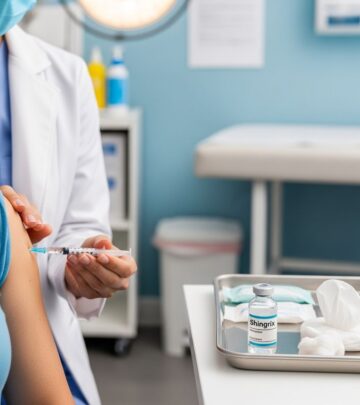
Pacemaker Insertion: Complete Guide to the Procedure
Learn about pacemaker insertion, why it's needed, what to expect, and recovery guidelines.
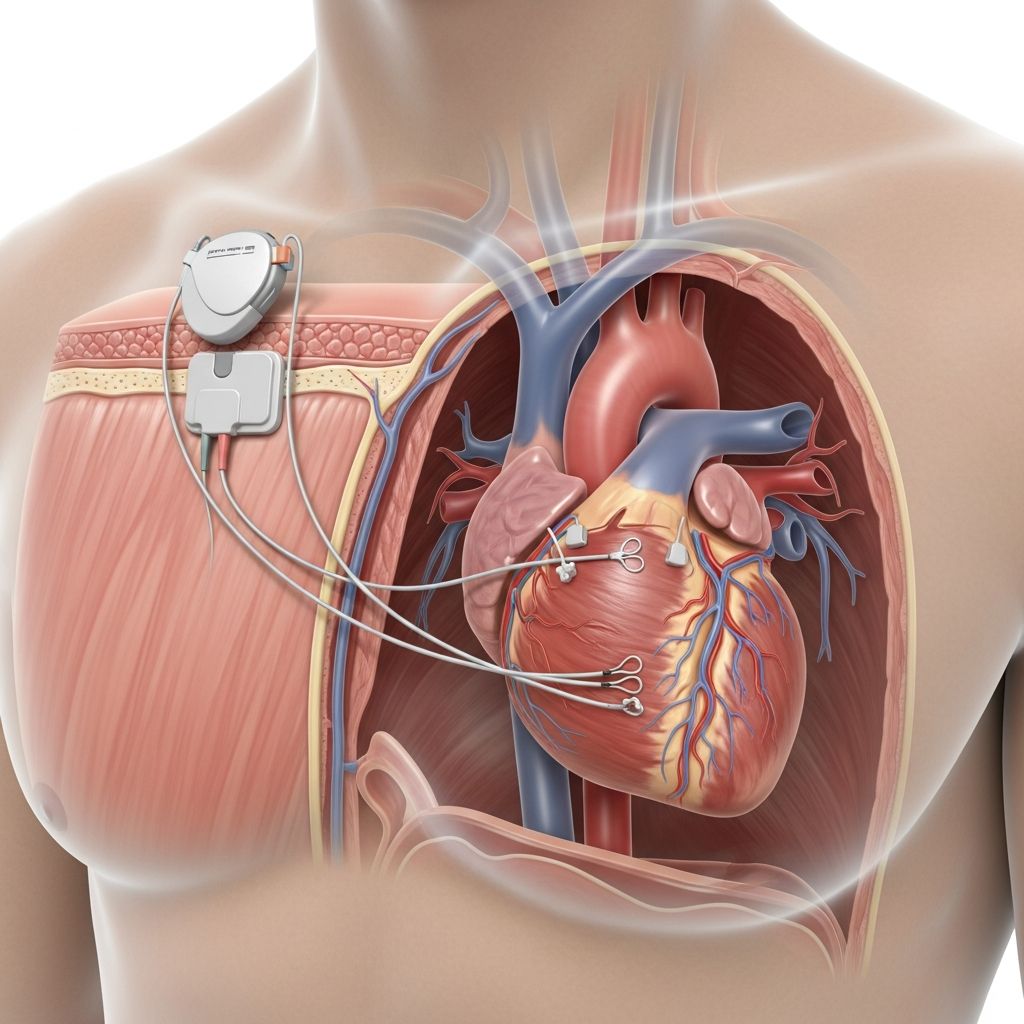
Understanding Pacemaker Insertion
A pacemaker is a small, battery-powered device designed to help regulate your heart’s rhythm by sending electrical impulses to the heart muscle. Pacemaker insertion is a minimally invasive surgical procedure that implants this device beneath your skin, typically near the collarbone. This procedure can be used as a short-term or long-term treatment, depending on your specific cardiac condition and medical needs. The device works continuously to monitor your heart’s electrical activity and delivers precisely timed electrical pulses when your heart rate becomes too slow, irregular, or abnormal.
