Osteoarthritis vs Rheumatoid Arthritis: Key Differences
Understanding the distinct causes, symptoms, and treatments of OA and RA for better joint health management.
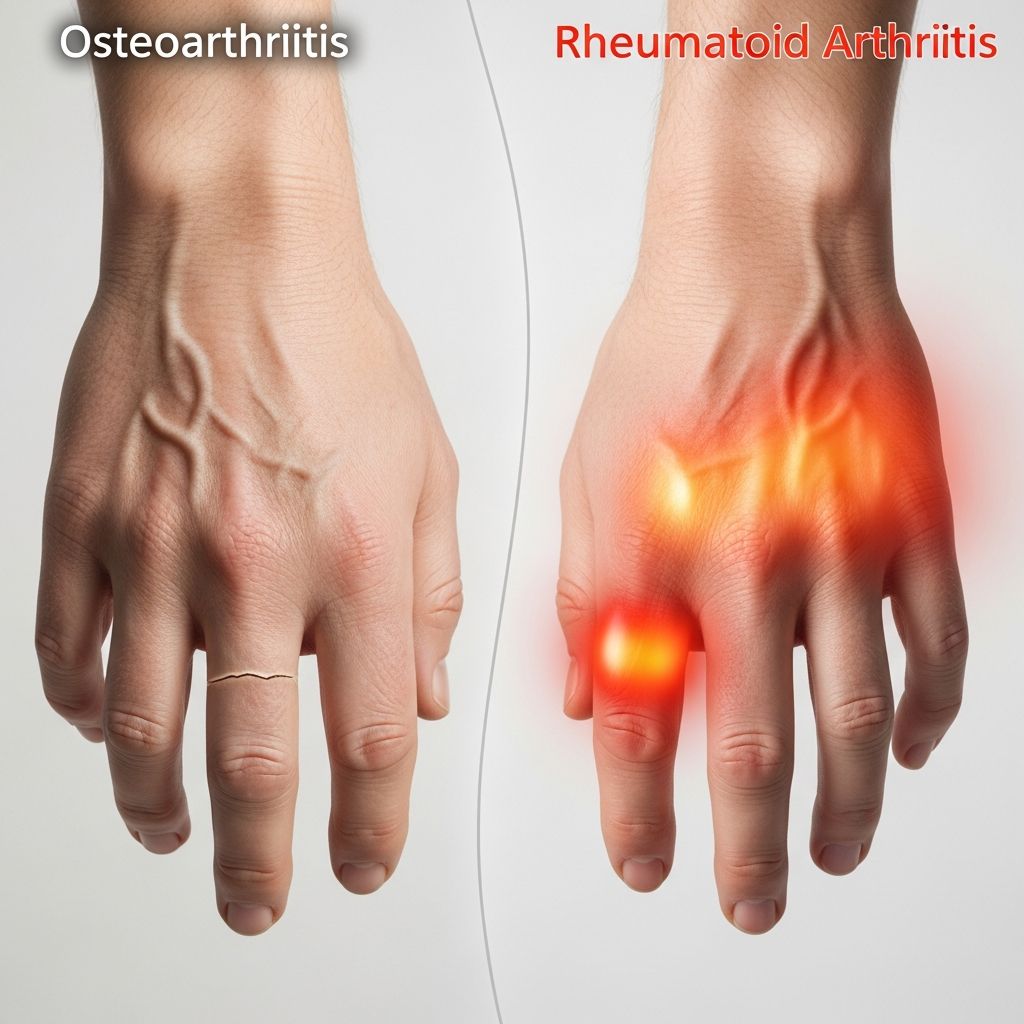
Explain the Pain: Is It Osteoarthritis or Rheumatoid Arthritis?
Joint pain affects millions of people worldwide, and two of the most common culprits are osteoarthritis (OA) and rheumatoid arthritis (RA). While both conditions cause joint discomfort, stiffness, and reduced mobility, they are fundamentally different diseases with distinct causes, progression patterns, and treatment approaches. Understanding the differences between these two types of arthritis is essential for accurate diagnosis and effective management. Between 30 to 50 percent of adults over the age of 65 have osteoarthritis, making it the most common form of arthritis. However, rheumatoid arthritis affects people across all age groups and requires different management strategies. This comprehensive guide explores the key distinctions between OA and RA, helping you better understand your symptoms and work more effectively with healthcare providers.
