bleeding from one or both nostrils. The good news is that only 0.5% of nosebleed cases result in emergency room visits, and fewer than 0.2% require hospitalization. Severe nosebleeds that cause fatality or life-threatening complications are extremely rare.
Common Causes of Nosebleeds
Nosebleeds can occur for various reasons, ranging from environmental factors to underlying medical conditions. Understanding these causes can help you identify what triggered your nosebleed and take appropriate preventive measures.
Environmental and Lifestyle Factors: Dry air, particularly during winter months or in heated indoor environments, is one of the most common causes of nosebleeds. When the mucous membranes lining your nasal passages dry out, they become fragile and prone to bleeding. Trauma to the nose, whether from an accidental bump, aggressive nose blowing, or picking at the nasal lining, can also trigger bleeding. Intranasal drug use is another significant cause that damages the nasal tissue and blood vessels.
Medical Conditions: Certain underlying health conditions increase the risk of nosebleeds. These include high blood pressure, blood clotting disorders such as hemophilia or Von Willebrand disease, and hereditary hemorrhagic telangiectasia syndrome. Additionally, infections affecting the nasal passages, sinus infections, and allergies can make the nasal lining more susceptible to bleeding.
Medications: Blood-thinning medications such as warfarin, aspirin, and other anticoagulants or antiplatelet medications significantly increase bleeding risk. If you take these medications and experience frequent nosebleeds, consult your healthcare provider about your treatment plan.
Other Contributing Factors: Aging is associated with increased nosebleed frequency, as blood vessels become more fragile with age. Recent nasal surgery, low humidity environments, and excessive alcohol consumption can also contribute to nosebleeds.
How to Stop a Nosebleed: Step-by-Step Guide
When a nosebleed occurs, staying calm is the first and most important step. Anxiety causes blood pressure and heart rate to increase, which can worsen the bleeding. Follow these evidence-based steps to stop the bleeding effectively:
Step 1: Position Yourself Correctly Sit upright or lie back at a 45-degree angle. Avoid tilting your head backward, as this can cause blood to flow down your throat instead of out through your nostrils, making it difficult to assess whether the bleeding has stopped.
Step 2: Apply Pressure Gently pinch the soft part of your nose (the lower third) between your thumb and index finger. Apply firm, steady pressure by compressing the sides of your nostrils together. This direct compression works by compressing the blood vessels in the front part of your nasal septum, an area rich with blood vessels and the typical source of most nosebleeds.
Step 3: Hold Pressure for Adequate Time Maintain firm pressure for 10 to 15 minutes without releasing to check if the bleeding has stopped. It takes 8 to 10 minutes for fibrin proteins in your blood to form a clot. If you release your grip too early to check, you risk washing away the developing clot, forcing your body to start the clotting process all over again.
Step 4: Apply Cold While holding pressure, you can apply an ice pack or cold compress to the bridge of your nose. This helps constrict blood vessels and may accelerate clotting. Do not place ice directly on your skin; wrap it in a thin cloth first.
Step 5: Check and Repeat if Necessary After 10 to 15 minutes, gently release your grip and check if the bleeding has stopped. If blood continues to flow, pinch your nose again for another 10 minutes. If you are taking blood-thinning medications, you may need to apply pressure for a longer duration.
Step 6: Avoid Common Mistakes Do not tilt your head backward, insert tissues or tampons into your nostrils, or blow your nose forcefully after the bleeding stops. These actions can irritate the nasal lining and restart the bleeding process.
Medical Treatment Options
While most nosebleeds can be managed at home, some require professional medical intervention. Healthcare providers have several treatment options available depending on the severity and location of the bleeding.
Nasal Compression and Topical Treatment: When you visit a healthcare facility, providers may first attempt nasal compression combined with topical vasoconstrictors. These medications narrow blood vessels to reduce bleeding and improve visibility of the bleeding site.
Nasal Packing: For patients with persistent bleeding despite nasal compression, clinicians may treat ongoing active bleeding with nasal packing. This involves inserting gauze or special nasal sponges into the nasal cavity to apply direct pressure and promote clotting. For patients with a suspected bleeding disorder or those taking anticoagulation or antiplatelet medications, healthcare providers should use resorbable packing material that dissolves naturally rather than nonresorbable packing that requires removal.
Nasal Cautery: When a specific bleeding site is identified, healthcare providers may treat it with nasal cautery, which uses heat or chemical application to seal the blood vessel. The bleeding site must first be anesthetized before cautery is applied, and treatment should be restricted only to the active or suspected site of bleeding.
Advanced Interventions: For severe or recurrent nosebleeds that don’t respond to conventional treatments, more complex management options include endoscopic arterial ligation and interventional radiology procedures such as arterial embolization. These advanced techniques are typically reserved for cases of posterior nosebleeds or those associated with significant comorbid conditions.
When to Seek Emergency Medical Care
While most nosebleeds resolve with home care, certain situations warrant immediate medical attention. You should seek prompt care at an emergency room or call 911 in the following circumstances:
Duration of Bleeding: If bleeding continues for more than 20 minutes despite applying firm, sustained pressure to your nostrils, seek emergency care. After two rounds of holding your nose for 10 minutes each, if blood continues to flow, it is time to get prompt attention at an emergency room or urgent care facility.
Severity of Bleeding: If you experience heavy bleeding that soaks through large amounts of tissue or blood clots, or if you feel faint or dizzy from blood loss, seek immediate medical attention.
Recurrent Nosebleeds: If you experience frequent nosebleeds occurring multiple times per week or month, consult a healthcare provider to identify underlying causes.
