Ovarian Cyst Causes: 7 Common Reasons And What To Watch
Understanding the common and rare causes of ovarian cysts, from functional types to serious conditions like endometriosis and PCOS.
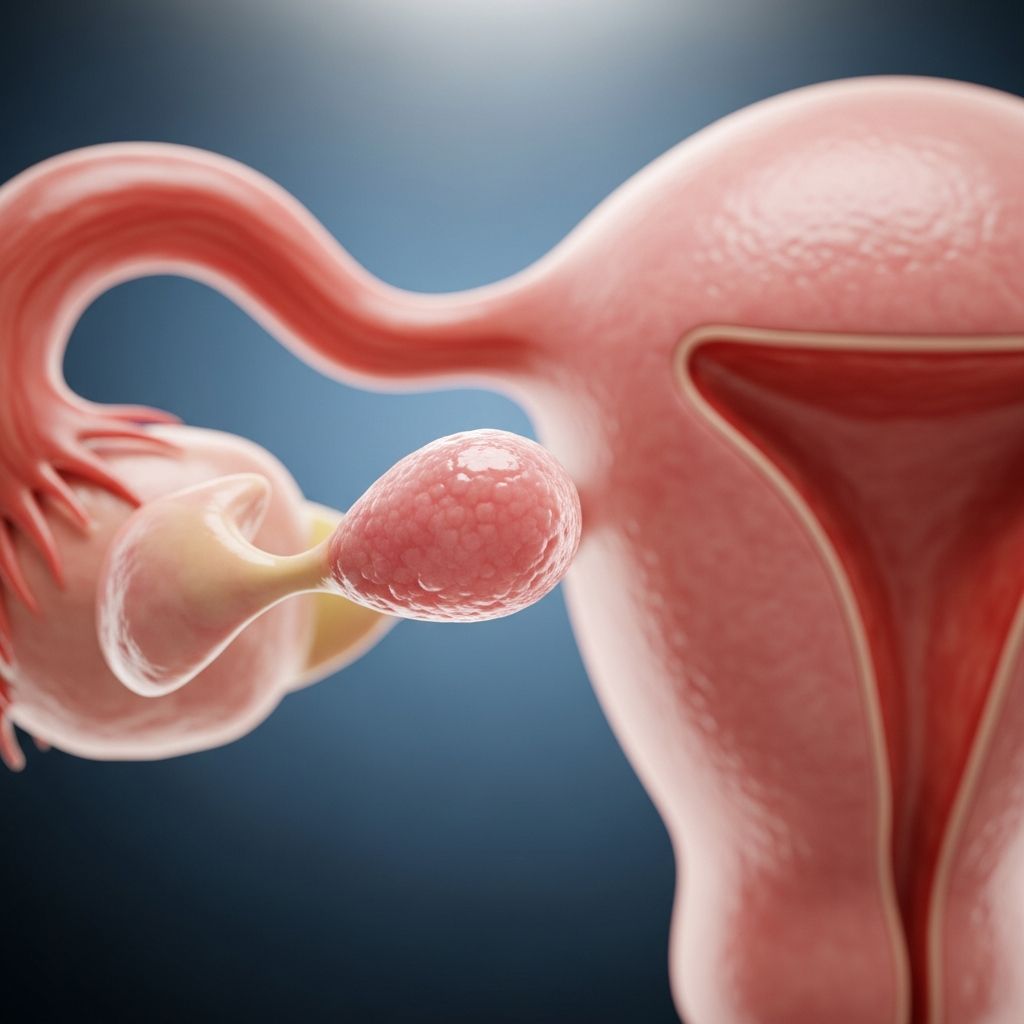
Ovarian cysts are fluid-filled sacs that develop on or within the ovaries, often during reproductive years, and most are benign and resolve without intervention.
What Are Ovarian Cysts?
An
ovarian cyst
is a sac filled with fluid or semisolid material that forms on or inside an ovary. These are common, affecting about 20% of women with at least one pelvic mass in their lifetime, particularly during childbearing years. Most cysts are noncancerous, asymptomatic, and disappear on their own within a few months. However, some can grow large, rupture, twist, or rarely become malignant, necessitating medical attention.Ovaries, almond-sized organs in the pelvis, produce eggs and hormones like estrogen and progesterone. Cysts arise from normal processes like ovulation or underlying conditions disrupting ovarian function.
Common Causes of Ovarian Cysts
Ovarian cysts stem from diverse etiologies, ranging from physiological ovulation to pathological conditions. Key causes include:
- Ovulation-related issues: Normal menstrual cycles involve follicle development; disruptions lead to cysts.
- Hormonal imbalances: Excess follicle-stimulating hormone (FSH) or absent luteinizing hormone (LH) surge prevents egg release.
- Endometriosis: Tissue similar to uterine lining grows on ovaries, forming blood-filled cysts.
