Osteopenia: Understanding Bone Density Loss
Learn about osteopenia, its causes, symptoms, diagnosis, and treatment options for healthier bones.
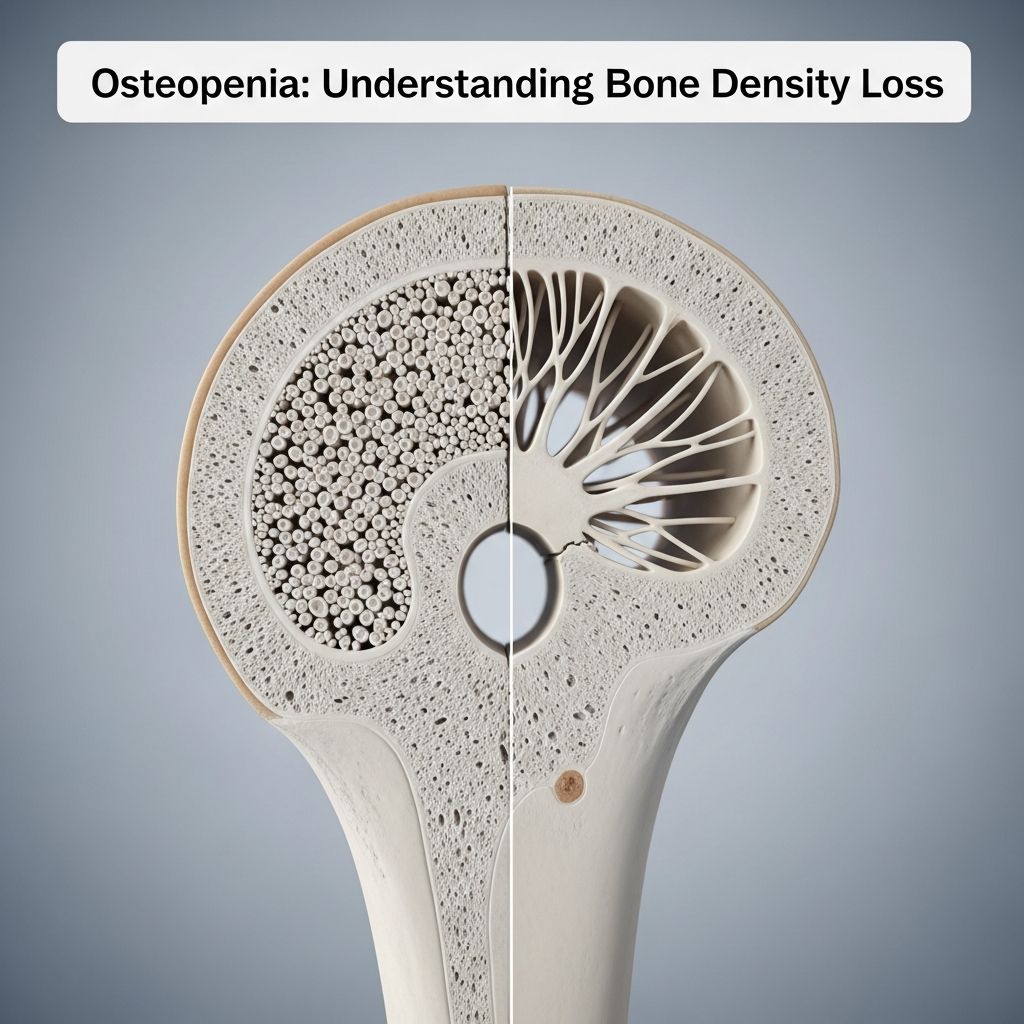
Understanding Osteopenia: A Guide to Bone Density Loss
Osteopenia is a medical condition characterized by a loss of bone density, meaning your bones contain less mineral content than they should. This reduction in mineral density makes your bones weaker and more susceptible to fractures, even from minor falls or injuries. While osteopenia is often referred to as a precursor to osteoporosis, it is important to understand that having osteopenia does not necessarily mean you will develop osteoporosis. Early detection and proper management can significantly slow bone loss and, in many cases, prevent the progression to more severe bone disease.
