Palisaded and Encapsulated Neuroma Pathology
Detailed pathology of palisaded and encapsulated neuroma: a benign dermal nerve sheath tumour with distinctive histological features.
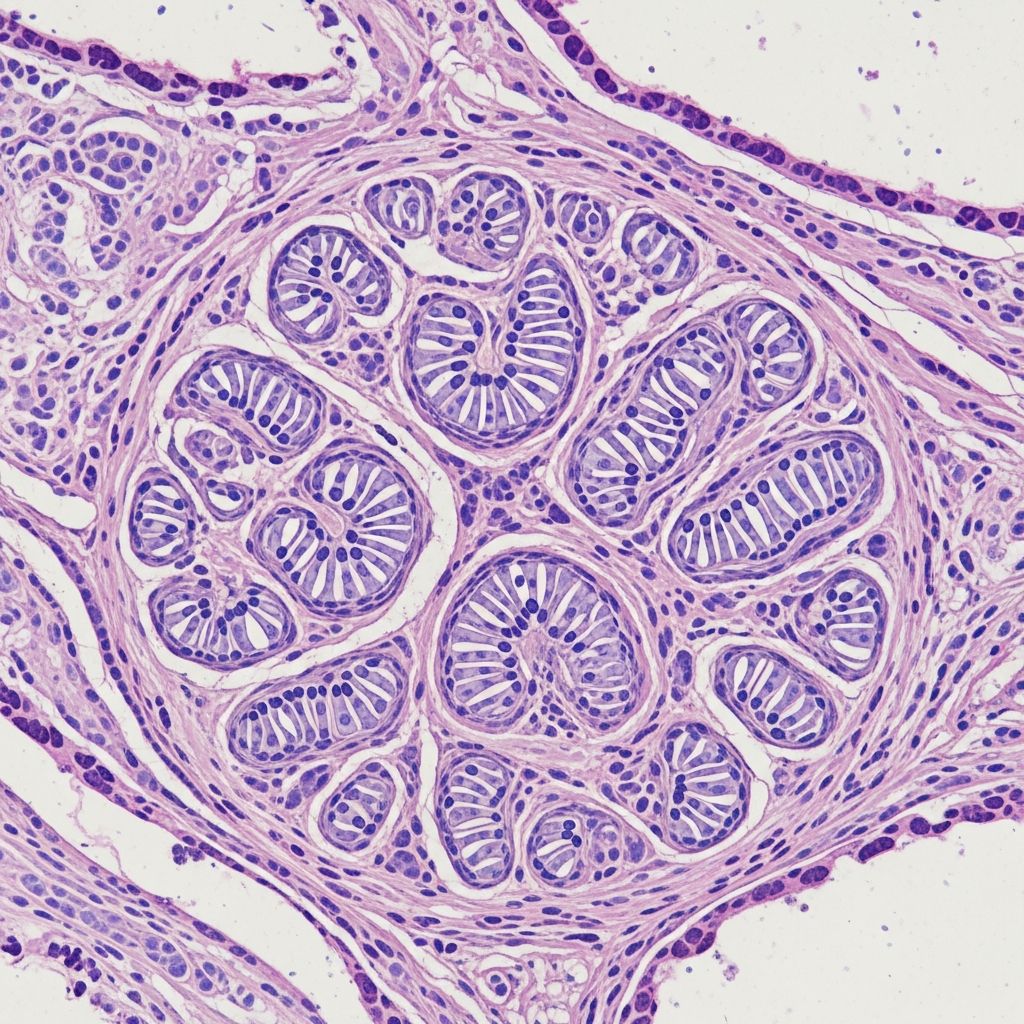
Author: Dr. Harriet Cheng, Dermatopathologist, A/Prof. Paul Chee, Dermatopathologist, DermNet New Zealand, www.dermnetnz.org 2024
Palisaded and encapsulated neuroma, also known as solitary circumscribed neuroma, is a rare benign cutaneous nerve sheath tumour characterized by a well-circumscribed dermal nodule. This tumour typically presents as a small, firm, flesh-coloured papule, most commonly on the face, and requires histopathological examination for definitive diagnosis due to its resemblance to other neural neoplasms.
Introduction
Palisaded and encapsulated neuroma (PEN) is a distinctive benign neoplasm arising from nerve sheath cells in the dermis. First described in 1993, it is distinguished by its encapsulated structure, palisading spindle cells, and presence of axons traversing the lesion, setting it apart from other neural tumours like schwannomas and neurofibromas. Clinically, PEN manifests as a solitary, slow-growing, dome-shaped nodule measuring 2-6 mm, predominantly affecting adults aged 40-60 years, with a slight female predominance. Although typically asymptomatic, lesions may occasionally cause mild tenderness. While the face, particularly around the eyes, nose, and mouth, is the most common site, rarer occurrences on the trunk, extremities, and acral areas have been documented. The aetiology remains unclear, with proposed associations to local trauma or reactive hyperplasia, though no definitive link to syndromes like multiple endocrine neoplasia type 2B has been established except in rare cases.
Clinical features
PEN typically appears as a small, firm, non-ulcerated, flesh-coloured or pink papule or nodule, often with a smooth surface. Lesions are usually solitary but multiple lesions can occur in up to 5-10% of cases. Common locations include the periorbital area, nose, cheeks, and lips, near mucocutaneous junctions. Less frequently, they arise on the trunk, arms, legs, hands, feet, or genitalia. The overlying epidermis is intact, and there is no epidermal collarette or tethering to the surface, distinguishing it clinically from basal cell carcinoma or epidermal cysts. Patients often report incidental discovery or mild irritation; pain is uncommon unless traumatized. Dermoscopic features are non-specific, showing a homogenous pink or white structureless area, prompting biopsy for suspected malignancy.