Understanding the Fundamental Differences
Osteoarthritis is a degenerative joint disease caused by the breakdown of cartilage over time. Cartilage is the smooth, protective tissue that covers the ends of bones and allows them to glide smoothly over each other. As cartilage deteriorates due to age, wear and tear, or injury, the underlying bones begin to rub together, causing pain, stiffness, and reduced joint function.
Rheumatoid arthritis, by contrast, is an autoimmune inflammatory disease. In RA, the body’s immune system mistakenly identifies the synovial membrane—the lining that lubricates and protects joints—as a threat and launches an attack against it. This autoimmune response causes inflammation, joint damage, and systemic symptoms that can extend beyond the joints to affect other parts of the body.
Symptom Patterns: How They Differ
Morning Stiffness Duration
One of the most reliable distinguishing features between OA and RA is the duration of morning stiffness. A general rule of thumb is that if your joints remain stiff in the morning for longer than 30 minutes, rheumatoid arthritis is more likely. If you experience stiffness for less than 30 minutes, osteoarthritis is more probable. In fact, RA often causes morning stiffness that can last an hour or more, significantly impacting daily activities.
Symmetry of Joint Pain
Joint symmetry provides another important diagnostic clue. Rheumatoid arthritis typically causes symmetrical pain, affecting the same joints on both sides of the body simultaneously. For example, if your right wrist is painful and swollen, your left wrist is likely experiencing similar symptoms. Osteoarthritis, however, is often asymmetrical, affecting joints unevenly. You might experience significant pain in one hand or wrist while the other remains relatively unaffected, since osteoarthritis targets joints based on use patterns and previous injuries.
Pain Type and Behavior
The nature of pain differs between these conditions. Rheumatoid arthritis produces inflammatory pain that typically worsens when at rest but improves with movement and activity. This is why RA patients often feel better after warming up their joints in the morning. Osteoarthritis, conversely, causes mechanical pain that worsens with movement and activity, then improves with rest. This distinction is crucial for understanding how to manage each condition effectively.
Visible Joint Changes
Beyond pain and stiffness, RA frequently causes visible swelling, warmth, and redness in affected joints. These signs reflect the underlying inflammatory process. Osteoarthritis may cause mild swelling, but it typically lacks the warmth and redness characteristic of RA. Additionally, OA can produce bony bumps over finger joints, known as Heberden’s nodes, which are less common in rheumatoid arthritis.
Systemic Symptoms and Disease Scope
A critical distinction between these diseases involves their systemic effects. Osteoarthritis is primarily a local, joint-specific condition. While it can damage multiple joints over time, the disease remains confined to affected joints. You won’t experience generalized symptoms elsewhere in your body.
Rheumatoid arthritis, being an autoimmune disease, often produces systemic symptoms that extend beyond joint pain:
– Persistent fatigue and low energy levels- Low-grade fevers- Decreased appetite- General malaise and illness feelings- Inflammation in other body systems, including the eyes and heart membrane- Increased risk for serious conditions like lung disease and cardiovascular disease
Affected Joints: Patterns of Distribution
Osteoarthritis Joint Patterns
Osteoarthritis typically develops in weight-bearing joints and joints subjected to repetitive use. Common sites include the knees, hips, spine, neck, and base of the thumbs. In the hands, OA most frequently affects the finger joints closest to the fingernails and the base of the thumb. OA rarely affects the wrist or the back in the way that RA does.
Rheumatoid Arthritis Joint Patterns
Rheumatoid arthritis shows a distinct preference for smaller joints, particularly those in the hands and feet. RA commonly affects the wrists, shoulders, elbows, knees, and ankles. Notably, unlike osteoarthritis, RA tends to spare the spine, making back pain a less typical feature of RA.