Why You Might Need a Pacemaker
Your cardiologist may recommend pacemaker insertion if you experience certain heart rhythm problems or conditions that affect how your heart functions. Understanding the reasons for this procedure can help you prepare mentally and physically for the surgery.
Common indications for pacemaker insertion include:
– A heart that beats too slowly (bradycardia) or unevenly- Heart rhythms that alternate between normal and abnormally slow or fast rates- Severe heart failure or cardiomyopathy (weakened heart muscle)- Complications following heart surgery- Conduction disorders where the electrical signals in your heart are blocked or delayed
Your doctor will perform comprehensive testing to determine whether a pacemaker is the right treatment for your condition. This may include electrocardiograms (EKGs), Holter monitors, and other diagnostic tests to assess your heart’s electrical activity over time.
Preparing for Your Pacemaker Procedure
Proper preparation is essential for ensuring the procedure goes smoothly and for minimizing complications. Your healthcare team will provide specific instructions tailored to your individual health status and medical history.
Pre-Procedure Consultation
Before your pacemaker insertion, you will meet with your surgical team to discuss important aspects of the procedure. During this consultation, your doctor will review your anesthesia options, discuss any drug allergies you may have, and review all current medications, herbs, and supplements you are taking. Some medications may need to be stopped before surgery, particularly blood thinners and certain heart medications. Your doctor will also discuss fasting requirements—typically you will need to avoid food and drink after midnight the night before your procedure. You should arrange for a ride to and from the hospital, as you will not be able to drive immediately after surgery.
Pre-Operative Tests
Your healthcare provider will order several tests before your procedure to ensure you are healthy enough for surgery. These tests typically include blood work, a chest X-ray, and an electrocardiogram. These tests help your surgical team understand your baseline health status and identify any potential risks that need to be addressed before the procedure begins.
What Happens During Pacemaker Insertion
Understanding the procedural steps can help reduce anxiety and prepare you for what to expect on the day of your surgery.
Anesthesia
During pacemaker insertion, you will receive local anesthesia to numb the area where the incision will be made. Unlike general anesthesia, local anesthesia keeps you awake but pain-free. Your medical team may also provide sedation to help you relax throughout the procedure. You will remain conscious enough to communicate with your surgical team if needed.
The Surgical Procedure
Your surgeon will make a small incision beneath your collarbone, typically about 1 to 2 inches long. Through this incision, the surgeon will insert the pacemaker device. The device’s wires, called leads, are carefully threaded through a vein from the collarbone area to the heart. The surgeon positions these leads so they make proper contact with your heart muscle, allowing them to both sense your heart’s natural electrical activity and deliver pacing pulses when needed.
Once the leads are properly positioned and tested to ensure they function correctly, the pacemaker is secured in place beneath the skin. Your surgeon will then close the incision with stitches and apply a sterile bandage over the site. The entire procedure typically takes about two hours, though this can vary depending on the complexity of your specific situation and whether you are receiving a single-chamber or dual-chamber pacemaker.
Pain During the Procedure
Because you receive local anesthesia, you should not feel pain during the procedure. However, you may feel pressure or mild discomfort as your surgeon works. If you experience any significant pain during the procedure, inform your surgical team immediately so they can provide additional anesthesia.