Bone density naturally decreases as we age, but several factors can accelerate this process. Understanding osteopenia, its causes, and available treatment options is crucial for maintaining long-term bone health and preventing serious fractures.
What Is Osteopenia?
Osteopenia is the medical term for reduced bone mineral density (BMD). When you have osteopenia, your bones are less dense than they should be, but not so severely weakened that they fracture easily like in osteoporosis. Think of bone density as a measure of how tightly packed the minerals and other components are within your bone structure. The denser your bones, the stronger they are and the more resistant they are to breaking.
Your bones are living tissues that constantly undergo remodeling—old bone is broken down and new bone is formed. During childhood and young adulthood, new bone is added faster than old bone is removed, so your bone mass increases. Most people reach their peak bone mass around age 30. After that, bone remodeling continues, but you lose slightly more bone mass than you gain.
Osteopenia represents an intermediate stage between normal bone density and osteoporosis. It serves as an important warning sign that your bones are becoming weaker and that you need to take steps to prevent further bone loss.
Osteopenia vs. Osteoporosis: Understanding the Difference
Osteopenia and osteoporosis are closely related conditions, but they differ significantly in severity and their effects on bone health. Understanding the distinction between these two conditions is essential for appropriate treatment and management.
Osteopenia is characterized by bone density that is lower than normal but not low enough to be classified as osteoporosis. In osteopenia, bones are weaker than healthy bones, but the reduction in density is less severe. People with osteopenia have an increased risk of fractures, but the risk is considerably lower than those with osteoporosis.
Osteoporosis is a more advanced stage of bone loss where bone density becomes severely reduced. Osteoporosis silently weakens your bones to the point where even minor falls, bumps, or coughs can cause fractures. The bones become so fragile that they may break spontaneously. Osteoporosis often develops without symptoms until a fracture occurs.
The key difference is that osteopenia is reversible or can be halted with appropriate intervention, while osteoporosis requires more aggressive treatment. This is why early detection of osteopenia is so valuable—it gives you the opportunity to prevent progression to osteoporosis through lifestyle modifications and, when necessary, medication.
Who Is at Risk for Osteopenia?
While anyone can develop osteopenia, certain groups of people are at higher risk for developing this condition. Understanding your risk factors can help you take preventive measures and seek appropriate screening.
Age and Gender: Women, especially postmenopausal women, face significantly higher risk for osteopenia and osteoporosis. The decline in estrogen levels after menopause accelerates bone loss. Men can also develop osteopenia, but it typically occurs later in life as testosterone levels decline. Most women should have bone density screenings regularly after age 50, while men typically need screening after age 70.
Family History: If you have a family history of osteoporosis or osteopenia, your risk is substantially increased. Genetic factors play an important role in determining peak bone mass and bone loss rates.
Body Frame Size: People with smaller body frames have less bone mass to draw from as they age, increasing their risk of developing osteopenia.
Lifestyle Factors: Sedentary lifestyles, smoking, excessive alcohol consumption, and inadequate calcium and vitamin D intake all contribute to increased osteopenia risk.
Health Conditions That Increase Osteopenia Risk
Several medical conditions can lower your bone density or worsen existing osteopenia:
- Thyroid disorders and hyperparathyroidism
- Digestive disorders affecting nutrient absorption (celiac disease, Crohn’s disease)
- Chronic kidney disease
- Rheumatoid arthritis
- Multiple myeloma and other blood cancers
- Hormonal conditions affecting calcium metabolism
- Eating disorders that limit nutrition
Medications That Increase Osteopenia Risk
Certain medications can increase your risk of developing osteopenia or accelerate bone loss:
- Corticosteroids (used for conditions like asthma and rheumatoid arthritis)
- Some anti-seizure medications
- Certain cancer medications
- Long-term heparin (blood thinner)
- Proton pump inhibitors for acid reflux
- Medications affecting hormone levels
Symptoms of Osteopenia
One important characteristic of osteopenia is that it typically produces no symptoms. You cannot feel your bones becoming weaker. This is why osteopenia is sometimes called a “silent” condition in its early stages. Many people discover they have osteopenia only when they undergo bone density testing for other reasons or after sustaining a fracture.