Pathology
Macroscopic
Grossly, the excision specimen reveals a well-circumscribed, tan-white nodule measuring 2-6 mm in diameter, confined to the dermis without subcutaneous extension. The cut surface is homogeneous and firm, with no haemorrhage or necrosis.
Microscopic
Histologically, PEN presents as a sharply demarcated, unencapsulated or thinly encapsulated dermal tumour beneath an attenuated or normal epidermis. A characteristic cleft or split forms between the tumour and adjacent dermis, creating a lacunae-like artefact (figures 1, 2). The lesion comprises interlacing fascicles of bland spindle cells with wavy, uniform nuclei exhibiting nuclear palisading reminiscent of Verocay bodies in schwannomas. The stroma is loose, myxoid or collagenous, with delicate collagen bundles separating cell bundles. Notably, axons course longitudinally through the tumour, confirmed by neurofilament staining, unlike true schwannomas. Mast cells are often prominent, and degenerative changes like hyalinisation may occur in older lesions. No cytological atypia, mitoses, or necrosis is seen, confirming its benign nature.
Key microscopic features:
- Well-circumscribed dermal nodule
- Clefting artefact between tumour and dermis
- Fascicles of spindle cells with palisading nuclei
- Loose myxoid or collagenous stroma
- Intra-tumoural axons
- Prominent mast cells
- Absence of atypia or mitoses
Immunohistochemistry
PEN shows strong, diffuse positivity for S100 protein in spindle cells, confirming neural differentiation. The perineurial capsule stains for EMA. Neurofilament highlights axons traversing the lesion. Spindle cells are negative for GFAP, SOX10 variable, and collagen IV positive around vessels but not diffusely. Factor XIIIa-positive dendritic cells are often intermixed. These markers distinguish PEN from neurofibroma (CD34+, collagen IV variable) and schwannoma (SOX10+, no axons).
| Marker | Staining Pattern |
|---|---|
| S100 | Diffuse strong positive in spindle cells |
| EMA | Positive in capsule (perineurial) |
| Neurofilament | Positive axons within tumour |
| GFAP | Negative |
| CD34 | Focal or negative |
| Collagen IV | Positive in vessels |
Electron microscopy
Ultrastructurally, spindle cells display features of Schwann cells, including mesaxon-like processes forming myelin figures, and perineurial-like cells with long processes and collagen pockets. Axons with neurotubules and neurofilaments are enveloped by tumour cells, supporting the reactive or hyperplastic theory over a true neoplasm.
Differential diagnosis
PEN’s clinical mimicry of basal cell carcinoma and histological similarity to neural tumours necessitates careful differentiation.
| Diagnosis | Key distinguishing features |
|---|---|
| Schwannoma | Encapsulated, Antoni A/B areas, Verocay bodies, no axons, deeper location, SOX10+ |
| Neurofibroma | Poorly circumscribed, wavy cells in mucinous stroma, CD34+, collagen IV variable/negative, no palisading |
| Neurotropic melanoma | Atypia, mitoses, junctional activity, MART-1+, HMB45 variable |
| Basal cell carcinoma (sclerosing) | Clinical pearly papule, basaloid islands, retraction artefact, BerEP4+, Ki67 high |
| Epidermoid cyst | Cystic, keratin-filled, epidermal lining |
| Melanocytic naevus | Melanocytes, junctional nests, HMB45+, MITF+ |
Schwannomas lack axons and show cellular heterogeneity, while neurofibromas are infiltrative with mixed cell types. Malignant mimics like neurotropic melanoma exhibit atypia and immunohistochemical divergence.
Clinicopathological variants
- Multiple PEN: Rare, associated with MEN2B or eruptive forms.
- Mucosal PEN: Oral cavity or genital mucosa.
- Atypical PEN: Increased cellularity or mitoses but benign behaviour.
- Acral PEN: Periungual or plantar sites in skin of colour.
Management
Complete surgical excision is curative, with no recurrence reported. Conservative excision suffices due to the superficial location and benign nature. No adjuvant therapy is required.
Prognosis
PEN is entirely benign with no malignant potential. Local recurrence is exceedingly rare post-excision.
Frequently asked questions
Q: What is palisaded and encapsulated neuroma?
A: A benign dermal nerve sheath tumour presenting as a small flesh-coloured papule, diagnosed by histopathology showing palisading spindle cells and axons.
Q: Is palisaded encapsulated neuroma cancerous?
A: No, it is completely benign with no risk of malignancy.
Q: Where do these lesions commonly occur?
A: Primarily on the face near mucocutaneous junctions, but can appear on trunk or extremities.
Q: How is it treated?
A: Simple surgical excision, which is curative.
Q: What does it look like under the microscope?
A: Fascicles of palisading spindle cells in a myxoid stroma with clefting and axons, S100 positive.
References
- Palisaded and encapsulated neuroma pathology — DermNet New Zealand. 2024. https://dermnetnz.org/topics/palisaded-and-encapsulated-neuroma-pathology
- A Case Report and Review of Palisaded Encapsulated Neuroma — NIH/PMC. 2016-08-25. https://pmc.ncbi.nlm.nih.gov/articles/PMC5016044/
- Palisaded encapsulated neuroma — Wikipedia (informed by primary sources). 2024. https://en.wikipedia.org/wiki/Palisaded_encapsulated_neuroma
- Palisaded Encapsulated Neuroma (Solitary Circumscribed Neuroma) — YouTube/Jerad Gardner MD. 2019-08-09. https://www.youtube.com/watch?v=sFpRPU4uHuY
Read full bio of Sneha Tete