Hospital Stay and Recovery Timeline
The length of your hospital stay depends on your individual circumstances and how well you recover from the procedure.
Immediate Post-Procedure Period
After your pacemaker insertion is complete, you will be moved to a recovery room where nursing staff will monitor your vital signs, heart rhythm, and overall condition. Most patients can go home the same day, though some may need to stay overnight for observation. Pain is common in the first few days following the procedure, but your doctor will provide pain medication to manage any discomfort. You should expect some soreness and mild swelling at the incision site, which is normal and typically resolves within a few weeks.
Recovery Duration
Initial recovery takes approximately one week, during which you should limit physical activities as directed by your healthcare provider. Full recovery can take up to eight weeks. During this time, you should avoid heavy lifting, straining, and strenuous exercise. Your doctor will provide specific guidance about when you can return to work, driving, and other normal activities. Most people can resume light activities within a week or two, with gradual progression to full activity levels as the incision heals.
Infection Prevention After Pacemaker Insertion
Infection prevention is crucial during your recovery. Healthcare providers take multiple precautions to minimize infection risk, including proper hand hygiene, use of sterile gloves and masks, and keeping your incision properly covered. You can also take steps to protect yourself from infection:
– Wash your hands frequently, especially before touching the incision area- Remind visitors and healthcare staff to wash their hands before contact- Request that staff wear gloves or masks when handling your incision- Do not allow others to touch your incision site- Keep the incision clean and dry as instructed- Change bandages according to your doctor’s instructions
Possible Complications
While pacemaker insertion is generally a safe procedure, all surgeries carry some risk. Complications are rare, but it is important to be aware of potential problems and discuss them with your surgical team.
Common Possible Complications
– Excess bleeding at the incision site- Infection at the surgical site or within the heart tissue- Device malfunction or failure- Muscle spasms in the chest and abdominal area- Rare but serious: rupture of the heart muscle- Collapsed lung (pneumothorax)- Lead displacement or fracture
Risk Factors
Certain factors may increase your risk of experiencing complications from pacemaker insertion:
– Smoking history- Excessive alcohol consumption- Chronic conditions such as diabetes or obesity- Advanced age- Severe kidney or liver disease- Bleeding disorders or use of blood-thinning medications- Poor overall health status
When to Contact Your Doctor
Following your pacemaker insertion, contact your healthcare provider if you experience any of the following symptoms:
– Signs of infection: fever, chills, or redness at the incision site- Excessive bleeding, redness, swelling, or unusual discharge from the incision- Pain that cannot be controlled with prescribed medications- Coughing, difficulty breathing, or chest pain- Irregular heartbeats: unusually fast, slow, or uneven heart rhythm- Dizziness or fainting episodes- Shortness of breath at rest or with minimal activity
Emergency Situations
Call emergency services immediately if you experience severe chest pain, difficulty breathing, loss of consciousness, or signs of a severe allergic reaction. Do not wait to see if symptoms resolve on their own in these situations.
Medical Tests and Procedures with a Pacemaker
After pacemaker insertion, most medical tests and procedures remain safe for you to undergo. However, you must always inform healthcare providers about your pacemaker before any test or procedure. Some imaging tests and procedures require special considerations:
| Medical Test/Procedure | Pacemaker Compatible | Special Considerations |
|---|---|---|
| MRI (Magnetic Resonance Imaging) | Newer machines only | Older MRI machines may interfere with pacemakers; inform technician |
| CT Scan | Yes | Generally safe; inform technician of device |
| X-rays | Yes | Safe; no special precautions needed |
| Ultrasound | Yes | Generally safe; inform technician |
| Electrocautery | Conditional | Devices creating energy may interfere; discuss with doctor |
| Dental Work | Yes | Safe; inform dentist of pacemaker |
Pacemaker Replacement and Maintenance
Pacemakers are powered by batteries that gradually lose charge over time. When your pacemaker’s battery runs low, typically after 5 to 15 years depending on usage, your device will need to be replaced. Unlike battery replacement in other devices, pacemaker replacement involves replacing the entire generator unit rather than just the battery. During replacement, your surgeon makes a small incision at the original surgical site and removes the old pacemaker while leaving the existing leads in place if they are still functioning properly. The new pacemaker is then connected to these existing leads. The replacement procedure is quicker than the original implantation, and recovery time is typically shorter as well.