Disease Progression: Speed and Timeline
The onset and progression of these conditions differ dramatically. Osteoarthritis develops gradually, often over months or even years. Patients might initially attribute joint discomfort to normal aging or overuse before realizing they have a chronic condition. This slow progression allows for early intervention and lifestyle modifications.
Rheumatoid arthritis develops and worsens rapidly, typically progressing within weeks or a few months. Without proper treatment, RA can cause significant joint damage relatively quickly. This rapid progression underscores the importance of early diagnosis and aggressive treatment to prevent irreversible joint damage.
Risk Factors and Susceptibility
Osteoarthritis Risk Factors
– Advanced age- Previous joint injuries or trauma- Obesity and excess weight- Repetitive joint stress from occupation or sports- Genetic predisposition- Joint misalignment or structural abnormalities
Rheumatoid Arthritis Risk Factors
– Female gender (RA is more common in women)- Family history of autoimmune diseases- Smoking- Genetic susceptibility (specific HLA genes)- Hormonal factors- Environmental exposures
Diagnostic Approaches
Rheumatoid Arthritis Diagnosis
Diagnosing RA typically involves a combination of methods:
Physical Examination: A rheumatologist assesses joint swelling, warmth, range of motion, and symmetrical involvement patterns.
Blood Tests: Specific blood markers help confirm RA diagnosis, including rheumatoid factor (RF) and anti-CCP antibodies. These tests can identify the autoimmune response characteristic of RA.
Imaging Studies: X-rays, MRI scans, and ultrasounds reveal characteristic changes in rheumatoid arthritis. RA typically shows eroded bone and cartilage, narrower spaces between joint bones, and loss of bone around affected joints.
Osteoarthritis Diagnosis
OA diagnosis relies on:
Clinical Assessment: Healthcare providers evaluate pain patterns, joint function, and symptom history.
Imaging Findings: X-rays and other imaging tests show characteristic OA changes including reduced space between bones, bone spurs, cysts, and thickened bone beneath remaining cartilage. These findings reflect the degenerative process rather than inflammatory damage.
Blood Tests: Unlike RA, blood tests are typically normal in OA, as there is no autoimmune component.
Treatment Strategies: Different Approaches
Osteoarthritis Treatment
OA management focuses on pain relief, improving function, and slowing disease progression:
– Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen for pain and mild inflammation- Acetaminophen for pain management- Topical creams and gels- Physical therapy and exercise programs- Weight management to reduce joint stress- Joint protection strategies and assistive devices- Heat and cold therapy- Corticosteroid injections for severe cases- Joint replacement surgery when conservative measures fail
Rheumatoid Arthritis Treatment
RA treatment is more aggressive, targeting the underlying autoimmune process:
– Disease-modifying antirheumatic drugs (DMARDs) to slow disease progression- Biologic agents that target specific immune system components- Nonsteroidal anti-inflammatory drugs (NSAIDs) for symptom relief- Corticosteroids to reduce inflammation and suppress immune responses- Physical therapy and occupational therapy- Lifestyle modifications including rest, exercise, and stress management
Early and aggressive treatment of RA is crucial to prevent irreversible joint damage and systemic complications.
Hand Involvement: Specific Patterns
Hand pain is common in both conditions, but the patterns differ significantly. In osteoarthritis, hand involvement often begins in a single hand, typically affecting the base of the thumb or the finger joints closest to the fingernails. OA may eventually affect both hands, but the initial presentation is often one-sided because OA targets frequently used joints.
Rheumatoid arthritis typically affects both hands symmetrically from the onset. If you experience pain and swelling in the joints of both hands in similar patterns, RA becomes more likely. RA also commonly affects the wrists, whereas OA rarely involves the wrist.
Long-Term Outlook and Progression
The long-term course of these diseases varies considerably. Osteoarthritis is a slowly progressive condition that tends to worsen gradually over time. However, progression rates vary widely among individuals. Some people experience minimal worsening over decades, while others see more rapid functional decline. Modern treatments and lifestyle modifications can help manage symptoms and maintain joint function.
