Osteoarthritis vs. Rheumatoid Arthritis: Key Differences
Understanding the distinctions between OA and RA for better joint health management.
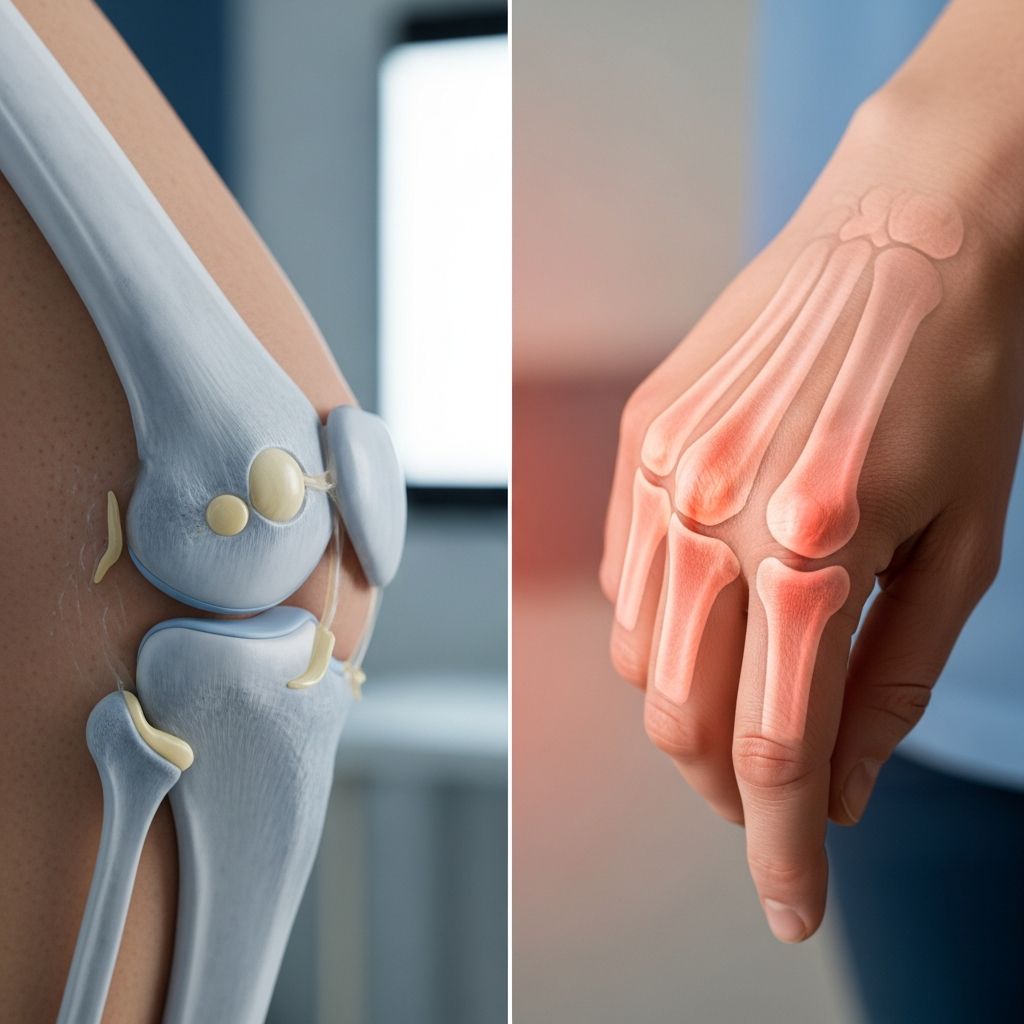
Understanding Osteoarthritis vs. Rheumatoid Arthritis
Arthritis is a common condition affecting millions of people worldwide, but not all arthritis is the same. Two of the most prevalent types—osteoarthritis (OA) and rheumatoid arthritis (RA)—are often confused due to overlapping symptoms. However, they are fundamentally different diseases with distinct causes, progression patterns, and treatment approaches. Understanding these differences is crucial for obtaining an accurate diagnosis and receiving appropriate care.
What is Osteoarthritis?
Osteoarthritis is a degenerative joint disease characterized by the gradual breakdown of cartilage that cushions the joints. Often referred to as “wear-and-tear” arthritis, OA develops over time as the protective cartilage deteriorates, eventually leading to bone-on-bone contact and pain. This condition is the most common form of arthritis, affecting approximately 32.5 million people in the United States alone.
Unlike rheumatoid arthritis, osteoarthritis is not an autoimmune disease. Instead, it results from mechanical stress on the joints combined with factors such as age, previous injuries, obesity, and genetic predisposition. The disease typically develops slowly over many years and is most common in older adults, though it can occur at any age depending on risk factors.