While osteopenia itself doesn’t cause symptoms, the main complication is an increased risk of bone fractures. Even minor falls or injuries that normally wouldn’t cause serious harm can result in broken bones if you have significantly reduced bone density. Some fractures, particularly hip fractures, can severely impact your quality of life and independence.
Diagnosing Osteopenia
A healthcare provider diagnoses osteopenia using a bone density test, commonly known as a DXA (dual-energy x-ray absorptiometry) scan. This imaging test measures the strength and density of your bones by using X-rays to determine how much calcium and other minerals are present in your bones.
During a DXA scan, you lie on a padded table while an X-ray arm passes over your body, typically scanning your hip, spine, and sometimes your forearm. The test is painless, non-invasive, and involves minimal radiation exposure. The results are presented as T-scores, which compare your bone density to that of a healthy young adult.
Understanding T-Scores: A T-score of -1.0 or higher is considered normal bone density. A T-score between -1.0 and -2.5 indicates osteopenia. A T-score of -2.5 or lower indicates osteoporosis.
When to Get Tested: Most people should have their bone density checked every few years after turning 50 or entering postmenopause. However, you might need more frequent monitoring if you have significant risk factors or a family history of osteoporosis. Your healthcare provider will recommend an appropriate screening schedule based on your individual risk factors.
Treatment and Management of Osteopenia
The good news about osteopenia is that it is manageable and often reversible with appropriate intervention. The goal of treatment is to slow bone loss and, in many cases, improve bone density before it progresses to osteoporosis.
Calcium and Vitamin D Supplementation
Calcium and vitamin D are fundamental to bone health. Calcium is the primary mineral that gives bones their strength, while vitamin D helps your body absorb calcium. Most healthcare providers recommend calcium and vitamin D supplementation as a first-line treatment for osteopenia.
The recommended daily calcium intake for most adults is 1,000-1,200 mg, with higher amounts needed for certain age groups. Vitamin D recommendations typically range from 600-2,000 IU daily, depending on age and other factors. Your healthcare provider can recommend appropriate supplement doses based on your individual needs and dietary intake.
Dietary Changes
Optimizing your diet for bone health is crucial. Focus on incorporating calcium-rich foods including dairy products like milk, cheese, and yogurt, as well as dark leafy greens such as spinach, kale, and broccoli. Other calcium sources include fortified plant-based milk alternatives, salmon with bones, and almonds.
Additionally, ensure adequate protein intake, as protein is essential for bone structure. Include sources of vitamin C, which is necessary for collagen formation in bones, such as citrus fruits, berries, and bell peppers.
Weight-Bearing and Strength-Training Exercise
Exercise is one of the most effective ways to maintain and improve bone density. Weight-bearing exercises—activities where your feet and legs work against gravity—stimulate bone formation and help maintain bone mass. These include walking, jogging, dancing, and hiking.
Strength-training exercises, where you use resistance to build muscle, are equally important. Muscle pulls on bones, which stimulates them to maintain or increase their density. Resistance training with weights, resistance bands, or bodyweight exercises can significantly benefit bone health.
Aim for at least 150 minutes of moderate-intensity aerobic activity and two or more days of strength training per week. Always consult with your healthcare provider before starting a new exercise program, particularly if you have significant osteopenia or other health conditions.
Lifestyle Modifications
Several lifestyle changes can help slow bone loss:
- Quit Smoking: Smoking accelerates bone loss and significantly increases fracture risk
- Limit Alcohol: Excessive alcohol consumption interferes with calcium absorption and bone formation
- Fall Prevention: Reduce your risk of falls by maintaining good balance, wearing appropriate footwear, and making your home safer
- Adequate Sleep: Bone remodeling occurs during sleep, so getting 7-9 hours nightly supports bone health
Pharmacological Treatment
In some cases, particularly when lifestyle modifications aren’t sufficient or when fracture risk is high, your healthcare provider may recommend medications to treat osteopenia. Various classes of medications can help slow bone loss or increase bone density, including bisphosphonates, hormone-related therapy, and other specialized treatments. Your provider will determine if medication is appropriate based on your specific situation.
