Osteoarthritis Symptoms: Signs, Causes, and Management
Understanding osteoarthritis symptoms: Pain, stiffness, and treatments for better joint health.
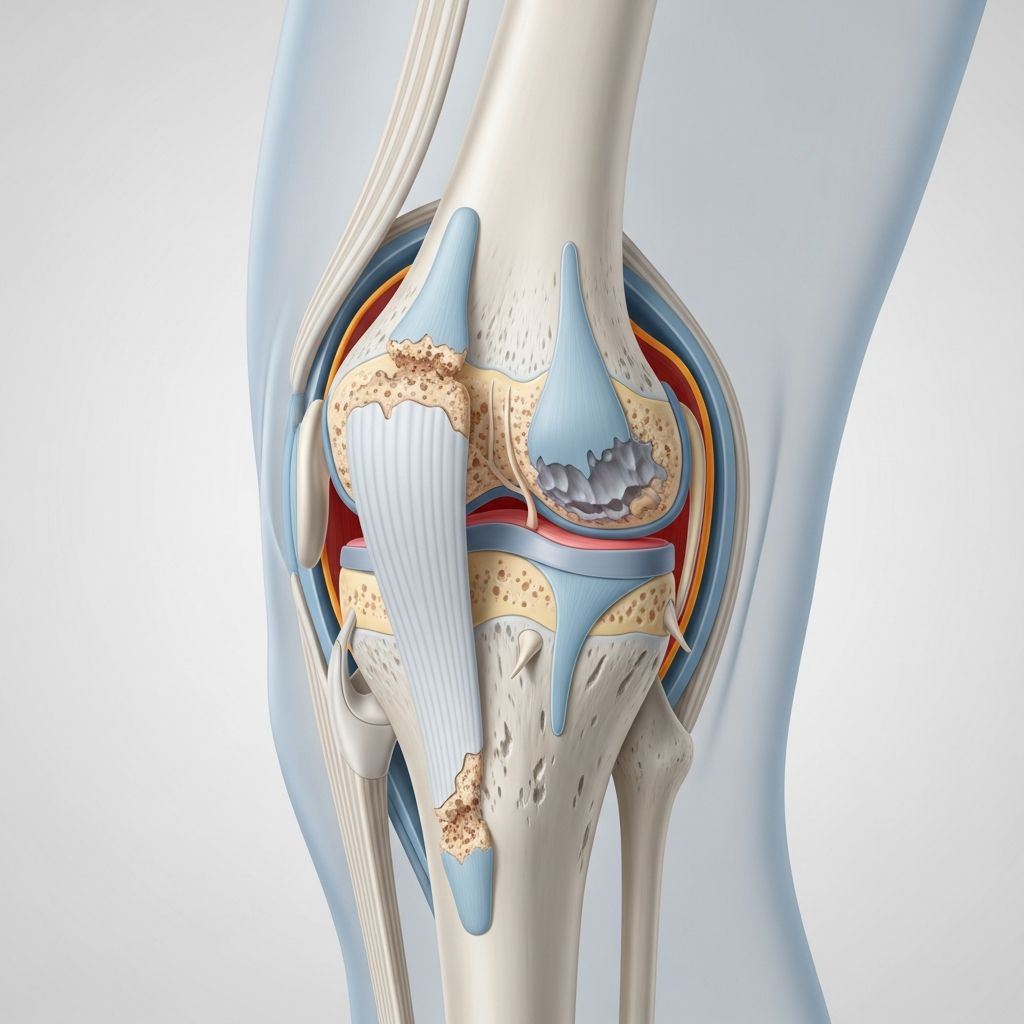
Understanding Osteoarthritis and Its Symptoms
Osteoarthritis is the most common form of arthritis, affecting millions of people worldwide. It occurs when the protective cartilage that cushions the ends of bones gradually wears down over time. Unlike other types of arthritis, osteoarthritis is non-inflammatory, meaning it doesn’t involve the immune system attacking the joints. While the condition can affect any joint, it most commonly impacts the hands, knees, hips, and spine.
The hallmark characteristic of osteoarthritis is the progressive breakdown of joint cartilage and the underlying bone, leading to pain, stiffness, and reduced mobility. Although osteoarthritis symptoms cannot be reversed once cartilage damage occurs, staying active, maintaining a healthy weight, and receiving appropriate treatments can slow disease progression and improve pain management.
Common Osteoarthritis Symptoms
Osteoarthritis symptoms typically develop slowly and worsen over time. Recognizing these early signs allows individuals to seek treatment and implement lifestyle modifications to manage the condition more effectively.
Primary Symptoms
- Pain: Affected joints may hurt during or after movement, particularly with weight-bearing activities.
- Stiffness: Joint stiffness is often most noticeable upon awakening or after extended periods of inactivity. This may improve gradually throughout the day as the joint warms up.
- Tenderness: Joints may feel tender when pressure is applied directly or to the surrounding area.
- Loss of Flexibility: Individuals may experience restricted range of motion, unable to move the joint through its complete normal movement pattern.
- Grating Sensation: Some people experience a grating or grinding sensation during joint movement, sometimes accompanied by popping or crackling sounds (crepitus).
Secondary Symptoms
- Bone Spurs: The body may develop extra bony growths (osteophytes) that feel like hard lumps around the affected joint.
- Swelling: Inflammation of the soft tissue surrounding the joint may cause visible swelling.
- Bony Enlargement: Joints may appear enlarged due to bone spur formation, particularly noticeable in the hands.