Special Populations: Your threshold for seeking professional care should be lower if you have been diagnosed with a bleeding disorder such as hemophilia or Von Willebrand disease. Similarly, if you have a bloody nose and take blood-thinning medication, seek medical evaluation even if the bleeding appears mild.
Associated Symptoms: Seek medical care if your nosebleed is accompanied by difficulty breathing, chest pain, severe facial trauma, or signs of infection.
Posterior Nosebleeds: Older patients with posterior nosebleeds that do not stop and continue to bleed should seek emergency care, as these require professional packing and ER evaluation to control the bleeding and manage comorbid conditions such as diabetes or sleep apnea.
Prevention Strategies
Preventing nosebleeds is often more effective than managing them after they occur. Implement these evidence-based strategies to reduce your nosebleed frequency:
Maintain Nasal Moisture: Use a humidifier in your home during dry months to maintain adequate moisture in the air. This prevents the nasal mucous membranes from drying out. Applying moisturizing or lubricating agents, such as saline nasal spray or petroleum jelly, to the inside of your nostrils can also help keep nasal tissues hydrated.
Avoid Nasal Trauma: Avoid picking your nose, blowing your nose forcefully, or inserting objects into your nostrils. When you need to clear your nose, do so gently using saline rinses or sprays.
Control Blood Pressure: High blood pressure increases nosebleed risk. Work with your healthcare provider to maintain healthy blood pressure through medication, regular exercise, and dietary modifications such as reducing sodium intake.
Manage Medications Carefully: If you take blood-thinning medications or antiplatelet drugs, discuss any frequent nosebleeds with your healthcare provider. They may adjust your dosage or recommend preventive measures specific to your situation.
Avoid Irritants: Refrain from intranasal drug use and limit alcohol consumption, both of which can damage nasal tissues and increase bleeding risk. Avoid smoking and secondhand smoke exposure.
Treat Underlying Conditions: Effectively manage allergies, sinus infections, and other conditions affecting the nasal passages. Use appropriate medications prescribed by your healthcare provider and follow their recommendations for treatment.
Stay Hydrated: Drink adequate water throughout the day to maintain overall hydration, which helps keep mucous membranes healthy.
Patient Education and Follow-Up Care
Healthcare providers should educate patients with nosebleeds and their caregivers about preventive measures for nosebleeds, home treatment strategies, and indications to seek additional medical care. If you undergo nasal packing, your provider should explain the type of packing placed, the timing and plan for removal if using nonresorbable packing, postprocedure care instructions, and warning signs that would warrant prompt reassessment.
Additionally, clinicians should document factors that increase the frequency or severity of bleeding for any patient with a nosebleed, including personal or family history of bleeding disorders, use of anticoagulant or antiplatelet medications, or intranasal drug use. Following treatment with nonresorbable packing, surgery, or arterial ligation or embolization, healthcare providers should document the outcome of intervention within 30 days or document transition of care to ensure continuity of treatment.
Frequently Asked Questions About Nosebleeds
Q: How long should I hold pressure on my nose during a nosebleed?
A: Apply firm, steady pressure to the lower third of your nose for 10 to 15 minutes without releasing. It takes 8 to 10 minutes for blood clotting proteins to form a clot, so releasing early can restart the process.
Q: What should I do if the bleeding doesn’t stop after 20 minutes?
A: Seek emergency medical care. If bleeding persists after two rounds of 10-minute pressure applications, visit an emergency room or call 911 for professional treatment.
Q: Is it normal to have frequent nosebleeds?
A: Frequent nosebleeds may indicate an underlying condition such as high blood pressure, blood clotting disorders, or medication effects. Consult your healthcare provider if you experience multiple nosebleeds per week or month.
Q: Should I tilt my head backward during a nosebleed?
A: No. Tilting your head backward causes blood to flow down your throat. Instead, sit upright or lean forward slightly to let blood drain through your nostrils.
Q: Can nosebleeds be life-threatening?
A: Severe nosebleeds that cause fatality or life-threatening complications are extremely rare. However, older patients with posterior nosebleeds that don’t stop should seek emergency care.
Q: What medications increase nosebleed risk?
A: Blood-thinning medications such as warfarin, aspirin, and other anticoagulants or antiplatelet medications increase bleeding risk. Discuss frequent nosebleeds with your healthcare provider if you take these medications.
Q: How can I prevent nosebleeds?
A: Maintain nasal moisture using a humidifier, avoid nasal trauma, control blood pressure, manage allergies and sinus infections, stay hydrated, and avoid intranasal drug use and smoking.
References
- Clinical Practice Guideline: Nosebleed (Epistaxis) — PubMed/National Center for Biotechnology Information. 2020. https://pubmed.ncbi.nlm.nih.gov/31910111/
- How To Stop a Nosebleed — Cleveland Clinic Health. 2024. https://health.clevelandclinic.org/how-to-stop-a-nosebleed
- When To Worry About a Nosebleed — Cleveland Clinic Health. 2024. https://health.clevelandclinic.org/do-you-get-too-many-nosebleeds-when-to-worry
- Understanding Nosebleeds with Dr. Mohamad Chaaban — Cleveland Clinic Podcasts. 2024. https://my.clevelandclinic.org/podcasts/health-essentials/understanding-nosebleeds-with-dr-mohamad-chaaban
- Nosebleeds While Pregnant: Causes, Treatment & Prevention — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/symptoms/22342-nosebleeds-while-pregnant
- Nosebleeds: Here’s what to do — Safety and Health Magazine. 2022. https://www.safetyandhealthmagazine.com/articles/22231-nosebleeds-heres-what-to-do
Read full bio of medha deb