Living with Your Pacemaker
After your pacemaker insertion and recovery period, most people return to their normal activities and enjoy an improved quality of life with better heart rhythm management. Your cardiologist will schedule regular follow-up appointments to monitor your pacemaker’s function through device checks. These checks can often be performed remotely using wireless technology. You will receive a pacemaker identification card that you should carry at all times and present to healthcare providers before any tests or procedures. Avoid placing magnets or electronic devices directly over your pacemaker, and inform security personnel about your device when passing through metal detectors.
Frequently Asked Questions About Pacemaker Insertion
Q: How long does a pacemaker insertion procedure take?
A: The procedure typically takes about two hours, though the duration can vary depending on the complexity of your condition and whether you require a single-chamber or dual-chamber device.
Q: Will I feel pain during the pacemaker insertion procedure?
A: No, you will receive local anesthesia to numb the area where the incision is made. You may feel pressure or mild discomfort, but you should not experience pain. Inform your surgical team if you do feel pain so they can provide additional anesthesia.
Q: Can I go home the same day after pacemaker insertion?
A: Many patients can go home the same day after pacemaker insertion. Some may need to stay overnight for observation. Your healthcare team will determine what is best for your individual situation.
Q: How long is the recovery period after pacemaker insertion?
A: Initial recovery takes about one week, during which you should limit physical activities. Full recovery can take up to eight weeks. Your doctor will provide specific guidance about returning to normal activities.
Q: What activities should I avoid after pacemaker insertion?
A: You should avoid heavy lifting, strenuous exercise, and activities that strain your chest area for several weeks. Your doctor will provide specific recommendations based on your individual recovery progress.
Q: Can I have an MRI with a pacemaker?
A: Newer MRI machines are compatible with pacemakers, but older machines may not be. Always inform your healthcare provider about your pacemaker before any imaging test so they can determine if special precautions are needed.
Q: How often do I need to have my pacemaker checked?
A: Your cardiologist will schedule regular follow-up appointments to monitor your pacemaker’s function. Many checks can be performed remotely using wireless technology. The frequency of checks depends on your individual needs and device type.
Q: How long does a pacemaker last?
A: Pacemaker batteries typically last between 5 and 15 years, depending on how often the device is used to pace your heart. Your doctor will monitor battery status during regular check-ups.
References
- Pacemaker Insertion — SUNY Upstate Medical University, Department of Cardiac Surgery. 2024. https://www.upstate.edu/cardiacsurgery/surgical-procedures/pacemaker-insertion.php
- Pacemaker Insertion in Congenital Heart Disease — Parent Teaching Education Development (PTED). 2024. https://www.pted.org/?id=pacemaker1
- Frequently Asked Questions About Pacemakers — Healthgrades. 2024. https://resources.healthgrades.com/right-care/pacemakers/frequently-asked-questions-about-pacemakers
- Techniques of Pacemaker and ICD Implantation and Removal — Johns Hopkins University. Published May 15, 2020. https://pure.johnshopkins.edu/en/publications/techniques-of-pacemaker-and-icd-implantation-and-removal/
- Cardiac Pacing: Permanent Pacemaker Insertion or Replacement — ACCA Rent Health. 2024. https://www.accarenthealth.com/procedure/list?patientType=ADULT&procedureTypeCode=05&procedureCode=33206A
Read full bio of Sneha Tete