What is Rheumatoid Arthritis?
Rheumatoid arthritis is an autoimmune disease in which the body’s immune system mistakenly attacks healthy joint tissue. Specifically, the immune system targets the synovial membrane—the lining that lubricates and protects joints—causing inflammation and pain. Unlike osteoarthritis, RA is a systemic condition that can affect multiple organs beyond just the joints, leading to widespread inflammation throughout the body.
RA can develop at any age but most commonly appears between ages 30 and 60. Women are three times more likely to develop RA than men, and risk factors include genetics, smoking, and environmental triggers. The disease tends to develop and progress quickly, sometimes causing permanent joint damage if left untreated.
Key Differences Between OA and RA
Root Cause
The fundamental difference between these two conditions lies in their origins. Osteoarthritis results from wear and tear on the joints over a lifetime, destroying cartilage through mechanical stress. In contrast, rheumatoid arthritis stems from an autoimmune response where the body’s immune system attacks joint tissues as if they were foreign invaders. This distinction is crucial because it determines treatment strategies and disease progression.
Symptom Patterns
While both conditions cause joint pain and stiffness, they manifest differently:
Osteoarthritis Symptoms:
- Asymmetrical joint pain affecting one side of the body more than the other
- Brief morning stiffness lasting less than 30 minutes
- Localized joint symptoms without systemic effects
- Joint noises such as cracking or grinding when moving
- Reduced joint stability and flexibility
- Bone spurs developing around affected joints
- Pain primarily in weight-bearing joints like knees, hips, and spine
Rheumatoid Arthritis Symptoms:
- Symmetrical joint pain affecting the same joints on both sides of the body
- Morning stiffness lasting more than one hour
- Systemic symptoms including fatigue, low-grade fever, and malaise
- Warm, tender, and visibly swollen joints
- Symptoms often beginning in smaller joints like fingers, wrists, and toes
- Potential development of rheumatoid nodules under the skin
- Low appetite and anemia
- Joints becoming forced into bent positions over time
Disease Progression
Osteoarthritis develops slowly over many years, and progression varies based on individual factors such as activity level and joint stress. In contrast, rheumatoid arthritis can develop and progress rapidly, sometimes causing irreversible joint damage within months if untreated. This difference in progression speed emphasizes the importance of early diagnosis and aggressive treatment for RA.
Joint Distribution
Rheumatoid arthritis is symmetrical, typically affecting corresponding joints on both sides of the body simultaneously. Osteoarthritis, conversely, is asymmetrical and usually begins in an isolated joint, often affecting only one side of the body. This pattern distinction is one of the clearest diagnostic indicators doctors use to differentiate between the two conditions.
Age and Risk Factors
Osteoarthritis Risk Factors
Osteoarthritis is more common with advancing age, typically developing after age 50. Key risk factors include:
- Previous joint injuries or trauma
- Obesity and excess body weight
- Genetic predisposition
- Repetitive joint use from occupations or sports
- Older age and female sex
Rheumatoid Arthritis Risk Factors
While RA can develop at any age, it most commonly appears between ages 30 and 60. Notable risk factors include:
- Genetic factors and family history
- Smoking and tobacco exposure
- Environmental triggers
- Female sex (three times more common in women)
- Ethnicity (more common in Black populations)
Diagnosis Methods
Diagnosing Rheumatoid Arthritis
Accurate diagnosis of RA requires comprehensive evaluation including:
- Blood tests for rheumatoid factor (RF) and anti-CCP antibodies
- Inflammatory markers such as ESR and CRP
- Complete physical examination assessing joint pain and swelling
- Imaging studies including X-rays and MRI to assess joint damage
Diagnosing Osteoarthritis
Osteoarthritis diagnosis typically involves:
- Physical examination and detailed medical history
- X-rays showing joint space narrowing and bone changes
- MRI for detailed cartilage assessment when necessary
- Blood tests to rule out other conditions like rheumatoid arthritis
Treatment Approaches
Rheumatoid Arthritis Treatment
RA treatment focuses on controlling inflammation and preventing permanent joint damage through aggressive intervention:
- Disease-modifying antirheumatic drugs (DMARDs)
- Biologic medications targeting immune system components
- Anti-inflammatory medications to reduce swelling
- Physical therapy and exercise programs
- Lifestyle modifications including stress management
Osteoarthritis Treatment
OA management emphasizes pain management and maintaining joint function:
- Over-the-counter and prescription pain relievers
- Anti-inflammatory medications
- Physical therapy and regular exercise
- Weight management and lifestyle changes
- Joint injections such as corticosteroids when appropriate
- Surgery in severe cases where conservative treatments fail
Comparison Table: OA vs. RA
| Characteristic | Osteoarthritis | Rheumatoid Arthritis |
|---|---|---|
| Disease Type | Degenerative | Autoimmune |
| Root Cause | Wear and tear | Immune system attacks joints |
| Onset Age | After age 50 | Ages 30-60 |
| Joint Pattern | Asymmetrical | Symmetrical |
| Morning Stiffness | Less than 30 minutes | More than 1 hour |
| Systemic Symptoms | None | Fatigue, fever, malaise |
| Primary Joints Affected | Weight-bearing (knees, hips) | Small joints (fingers, wrists) |
| Disease Progression | Slow over years | Rapid progression |
Why Proper Diagnosis Matters
Obtaining an accurate diagnosis is essential because these conditions require fundamentally different treatment approaches. Rheumatoid arthritis requires aggressive, early intervention to prevent permanent joint damage and systemic complications. Osteoarthritis management, by contrast, focuses on symptom relief, pain management, and maintaining mobility and function. A misdiagnosis can delay appropriate treatment, potentially leading to unnecessary joint damage and complications. Healthcare providers use the distinct symptom patterns, diagnostic tests, and risk factor profiles to differentiate between these conditions accurately.