- Polycystic ovary syndrome (PCOS): Multiple small cysts due to elevated androgens.
- Pelvic inflammatory disease (PID): Infection spreads to ovaries.
- Pregnancy: Elevated human chorionic gonadotropin (hCG) stimulates cyst formation.
- Infertility treatments: Gonadotropins cause ovarian hyperstimulation syndrome.
Postmenopausal women face higher malignancy risks with any cyst, warranting vigilant monitoring.
Types of Ovarian Cysts
Over 30 subtypes exist, classified as functional (benign, ovulation-related) or pathologic (disease-associated, potentially neoplastic). Here’s a breakdown:
Functional Cysts
The most prevalent, forming during the menstrual cycle and typically resolving in 1-3 months.
- Follicular cysts: Occur when the follicle fails to rupture and release the egg mid-cycle, growing larger than 2.5 cm due to FSH overstimulation. They produce excess estradiol, causing irregular menstruation.
- Corpus luteum cysts: After egg release, the follicle becomes the corpus luteum; if the opening seals, fluid accumulates.
- Theca lutein cysts: From hCG overstimulation in pregnancy, gestational trophoblastic disease, or hyperstimulation.
Pathologic Cysts
- Endometriomas (chocolate cysts): Endometriosis invades ovaries, filling cysts with old blood. They appear as complex masses with ‘ground glass’ echoes on ultrasound and raise malignancy risk slightly.
- Cystadenomas: Benign surface growths filled with watery or mucous material; can become very large.
- Teratomas (dermoid cysts): From germ cells, containing hair, skin, teeth; noncancerous but odd.
- Polycystic ovaries in PCOS: Enlarged ovaries with numerous small follicles from hyperandrogenism, affecting 5-10% of reproductive-age women and linking to infertility, diabetes.
Note: Neoplastic cysts from cell overgrowth may be benign (serous/mucinous) or malignant, especially if solid or mixed.
Risk Factors for Developing Ovarian Cysts
Certain factors elevate cyst likelihood:
| Risk Factor | Description |
|---|---|
| Age | Reproductive years common; postmenopausal higher malignancy risk. |
| Pregnancy | hCG peaks in second trimester. |
| Infertility drugs | Gonadotropins induce hyperstimulation. |
| Hypothyroidism | Hormonal disruption. |
| Cigarette smoking | Increases incidence. |
| Tamoxifen use | Hormone therapy side effect. |
| Tubal ligation | Associated with functional cysts. |
| History of cysts | Recurrence risk. |
While unavoidable factors exist, smoking cessation and regular check-ups mitigate risks.
Symptoms of Ovarian Cysts
Many cysts are silent, discovered incidentally via ultrasound. When symptomatic:
- Mild: Pelvic pain (one side), bloating, painful intercourse, heavy/painful periods.
- Severe (emergency): Sudden sharp pain, fever >101°F, nausea/vomiting, dizziness—indicating rupture, torsion, or infection. Seek immediate care.
Large cysts press on bladder/bowel, causing urinary/frequency issues.
Diagnosis and Treatment
Diagnosis involves pelvic exam, transvaginal ultrasound (gold standard for characterizing cysts), blood tests (CA-125 for malignancy risk), or laparoscopy. Management depends on type, size, symptoms, age:
- Watchful waiting: For small, functional cysts in premenopausal women.
- Medication: Hormonal birth control prevents new functional cysts.
- Surgery: Laparoscopy for large/persistent/suspicious cysts; oophorectomy if cancerous.
Pregnancy-adapted approaches avoid fetal harm.
Prevention and When to See a Doctor
No sure prevention, but oral contraceptives reduce functional cysts. Routine pelvic exams aid early detection. Consult a provider for unexplained pelvic pain, abnormal bleeding, or bloating, especially postmenopausal.
Frequently Asked Questions (FAQs)
Are ovarian cysts cancerous?
Most are benign, especially functional types. Postmenopausal or complex cysts raise concern; ultrasound/CA-125 guides evaluation.
Do ovarian cysts affect fertility?
Usually not, but PCOS or endometriomas can. Treatment often restores fertility.
How long do ovarian cysts last?
Functional cysts resolve in 1-3 months; others may need intervention.
Can ovarian cysts burst?
Yes, causing severe pain; rupture is medical emergency if infected.
Do all women get ovarian cysts?
No, but 20% develop at least one adnexal mass lifetime.
References
- 5 Signs You May Have an Ovarian Cyst — AdventHealth. 2023. https://www.adventhealth.com/blog/5-signs-you-may-have-ovarian-cyst
- Ovarian Cyst – StatPearls — NCBI Bookshelf / StatPearls Publishing. 2023-10-16. https://www.ncbi.nlm.nih.gov/books/NBK560541/
Read full bio of Sneha Tete











