Osteoarthritis: Symptoms, Causes and Treatment
Comprehensive guide to understanding and managing osteoarthritis with expert treatment options.
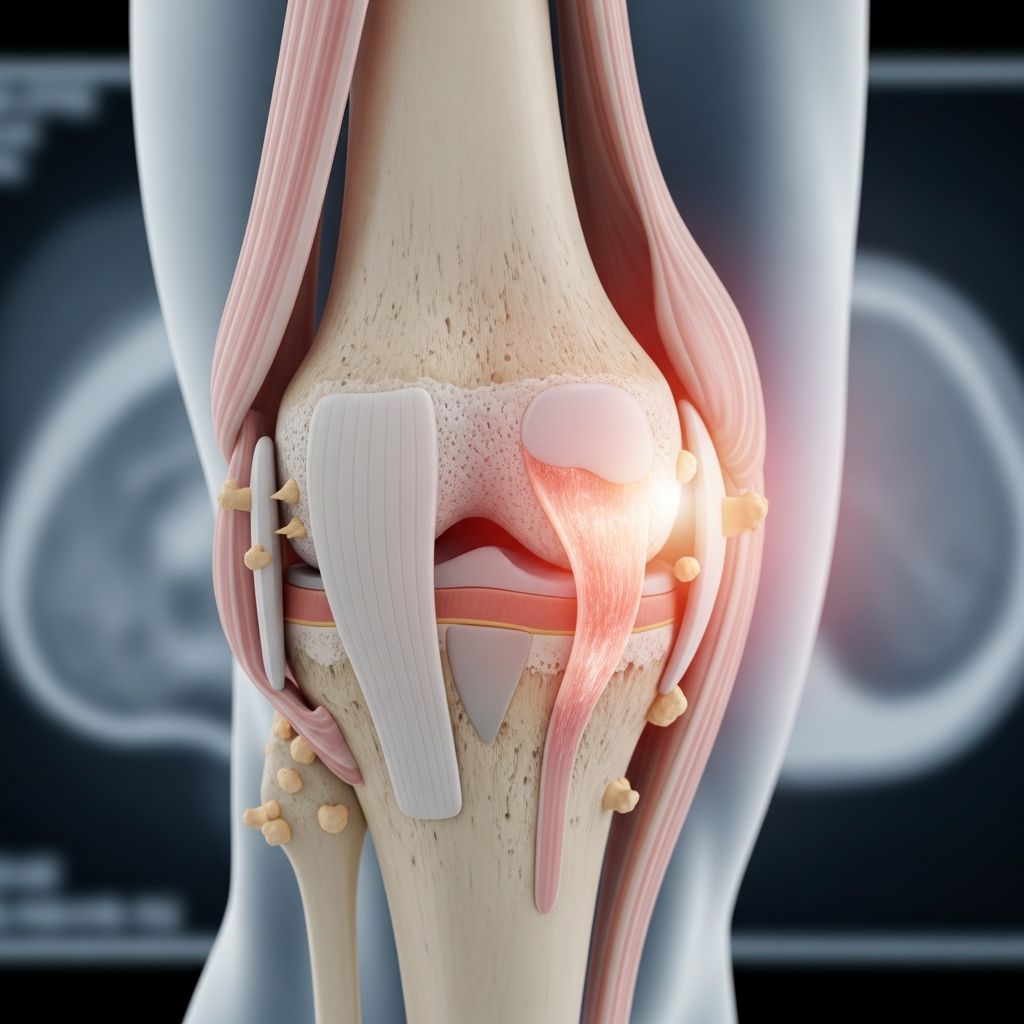
Understanding Osteoarthritis: A Comprehensive Guide
Osteoarthritis is the most common type of arthritis affecting millions of people worldwide. This degenerative joint disease occurs when the protective cartilage that lines your joints gradually wears down, causing your bones to rub directly against each other. Unlike other forms of arthritis that result from autoimmune conditions or infections, osteoarthritis develops over time through wear and tear on the joints. While it is a chronic condition with no cure, various treatment options can help manage symptoms, reduce pain, and maintain your quality of life. Understanding the condition, its progression, and available treatments empowers you to take an active role in managing your health.
What Is Osteoarthritis?
Osteoarthritis, often referred to as OA, is a progressive degenerative disease affecting the joints throughout your body. The condition develops when the cartilage—the smooth, slippery tissue covering the ends of bones where they meet in joints—breaks down over time. Cartilage serves critical functions: it provides cushioning between bones, allows smooth movement, and absorbs shock when you place weight on your joints. As cartilage deteriorates, these protective functions diminish, leading to pain, stiffness, inflammation, and reduced mobility.