Can You Have Both Conditions?
While uncommon, it is possible for individuals to have both osteoarthritis and rheumatoid arthritis simultaneously. This situation requires careful management and individualized treatment plans that address both conditions’ unique needs. Patients with both conditions should work closely with rheumatologists to ensure comprehensive care addressing all aspects of their arthritis.
Frequently Asked Questions
Q: What is the main difference between osteoarthritis and rheumatoid arthritis?
A: The primary difference is the cause. Osteoarthritis results from mechanical wear and tear on joints over time, while rheumatoid arthritis is an autoimmune disease where the immune system attacks joint tissue.
Q: Which type of arthritis is more common?
A: Osteoarthritis is significantly more common, affecting approximately 32.5 million Americans. Rheumatoid arthritis affects about one-tenth as many people as osteoarthritis.
Q: At what age do these conditions typically develop?
A: Osteoarthritis typically develops after age 50, while rheumatoid arthritis most commonly appears between ages 30 and 60, though both can occur at any age.
Q: How are these conditions diagnosed differently?
A: RA diagnosis involves blood tests for antibodies and inflammatory markers, while OA diagnosis relies on physical examination, X-rays, and sometimes MRI imaging to assess joint changes.
Q: Can morning stiffness help distinguish between the two conditions?
A: Yes. Rheumatoid arthritis causes prolonged morning stiffness lasting more than one hour, while osteoarthritis typically causes brief stiffness lasting less than 30 minutes.
Q: Are the treatment approaches different for these conditions?
A: Yes, significantly. RA treatment focuses on controlling inflammation and preventing joint damage using DMARDs and biologic medications. OA treatment emphasizes pain management, physical therapy, and weight management.
Q: Which arthritis type progresses more quickly?
A: Rheumatoid arthritis can progress rapidly and cause permanent joint damage, while osteoarthritis develops slowly over many years.
Q: What joints are typically affected by each condition?
A: Osteoarthritis commonly affects weight-bearing joints like knees, hips, and the spine, while rheumatoid arthritis typically begins in smaller joints like fingers, wrists, and toes.
References
- Rheumatoid Arthritis vs Osteoarthritis: Key Differences — MidAtlantic Rheumatology. 2024. https://www.midatlanticrheum.com/rheumatoid-arthritis-vs-osteoarthritis/
- Rheumatoid Arthritis vs Osteoarthritis: What’s the Difference? — WebMD. 2024. https://www.webmd.com/rheumatoid-arthritis/rheumatoid-arthritis-osteoarthritis-difference
- How Osteoarthritis and Rheumatoid Arthritis Differ — Michigan Medicine. 2024. https://www.michiganmedicine.org/health-lab/how-osteoarthritis-and-rheumatoid-arthritis-differ
- Rheumatoid Arthritis Vs. Osteoarthritis — Summit Rheumatology. 2024. https://summitrheumatology.com/patient-lifestyle/rheumatoid-arthritis-vs-osteoarthritis/
- Comparing Rheumatoid Arthritis and Osteoarthritis — MyHealth Alberta. 2024. https://myhealth.alberta.ca/Health/pages/conditions.aspx?hwid=aa19377
- A comparison of risk factors for osteo- and rheumatoid arthritis using NHANES data — National Center for Biotechnology Information. 2020. https://pmc.ncbi.nlm.nih.gov/articles/PMC7689317/
Read full bio of Sneha Tete