Rheumatoid arthritis, when left untreated, can cause significant disability. The systemic nature of the disease means it can affect multiple organ systems beyond the joints. However, with modern disease-modifying treatments, many RA patients achieve remission or low disease activity, preventing progressive joint damage and preserving function.
When to Seek Medical Attention
Regardless of the type of arthritis, certain warning signs warrant prompt medical evaluation:
– Joint pain lasting more than a few weeks- Symmetric joint swelling affecting both sides of your body- Morning stiffness exceeding 30 minutes- Unexplained systemic symptoms like fatigue and fever accompanying joint pain- Rapid onset of joint symptoms- Visible joint swelling, warmth, or redness
FAQ: Common Questions About OA and RA
Q: Can osteoarthritis develop into rheumatoid arthritis?
A: No, osteoarthritis cannot develop into rheumatoid arthritis. These are distinct diseases with different underlying causes. OA is degenerative while RA is autoimmune. However, a person can develop both conditions simultaneously.
Q: Is rheumatoid arthritis always worse than osteoarthritis?
A: Not necessarily. While RA tends to progress faster and has systemic effects, OA can also cause significant disability, especially when multiple joints are affected. The severity depends on individual disease progression and treatment effectiveness.
Q: Can young people get rheumatoid arthritis?
A: Yes, RA can develop at any age, though it most commonly appears during midlife and is more frequent in women. Young adults with RA require early diagnosis and aggressive treatment to prevent joint damage.
Q: Can lifestyle changes reverse osteoarthritis?
A: While lifestyle changes cannot reverse established OA, they can significantly slow progression and manage symptoms. Weight loss, regular exercise, and joint protection strategies are crucial components of OA management.
Q: What is the difference between arthritis and rheumatism?
A: Rheumatism is not a specific diagnosis but a general term describing rheumatic diseases—a broad category including all types of arthritis and other conditions affecting joints, muscles, tendons, ligaments, and bones. Rheumatic diseases may also involve internal organs in some cases.
Q: Are there preventive measures for these conditions?
A: For osteoarthritis, maintaining a healthy weight, staying physically active, protecting joints from injury, and avoiding excessive repetitive stress can help prevent or delay onset. RA prevention is more complex due to genetic factors, though smoking cessation and maintaining overall health may reduce risk.
Conclusion: Getting an Accurate Diagnosis
Distinguishing between osteoarthritis and rheumatoid arthritis is essential for receiving appropriate treatment and managing your condition effectively. While both cause joint pain and stiffness, their fundamentally different causes—degenerative wear and tear versus autoimmune inflammation—require different therapeutic approaches. By understanding the key differences in symptom patterns, disease progression, affected joints, and systemic effects, you can better communicate with healthcare providers about your symptoms and concerns. Early diagnosis, particularly for rheumatoid arthritis, can prevent irreversible joint damage and systemic complications. If you experience persistent joint pain, morning stiffness, or symmetric joint involvement, consult a healthcare provider or rheumatologist for proper evaluation and diagnosis. With accurate diagnosis and appropriate treatment tailored to your specific condition, most people with arthritis can manage pain effectively and maintain good quality of life.
References
- Osteoarthritis vs. Rheumatoid Arthritis: Symptom Differences — MyRaTeam. 2024. https://www.myrateam.com/resources/osteoarthritis-vs-rheumatoid-arthritis-are-they-one-and-the-same
- Rheumatoid Arthritis vs Osteoarthritis: What’s the Difference? — WebMD. 2024. https://www.webmd.com/rheumatoid-arthritis/rheumatoid-arthritis-osteoarthritis-difference
- Osteoarthritis: Causes, Symptoms, and Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/5599-osteoarthritis
- Rheumatoid Arthritis Overview — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/rheumatoid-arthritis/symptoms-causes/syc-20353648
- Autoimmune Disorders: Understanding the Immune System — National Institute of Allergy and Infectious Diseases (NIAID). 2024. https://www.niaid.nih.gov/
- Joint Pain and Arthritis Management Guidelines — American College of Rheumatology. 2024. https://www.rheumatology.org/
Read full bio of medha deb