Osteoarthritis by Joint Location
Osteoarthritis symptoms and progression vary depending on which joints are affected. Understanding location-specific symptoms helps with early diagnosis and targeted management.
Hand Osteoarthritis
Hand osteoarthritis is particularly common, especially in women. Symptoms include bony enlargements in the joints nearest the fingertips and middle knuckles, creating a characteristic “knobby” appearance. Many individuals experience difficulty with fine motor tasks such as buttoning clothes, writing, or gripping objects.
Knee Osteoarthritis
The knees are among the most commonly affected joints due to their weight-bearing role. Knee osteoarthritis often produces crepitus (crackling sensations) and can significantly impact walking, stair climbing, and other daily activities.
Hip Osteoarthritis
Hip osteoarthritis causes pain during movement and can restrict hip mobility. This condition often affects activities such as walking, sitting, and climbing stairs.
Spine Osteoarthritis
In the spine, osteoarthritis leads to disk narrowing and bone spur formation. This may cause neck or lower back pain and, in some cases, nerve compression symptoms.
Risk Factors for Developing Osteoarthritis
Several factors increase the likelihood of developing osteoarthritis. Understanding these risk factors allows individuals to take preventive measures.
Non-Modifiable Risk Factors
- Age: Osteoarthritis risk increases significantly with advancing age.
- Sex: People assigned female at birth are more likely to develop osteoarthritis, though the exact reasons remain unclear.
- Genetics: Some individuals inherit a genetic predisposition to osteoarthritis.
- Bone Deformities: Being born with malformed joints or defective cartilage increases vulnerability.
Modifiable Risk Factors
- Obesity: Excess body weight contributes to osteoarthritis development in multiple ways. Added weight increases stress on weight-bearing joints like the hips and knees. Additionally, fat tissue produces proteins that promote harmful inflammation in and around joints.
- Joint Injuries: Past injuries from sports, accidents, or trauma can increase osteoarthritis risk, even if the injury occurred years ago.
- Repetitive Stress: Occupations or sports involving repetitive joint stress may lead to osteoarthritis development over time.
- Certain Metabolic Diseases: Conditions such as diabetes and hemochromatosis (excessive iron accumulation) increase osteoarthritis risk.
The Progression of Osteoarthritis
Osteoarthritis is a progressive disease that worsens over time. The condition extends beyond simple cartilage wear, affecting the entire joint structure. As cartilage deteriorates, changes occur in the underlying bone, and the strong connective tissues holding the joint together weaken. In advanced cases where cartilage completely wears away, bone may rub directly against bone, causing significant pain and dysfunction.
Impact on Daily Life and Complications
Osteoarthritis can profoundly affect quality of life. Joint pain and stiffness may become severe enough to make routine tasks difficult. For people with hand osteoarthritis, simple activities like opening jars, typing, or dressing become challenging. The chronic pain associated with osteoarthritis can lead to secondary complications including depression and sleep disturbances, which further impact overall health and well-being.
When to Seek Medical Attention
If joint pain or stiffness persists and doesn’t resolve with rest or over-the-counter remedies, consulting a healthcare professional is essential. Early diagnosis allows for timely intervention and management strategies to slow progression and maintain mobility.
Management and Treatment Approaches
While osteoarthritis damage cannot be reversed, multiple treatment approaches can effectively manage symptoms. The treatment goals focus on reducing pain and stiffness while maintaining joint function. Management strategies often include a combination of physical activity, weight management, and medical treatments. Staying active is particularly important—research shows that exercise helps reduce symptoms, though individuals should listen to their bodies and stop if they experience pain or discomfort.
Frequently Asked Questions About Osteoarthritis
Q: Can osteoarthritis be prevented?
A: While osteoarthritis cannot be completely prevented, especially given genetic and age-related factors, maintaining a healthy weight, staying physically active, protecting joints from injury, and avoiding repetitive stress can significantly reduce your risk.
Q: Is osteoarthritis the same as rheumatoid arthritis?
A: No. Osteoarthritis is a non-inflammatory degenerative joint disease caused by cartilage wear, while rheumatoid arthritis is an inflammatory autoimmune condition. They have different causes, progression patterns, and treatment approaches.
Q: How is osteoarthritis diagnosed?
A: Diagnosis typically involves a medical history, physical examination, and imaging tests such as X-rays to assess cartilage and bone changes. Blood tests may also help rule out other types of arthritis.
Q: Can exercise help osteoarthritis?
A: Yes. Regular physical activity helps reduce symptoms, maintain mobility, and improve overall function. However, it’s important to exercise within your pain tolerance and consult with a healthcare provider about appropriate exercise types.
Q: What lifestyle changes can help manage osteoarthritis?
A: Weight loss (if overweight), regular low-impact exercise, joint protection strategies, heat and cold therapy, and adequate rest between activities all help manage symptoms.
Q: Are there different types of osteoarthritis treatments?
A: Treatment options include lifestyle modifications, physical therapy, over-the-counter and prescription medications, injections, and in some cases, surgical interventions. Treatment plans are individualized based on symptom severity and joint involvement.
References
- Osteoarthritis – Symptoms & Causes — Mayo Clinic. 2025-04-08. https://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes/syc-20351925
- Osteoarthritis: Symptoms, Risk Factors, Diagnosis, and Treatment — Mass General Brigham (Marcy Bolster, M.D., Rheumatologist, Harvard Medical School). 2022-04-08. https://www.youtube.com/watch?v=Rgtl97yO5ec
Read full bio of Sneha Tete