The hallmark characteristic of osteoarthritis is its progressive nature. Once cartilage is damaged, it cannot regenerate or repair itself naturally. This means the condition typically worsens gradually over months and years. However, the rate of progression varies significantly from person to person, depending on numerous factors including age, genetics, joint usage patterns, and overall health status. While osteoarthritis is a lifelong condition, modern treatment approaches focus on slowing progression and managing symptoms effectively.
Symptoms of Osteoarthritis
Osteoarthritis symptoms develop gradually and vary in severity depending on which joints are affected and the stage of the disease. Common symptoms include:
- Joint pain and aching, particularly during or after physical activity
- Stiffness in joints, especially after periods of rest or inactivity
- Swelling and inflammation around affected joints
- Reduced range of motion and flexibility
- Tenderness when applying pressure to the joint
- Cracking or popping sounds when moving joints
- Bone spurs or hard lumps forming around affected joints
- Weakness in muscles surrounding the joint
Symptoms often worsen with activity and improve with rest, though some people experience pain even at rest during advanced stages. Weather changes, particularly cold and damp conditions, may intensify symptoms for some individuals. Pain intensity can fluctuate from day to day, making consistent symptom management important for maintaining daily functioning.
Causes and Risk Factors
Osteoarthritis develops through a combination of factors, rather than a single identifiable cause. Understanding these risk factors helps you assess your personal risk and take preventive measures when possible.
Primary Risk Factors
Age: The risk of developing osteoarthritis increases significantly with age. Most people diagnosed with OA are over 45 years old, though the condition can develop in younger individuals under certain circumstances.
Genetics: Family history plays a substantial role in osteoarthritis development. If your parents or siblings have OA, your risk is considerably higher.
Joint Injuries: Previous injuries to joints, including fractures, ligament tears, or cartilage damage, significantly increase the likelihood of developing osteoarthritis in that joint later in life.
Repetitive Stress: Occupations or activities requiring repeated joint movements place excessive stress on cartilage, accelerating wear and tear.
Obesity: Excess body weight increases pressure on weight-bearing joints like the knees, hips, and feet, accelerating cartilage degradation.
Gender: Women are more likely to develop osteoarthritis than men, particularly after menopause, possibly due to hormonal changes affecting cartilage health.
Muscle Weakness: Weak muscles surrounding joints fail to provide adequate support and stabilization, placing additional stress on cartilage.
Diagnosis of Osteoarthritis
Diagnosing osteoarthritis typically involves a multi-step approach combining clinical evaluation with imaging studies. Your healthcare provider will begin by reviewing your medical history and discussing your symptoms in detail. This conversation helps establish when symptoms began, which activities trigger pain, and how the condition affects your daily life.
Physical Examination
During the physical examination, your healthcare provider will:
- Inspect the affected joint for swelling, redness, or deformity
- Gently move the joint through its full range of motion to assess flexibility and identify pain triggers
- Apply pressure to the joint to evaluate tenderness
- Check muscle strength in the surrounding areas
- Assess joint stability and alignment
Imaging Tests
X-rays: X-rays are typically the first imaging study ordered for suspected osteoarthritis. They reveal the joint space, bone structure, and signs of cartilage loss, including bone spurs and joint narrowing characteristic of OA.
MRI (Magnetic Resonance Imaging): MRI provides detailed images of soft tissues, cartilage, ligaments, and tendons. It’s particularly useful for assessing cartilage quality and identifying early-stage disease when X-rays may appear normal.
CT (Computed Tomography) Scan: CT scans offer three-dimensional images of the joint, helping your provider visualize complex joint anatomy when detailed structural information is necessary.
No blood tests specifically diagnose osteoarthritis, though blood work may rule out other conditions like rheumatoid arthritis or lupus that cause similar symptoms.
Treatment Options for Osteoarthritis
Osteoarthritis treatment is highly individualized, taking into account your age, overall health, the severity of your condition, and how significantly symptoms impact your daily activities. Healthcare providers typically employ a progressive approach, starting with conservative treatments and advancing to more intensive interventions only when necessary.
Nonsurgical Treatments
Lifestyle Modifications: Maintaining a healthy weight reduces stress on weight-bearing joints. Regular, low-impact exercise like swimming, walking, or cycling strengthens supporting muscles and improves joint flexibility. Applying heat to stiff joints or ice to swollen joints provides symptom relief. Additionally, using proper body mechanics during daily activities prevents unnecessary joint stress.
Physical and Occupational Therapy: Physical therapists design customized exercise programs that strengthen muscles around affected joints, improve flexibility, and enhance overall function. Occupational therapists suggest modifications to your home and work environment, recommend assistive devices, and teach adaptive techniques for performing daily tasks more comfortably.
Medications: Over-the-counter pain relievers like acetaminophen provide mild symptom relief. Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen reduce both pain and inflammation. Topical creams and gels containing NSAIDs or capsaicin provide localized relief. Prescription medications may be necessary for more severe pain.