Can Osteopenia Be Reversed?
The encouraging news is that osteopenia can often be reversed or halted with appropriate intervention. Some people can regain a typical amount of bone density through consistent implementation of lifestyle modifications and, when appropriate, medical treatment. The sooner you know you have osteopenia, the better your chances of preventing progression to osteoporosis and potentially reversing bone loss.
Prevention Strategies for Bone Health
Whether you have osteopenia or want to prevent its development, these bone health strategies are essential:
- Ensure adequate calcium and vitamin D intake through diet and supplementation
- Engage in regular weight-bearing and strength-training exercises
- Maintain a healthy body weight
- Avoid smoking and excessive alcohol
- Get regular bone density screenings as recommended by your healthcare provider
- Manage underlying health conditions that affect bone health
- Review medications with your provider to identify any that might affect bone density
Frequently Asked Questions (FAQs)
Q: How often should I get bone density tests if I have osteopenia?
A: Your healthcare provider will recommend an appropriate screening schedule based on your age, sex, and risk factors. Generally, bone density tests are repeated every 1-2 years to monitor changes and track the effectiveness of treatment.
Q: Is osteopenia hereditary?
A: Yes, osteopenia has a genetic component. If your family members have osteoporosis or osteopenia, you have a higher risk of developing these conditions. However, lifestyle factors also play a significant role, so preventive measures are important even with family history.
Q: Can young people develop osteopenia?
A: While osteopenia is more common in older adults, younger people can develop it due to certain medical conditions, medications, lifestyle factors, or genetic predisposition. Young people with risk factors should discuss bone health screening with their healthcare provider.
Q: How long does it take to see improvement in bone density with treatment?
A: Improvements in bone density typically take 1-2 years to become measurable on bone density scans. Consistency with exercise, nutrition, supplementation, and medication (if prescribed) is essential for seeing positive results.
Q: Does osteopenia always progress to osteoporosis?
A: No. With appropriate management, many people with osteopenia never develop osteoporosis. Early intervention and lifestyle modifications can halt bone loss progression and sometimes reverse the condition.
Q: Can I exercise if I have osteopenia?
A: Yes, exercise is one of the best things you can do for osteopenia. Weight-bearing and strength-training exercises help maintain and build bone density. However, consult your healthcare provider about appropriate exercises for your specific situation.
Q: What is the cost of bone density testing?
A: DXA scan costs vary depending on your location and healthcare facility, but many insurance plans cover bone density screening for eligible individuals. Ask your healthcare provider about coverage and costs in your area.
References
- Osteopenia: What Is It, Symptoms, Causes & Treatment — Cleveland Clinic. 2024-03-19. https://my.clevelandclinic.org/health/diseases/21855-osteopenia
- An observational study on the adherence to treatment guidelines of osteopenia and osteoporosis — National Center for Biotechnology Information. 2009. https://pubmed.ncbi.nlm.nih.gov/19514830/
- What Is Osteopenia and How Does it Affect Older Adults? — National Council on Aging. 2024. https://www.ncoa.org/article/what-is-osteopenia-and-how-does-it-affect-older-adults/
- DXA and Clinical Challenges of Fracture Risk Assessment in Primary Care — Cleveland Clinic. 2024. https://consultqd.clevelandclinic.org/dxa-and-clinical-challenges-of-fracture-risk-assessment-in-primary-care
- In rebuttal: Osteopenia is a useful diagnosis — Cleveland Clinic Journal of Medicine. 2006. https://www.ccjm.org/content/ccjom/73/1/34.full.pdf
- 8 Tips for Healthy Bones — Cleveland Clinic. 2024. https://health.clevelandclinic.org/bone-health
Read full bio of medha deb