Injections: Corticosteroid injections delivered directly into the joint reduce inflammation and provide temporary pain relief lasting weeks to months. Hyaluronic acid injections supplement the natural fluid within joints, improving lubrication and reducing pain. Platelet-rich plasma (PRP) and other biologic treatments show promise in some cases by promoting tissue repair.
Assistive Devices: Braces and supports stabilize joints and reduce pain during activity. Canes, walkers, or crutches reduce weight-bearing stress on affected lower-extremity joints. Specialized shoes or shoe inserts improve alignment and reduce joint strain.
Surgical Treatments
When conservative treatments no longer adequately manage symptoms, surgical interventions may become necessary:
Arthroscopy: This minimally invasive procedure involves inserting a small camera into the joint to visualize internal structures, remove loose cartilage fragments, and smooth rough cartilage surfaces.
Osteotomy: This surgical procedure realigns bones to redistribute weight away from the damaged cartilage area, reducing pain and slowing disease progression.
Joint Replacement: When osteoarthritis severely damages the joint, replacement with an artificial prosthetic provides significant pain relief and restores function. This is particularly common for hip and knee replacements.
Living with Osteoarthritis
Successfully managing osteoarthritis requires ongoing commitment to treatment and lifestyle adjustments. Most people with OA need to manage their condition throughout their lives, adapting their approach as the disease progresses. Staying physically active remains crucial, as sedentary lifestyles increase the risk of serious health conditions including heart disease, diabetes, and certain cancers.
Your daily routine may require modifications depending on symptom severity and triggers. You might need to adjust work responsibilities, modify exercise routines, or change how you perform household tasks. These adaptations are temporary adjustments, not permanent limitations. As treatment options improve symptom control, you can often resume more activities.
Prevention and Risk Reduction
While you cannot entirely prevent osteoarthritis, particularly if you have genetic predisposition or previous joint injuries, you can reduce your risk through several strategies:
- Maintain a healthy weight to reduce stress on weight-bearing joints
- Engage in regular, moderate-intensity exercise to strengthen muscles and maintain joint flexibility
- Use proper body mechanics during work and daily activities to minimize joint strain
- Warm up before exercise and cool down afterward
- Protect joints from injury by using appropriate protective equipment during activities
- Manage other health conditions like diabetes and heart disease
- Avoid smoking and limit alcohol consumption
- Maintain good posture to reduce unnecessary stress on joints
- Take breaks during repetitive activities to prevent overuse injuries
When to Seek Medical Attention
Contact your healthcare provider if you experience persistent joint pain lasting more than a few weeks, significant swelling or stiffness, reduced range of motion that affects daily activities, or if pain interferes with sleep or work. Early diagnosis and treatment intervention can slow disease progression and prevent further joint damage. Don’t wait until the condition severely impacts your quality of life to seek professional help.
Frequently Asked Questions
Q: Is osteoarthritis curable?
A: No, osteoarthritis is not curable because damaged cartilage cannot regenerate. However, various treatments can effectively manage symptoms, slow progression, and maintain quality of life.
Q: Can young people develop osteoarthritis?
A: Yes, though less common, osteoarthritis can develop in younger individuals, particularly following joint injuries or due to genetic predisposition.
Q: How quickly does osteoarthritis progress?
A: Progression rates vary significantly between individuals. Some people experience slow progression over decades, while others progress more rapidly. Factors like age, weight, activity level, and genetics influence progression speed.
Q: Is exercise beneficial for osteoarthritis?
A: Yes, regular moderate exercise strengthens supporting muscles, improves flexibility, and reduces pain. Low-impact activities like swimming, walking, and cycling are particularly beneficial.
Q: What is the best treatment for osteoarthritis?
A: The best treatment is individualized and often involves a combination of approaches including lifestyle modifications, physical therapy, medications, and sometimes injections or surgery, depending on severity and patient preferences.
Q: Can weight loss help osteoarthritis?
A: Yes, maintaining a healthy weight significantly reduces stress on weight-bearing joints, can slow disease progression, and often reduces pain and improves mobility.
References
- Osteoarthritis: Symptoms, Causes and Treatment — Cleveland Clinic. 2023-10-02. https://my.clevelandclinic.org/health/diseases/5599-osteoarthritis
- Knee Osteoarthritis: Symptoms, Stages, Causes & Treatment — Cleveland Clinic. 2025-01-30. https://my.clevelandclinic.org/health/diseases/21750-osteoarthritis-knee
- Osteoarthritis Treatment — Cleveland Clinic. https://my.clevelandclinic.org/services/osteoarthritis-treatment
- Rheumatoid Arthritis & Osteoarthritis Center — Cleveland Clinic. https://my.clevelandclinic.org/departments/orthopaedics-rheumatology/depts/arthritis-musculoskeletal
Read full bio of medha deb











